Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
When will my Dad Wake up from an Induced Coma if He is Heavily Sedated in the ICU?
You can check out last week’s question by clicking on the link here.
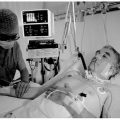
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Eric, as part of my 1:1 consulting and advocacy service! Eric’s dad is with a breathing tube and is on a ventilator. Eric is asking why the ICU team is limiting their treatment to his dad in the ICU.
The ICU Team Does Not want My Dad to Have Dialysis. Why Are they Limiting their Treatment To My Dad?
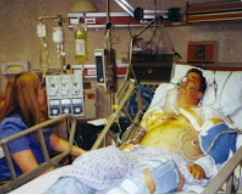
Eric: Yeah, it’s… Yeah. I think people are getting stressed out. And I think as well, with the vaccines, just that they start making outlandish to all the staff.
Patrik: Oh, it’s the same here.
Eric: They all want it as well. They’ll end up losing more people.
Patrik: They’ll end up losing more people. They mandated the vaccine here, for healthcare workers, and the industry is losing people, because not everybody wants to get vaccinated.
Eric: Yeah. It’s like an eye-opener. Now I’ve got COVID, I think I should have the antibodies, really, now.
Patrik: You should have, yeah.
Eric: Do you think it’s worth having the antibody tests done?
Patrik: I think its worth, for you, having the antibody tests done. I mean, I am not in the business of telling people whether they should or shouldn’t have the vaccine. I had the vaccine.
RECOMMENDED:
Eric: No, it’s freedom of choice.
Patrik: Freedom of choice. I had the vaccine myself, but I had it forced upon me, because obviously I’ve got businesses in healthcare. And I still have frontline contact with clients here. And I could have more or less closed my business down if I hadn’t been vaccinated, but I didn’t feel good about taking the vaccine. I would have taken the vaccine in my own time, but not being forced from the government. But that’s what I ended up doing. That doesn’t feel right.
Eric: Yeah. I know you have…
Patrik: Doesn’t feel right.
Eric: And they’re wanting to mandate it all.
Patrik: I think they’re trying to implement the mandates all over the world, really. And I strongly disagree with that. Strongly.
Eric: Yeah. I do. It’s scary. It’s all about control, isn’t it?
Patrik: All about control. Because what’s next? You know? What’s next?
Eric: Yeah.
Patrik: If they force people to vaccinate, what’s next?
Eric: Yeah.
Patrik: People need to wake up. If someone wants to take the vaccine, go for your life. I have no problem with people taking the vaccine. I do have a problem with the government trying to mandate it. That’s what I have a problem with.
Recommended:
Eric: Yeah.
Patrik: That’s right.
Eric: It’s like..
Patrik: That’s right. And what are we not counting? We’re counting COVID, and what are we not counting? Mental health. And businesses being closed, and the list goes on.
Eric: Yeah.
Patrik: It’s, look, I don’t know about the UK, but what I can see in Europe… and I’ve got family in Germany. And people are going on the streets, going to the streets, and here, as well. There’s big protests, here, and it’s time. It’s time. This madness needs to stop.
Eric: Yes. It is. And that thing that reminds me of dad, because he was really like me. He really agreed on what you’re right saying, Patrik. But, I mean, they say this is COVID, but dad probably would might have got that pneumonia anyway, without the COVID.
Patrik: Exactly. You know? This is… people get sick whether there’s COVID or there’s no COVID. Your dad might have had a pneumonia, and he may have been asymptomatic from COVID. Your dad might have had a genuine pneumonia, irrespective of whether he had COVID or not.
Suggested links:
Eric: Yeah. And I think that, because I mean, even my dad, when he got sick and it’s so hard now to get a doctor. And also, they only get you into hospital now if you’ve got breathing difficulties.
Patrik: It’s very difficult. Very difficult times. But it’ll sort itself out. But, look, what we can do, Eric… I need to go in a couple of minutes. What we can do next, let me know when you want to talk next. We can do the same. I actually do believe nighttime or evening time might actually be better than daytime, because it’s usually less busy. Also, sort of the events from the day have passed, and it’s almost better to have a summary of the event from the days. If we called them in the morning, A. they are busy…
Eric: Yeah. They are sure busy, yeah. Because the doctors are going around, and they’re trying to clean them and give them breakfast, and…
Patrik: Exactly.
Eric: But I know, not on these people also.
Patrik: Exactly. And if we do it at nighttime, the day has passed, they can summarize what’s happened during the day. I think it’s much better.
Eric: Yes. Definitely. And I know that, if they’ve got anything to tell me, they’d ring me up anyway.
Patrik: Exactly.
Eric: So, if anything’s important…
Patrik: Exactly.
Eric: They’d ring me in the daytime. Yeah.
Patrik: Yeah. Exactly.
Eric: So, obviously, I’m not really, really a rich person. So that’s why, at the minute, I only get, like, an hour free.
Patrik: That’s all right. We’ll do it again tomorrow, or when you’re ready. It’s fine. We’ve only used half an hour. It’s all good. It’s all good.
Eric: Oh, brilliant. So what should I do, Patrik? Should I ring you up? When am I best to ring you up?
Patrik: Yep.
Eric: This this time of day?
Patrik: Yeah. Just, can you text me? Just send me a text if you can.
Eric: Yeah, of course I can. Yeah.
Patrik: Just send me a text when you want to talk next.
Eric: Yeah.
Patrik: Yep.
Eric: Yeah. Oh, thank you. Yeah. You’ve been really helpful, and you’ve brought me into the picture again.
Patrik: Yep, all good.
Eric: It could go anywhere for my dad at the minute, really.
Patrik: Yeah. Okay. That’s good, that’s good. Okay, Eric, I need to run. Let me know.
Eric: Yeah, thank you.
Patrik: Let me know when you want to talk next. Thank you so much.
Eric: Yeah. Thank you, Patrik. Bye.
Patrik: Thank you. Bye. Bye.
Recommended:
Patrik: Hi Eric. How’s your dad?
Eric: He’s deteriorating according to them.
Patrik: Right.
Eric: And they said the kidneys are struggling now as well.
Patrik: Right.
Eric: So, they keep saying that he’s deteriorated. But they’ve been good, they’ve let us see him and then they’ve let us to go again to say night-night. They say his kidneys, they’re like to a degree where things are not getting any better. And they said as well about the kidney dialysis, they said if he needs it back but because of his illness it’s going to be too cruel for him.
Patrik: Right.
Eric: So…
Patrik: Look, okay… So, he’s now on a 100% of oxygen?
Eric: Yes.
Patrik: Did they tell you why they think that’s happened?
Eric: They keep saying that he’s deteriorated and he’s extremely weak now.
Patrik: Yeah.
Eric: And, they are being negative about our dad’s condition now. And they’re telling something about, it could be over night or it could be a week.
Patrik: Right. What else are they saying anything else, is anything else happening in terms of..
Eric: They’re talking about the ECMO. But they have a concern about his age. They have tried it to the same other patients before. They don’t recommend it. They said it made them deteriorate more.
Patrik: Look ECMO has saved many lives and continues to save many lives. What I will say is I have not seen many patients go on ECMO above the age of 65 that all. But that is not because they can’t have or tolerate ECMO. It’s usually that there is an age cut off unfortunately. They usually make ECMO available for younger patients.
Eric: Yeah
Patrik: Right, so they may not be wanting to tell you that straight forward, but that is most likely the reason why they are staying away from ECMO. Is he being proned?
Recommended:
Eric: No, they don’t seem to be doing that, they said it didn’t work. He’s laid on his back.
Patrik: When they say, it doesn’t work, I mean I do remember what the nurse told us. Have they been more specific why it doesn’t work?
Eric: No, not really. I think because of the feeding tube, there’s a problem with it or…
Patrik: I’ll tell you the reasons why it may not work. It may not work because he becomes too unstable. His blood pressure might be jumping up and, might be jumping down if anything, probably not up. Blood pressure might go down to a point where they think its life threatening. It might be..
Eric: Yeah, I think the Doc told me that problem is partly blood pressure, it’s been so low.
Patrik: Right, so that could be one of the reasons. I’m just trying to think what else. Feeding, they can stop the feeding.
Eric: They said they’re still feeding him. We’ve noticed he’s had his urine back. So, I think they’ve been giving him the fluids and the food.
Patrik: Look, I’ll tell you what I have a problem with. The dialysis, unless they’re trying to do it, who knows whether he can tolerate it or not. Do you know, is his blood pressure still low?
Eric: It’s still very low.
Patrik: Right, look, I’ll tell you what I’m thinking. They can be very quick in being negative and I’m not… Some of the things might be happening what they’re saying, but the reality is this, if you’re not trying dialysis. You’re not going to improve the kidneys, if the kidneys are failing. Now, his blood pressure might be low to a point where he can’t have dialysis, I get that but then that’s sort of why I’m wondering what is his blood pressure like.
Recommended:
Eric: Yeah, I think actually tonight they’re going to let me ring them up, do you want to do a talk with them?
Patrik: I think so, I think that might be the best way to go about it, get a little bit more information from them.
Eric: Would you talk with the nurse tonight?
Patrik: I would be very happy to do that. You see, here is my take on CPR, Eric. Yes, CPR is not a nice thing, of course it’s not a nice thing. However, if someone dies, they’re dead. And they will tell you all about, for someone to revive from cardiac arrest, you’ve got to crack the ribs. They give you all this talk. But, the question is, do you want to save a life or do you want to focus on the negatives? Do you want to focus on the negatives of saving a life or do you want to focus on the positives of not saving a life?
Eric: Yeah.
Patrik: Right, I..
Eric: Yeah, I fully get what you mean.
Patrik: Right, and from their end, they’re saying, “It wouldn’t be in the best interest of your dad to crack his ribs.” I know the terminology bends. Okay, I’ll take that as a statement. Okay, but once he’s dead, what’s there…? There’s nothing left. And for them, it’s about saving money, it’s about saving staff, it’s about saving beds. And I understand, I’m just opposed to hospitals and ICUs constantly saying, “Oh, it’s not in the best interest of a patient to live.”
Eric: Yeah.
Patrik: That to me is insanity. I’m not saying pay every price for someone to live. But look, it’s not… As far as I’m concerned, it’s not black and white.
Suggested links:
Eric: Yeah
Patrik: It’s not black and white, it’s not as simple as, “Oh, we won’t crack the ribs, therefore, it’s in the best interest of your dad.” I just don’t… Do you want, as a next step, do you want us to talk to the nurse again?
Eric: Yeah, if you phone.. We scheduled for 9 in the morning.
Patrik: Or we can call them later it doesn’t have to be now, you’ll let me know. They’re handing over now aren’t they?
Eric: Yeah, yes they are because we just called up the hospital.
Patrik: Let’s do that.
Eric: Okay.
Patrik: When do you want to do that, when is a good time?
Eric: I’m going to say 9 in the morning. So do you think..
Patrik: 9 in the morning.
Eric: Alright.
RECOMMENDED:
Patrik: I’ll call you then.
Eric: Yeah, that’d be lovely, thank you. Bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!