Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode as part of a multisequence 1:1 consulting and advocacy series was
I think the dialysis nearly killed my Mom. How can they do that differently next time?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer a question that we get quite frequently from our readers as well as clients here at our popular “YOUR QUESTIONS ANSWERED” section and the question is
Is INTENSIVE CARE AT HOME a genuine alternative to ICU and LTAC?
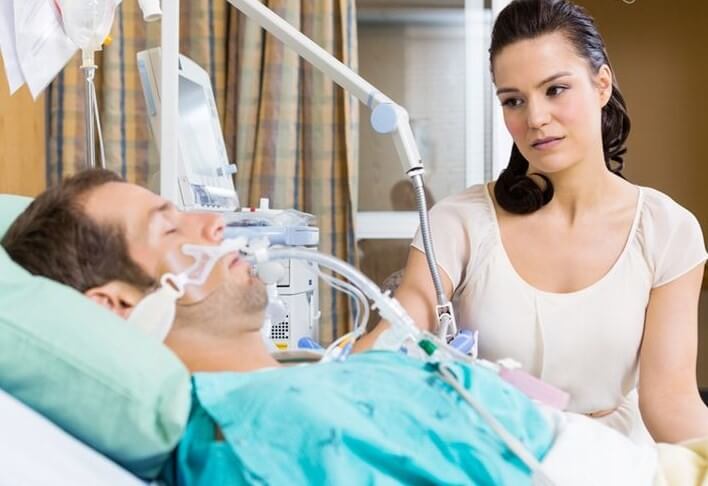
Many families in Intensive Care come to us when their loved one is in Intensive Care with a breathing tube/endotracheal tube, in an induced coma and they want to know if their loved one should have a tracheostomy or not.
Unfortunately, this is the wrong question.
As I always say, the biggest challenge for families in Intensive Care is that you don’t know what you don’t know, you don’t know what questions you need to ask and you don’t know what you need to be looking for!
Because Intensive Care is such a complex, challenging, unpredictable and volatile environment, you will need somebody to guide and “hand-hold” you during this “once in a lifetime” challenge that you can’t afford to get wrong.
The question you should be asking instead is if all resources have been maximized in order to get your loved one off the ventilator and the breathing tube/endotracheal tube in the first place.
How?
I’m glad you’ve asked…
Please click on the link here to get that question answered once and for all
Next, once you know that all resources have been maximized to get your loved one out of the induced coma, off the ventilator and the breathing tube/endotracheal tube and they have followed all the steps from the article/video above, then and only then should you be looking at the possibility of a tracheostomy!
Only then should you be looking at the next steps here
Once you and your family know that the only alternative is a tracheostomy, because your loved one can’t be weaned off the ventilator and the breathing tube/endotracheal tube only then should you give consent to a tracheostomy!
Why should you be waiting and do some research before you give consent to a tracheostomy?
Especially if you are in the United States, you may be aware that once a tracheostomy is done the ICU (Intensive Care Unit) will be very quick and try and move your loved one to LTAC (Long-term Acute Care).
If you are in Canada, the UK, Australia, Ireland or New Zealand the situation is different and I come to that in a moment.
Let’s quickly stick with the USA for now and look at what’s happening in detail once a tracheostomy has been done.
Many families in Intensive Care in the US are taken by surprise when they have given consent for a tracheostomy for their critically ill loved one and then almost the very next day after the tracheostomy has been done, the ICU will want to transfer your loved one to LTAC (Long-term acute care).
This often goes without any forewarning or explanation and if you are not prepared or if you haven’t done your research you and your critically ill loved one are doomed!
I can’t tell you how many families come to us and complain about the LTAC’s their loved one has been sent to after they had a tracheostomy.
Here is the thing: anybody on a ventilator with tracheostomy must never be moved to LTAC or even worse to a nursing home.
Why?
I’m glad you’ve asked.
Imagine this. In Intensive Care you have Intensive Care doctors, Intensive Care nurses, Respiratory therapists (US & Canada), Physical therapists etc…
They are highly trained and highly specialized professionals dealing with life or death, critical illness, life support including ventilation and tracheostomy every single day.
They had to do many years’ worth of specialized training to work in a highly stressful, demanding, volatile and unpredictable environment in order to look after Patients on ventilation and other life support devices.
Going to LTAC on ventilation with tracheostomy therefore is a disaster waiting to happen!
Why?
Because in LTAC you have no ICU nurses, no ICU doctors, potentially one Respiratory therapist for 30 Patients and often only one doctor or specialist overseeing the care of 30 Patients who are life support dependent on mechanical ventilation with tracheostomy!
Therefore your loved one would be going from ICU with all the infrastructure and specialized skills needed to get them off the ventilator and tracheostomy to LTAC where they have no skills to deal with such a massive clinical challenge!
Prolonged weaning off the ventilator and tracheostomy is challenging WITH all the specialized skills, knowledge and expertise available in ICU, but if it can be done anywhere it can be done in Intensive Care (ICU) and not outside of ICU.
The only exception is that after a few failed weaning attempts in Intensive Care, you and your family should then definitely consider INTENSIVE CARE AT HOME.
But you should never ever consider LTAC or long-term acute care.
The only two reasons Intensive Care Units (ICU’s) are wanting to send your loved one out to LTAC after a tracheostomy has been done are
- Free up one of their precious, expensive and in-demand ICU beds
- Save money because the health funds often don’t want to continue paying for a $5,000 per bed day ICU bed
You can see that those decisions are not clinical decisions. They are decisions based around perceived resources available.
It’s getting worse. If your loved one was to go to LTAC and can’t be weaned off the ventilator and tracheostomy- and most of the time they can’t be weaned off the ventilator and tracheostomy because of the reasons I have mentioned- after a period of time that is often determined by the health care funding agency, the next step is for your loved one to end up in a nursing home, where there are even fewer skills and expertise available!
Your loved one would be going from bad to worse. A disaster waiting to happen!
How do I know?
Well after having worked in Intensive Care and with INTENSIVE CARE AT HOME for nearly 20 years as well as consulting and advocating for families in Intensive Care every day of the week, all over the world, I know first hand that LTAC is a very cheap option for the health funding agencies but it’s an extremely poor option for Patients on ventilation and their families!
We have done and are doing a tremendous amount of advocacy work for Patients in LTAC because they simply lack the skills, expertise and specialized staff to look after Patients on ventilation and tracheostomy.
When I talk to health professionals in LTAC they often lack basic knowledge when it comes to weaning off ventilation and tracheostomy!
Therefore do never agree to go to LTAC ever!
Sow what do you need to do instead if your critically ill loved one needs a tracheostomy and ventilation?
Here are some options you should consider
- Do your own research and question everything
- Get 1:1 consulting and advocacy here at INTENSIVE CARE HOTLINE
- Consider INTENSIVE CARE AT HOME as a genuine alternative to a long-term stay in Intensive Care. For example INTENSIVE CARE AT HOME reduces the cost of an ICU bed by 50%, frees up a precious, expensive and in-demand ICU bed and it improves the quality of life/quality of end of life for long-term ICU Patients and their families. It’s a win-win situation!
Unfortunately, Intensive Care Units are not always transparent when it comes to mechanical ventilation, tracheostomy and the next steps ahead.
But you can be in control if you are not intimidated, if you keep asking the right questions and if you get consulting and advocacy.
For example, last year we worked with a client in Cleveland and we managed through our 1:1 consulting and advocacy to keep a tracheostomised and initially ventilated Patient in ICU until they were weaned off the ventilator.
The ICU wanted this gentleman in LTAC the minute the tracheostomy was done. Thankfully the family refused because they had done their own research and they engaged our 1:1 consulting and advocacy service to get the outcomes they wanted for their loved one!
One of the biggest problem for families in Intensive Care is that you can’t argue on a clinical level. Without the clinical advocacy and without the clinical insights, you’d be fighting an uphill battle!
So here is a link to a multi-part case study where we helped a client James to keep his Dad in ICU until he got weaned off the ventilator, despite the ICU and the hospital trying to push him on to LTAC!
Remember, you don’t know what you don’t know and you don’t know what to look for, you don’t know what questions to ask and you simply need the insider knowledge and expertise from someone who knows and understands Intensive Care inside out!
Here is the link to the multi-part case study
Next, if you are in Canada, Australia, the UK or Ireland and your loved one is in Intensive Care (ICU) with tracheostomy and ventilation and they can’t be weaned off the ventilator, you should definitely consider INTENSIVE CARE AT HOME, no doubt about it.
Recommended:
It’s a proven concept and it’s doing all the things I mentioned before.
- It improved quality of life/quality of end of life for long-term ICU Patients and their families
- It reduces the cost of an ICU bed 50%
- It frees up an in-demand, expensive and precious ICU bed
- It decreases infection risk
- Weaning is also possible at home, because INTENSIVE CARE AT HOME is exclusively provided by ICU nurses up to 24/7
Here are some INTENSIVE CARE AT HOME case studies
Here are also some other resources that will help you
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!