Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is new episode series of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
My mother needed a breathing tube and is now in an induced coma, how can she get out of it?
You can check out last week’s question by clicking on the link here.
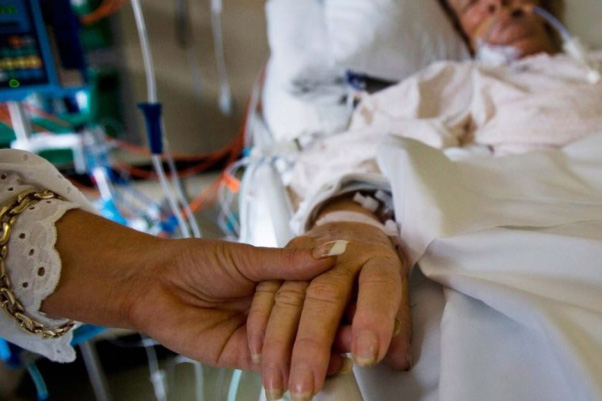
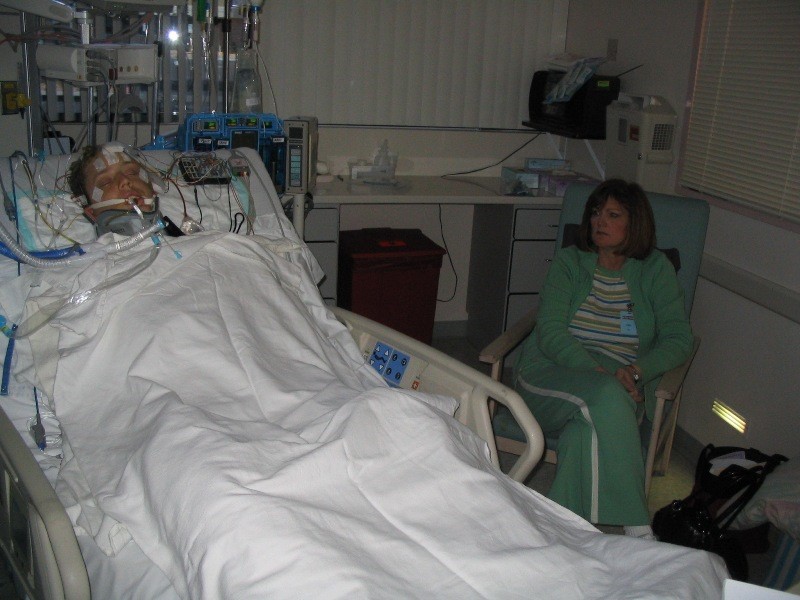
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Sharon who has her 64 year old mother transferred in the Intensive Care due to severe difficulty in breathing and alteration in mental state. Ultimately, her mother was diagnosed with liver failure and is on blood pressure medications and may subjected to dialysis due to kidney failure.
I think the dialysis nearly killed my Mom. How can they do that differently next time?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Sharon here.”
Hi Patrik,
We’ve been told they are now using Fentanyl for the pain.
What does it mean?
Kind Regards
Sharon
Hi Sharon,
Fentanyl sounds right for pain.
What about sedation? They may be using Propofol or Midazolam (Versed).
Kind Regards
Patrik
Hi Patrik,
Oh not sure. I don’t think she is doing much on her own. I can’t believe it changed so fast but you warned me.
Also, my mom is almost off all the blood pressure medicine the doctor said she’s very sick but to take it one day at a time
Kind Regards
Sharon
Recommended:
Hi Sharon,
Ok, that’s good news Sharon!
Again, without the BP medicine she needs one less form of major life support.
Major forms of life support in ICU are
- Mechanical ventilation and the breathing tube to support the lungs/breathing
- Haemodialysis or Hemofiltration to replace kidney function
- Inotropes like Norepinephrine and/or Epinephrine to maintain a life sustaining blood pressure your mom is off this for now and that’s great news
Yes, once again, the liver is not doing great, but there are some small wins and that should be your focus.
If the clotting was that bad, they wouldn’t be able to sustain Hemofiltration.
It would be great if on your next visit you can pull out your cell phone and put me on to the bedside nurse so I can have a chat to them and find out what’s exactly going on.
Kind Regards
Patrik
Recommended:
Hi Patrik,
Ok that’s my plan for tomorrow thank you Patrik you are really awesome!
They are trying to do dialysis now. They have an open line.
Her blood pressure went very low during dialysis and they need to do a cat scan to see if she had stroke she’s back on meds and the ventilator went up in support too.
She’s back on blood pressure (inotropes or vasopressors) meds too.
They really they said she seems less alert now as well, could she have had a stroke?
Sharon
That’s Ok Sharon.
I mentioned to you in recent days that dialysis will get blood pressure down, you may remember.
As long as they are managing it and acting on it, it’ll be fine.
Try not to use the negative language that they are using and try and use more positive language.
It’s not so much what they are saying it’s more what you observe.
You are still focusing on the negatives. Stop focusing on the negatives!
Their judgement is clearly clouded. If it was for them your Mom would be dead by now. She was waking up initially from what you shared.
Do you remember, two steps forward and one step back.
Be patient, your Mom has made tremendous progress in the last 48 hours even though they are now saying she’s less alert.
Could she have had a stroke? Possible, but not likely. Your mother might be less alert because she’s in an induced coma, the liver is failing and the kidneys are failing. She’s critically ill and therefore unconscious.
If she was to have a stroke, it would be a haemorrhagic stroke due to a bleed. The blood is often so thin during liver failure, due to the blood clotting being off and therefore blood coagulation is not working. Therefore, a brain bleed might occur. This would show up in pupils being blown and hopefully they would check for those signs and symptoms.
Currently your mother has more issues than worrying about a stroke.
I also mentioned to you previously that if dialysis is going to be effective she will drop her BP and will need the Norepinephrine again.
No big deal, it’s ICU and it’s expected.
Be patient.
2 steps forward and one step back.
Your Mom is alive, focus on the positives and not the negatives.
Do not use words like “emergency” or “bad news”, it doesn’t serve you.
I’m not surprised that ventilation support went up. Given that she went back into an induced coma and that her blood pressure dropped, it was to be expected.
Kind Regards
Patrik
Related article/video:
Hi Patrik,
Thanks for your explanations.
It helps me keeping my sanity during this very stressful time in my life!
Is it standard for them to then do a brain cat scan? They felt she was a little more unfocused.
She now is back from cat scan and there is no news.
Sharon
Hi Sharon,
Does no news mean the CT scan results are not back yet or does it mean the CT scan was positive?
Kind Regards
Patrik
Hi Patrik,
The CT scan of the brain showed no stroke.
I have also attached some pictures if the ventilator, some infusions and the monitor from today.
Please comment.
Kind Regards
Sharon
Hi Sharon,
Thank you for those images.
Are those images from today?
15 of Norepinephrine is a fair bit.
On the ventilator settings, the ventilator is doing all of the work, which is a surprise to me, given that your Mom has had periods of alertness.
Especially when Patients are more awake in ICU there should be a plan of weaning them off the ventilator. This doesn’t seem to be the case at present.
Normally the first steps to wean somebody off the ventilator is to reduce some of the support from the ventilator if possible at all.
If you could clarify when the images where taken, i.e. before or after she was alert/ before or after CT of the brain it would help to clarify.
Kind Regards
Patrik
More information about ventilators:
Hi Patrik,
This was after the CT scan and the dialysis when her blood pressure dropped.
The weird thing is they said they were using something different.
Sharon
Hi Sharon,
Ok, that’s good to know.
Your Mom would have had a fair bit of sedation to go for a CT scan.
The combination of sedation and the dialysis would have most likely been enough to get blood pressure down and her needing some Norepinephrine.
It says Norepinephrine on the pump which what she had all the way along as far as I understand.
It’s also the standard drug in ICU for low blood pressure.
The sedation would have also been enough to warrant the ventilator doing all of the work for now.
Maybe a question you can ask tomorrow if they are planning to wean her off the ventilator and what steps they have in mind.
Kind Regards
Patrik
Hi Patrik,
My dad just called they adjust ventilation and plan to take the blood pressure meds down again. She is fully alert responds to her name no more dilated pupils.
Sharon
Hi Sharon,
That’s great to know.
It looks like she might have just been sedated from the CT scan and now she’s hopefully waking up again.
Generally speaking, the more awake a patient is and the less sedation they need, blood pressure keeps coming up, hence less need for Norepinephrine.
Kind Regards
Patrik
Hi Patrik,
I think the dialysis nearly killed her. How can they do that differently next time?
Sharon
Recommended:
Hi Sharon,
They may have to start on lower settings.
If they removed 200-300 ml/hr to begin with it would have taken her blood pressure down very quickly.
It’s well known in ICU for doctors and nurses, therefore the Norepinephrine.
Next time they may have to gradually increase fluid removal, maybe starting with 50 ml/hr and then slowly go up to 200-300 ml/hr
Kind Regards
Patrik
Hi Patrik,
Yes, I know they were at 200 ml/hour and that’s a lot from what I understand.
Also, my mother is off BP med again and more awake Just don’t know what’s next?
Kind Regards
Sharon
That’s good news Sharon!
Just wait. Please be patient.
Remember, two steps forward and one step back.
Your mother has come a long way in recent days.
Give her the time she needs to battle this.
Stay positive and keep watching their actions more than their words.
But also keep in mind that ICU is unpredictable and volatile!
Kind Regards
Patrik
Related article:
Hi Patrik,
Blood Pressure went low again. Back with the blood pressure meds.
They also had to stop the dialysis again!
They also want to start preparing for a tracheostomy!
What do you think?
Many thanks
Sharon
Hi Sharon,
Here is more information around tracheostomy
Here is also some information around the MELD system
https://en.wikipedia.org/wiki/Model_for_End-Stage_Liver_Disease
You mentioned, your mother’s MELD is 42
I still wouldn’t panic as all of their predictions have been incorrect at this stage.
Again, keep watching what your mother is doing rather than putting too much weight on their words.
I’m still not too worried about them stopping Dialysis as long as they continue to do the Hemofiltration.
As long as they can remove fluids, that’s the main thing.
Kind Regards
Patrik
Hi Patrik,
They are not sure if she’s stable enough for tracheostomy. They are putting her back on antibiotics because of something in the blood. It seems a lot of steps back today.
Thank you
Sharon
Recommended:
Hi Sharon,
Yes, your Mom might need to be more stable before she can have the tracheostomy.
She still has come a long way since first admitted to ICU and given they are now talking about a tracheostomy instead of end of life is a very different and more positive conversation to have.
Especially with the tracheostomy, your Mom might need ICU for some time to come. Again, it’ll buy her time to recover.
Do you know where the infection is?
Kind Regards
Patrik
“Thank you very much for being a part of the previous series of 1:1 consulting and advocacy sessions. We hope you will find these new upcoming episodes informative and empowering.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!