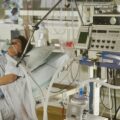
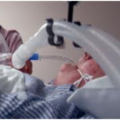
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Iyah, as part of my 1:1 consulting and advocacy service! Iyah’s dad is in the ICU, on a ventilator and she wants her dad’s condition to improve in the ICU but the doctor says he will need long-term dialysis.
I Want My Dad’s Condition to Improve in the ICU, But the Doctor Says He Will Need Long-Term Dialysis. Help!
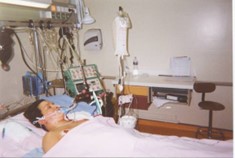
You can also check out previous 1:1 consulting and advocacy sessions with me and Iyah here.
Nurse Ron: It’s the same. We’re up against the exact same problem as the trach through the throat. The tube through the throat, the tube in the nose and down through the throat is at risk of rubbing, making a little infection there, making huge open holes, sores, infections. So, we have to get them out and put them in an area that has stronger walls to hold and not get wounds rubbed into them. So, in the stomach, that’s used to having acid in there, it’s not going to make this big, huge abscess as easily as something, a tube down through your nose. So that’s why they always put a trach and a feeding tube in the same surgery. You want to get everything out of here.
Iyah: Out of the nose.
Nurse Ron: … out of the nose and out of the mouth. Yes.
Dr. Shelby: People who are on a ventilator are usually already on a feeding tube for a few weeks as well. So those things are lined up time-wise. So, they do them at the same time, because that way, if they need long-term, they’re there. If they come out in a few weeks, they take them out in a few weeks. And they both can come out. But that would be the next step, that if he is still on a ventilator a week later, from now, he probably would end up getting a tracheostomy and PEG (Percutaneous Gastrostomy Tube) if that was the path that everyone wanted to go down for his care.
Patrik: Dr. Shelby, with all due respect, I mean, you don’t even know what ventilator settings he’s on. What if he’s breathing on CPAP (Continuous Positive Airway Pressure) at the moment, or on pressure support? He might be able to-
Ron: He is not on CPAP.
RECOMMENDED:
Patrik: Can I just finish please? He might be able to avoid the trach. I think it’s critically important that you evaluate in this meeting on his ventilator settings.
Dr. Shelby: He is not on CPAP.
Patrik: Okay. And is he still on sedation?
Dr. Shelby: Yes.
Patrik: How much sedation is he on? I mean, if sedation is being weaned, is it realistic for him to go into pressure support? I think those are all questions that are important in this context.
Ron: When I turned off his sedation, he made it over two hours before his heart rate and his blood pressure and his respiration shot up, which was good. And then I turned his sedations back on at half the strength they were, his PRECEDEX is at 0.7 micrograms per kilogram per hour, and his Versed is on at 1.2 micrograms per hour.
Patrik: Okay. Okay. And is he also on any opiates? Is he on Fentanyl, or is he on morphine?
Ron: He gets Fentanyl? He gets fentanyl in a PRN (if necessary) situation. If he looks like he’s in pain, he gets Fentanyl.
Patrik: I see. I see. So basically, no spontaneous breathing trials have taken place at this point.
Ron: We can start those because he’s now down to 40%.
Patrik: Right. So-
Iyah: Excellent.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Ron: And his PEEP (Positive End Expiratory Pressure) is now at eight. His PEEP was at 10 or higher until this morning.
Patrik: Right. Okay. Right. But to this point, no spontaneous breathing trials have taken place.
Dr. Shelby: Correct.
Patrik: Right. Okay. That’s… Yeah. Sure. Thank you.
Dr. Shelby: Yeah.
Ron: No, I’m sure they’ve done a few, and he didn’t pass.
Dr. Shelby: Oh, they may have done some, but-
Ron: Yeah.
Dr. Shelby: So if he stays on the ventilator for another week and is unable to get off, then there’s a decision of whether to do the tracheostomy and PEG tube or not. And if they do the trach and PEG, then he’ll go on to an acute care facility after leaving the hospital. They’ll continue the treatments, hopefully, trying to wean him down, if possible, and then kind of go from there and reassess.
If, however, he declines further where he still needs to be on pressure, or they need to be restarted because his pressure drops again, or he’s unable to tolerate dialysis, then we get into a really tricky situation. We run out of options of things to do.
Iyah: Pressure, are you talking about oxygen pressure-
Dr. Shelby: Blood pressure.
Iyah: … or blood pressure?
Dr. Shelby: Blood pressure. So if that comes down again or he gets worsening signs of infection, then it gets harder and harder to treat what we’re already trying to treat.
Iyah: What level of blood pressure you’re talking about, that’s low?
Dr. Shelby: So like eighties over fifties. When he was out there a day or two ago. He’s better today, and he actually was high for a bit, but maybe due to pain.
Iyah: Yeah, I’ve seen that.
Dr. Shelby: Yeah. The worst outcome would be that he declines further, and no matter what we do, we can’t help him, and he ends up passing away. That is the worst outcome. In terms-
Liza: I have a question. So the condition of him not improving within one week and starting the breathing trials, would it help to include more medications, such as Quinine and Zinc? Because you’re only giving him antibiotics. I’m not sure if that takes care of everything that needs to be addressed with the infection.
Dr. Shelby: They’re using the treatments that are approved and part of the hospital protocols.
Liza: And what do you mean by that?
Ron: First of all, his kidneys are so bad, we’re not going to give a bunch of other meds, unless we have proof that it’s going to help. Because we can’t keep… You know what I mean? It’s not going to clear, he’s just going to become more encephalopathy and more toxic. And second of all, unfortunately, our hospitals can’t just give what they think is good for the patient. They have to follow the state-sanctioned protocols and the FDA (Food and Drug Administration) approved medications. Even if our doctor wanted to do it, he wouldn’t be allowed to do it. We have to follow the laws that are put on the hospital.
Liza: Well, is there a way that we can get a list of these approved medications, so we can see which ones we think would help the most?
Ron: Yeah, you can go on the websites.
Liza: Okay.
Ron: Yeah.
Liza: Thank you
Ron: You’re welcome.
Suggested Links:
Dr. Shelby: So I think my biggest concern is that if he survives, he may end up needing to be on long-term dialysis. And I saw on his chart, a mention of his prior statement that he had made that he would not want to be back on long-term dialysis again. Did I read that correctly?
Michael: Yes.
Iyah: Yeah. That was relayed to me. And he said, “If I had to go back on dialysis, it would kill me.” Then again, if a person’s faced with life or death, they may want to continue breathing.
Dr. Shelby: They may-
Iyah: Fight for something.
Dr. Shelby: They may or may not. So it depends.
Iyah: So it’s very subjective.
Michael: He said it to me also.
Iyah: He, what?
Michael: He has mentioned it to me also, he does not want to go back on to dialysis.
Ron: I’ve heard many people tell me, that are on dialysis, that you get your blood clean, and then you just feel really icky. When you just start to finally feel better, you have to do dialysis again. So it tends to be a very uncomfortable thing for people to have to do.
Iyah: Yeah. It was a nightmare for him when he started dialysis-
Michael: He was in for some years.
Iyah: … in the nineties.
Ron: Yeah. Yeah.
Iyah: It was the worst time of his life, yeah.
Ron: Right. Yeah. Because you never feel good. You feel icky all the time. Aches and pains and nausea and things like that.
Iyah: Yeah.
Liza: Well, there are ways where you can flush the kidneys through baking soda, water, Niacin, I believe.
Iyah: He’s already taking sodium bicarbonate.
Liza: There’s a lot of people who have had success rates, even with severe kidney disease.
Ron: He has pH issues, so we would have to be very careful with anything like baking soda, that kind of thing.
Iyah: =Well, he’s already taking sodium bicarbonate-
Ron: Correct.
Iyah: … for medicine.
Ron: Correct.
Suggested Links:
Liza: Right. But pH issues can be resolved also through diet and herbs and other types of medications. So pH is just water, level blood, so it’s a chemical mixture. So it is adjustable.
Dr. Shelby: Well, right now, we kind of have to go with the information we have. So we use the family to act as the surrogate for the patient if they can’t speak to us. So your role as his children is to act, hopefully, in unison and not to think about what you think is best for him, but what you think he would think is best for himself. And that’s really what you’re tasked with when you’re acting as his surrogate.
Liza: Well, I believe that is an immoral thing to put onto their children. I always will do everything I can to help improve him.
Iyah: I feel the same way.
Dr. Shelby: So in my understanding now you’re saying that you do not plan to follow up on his wishes, but upon your wishes for him?
Liza: No, that’s not what I’m saying. You’re not listening to what I’m saying. I’m saying that I want to do everything I can possibly do, to improve his condition.
Dr. Shelby: Right.
Ron: And we would like that as well. It does come to a point where we can’t make things better and he’s just constantly uncomfortable.
Iyah: It seems like he’s getting better though with oxygen settings being decreased from last night. So it seems like we’re having some encouraging things.
Ron: Remember I told you we seem to be doing the two steps forward one step back.
Iyah: I’m aware of that.
Ron: The thick secretions he has way more of them and now they’ve got the blood in them. So it’s a back and-
Liza: What I’m gathering is that, why are we having this conversation now, rather than one week from now, since we can start doing the breathing trials? Maybe it is because he has dropped down recently? So I would like to reschedule this meeting to one week from now and start doing breathing trials and seeing if he can get off the ventilator and just not do the-
Ron: That’s why we’re having this conversation because he’s already passed the two weeks by almost a whole week. So we’ve already stretched it very far. So therefore, we would like the family to try to come to terms with either they are going to go with letting nature take its course or put a tracheostomy in and a PEG (Percutaneous Endoscopic Gastrostomy Tube) in so that we can see if she gets better with getting more dialysis.
Liza: I would rather wait one week and have him start doing breathing trials since he is around 40.
Iyah: I agree. He is doing better now.
Dr. Shelby: So these things are not mutually exclusive. When we have this meeting, we’re not asking for all things to be decided today in one visit. We’re trying to lay out what may happen and also deal with what has happened in case of emergencies in the meantime. Because two days ago he was incredibly sicker than he was right now and that could happen again.
Iyah: When you say incredibly sicker, could you specify?
Dr. Shelby: His blood pressure was extremely low and he could not tolerate dialysis.
Iyah: Was that during dialysis or without the dialysis?
Dr. Shelby: Without dialysis?
Iyah: No I’ve seen it.
Ron: Yeah, no that was just lying in bed while-
Iyah: That was going on for two days, right? Or two or three days?
Ron: And that’s a sign of sepsis.
Suggested Links:
Liza: I’m not sure of the duration.
Iyah: I’ve noticed it quite a bit though, since last week. He also had a fever…
Ron: Yes.
Iyah:So that could’ve been a-
Dr. Shelby: So all these are concerning things that can come up. So our goal is to not wait for an emergency to happen and then try to make calls and plan, it’s to have a plan in place prior to emergencies, plans that can change based on how he does day-to-day.
Liza: Right. My concern mainly also is the foods that you are giving him. How can we improve the foods that they are giving him? We all know how important food is and he’s on a ventilator right now. So I think that is one of the most important things to look into. What options do we have in terms of what foods can we give him?
Iyah: I believe he has a dietitian following him and getting tube feeds.
Ann: Yes he does have a dietitian, he is on a diabetic source formula, getting protein and the vitamins and minerals to make sure he’s getting the nutrition to help himself heal and through.
Liza: And is there a way that we can try to do more trials to see if there are certain different formulas that will improve his condition better?
Ron: Going with trials and things you have to have the permission of the participants. He’s not able to give us permission at this time.
Liza: I know my father and he’s very picky with food and he would love for us to give that permission for him, I feel, because when I called during the first week when he was admitted, I asked the nurse specifically what was in the formula and he told me protein, sugar and nutrition and so I already know that sugar, is it white sugar? What kind of sugar is it?
Eva: It’s not the same nutrition that he’s had in the first-
Ron: He gets dextrose.
Liza: Dextrose?
Ron: Yeah.
Liza: And is that the sugar name or is that the formula?
Gab: That’s the sugar. That’s part of the formula mix that he gets.
Liza: And what is the formula name?
Gel: Diabetisource.
Liza: Diabetisol?
Ron: Source.
Liza: Source?
Ron: Correct.
Liza: And so where can I find more information on options, other options that we can give him? You know, everyone’s bodies are different and require different nutrition.
Dr. Shelby: Let me step in. Ruth, would you be able to ask the dietitian to reach out to Liza, when he’s able to, to discuss the nutrition that he’s getting in more detail?
RECOMMENDED:
Ron: Yeah.
Iyah: Well the thing with the sugar is his body needs carbohydrates still, your body needs it. Right?
Ann: I can see the bag right now so you guys can have the bag to read the ingredients.
Iyah: Diabetes wasn’t the reason why he was here and he’s here.
Ron: It all correlates together when you’re very sick, your body tends to keep your blood sugar high and we don’t want him to have all that high blood sugar. It causes damage. It is not like we’ve isolated part of his body over in one corner. It all has to work together.
Liza: I understand, whatever you’re putting in, also is most important, however.
Dr. Shelby: So we’ll have the dietitian reach out to you and hopefully be able to answer your questions a little more in depth than we’re able to.
Ann: You bet. Yeah.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!