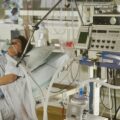
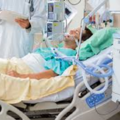
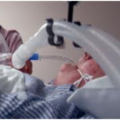
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can Dad Stay in the ICU with Tracheostomy & Avoid Going to LTAC (Long-Term Acute Care)?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Iyah, as part of my 1:1 consulting and advocacy service! Iyah’s dad is critically ill in ICU, and she is asking if having tracheostomy and dialysis for her dad means the end of life for him.
Do Tracheostomy and Dialysis Mean End of Life for My Critically Ill Dad in ICU? Help!
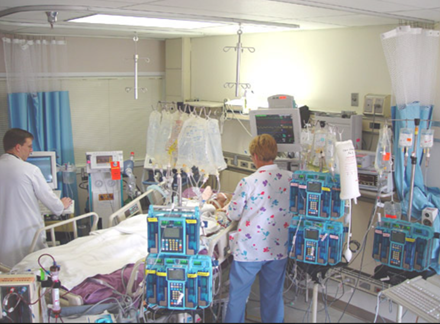
You can also check out previous 1:1 consulting and advocacy sessions with me and Iyah here.
Patrik: Right. There are ways to keep him in the ICU. I think here is what I would advise you to do next. Sleep over it. I do believe that a tracheostomy is almost inevitable. Sleep on it, think about a tracheostomy, and then we can strategize that once you’re clear, you and your family are clear that you want a tracheostomy, then we can strategize how you can keep him there without him going into LTAC. And there are ways of doing that. A lot of the work that we are doing is keeping patients in the right places through the advocacy. But that’s something, I think you should sleep over it, discuss with your family. The other thing that I want to advise you on is, you might’ve heard him saying he needs a trach and a PEG. Have you heard of a PEG (Percutaneous Endoscopic Gastrostomy Tube)? Do you know what a PEG is?
Iyah: Yeah, it’s on the videos. Yes. It goes through the stomach rather than the nasal-
Patrik: That’s right. That’s right. So, once a patient has a PEG and a trach, and they’re stable, they can go to LTAC. Now, one of the strategies that we are implying to families is, don’t consent to a PEG straight away. They can do the tracheostomy…
Iyah: Yeah, right it’s from the videos, yeah.
Patrik: Hold off on a PEG (percutaneous endoscopic gastrostomy), and there’s plenty of time to consent to a PEG if need be. Because if he doesn’t have a PEG, no LTAC (long term acute care) will take him.
Iyah: Oh, yeah, that’s right. From your videos, I do remember that.
Patrik: Right. Right. So, you know, this is just food for thought. And I think as far as I can see, he’s on too much support from the ventilator at the moment to come off it. He’s reached sort of the two-week mark. I also believe now is still a good time to do a trach because then he can hopefully start some physical therapy pretty quickly.
Iyah: Yeah, I agree, the two-week mark, that’s the scary part.
Patrik: Yes, absolutely.
Iyah: I know his lung tissue will start deteriorating.
Patrik: Yeah.
Iyah: And then it’s further infections possibly.
RECOMMENDED:
Patrik: Absolutely. So, I think he’s in a good position to have this done now, and then hopefully move in the right direction quickly. Here is the other thing, Iyah, that’s important. So, the metabolic alkalosis is causing issues in his brain, it’s making his brain foggy. And on top of that, he’s on sedatives, meaning his brain is foggy from the sedatives and from the metabolic alkalosis. Once he has a tracheostomy, they can at least stop the sedatives, and his brain will be less foggy. So, I think it all makes sense in that end.
Iyah: Yeah. I agree.
Patrik: But obviously, you should chat to your family about this. I’m also very happy, if you see value in that, I’m also very happy if you wanted to set up a conference call with your family and have me there, I’m very happy with that.
Iyah: Thank you.
Patrik: You guide me with what you want.
Iyah: I would like that very much. As I mentioned to you earlier, between my three other siblings, the four of us, we are at a split to want…
Patrik: Right.
Iyah: Well actually, I want tracheostomy because I understand it. Too long on ventilator is not good, and he’s not able to breathe on his own at this time, so he needs more time with a tracheostomy. My younger brother, he doesn’t want to tracheostomy at all. He just wants him to be off the ventilator, but that’s not possible, and..
Patrik: Not really at the moment.
Iyah: Yeah. So, my other two siblings want to choose end-of-life to end his suffering because his quality of life would be diminished. But I want to give him a chance.
Patrik: Yeah. I think that’s what it comes down to giving him a chance.
Iyah: Yeah. If there’s anything that he can speak on his own and voice his own opinions on things…
Patrik: Yeah. Yeah. I think we’ve got enough information to say to you, look, I think this is the next best step for him.
Iyah: Yes.
Patrik: And go from there.
Iyah: Yes.
Patrik: Have you found that when you speak to other nurses there that they are as helpful as this guy was?
Iyah: Oh, he was very helpful. The other nurses are not as helpful as him.
Patrik: Right.
Iyah: Other nurses when I ask question, they just shut down what I’m asking. Such as asking if there are alternatives to fentanyl.
Patrik: Right. Once he has a tracheostomy, you probably don’t need to worry about fentanyl anymore.
Iyah: Correct. Correct.
Patrik: If you wanted to, I don’t know, again, if that’s helpful for you, Iyah, once we get off this call, you could share this recording with your family if you want to. It’s entirely up to you.
Iyah: Yeah. Yeah. I will do that.
Patrik: You know?
Iyah: Yeah. I would like that. And also, I would like to have you on a call to answer the questions that they may have. Maybe you may not be able to answer, but with my dad’s condition, may there be a chance that the tracheostomy may be temporary?
Patrik: Oh, look, that is always the goal of the tracheostomy. That is always the goal.
Iyah: And that’s the thing with the palliative doctor. It was open-ended. The choices she gave us were end-of-life or think about his quality of life with a tracheostomy, and they were saying it may be temporary or permanent.
Suggested links:
Patrik: Look, like with anything in life, there’s a risk, and there’s no guarantee. But, got to give it a go. The goal of the tracheostomy can always be that it’s only temporary. The only way a tracheostomy is permanent is, for example, if someone is a quadriplegic because of a spinal injury.
Iyah: Yes. That’s what I’ve come across, yeah.
Patrik: Right. So, that’s the only time. Of course, there are exceptions to the rule, that for someone like your dad in this situation, he may never get off the trach. But I think it’s too difficult to say.
Iyah: Yep. Yeah, it sounds like he’s having a regular breathing, so he is having some breathing of his own. Is that correct?
Patrik: He does. But it’s not enough. It’s not enough.
Iyah: Yeah. So, I am supposed to get a call from a palliative staff to arrange a call between my family and I on Monday. But from what I was told, I’m a guardian of my father’s, and that I would be the one to make the decision. But I still would like to have a family conversation, and have you be an advocate, so it’s clearer.
Patrik: Right. With palliative care, can I just ask… But palliative care just wants to push him towards the end of life. They’re not interested in doing a trach, are they?
Iyah: The way she posed it was, first it was end-of-life, and then think about his quality of life if there’s a tracheostomy. So, it was all gloom. She didn’t mention tracheostomy, the goal is for it to be temporary. She just said, “Think about his quality of life. He has kidney failure, 23 years kidney transplant, and now he has to go on dialysis. Think of his quality of life and think about end-of-life.”
Patrik: And who has been asking you for tracheostomy? Who was that?
Iyah: The palliative doctor.
Patrik: Oh, okay. Interesting.
Iyah: She mentioned the possibility of tracheostomy but think about the quality of life.
Patrik: Sure. Sure, okay. Fair enough. Fair enough.
Iyah: But she never mentioned the goal was for it to be temporary with the tracheostomy.
Patrik: Yeah. Yeah. Sure. Sure, okay. Okay, well what we might do as a next step, have a think about it. And I’ll send you the recording. Have a chat to your family, and then we can map out the next steps.
Iyah: Yeah. And like I said, I’ve already got my mind set.
Patrik: Yeah. Yeah, sure. I get that.
Iyah: I do want him to get off the ventilator as soon as possible-
Patrik: Of course.
Iyah: … and the only option is the tracheostomy, to give him more time to recover.
Patrik: Yeah, I think so.
Iyah: So, I’m on board with that. I wanted to ask about his kidney failure now. Is there a chance that his kidney functions may come back if he improves, or anything?
Patrik: That part I really can’t answer, and that part is something you would need to ask the nephrologist.
Iyah: Yeah.
Patrik: I think there is a chance. However, from experience, I do believe if a kidney transplant patient has gone into kidney failure and on dialysis, I think chances are fairly slim that kidney function’s coming back. But this is a question definitely for the nephrologist rather.
Iyah: Yeah. And dialysis doesn’t necessarily mean end of life?
Patrik: Oh, no, no, not at all, not at all. I mean, as you’re probably aware, many people live with dialysis.
Iyah: Yeah, so he does have a procedure done, a tunnel catheter.
Patrik: Right.
Iyah:Above his chest.
Patrik: Right. Right. So, you know, that should not stop your dad from having a tracheostomy. Because, I mean, there’s many, many people living in the community with kidney failure that go on dialysis three times a week.
Iyah: Yeah.
Patrik: But this is a question that you should be asking the nephrologist.
Iyah: Yeah. Oh, is that correct, three times a week?
Patrik: Again, it depends probably on a case-by-case basis.
Iyah: That’s what I just recall.
Patrik: Yeah. Most of the time, from my experience.
Iyah: Okay. Yeah, like I said, I’m on board with him getting a tracheostomy procedure done. And it sounds like Monday I’m going to get a call from the palliative staff to set up a day and time to meet, discuss with the family and make a decision.
Patrik: Yeah.
RECOMMENDED:
Iyah: I guess we can skip that, because if I’m the guardian…
Patrik: You can just say you want a tracheostomy.
Iyah: Yeah. So, tomorrow’s Sunday for me. Palliative doctors and all, they’re normal business hours, right, Monday through Friday?
Patrik: Look, not… It depends. You got to ask.
Iyah: Yeah. Okay. I guess the thing is, being at odds with my siblings, that are not in line with wanting to give Dad a chance. You may have come across this with other family members and such. What may be the best way to approach this, having a person like you be able to speak about it, clarify?
Patrik: Do you feel like sharing this recording with your family might help?
Iyah: It may be a little too lengthy, but it might help.
Patrik: Well, let’s stop it now. Let’s stop the recording now. Just give me a second.
Iyah: Sure.
Patrik: Just give me a second.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!