Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Iyah, as part of my 1:1 consulting and advocacy service! Iyah’s dad is in the ICU and on a ventilator. Iyah is asking if it is possible to wean her dad off the ventilator and avoid a tracheostomy.
Is it Possible to Wean My Dad Off the Ventilator and Avoid a Tracheostomy in the ICU?
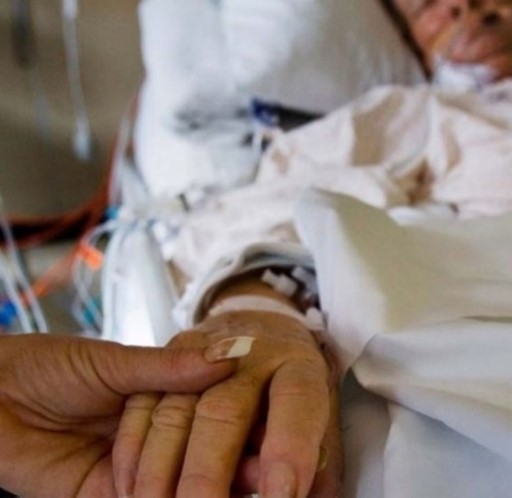
You can also check out previous 1:1 consulting and advocacy sessions with me and Iyah here.
Dr. Shelby: So in the big picture, there are kinds of three paths to care that we have in medicine I want to just kind of address in brief terms. The first path is what we call care to prolong life kind at all costs. So in this path, it’s what we call full care sometimes euphemistically and it means that all our energy is geared with keeping someone alive no matter what the burden is to them in terms of quality of life or suffering or whatever they’re being put through.
That’s kind of the standard of care people have for most of their life. If you’re in the hospital right now, you’d have that for your care and right now that’s what your dad is getting too. So that means that all the care he’s getting, being on a ventilator, having the meds to raise his blood pressure, antibiotics, IV (Intravenous) fluids, dialysis, feeding tubes, all those things with the goal of helping him recover, get stronger and live longer.
RECOMMENDED:
It also means that if he got worse and actually if he even passed away here in the hospital, it means that they would do CPR (Cardio Pulmonary Resuscitation), which means chest compressions, shocking in the heart and he’s already intubated, to try to bring him back to life if he passed away, which can work sometimes, but if someone’s really ill and despite maximum care they die, need CPR, the odds of them surviving and recovering gets very, very low. Whereas the odds of them surviving by maybe having some brain damage or having several broken ribs or having a long-term disability in a long-term care facility goes up a lot if they do survive. But that’s the care path he’s on the moment, that’s kind of the default.
There’s another path we call selective care. And on that pathway, the goal is still to try to prolong and preserve life but it’s also trying to balance that with helping to maximize quality of life.
So a little bit more of a balancing act, which can be tough. And for that pathway, there’s more flexibility for choices. So someone may say I don’t mind or I accept being on a ventilator or I accept doing dialysis, but I wouldn’t want A, B, or C interventions. I wouldn’t want a massive surgery or I wouldn’t want to do CPR if I was dead. If I was dead just let me be dead don’t try to bring me back.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
So, it allows someone to have a little bit more flexibility to say what things they accept, what things they don’t to try to not put them through horrible suffering if there’s little help of actually benefiting them.
The third path is what we call comfort-focused care. And on that path someone says, I’m extremely ill, I know my time could be very limited and I want to focus all my attention on maximizing comfort and not doing things that cause discomfort or suffering of any kind.
And on that path usually, we would not do things like dialysis or ventilator or keep those things going. We would mostly do medications to maximize comfort, to eat as desired and to allow time with family if someone’s near the end of life.
Right now your dad has set us on the first path, the life-prolonging path. I think that’s a reasonable path. I think also, given how sick he’s been, I do worry about putting someone like his position through CPR. If he got so sick, despite the care he’s getting that he actually died, I worry that putting him through CPR would have very low chance of him coming back and being awake and alert in a way that most people would find acceptable to quality of life.
Again, there are lots of unknowns here, but I think it’s something that’s worth considering as a family to think about from talks you’ve had with him, what you think he might find acceptable in terms of if he survived but could no longer ever get out of bed again, would he find that acceptable quality of life or not? And those are really tough things to consider.
No one knows the answer except him and you guys know him a lot better than we do, so we turn to you to try to act as his advocates to think about what you think he would say if he could be here with us right now and seeing the position that he’s in, which is hard, but I think those two paths would make the most sense are both very reasonable.
Liza: And from my understanding, he isn’t really able to speak or make up his own decisions mainly because he’s on the bench to take him through the sedation and the medications are suppressing his body and consciousness. Is that correct?
Suggested Links:
Ron: Yes and no. It’s two things. It is that and he also has some encephalopathy from being septic, from being a little on the toxic side with his kidneys not cleaning the toxins out. So when he’s completely off sedation and wide awake, he does not follow commands. So I believe-
Liza: He usually doesn’t follow commands. That’s normal of him.
Iyah: But then again his brain is cloudy right now too so he can’t even comprehend really.
Iyah: That’s what he’s saying that there’s some delirium.
Ron: I’m saying encephalopathy is delirious.
Iyah: I didn’t know that.
Ron: Yeah. I’ve rarely had a person not follow commands in a hospital because they simply aren’t going to cooperate, stubbornness kind of thing. Because when a person is coherent, when they’re there, when they are aware of their surrounding they would cooperate with medical staff to help get better. But with him and encephalopathy-
Liza: Is it a logical concern or a brain concern or-
Ron: It’s not like the brain is damaged, it’s like the infection has affected the brain. So it is like a swelling and the toxicity can cause your brain not to function well. So it’s not like he has brain damage that we’re completely aware of but this is very common to have encephalopathy.
Iyah: While being on a ventilator?
Dr. Shelby: No, just from being sick and from being on meds like heavy sedation.
Ron: It’s not because of the ventilator, it’s from being that sick.
Dr. Shelby: It’s being in the hospital and being on the meds.
Liza: Right. So there’s a chance that this can improve, correct?
Dr. Shelby: Absolutely.
Liza: Okay. That’s good to know.
Dr. Shelby: It can take days or weeks or months in some cases. So it’s hard to put a call on how fast it improves but generally, if someone gets off a ventilator and they’re recovering, usually within days to weeks their mental status improves a fair amount for the most part.
Ann: This is why this discussion about whether we’re doing tracheostomy because we can’t continue to leave that breathing tube going down his throat through his vocal cords.
Liza: Well what is the timeframe if it is so urgent that we can’t continue anymore when I heard earlier is, within one week from now we can start breathing trials right now and within one week or two weeks then that is the timeframe where we have to start doing that.
Dr. Shelby: What have you heard from the ICU, doctors?
Ann: Now that he’s on 40%, which we just got this morning, we’ll be able to start trying. They’re usually not successful until the patient can start following commands because if they can’t follow commands they can’t get encouraged to calm their own breathing down with me sitting there explaining to them I know how you feel-
Dr. Shelby: Trying to coach them.
Ann: Yeah and coach them into relaxing.
Dr. Shelby: So do you have a sense of how long until the extra doctors are putting pressure on to make a decision?
Ann: I’m going to actually contact him and see if he wants me to do one this afternoon. The dialysis lady was going to go upstairs and do her patient and then come back down here so we could do one, I can go turn off the sedation again and we can do one and then do another one tomorrow.
Gel: Yeah, while we’re here in the room with him.
Ann: Yeah. I suspect he’ll fail very quickly but it’s common to fail very quickly the first couple of times anyway, but we just start the whole process.
Iyah: Could you please elaborate on what that all entails with the breathing trial?
Ron: Breathing trials are when we actually turn off sedation because sedation will suppress respirations, which is the in and out, that’s all respirations are it’s getting air in-
Iyah: How long does it usually take for the respiration to start coming back?
Ron: As soon as he’s awake from the sedation being off. All you got to do is-
Iyah: But everyone’s a little different, right? It may take them a little longer.
Ron: Right. But most of the meds we have-
He’s on meds that will take him a little longer. It took him over two hours to wake up.
Iyah: I’d just like to know, would you turn off the sedation and then wait an hour or wait half an hour?
Suggested Links:
Ron: Yeah, we wait until I know he’s awake. If he was on Propofol it’s two and a half to five minutes, but he’s on Precedex and he’s on Versed, so it’s going to be a couple of hours. I would turn it off for a couple of hours then they take the ventilator settings and put them on CPAP (Continuous Positive Airway Pressure) and see if they can oxygenate.
If he starts breathing over 30, that’s a fail. If his heart rate starts going up into the high 100’s, 130’s and above. That’s a fail and it’s likely that he’ll do that the first couple of times.
Liza: I believe I read that some of the sedation can last up to six hours, is that right?
Ron: Yeah, some can and it really depends on each person and people who have more girth on them can take even a couple of days. He wakes up for me within two hours.
Iyah: That’s good
Ron: He did this morning.
Iyah: How does he wake up for you? Is it-
Ron: He’s right wide awake and you can tell by the way he’s breathing and by the way his heart rate’s a little higher-
Dr. Shelby: Yeah.
Ron: Yeah.
Liza: What I would like to address is, maybe starting the breathing trials a little bit later, waiting longer, a couple of days, six hours to a couple of days because I’m concerned that the testing timeframe may be too early. Because my dad is very weak.
Ron: We don’t have a lot of time before we make a decision for a trache. You’re already over the two-week limit.
Liza: So just that I would like it to just give him a lot more time than the usual.
Dr. Shelby: No, the more time we give, that means we have less time to actually help him get better before we have to do a tracheostomy. So, we’re into that deadline, no matter what.
Ann: We’re in a deadline.
Dr. Shelby: Because they won’t let him linger for a month on the bench, because there’s such a high risk of him getting-
Liza: Giving him more time, I don’t believe it would be extended out damage further.
Ron: What do you consider more time?
Liza: Say if you wait one hour, wait three hours, instead of all on the same day.
My concern is that if you test him too early, he’s going to fail. But if you test him later on-
Ron: I see what you’re saying. You mean don’t change the vent settings yet?
Liza: Yes.
Ron: Yeah. So-
Liza: I’m concerned that you’re going to test him and fail him-
Ron: Right. That’s perfectly reasonable. I’d be happy to wait three hours, but I do want you to be aware-
Liza: With one of our siblings there, because it would cause him more comfort because he’s not comfortable with strangers- `
Ron: Liza, let me tell you, he’s going to fail the first couple of times.
Liza: I understand.
Ron: Today his respirations were in the 40’s…
Patrik: Can you see the notes?
Iyah: I have not checked, but I will.
Ann: His heart rate was in the 160s, and his pressure was going up to 200.
Ron: And that’s even before-
Patrik: I would do that now, Iyah.
Ron: that even the vent. That’s considered a fail. You understand?
Liza: Can you repeat that?
Suggested Links:
Ron: Yeah. When he hits, by the time he hits the three-hour mark of no sedation, his respirations were over 40 a minute, his heart rate was over 160 a minute and his blood pressure was climbing up to 90 to 200. That would be considered a fail, even before we turned the vent to the CPAP mode, he had to be able to breathe less than 30. So we try anyway even though we know they’re going to fail because we got to keep giving them a chance and every time we do it, it helps their lungs exercise.
Liza: Right. And so the failing, is it from the heart or lungs, or where’s it coming from?
Ron: From all of it. It’s all interrelated. The whole person, it’s all interrelated.
Dr. Shelby: Liza, these are very valid concerns and I want you to, hopefully, trust that this ICU team, they do these all the time here in the ICU. They’re constantly dealing with spontaneous breathing trials and dealing with ventilators and get people off of ventilators. So they do this all the time. They have the protocols in place and they adjust them and tailor them to individual needs. So he’s in good hands in terms of giving his the best shot of getting off the ventilator and hopefully avoiding having to go through a surgery for the tracheostomy and PEG (Percutaneous Endoscopic Gastrostomy) too.
Iyah: May I ask how frequent these trials may be? Once a day, daily in the morning?
Ron: Yeah.
Iyah: Is that when they may be more alert?
Ron: Sometimes keep them in the afternoon, all depends on how the units function.
Iyah: I do want to add that my dad’s sleep schedule is off, his body being awake is usually around late afternoon.
Ann: Well, most of our patients are. They don’t get to see the sun come up and go down. It’s something we deal with later, after we get them more well. It is just expected.
Dr. Shelby: So let me ask you guys, since you’re all here right now, if a week or whatever time goes by that I see doctors allow and he’s not showing signs of doing well with the breathing trials, what are you guys’ thoughts about doing the tracheostomy and the feeding tube? Just to kind of get a sense, not at a decision, but just a sense of where you guys’ minds are at.
Liza: Yeah, that would be the next step for me. I ultimately want him to be off the ventilator and avoid the tracheostomy if he can, but if not, then go that route so then he can at least regain his consciousness and whatnot. So that would be my next route.
Iyah: I agree, but with the tracheostomy, I would prefer to try the nasal feeding tube rather than the stomach feeding tube right away because the stomach feeding tube is going to make it permanent.
Suggested Links:
Ann: He already has the nasal feeding tube.
Iyah: Correct. So I would want not to do the PEG.
Ann: What are you uncomfortable with the PEG (Percutaneous Endoscopic Gastrostomy Tube) about?
Iyah: Because that would make it permanent.
Ann: No, it’s not permanent.
Iyah: We have to send her to a long-term care.
Ann: It’s not permanent.
Dr. Shelby: They can both be temporary.
Iyah: They can both be temporary.
Dr. Shelby: Yeah, they both could be either permanent or temporary.
Iyah: But one seems a little more invasive than the other.
Dr. Shelby: One’s a hole in the neck and one’s a hole in the stomach. They’re both fairly invasive.
Ann: Yeah.
RECOMMENDED:
Liza: It’s all temporary, Iyah.
Ron: It’s where we’re at with him.
Ann: It is where we’re at. Even if he has a tube in his nose, if he is stable, like his blood pressure has stayed stable, he’s tolerating the dialysis, we won’t have a choice but to send him to another facility.
Iyah: From my understanding with a nasal feeding tube, he wouldn’t need to stay in ICU.
Ron: No.
Iyah: But with a PEG feeding tube he would’ve to be sent to a long-term care facility.
Ron: That’s not true. It has to do with his body being stable. Is his blood pressure stable? Can he tolerate being on dialysis?
Dr. Shelby: We’ve had patients at home with both kinds of tubes before. It just depends on the situation. But what’s keeping him in the hospital right now is being on the ventilator and the dialysis for the time being.
Iyah: That’s all I got.
Ron: And just because he’s stable enough to go to a facility, it stitakes days to get it arranged.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!