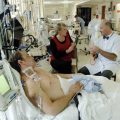
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Dad has Lung Failure in the ICU. Can We Get Him Off the Ventilator?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Iyah, as part of my 1:1 consulting and advocacy service)! Iyah and her siblings will attend the family meeting for their dad in the ICU. She is asking what to expect during the family meeting for her dad in ICU.
What To Expect During the Family Meeting for My Dad in ICU?
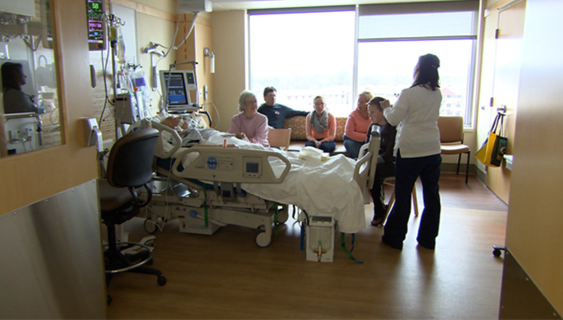
Patrik: Hello Iyah! How are you?
Iyah: Hi Patrik. I‘m good. I am here in the hospital. Do you like to call via Skype or Zoom?
Patrik: No, no. Skype is good. Skype is good for me. Hang on.
Iyah: Is it typical to have the meeting in my dad’s room? Should it be done away?
Patrik: It probably should. Who’s going to be there?
Iyah: My siblings, the nurse, and the doctor, I assume.
Patrik: Look, I don’t think it should be done in front of your dad, unless your dad is awake and can participate, but I don’t think that’s the case, is it?
Iyah: It’s not the case, no. So yeah. We need to go out.
Patrik: Because it could be very upsetting for your dad if he can hear but he actually can’t talk.
Iyah: That’s correct.
Iyah: Yeah, I will let the nurse know I prefer not to be in the room with our dad.
Patrik: Yes, I think that’s very reasonable. They should have a meeting room.
RECOMMENDED:
Iyah: So, it’s really encouraging to see him more relax now.
Patrik: Yeah, that’s good. I think from experience, Iyah, there’s many ups and downs when someone is in a situation like your dad. It’s often two steps forward, one step back, sometimes two steps forward, two steps back. So, it’s easy to jump to conclusions, but once you can see that it’s fairly unpredictable, that there’s many ups and downs, you almost will need to grow patient in this. I’m not surprised by anything that you are sharing with me, the ups and downs, it’s just a part of what’s happening in those situations, unfortunately.
Iyah: Yes.
Patrik: Regarding the medical records, you should be able just to request them.
Iyah: Correct. Yes.
Iyah: So, we’re going to go to the waiting room, there’s no meeting room.
Patrik: Right.
Iyah: There’s no privacy in the waiting room either.
Patrik: Right. So where are they going to hold this meeting?
Iyah: At the waiting room, in front of ICU, or in other areas.
Patrik: That’s very poor planning from their end.
Iyah: Yes, I agree.
Patrik: Because if they were doing it in the waiting room, there may be other visitors around.
Iyah: That’s correct, no privacy.
Patrik: … there’s no privacy. That’s very inappropriate.
Iyah: So, there’s no meeting conference room that we can be in, Nurse?
Nurse Ron: Let me look at our nurse’s meeting room, okay?
Iyah: Thank you for checking. We’re going to want some privacy on this matter.
Dr. Shelby: Yeah, we usually have one, but after the pandemic they’ve had it closed down for a while.
Iyah: So, we’re going to check on, see if there’s a meeting room for the nurses. I’m Iyah, by the way, Doctor.
Dr. Shelby: Dr. Shelby.
Iyah: Hi, Dr. Shelby. I have my friend on the line, his name is Patrik. Patrik, this is Dr. Shelby.
Dr. Shelby: Hi there, nice to meet you.
Patrik: Hi, nice to meet you, Dr. Shelby.
Dr. Shelby: Thank you.
Iyah: He has experience as an ICU nurse, helping with questions that we need to ask.
Dr. Shelby: Perfect. And you’re Michael?
Michael: Yes, Michael. Iyah’s brother. Nice to meet you, Dr. Shelby.
Iyah: So, we’re still just waiting here.
Dr. Shelby: So, Liza’s going to be calling you?
Michael: Yes.
Dr. Shelby: Is your mother going to be calling you, too?
Michael: No, I don’t think so.
Iyah: Michael, did Pete let you know he can’t come?
Michael: Yeah.
Iyah: He wanted to call.
Dr. Shelby: Can I send him my link that I had for Zoom?
Michael: Yeah.
Iyah: Why does it have to be Zoom? Why not just over the phone?
Dr. Shelby: If you want to?
Iyah: Yeah.
Michael: I would want Zoom. If there’s a choice.
Suggested links:
- Should You Go into A Family Meeting with The ICU Team When You Have a Loved One In ICU? Live Stream!
Dr. Shelby: Just before the meeting, are we still waiting for someone else or are we ready to come with me now?
Iyah: My dad’s hearing all this stuff. He’s in a good state right now, with a little bit of improvement. Just want to keep him relaxing.
Dr. Shelby: That’s fair. He’s under a fair amount of sedation too, so I’m not sure how much he would, but we never know for sure.
Iyah: Right.
Dr. Shelby: So, yeah, whatever you guys want.
Iyah: So, my dad’s blood pressure went up to I don’t know how much, but when I walked in, maybe 120. So, right now they’re giving him some sedation through IV.
Patrik: Right.
Iyah: How high did his blood pressure go?
Dr. Shelby: 170s.
Iyah: Blood pressure 170. What about the heart rate? How high did that go up?
Dr. Shelby: I saw the 120s a minute ago.
Iyah: Okay, thank you.
Patrik: Iyah. So, you’ve seen your dad this morning?
Iyah: Yes.
Patrik: Is he awake?
Iyah: Well, his eyes are open, yes, he was awake. The first time I saw both of his eyes open without struggling to keep them open. That was very encouraging. He looked relaxed.
Patrik: Right.
Iyah: His mouth, he didn’t have the jaw up and down motion today, so that was good not to see that.
Patrik: Right. If you asked him to squeeze your hands, would he do that?
Iyah: No. He’s unable to. He has no movement.
Patrik: Right, right. Okay. If you ask him-
Iyah: He has no voluntary movements to do anything other than try to keep his eyes open.
Patrik: Right. And if you ask him to keep his eyes, or let’s just say he has his eye closed and you ask him to open his eyes, will he do that?
Arlene: I saw him closing his eyes.
Iyah: No, I think it’s just, he isn’t strong enough to.
Patrik: Right, fair enough.
Iyah: This morning he was strong enough to keep his eyes open.
Patrik: Right, right. Okay. I am just sending you a link in Skype, just a link to a website where it clearly states that you have the right to access medical records
Iyah: Got the link up there.
Patrik: So, from the team there, who’s going to be there, palliative care?
Iyah: Dr. Shelby from palliative care.
Dr. Shelby: Yeah.
Iyah: Thank you. And also the nurse.
Patrik: Right? And you’re waiting for other family members to come in?
Iyah: No. We’re waiting on meeting rooms to go to.
Patrik: Oh, I see. Right, right. Okay, then I guess we’ll just wait, I suppose?
Iyah: Yeah, just a waiting game right now.
Patrik: Yeah, sure, sure. But you are feeling more positive today?
Iyah: Yes, yes, very much so.
Patrik: That’s good.
Iyah: Thank you. We did expect this, right? Two steps forward, one step back.
Patrik: Two steps forward, one step back. Definitely expected.
Iyah: I don’t want him to hear any of this stuff right now. I would prefer to leave his room. Can we please leave his room? Can I just go to the waiting area for now?
Dr. Shelby: I’m just waiting to hear back from Ron if he’s ready now.
Iyah: Okay. And the nurse’s name is Ron. Day shift nurse.
Nurse Ron: There is an available room now.
Iyah: Okay, we have a room we can go to.
Michael: I’m going to bug you for a second.
Nurse Ron: Yeah?
Dr. Shelby: That’s no problem. They’re not anticipating anything, we need to be done with meeting urgently.
Iyah: Still waiting.
Patrik: Yeah, that’s okay. I will just wait. I’ve worked in hospitals for over 20 years so I know that hospitals are never on time. There’s no novelty there.
Iyah: Yes.
RECOMMENDED:
Nurse Ron: All right.
Iyah: Okay, we’re in the room now.
Patrik: Okay.
Dr. Shelby: Or do you guys have a layout? Do you guys have a specific layout of whatever you guys want?
Iyah: Would you mind coming a little closer, because of the video, close to my friend?
Nurse Ron: If you give me COVID I’m going to make you buy me a McDonald’s.
Iyah: I’ve been seeing you for the past three days.
Nurse Ron: I know, I’m teasing.
Iyah: We’re still waiting for Mom to be joined via Zoom, and also my younger brother via Zoom.
Dr. Shelby: Do you want to start without them, or wait a little bit more?
Arlene: Call Liza.
Michael: Liza? You’re going to call Liza?
Arlene: Yeah, she told me to.
Iyah: Why don’t we just do a call speakerphone?
Michael: Yes.
Iyah: There’s no need for her to see anything.
Michael: Yeah, she would like the speakerphone thing.
Iyah: Because it’s too much to do with Zoom.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!