Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
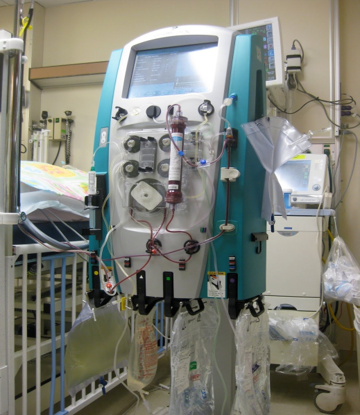
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Peter, as part of my 1:1 consulting and advocacy service! Peter’s mom is in ICU with kidney failure but the doctors don’t recommend dialysis and Peter is asking if it is a form of treatment limitation.
My Mom is in ICU with Kidney Failure but the Doctors Don’t Recommend Dialysis. Is it a Form of Treatment Limitation?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Peter here.”
Patrik: Yeah, so you could use one of the unlimited options of course or you could just book an hour if that’s the case. So I have options. I have unlimited options and I have just the hour option. Depending on how long you think it’ll take. We can look into that once you’ve reached … I’ll email all of that to you and then have a look and then if you have any questions regarding those options please let me know.
Peter: Okay, great. Thank you so much.
Patrik: You are very welcome. I’ll talk to you soon. Take care for now.
Peter: All right, thanks, bye bye.
Patrik: The very best. Bye.
Peter: Bye.
RECOMMENDED:
Peter: No, I left the hospital. I actually came home to take a shower. I was there, I was there to hold them, so I came right over.
Patrik: Right. Overnight? Are you there overnight as well?
Peter: I was there to like midnight and my sister came and um, relieved me till this morning. Yeah. She’s not looking. She’s swollen. Her face is more puffy now. I don’t know. I’m confused. I’m just confused.
Patrik: Is she alert?
Peter: She is not alert right now. No, she wasn’t. She’s alert because they put a Nasogastric tube cause she’s just, she’s draining out a lot of fluids. They put an NG tube in her, but this today didn’t hurt because when she’s awake when she’s alert, she’s uncomfortable.
Patrik: Right. Do you think she’s uncomfortable or in pain?
Peter: I think it’s more pain. I think. More pain maybe. Yeah, it sounds like more pain.
Patrik: What are they giving her for pain? Do you know?
Peter: Oh, I’m not sure. The doctor just said, you know, I’m not sure what they gave her. I’ve asked my sister something. Yeah. The doctor just said they’re going to give her some pain and we didn’t have that speech this morning about, we don’t want to keep suffering her and her kidneys. Now the creatinine is going from 1.8 to around 2, two-point something. So they sent her, she’s going into kidney failure right now and they gave her albumin two days ago. I don’t know. Not that fluid is what is called what caused this, I don’t know, cause the albumin made
Patrik: What? What did the albumin do to her? What do you think?
Peter: Because they say albumin is fluid, so I know it’s supposed to help and protein and stuff, but it’s like she became a way more swollen.
Patrik: It’s, I think, uh, tell you what it normally does. Albumin is reducing swelling, but what could happen is the Albumin may have been so low that what they’ve given, it’s like a drop in the ocean. Right? Usually I’ll boom in reduces swelling, but if her kidneys are failing on the other hand, the albumin may not do anything at all. I’ll be mean. It’s good for swelling, but if the kidneys are failing, it may not be enough. Yeah. What, what, what, what are they doing for the kidney failure?
Peter: They asked us dialysis, but they told me that if she was my mother, I wouldn’t put it up. The dialysis should be too much suffering or what would the family’s willingness to do? Dialysis, you know, so,
RECOMMENDED:
Patrik: And then, then you need to push for that. I mean, if you’re okay, I’ll tell you what I think if your mom wants to fight, then they need to let her fight. Right, is your mom a religious person?
Peter: Yes, she’s spiritual. She believes in God and she’s very spiritual. So she believes in a miracle at the last hour or so. She’s a really spiritual person, you know.
Patrik: Okay. The other reason I’m asking is, you know, terms of religion. So let’s just say, you know, in some situations from what you’re describing, you know, they might say, look, let’s make your mom comfortable and let’s stop treatment and let’s make sure she’s not in any pain. And you know, potentially give her a little bit more than she needs. And then she may pass away peacefully.
Patrik: But some people, especially if they are religious or spiritual and they believe in God, they may think, Oh, that could be perceived as euthanasia. Have you heard of the term euthanasia before?
Peter: Yeah. Euthanasia is the painless something killing of someone with like medicine or something?
Patrik: Yeah, yeah, very much so. Very much so. You know, and depending on where you stand, you know, on a religious, spiritual sort of belief level that goes against some people’s values and beliefs, you know, and if that’s your mom, then you know who you probably need to push in the other direction and you need to, they need to be proactive in treatment. Will that save your mom’s life, I don’t know, will it prolong your mom’s life. Possibly. How long will it prolong your mom’s life? I don’t know. But for some people, that’s very important, you know
Peter: Ok.
Patrik: And that is something I cannot answer for you what’s important for you. But what I can answer for you is that, you know, if she wants everything done and there is no DNR, then they need to do it.
RECOMMENDED:
Peter: Yeah. Yeah. Then the report you saw about the cancer, I mean I don’t really understand that report. Is that is that an advanced, cause I saw metastatic there and I heard metastatic is spreading.
Patrik: Yeah. Metastatic is spreading into other organs. But wasn’t that in January? Wasn’t that report? That was January.
Peter: Correct. Right, right.
Patrik: So I mean now it’s July, I guess. You know, she might have deteriorated since. I don’t think that metastatic cancer is curable, you know, that’s, but I don’t think that’s even what you or your mom wants to achieve. I guess what you and your mom want to achieve is potentially have the treatment and also have it on her terms and not on their terms. Is that something you can resonate with or,
Peter: Yeah, but the question then is like for how long, if the end result is still going to be the same, right.
Patrik: But I mean it’s, is living for another week is, you know, or even for another month or even for a few days. Is that something that’s important to you and your mom and your sister? Is that important to you?
RECOMMENDED:
Peter: Yeah, yeah, absolutely. I mean, life is, you know.
Patrik: Right, right. So, you know, and then on that end, you know, that’s, that’s a valid and reasonable argument. You know, if your mom is willing to go through whatever she’s going through, then that’s a reasonable argument. It’s not for them to put any judgment on. It’s not, for me it would be any judgment.
Peter: It’s tough.
Patrik: Oh, it is tough.
Peter: Yeah. So I mean, okay,
Patrik: What’s standing, what’s standing in the way of them doing a CT scan?
Peter: Or they just, they just, they just did. The doctor came this morning and said they’re going to do on the one know the doctor last night was, wasn’t trying to do one and then the doctor this morning too. We’ll do one. No
Patrik: Good. Good. They need to follow your wishes. I mean, or your mom’s wishes, you know. And if for whatever reason she hasn’t, she had enough. Fair enough. But she’s not at that point.
Peter: Yeah.
Patrik: You said your mom believes in a sort of like a last-minute turnaround, she believes in miracles. Is that accurate?
Peter: Yes, that is accurate.
Patrik: Okay. And again, if that’s the case, it’s not good or bad, it just is.
Peter: But they said they were, they said they were going to, I’m thinking they’re trying to get ethics and rules.
Patrik: Oh, I see. Yeah, yeah.
Peter: Oh that would give us the medical facts. Someone on their team who gives us all the medical facts. If we can’t make a decision and say, look, based on all the clinical data your mom’s not gonna ever recover. So it’s in our best interest too. Is that a meeting that I can decide not to attend?
RECOMMENDED:
Patrik: Very much? You know, it’s for you to decide what’s ethical. It’s not for them to decide what’s ethical. Look, Peter, I can’t tell you I have seen so many over the years, so many quote-unquote ethics meetings. They were all designed to empty ICU beds, right? Well, what’s ethical for them is not ethical for you. Most of the time and vice versa. Ethics in a hospital is designed to manage a hospital, it’s not designed to be ethical from my perspective. They will argue that it’s not ethical to continue treating your mom. That’s what they will argue. Right? But again, that’s not for them to decide.
Patrik: If your mom wants to have everything done, then they need to respect that. Your mom can make up her own mind. Why would they have a meeting potentially behind your mom’s back and decide what’s best for her or what they think is best for her? If your mom wants to have everything done, it’s not for them to judge.
Peter: Ok.
Patrik: Is it important for you and your mom to go potentially go with you with her head held high and sort of, you know, if your mom was to die, if she can say to herself and you as a family can say to yourself, Hey, you know, she didn’t survive but we try to everything we could. Is that important to you?
Peter: Absolutely.
Patrik: Right. And that is something you need to mention to them, but don’t worry about what they say or if it was my mom, it’s not their mom.
Peter: Oh man. Cancer, cancer, cancer. It’s tough.
Patrik: How old? How old is your mom? 64
Peter: 63 yeah. 63, 64 she’s not, you know, she’s still young. I mean that’s just cancer. No, at this point I’m even confused. I don’t even know, but it’s, I guess it sounds like a decision. I need to get my siblings and see. Right now she’s swollen a lot. Her kidneys are not working. Well they say her creatinine is high. But what number does the creatinine need to be to know that her kidneys are in failure?
Patrik: Probably sort of 150. 150 and more.
Peter: No, you’re saying it has to be 150 as a one? As a number one. So that’s like, yes.
Patrik: That could be the urea, not the creatinine.
Peter: So 2 sounds like it’s very small compared to 150 though.
Patrik: Yes. Yeah. But if it’s 2, they’re referring probably to the urea and not to the creatinine. There’s 2 kidney markers, one of them is urea and one of them is creatinine. The creatinine is, as I said, sort of above 150 sorts of that’s when the kidneys start to fail and urea is sort of above 12 when the kidneys start to fail.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Peter: Sorry, go ahead. I apologize for interrupting you. So go ahead.
Patrik: Yeah, no, no, that’s okay. And sometimes what could happen as well, let’s just say if creatinine is 2 indeed it would be a different scale. What it means is that telling you creatinine is 2, it could be what I’m referring to is usually I think it’s milligram per deciliter or something like that. And if it’s 2, usually it’s a different scale? That’s all it is. But at the end of the day it’s the same. I would have to look it up and Google. It could be that they’re referring to 2 for creatinine.
Peter: Yeah, exactly. Something like, I’m like, if it’s two, then 150 is still far away. I don’t know.
Patrik: Yeah, they’re probably using a different scale. That’s all. 2 is probably 200 most likely. But I would have to look that up. They are telling you they are failing.
Peter: Yeah, they told me. Yeah. And her kidneys are failing because of the Creatinine number. It’s like her kidneys are starting to fail, but they put a urinary catheter in her to see if she’ll pee out stuff.
Patrik: And if she’s not peeing, they’re probably giving her Furosemide and if that’s not working then they would consider most likely the dialysis. Now with going into ICU, has she had an arterial line or a central line? Do you know?
Peter: Yeah. I think she has a central line that causes she was on some like different antibiotics before she got here. So she has a central line?
Patrik: Right. Okay. I think if, if what we spoke about is important for you and your mom, then you know, don’t go into any ethics committee. You can brush them off. I mean the reality is, you know, as soon as ethics gets involved, you know, they’ll probably try and walk all over you.
Peter: Right.
Patrik: Okay. Who is the main decision maker there at the moment?
Peter: Yeah. From the hospital or from the family.
Patrik: Yeah, yeah. From the hospital.
RECOMMENDED:
Peter: Just the attending physician last night, he was an Indian guy. He was the attending physician. Very nice, well-spoken. This ICU environment is more or less pressure than the other ones we’ve been in. This ones seem more calm. They’re like, you know, it not as intense as the other ones we’ve been in.
Patrik: Why did you not go back to one of the other ones there was no bed?
Peter: The reason why was because I don’t believe there had a bed at the time, you know, so we just went to where they had a bed because she was deteriorating. Yesterday, I could tell she wasn’t okay. Looking at her face, it was like she was in breathing distress. Her face got fatter. You can tell she was uncomfortable yesterday. I don’t know too many fluids in her. I don’t know if that’s one of the reasons too.
Patrik: There’s a chance she has too many fluids on board because of the kidneys failing. And then if she’s ventilated and she has too many fluids on board, you know, there’s a chance that her ventilation won’t improve for now.
Peter: Correct. So she will need dialysis.
Patrik: Yeah. She will most likely need dialysis to see if she’s not starting to pee with the Furosemide.
Peter: Ok.
Patrik: When are you back in the hospital?
Peter: I’ll be there in the next hour or two hours. Next few hours I’ll be there maybe two to three hours or maybe even an hour.
Patrik: Right, right. Okay. The other thing that I, you know, I have been asking a few times about the DNR, the do not resuscitate, do not agree to that.
Peter: Oh no. She’s a full code. No, no.
Patrik: Yeah, I know. I know. But what I do know is with what you’ve shared, they will keep pushing for that.
Peter: Yes.
Patrik: Just to be prepared. That’s all.
Peter: I appreciate that. Yeah. It’s, I mean, I don’t know. It’s tough.
Patrik: It is. Yeah. That’s okay.
Peter: It’s, I mean, you know, I guess I’ll just keep doing what she wants and you know, if the family feels like, you know, we don’t want to continue, then we just have to probably pull the plug. But right now it’s just probably dialysis and I’m hoping her kidneys and then people who go into kidney failure and would the kidney comes about working again?
RECOMMENDED:
Patrik: Oh, it does. Absolutely. The kidney is the most forgiving organ. Well, if there’s an organ that recovers, it’s the kidneys first, liver as second, lungs third, heart fourth, brain fifth.
Peter: Her lungs are good yesterday. He’s like, oh, I don’t have an issue. And then, he said, you know, I don’t want to do a CT scan because you know, if I do a CT scan, then I heard a medicine. If they do something, you have to obligate it to treat the findings. Kind of like, it’s like pretty much saying if I do a CT scan and I see findings, then I got to go treat what I find. And he’s like, I don’t want to go there. You know that’s, that’s, that’s pretty much what he was trying to say yesterday.
Patrik: Yeah. And how long has she been in the ICU environment now?
Peter: Oh, just yesterday was when I messaged you is when she there, you know, we were waiting on a bed. Okay. So she got approved by a surgical oncologist in another place called the Tennessee Medical Center, one of the biggest, you know. I’m in Tennessee, they are one of the biggest cancer centers. I was willing to see them, but the problem was the waiting time. So we couldn’t wait any longer. So we had to go to another hospital system, like a sister hospital in a different location. That’s why we went to this place in Brownsville. And they seem like a big facility. Can I request a surgical oncologist at this point because, or that would be too much or that would be pushing too much?
RECOMMENDED:
Patrik: Well, I think you need a surgical oncologist consult. I think you need that opinion from that person. Definitely need that opinion. Especially if they’re doing a CT scan, that surgical oncologist has a time and a place at least for a consult.
Peter: Ok.
Patrik: Does that make sense?
Peter: Yes. For consult. Okay.
Patrik: Yeah. And, then he can give you his opinion. Right. And then you can see where it leads you. But, somebody like that has a role to play that, you know, it would be like, you know, God forbid if your mom had a heart attack, it would require a cardiologist consult.
Peter: Yes. But right now the only general doctors are treating her. No oncologist has come, no surgical. But someone as not really comfortable look at her because I think she’s so malnourished. They’re scared that if she does surgery, she might not wake up. So I was thinking surgical oncologist to see, is the tumor removable, is it possible at this point or not?
Patrik: That could be, but sometimes the surgical oncologist, you know, let’s just say your mom has bowel obstruction, which it sounds like she may have, you know, if she has bowel obstruction from cancer and she has potentially stool coming out of her Nasogastric tube or whatever, she needs to have surgery and in that instance, it’s probably not about, is the tumor removable or curable? It’s about relieving the symptoms. Right. So I don’t think that a surgical oncologist would come to you or your family would say, “Hey, I can cure your mom”.
Peter: Right.
Patrik: It’s not, it could be just symptom management. Does that make sense?
Peter: Yes, I see what you’re saying. Yes.
Patrik: So, you know, sometimes there are the things happening in a situation like that you can’t cure, but at least you could manage or treat the symptoms and that will require the discussion from, with the specialist.
Peter: Okay. Alright.
Patrik: Okay. It’s, it’s difficult. It’s tough. I know, but if that’s what your mom wants and if you think she’s not, you know, if she comes to the point where she’s really suffering, you know, maybe you will change course then, but it sounds to me like it’s probably not quite there yet.
RECOMMENDED:
Peter: Yeah, it’s not quite there yet and that’s where I’m at. If I feel like she’s too much, too much, cause right now she’s, and then yes, I’ll probably just let her go. The family let her go, but for right now, yeah.
Patrik: Yeah. Let, let me know what you need next. Let me know if you want me to talk to the doctors. Just hit me up.
Peter: I will. I will. Thank you so much man. I appreciate it. Very welcome. You’re very welcome. All the best for now.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!