Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can We Keep that Fighting Spirit So our Sister Can Survive in ICU?
You can check out last week’s question by clicking on the link here.
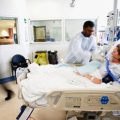
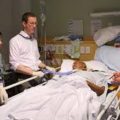
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joyce, as part of my 1:1 consulting and advocacy service! After a couple of months of fighting with her condition, Joyce’s sister is now off the ventilator but still has a tracheostomy, can’t be weaned, and had developed severe pressure sores. Joyce asks how to stay positive whilst her sister is suffering in ICU.
How to Stay Positive Whilst My Sister with a Tracheostomy & Severe Pressure Sore is Suffering in ICU?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Joyce: I mean, she’s like, “I want to get out of here, I want to get out of here.” And I don’t know what to tell her. “Where are you going to go? Can’t come home, and you can’t go there. You’re stuck here.” She’s not going to want to … If I told her, “You’re going to be stuck here for the next X amount of time.” But no one’s really telling her.
Patrik: Right, but she would be asking.
Joyce: What do you mean?
Patrik: Is she asking what are the next steps?
Joyce: No. She just says, “I want to go home.” And I said, “You can’t go home because the wound is very, very bad. It’s severely bad.” And she stopped asking because we kind of gave her the scenario. Said, “If you’re frustrated, I understand. You make a decision. You want to pull off the tube, go ahead, we support you. Whatever you decide.” And ever since that, she has stopped even touching it, which would make it easier for us if she did. How horrible is this? I mean, I feel so..
Patrik: Horrible.
Joyce: … even talking to you about this because-
Patrik: No, I have these discussions all the time, and I am confronted with this-
Joyce: I feel guilty. I feel so guilty. I feel so guilty, because I feel so..
RECOMMENDED:
Patrik: Do you think that as of today, you wish your sister wasn’t here? Is that how you feel? And it’s fine if you feel that way.
Joyce: I feel like the way she is, and the agony she’s going through, I wish something would happen naturally without us making a decision and making peace, because it’s taken a toll on everybody. And not really from me, but it pains me to see her this way.
Patrik: Of course.
Joyce: … without having an option. I don’t have an option, and I guess the prognosis is so poor with it. And I saw it with my own eyes. If I didn’t see the wound, then I’d be naive. It’s so bad, and so horrific. I trust these people saying, “She can’t even be in a wheelchair.” And if it wasn’t for her being in so much pain and needing to be on Dilaudid, that’s not life, Patrik.
Patrik: No, no. I-
Joyce: Even being on painkillers. That’s not life.
Patrik: No, I agree.
Joyce: That’s not quality of life, she’s suffering. I mean, she’s … Listen, the reason she’s okay is because they’re taking really good care of her, and making her really comfortable. Give her one day with nothing, I would shoot her with a gun of how uncomfortable she is. Do you understand what I’m saying? They’re taking really good care of her, so we have a false sense that she’s smiling, and she’s waving because she’s not in pain. Take that all away, she’s not that smiling lady anymore. So that’s what the palliative care said it to me, and he made perfect sense. He goes, “We’re just doing really good job at our job, keeping her comfortable. If she wasn’t comfortable, you would not have that sister who smiles,” which he’s right, in a sense. So, anyways..
Suggested links:
Patrik: I wish I had-
Joyce: I knew going into it, you’re not going to have answers, but what I wanted to just sum up with you is, I wanted to make sure I’m not leaving anything else-
Patrik: Unturned.
Joyce: … on the table. Because you know I started with you, and I want to make sure I’m not missing any. Even though I’m getting 1000 professionals at the hospital that I trust, I still trust you because, you’re completely my advocate, and I want to make sure that if I go through the next steps, I’ve done absolutely everything.
Patrik: I tell you something. The more that I think about this, I’m picturing my practice when I worked in ICU. I worked in big ICUs, like 40, 45 beds. And they have always been one or two patients in big units that would’ve been there for months, up to … The worst that I’ve seen is up to two years. And they would’ve been in somewhat similar situations than your sister. And you wonder why do we continue? And there’s this similar, what if? What happens if we just stop everything? Is it right morally, ethically? What’s this person’s life philosophy? What’s the family’s life … There’s all these questions.
Patrik: And what I will tell you is, there are people at home where you’d think, “Oh my goodness, what’s their quality of life?” And yet, we can see what it is. But it’s very unique to the individual. It’s not a one size fits all. For the outsider looking in, they would say, “Oh my goodness, there’s this 19-year-old teenager on a ventilator, possibly for the next two decades, if she stays fine.” But she lives with her family, the family … It’s all these questions that’s … Who am I to give life or take away? Who am I?
Joyce: That’s what our family believes.
Patrik: Right.
Joyce: That’s what my mom has been … but because emotionally, the other side looks so bad, that my sister doesn’t know the other side. Sitting in a dark room, not having us. That will … right now, she has us 12 hours a day. We are literally doing four hour shifts. Every single day.
Recommended links:
Patrik: How far away is the hospital from your family?
Joyce: 15 minutes.
Patrik: Okay, so it-
Joyce: Everybody … doesn’t matter, but the point is that our life has stopped. I mean, this is all our lives.
Patrik: Oh, of course, of course.
Joyce: And it’s not just two months. This is going on more than six months.
Patrik: And there’s no end in sight.
Joyce: And there’s no end in sight, there’s no end in sight. And it’s like-
Patrik: I wish I had easy answers for you, and I don’t. I have seen too much in all facets, where I think, okay, I’ve seen people having life support stop prematurely. I have seen people not having life support stopped when it should’ve been. There’s all these …
Joyce: And you see? My sister made it. My sister is a survivor. And she shouldn’t have survived this, Patrik.
Patrik: Yeah, I agree. So at the end, maybe … Maybe, I don’t know if you’re a spiritual person, on a spiritual level, is it like, what’s the reason? I can’t answer this for you, but that’s the way I would approach it if it was my family member. Said, “Okay, well there is a reason why they’re still here. Maybe I haven’t got the answer today, but maybe I will find the answer tomorrow, why they’re still around.”
Joyce: And so, in order to cap this, we’d say wait until something happens, and let the body direct us.
Patrik: I think in medical terms you’d say that if that happens, the person declared themselves. And I’m sure you’ve heard this in other situations. But in medical terms, it’s sort of, if something like that happens, you would say, “Okay, the body declared itself.” But you should also look at it from the other end, the body hasn’t declared itself.
Joyce: Yeah, because I did all this aggressive treatment, and now to stop, it’s like..
Patrik: Or is there a point where you and your family can work with timelines? And again, that sounds horrible in and of itself. But is there something you’d say, “Okay, we’ll watch this for another two weeks, three weeks, three months, whatever, and then we’ll really sit down with our sister and make a decision.” I don’t know.
Joyce: We’re letting the hospital think that, because we’re just riding the wave. Well, we’re riding the wave to see when the next thing they come up with. You know what I’m saying? Every other week, it’s been like, “Subacute, subacute.” “Okay, they declined.” “Subacute, subacute.” “They declined.” So every week, we’ve been dodging the bullet, but we don’t know when the next one’s coming. And I don’t want to do this at a subacute. I don’t want to do it.
Recommended:
Patrik: Yeah, no, no. It’s not-
Joyce: But do you see my dilemma?
Patrik: Oh, the dilemma is huge. Are you a religious family?
Joyce: My mom is. We’re traditional. But I can’t take a life putting her in a place that she won’t have us.
Patrik: Is your sister religious?
Joyce: We’re all the same.
Patrik: All the same.
Joyce: We observe it, we’re traditionalist. We’re not one way or the other. But I emotionally can’t think of her being in a room with these-
Patrik: Yeah, yeah. I get it.
Joyce: I can’t.
Recommended:
Joyce: We know the answer to all these is absolutely like, you go all the way, not in your hands, God decides. But to be honest with you Patrik, I can’t.
Patrik: Yeah, you’re seeing the limitations of what that approach can do-
Joyce: Because you saw how far I did, right? I went, went, went, went, went. And now, the suffering, it’s a lot. I don’t know.
Patrik: I wish I had easy answers for you, and I don’t. I don’t have an easy answer for you.
Joyce: Do you think she’ll be able … I mean, from what they say, the wound won’t cover, it won’t heal. It’s bad. Patrik, it’s bad.
Patrik: Oh, I’m not disputing that for a minute. I’m not disputing that for a minute. If-
Joyce: So how long could somebody live … If I were to aggressively treat this, they could be doing this for years.
Patrik: I have seen … Remember, when I did my nurse training, I remember having worked in a nursing home. I remember, there were people in nursing homes that had these massive wounds. Now, I’m not saying they had any quality of life. I’m not suggesting that for a minute, but I can tell you, I know that people have lived in nursing homes and whatnot with massive, nasty wounds for long periods of time. I’m not even remotely suggesting they had any quality of life, but they were living.
Joyce: But at what point?
Patrik: Yeah. So it’s-
Joyce: I don’t think my family can take any more. I don’t think our family can take any more suffering, can’t. And I don’t know if I’ll be … So far, we have not made any decisions, right? We’re just riding it out. I don’t know what I … Right now, I’m acting very robotic, but emotionally, this is going to land, and I don’t know how it’s going to land. And I don’t know if I’m going to mentally scarred forever. I know that … I don’t know.
Patrik: Yeah, yeah. I would imagine, having seen this over and over again in couple of decades, I believe I’m mentally scarred to a degree. And I can only imagine, this is your sister, how that feels like for you. There’s-
Joyce: You think people make this decision and forever carry it with them?
Patrik: And that’s what I mentioned to you early on when we started working together. I said, “No matter what you decide, you’re opening up a can of worms emotionally, one way or another.” If you had stopped there and then, for the rest of your life, you would’ve asked, “What if?” So now you’ve gone in the other direction, and now you’re at a point of, “Okay, well. I’ve done all of that. Well, it’s a big mess,” for lack of a better term. And you are emotionally scarred, because of everything, you’ve seen your sister suffer, you’ve seen your siblings and your parents suffer.
Recommended links:
Joyce: It’s a lot. It’s a lot. It’s-
Patrik: 200 years ago, your sister would’ve died just …
Joyce: Yeah.
Patrik: And now you’ve got all this crazy technology and medicine and whatnot, and we’re saving lives, we’ve very good at saving lives. And then you’re-
Joyce: I remember you told me you had a client that saved his sister, was 97. Remember you told that?
Patrik: Oh, yeah.
Joyce: It was a woman, and he said, “I won’t regret it.” And that story stuck with me, because I’m like, “Okay, well, she did all this, and we went through all the tracheostomy and everything like that. I don’t regret not pull …” You know what I’m saying? I’m happy that I got to see this part, because I got my sister back, and she got to see us. We got this communication. But I don’t know how much farther I want to end this suffering.
Patrik: I know, I know. Are you and your family, are you seeking any counseling? Or-
Joyce: I mean, we’ve been just kind of dealing. I mean, we’re very strong. At least, I am. I’m strong.
Patrik: Yeah, for sure.
Joyce: We’ve been holding it together. I like talking to you, because you’re … You know what I’m saying? It’s not emotional, it’s very … You know what I’m saying? And that’s kind of how I operate, business thing. I don’t know, emotionally, I don’t know. I don’t know where this is going to land. Right now, I have to move the train and land it somewhere, and that’s where my mindset right now is. I can’t think of my emotions, I just got to think of her and put her first. You understand what I’m saying?
Patrik: Yeah, absolutely.
Joyce: I haven’t been feeling. I have no feelings. I mean, I have feelings, but I haven’t … I’m not touching my feelings right now, because ..
Patrik: No.
Joyce: … 100% on my sister and what she’s going through. What I’m going through will be dealt with later. That’s kind of how I’m operating. That’s how I’m able to survive.
Patrik: I get it, I get it.
RECOMMENDED:
Joyce: All right.
Patrik: So I do apologize that I don’t have any easy answers. And it’s, I would say, sit and wait. Sit and wait. Time. I believe time will give you the answers.
Joyce: Okay.
Patrik: Time will give you the answers, but it’s a lot to take in for you and your family, for sure.
Joyce: But you think there’s infection? Once she has a bone infection, it’s still there?
Patrik: If she has a bone infection, I would argue she may not make it. But again, who am I-
Joyce: But she’s been able to have it three weeks without it flaring up, and it will flare up again?
Patrik: Possibly, possibly.
Joyce: So it’s just a matter of … the infection is coming, no matter what.
Patrik: If the wound is as big as you described it, I think it’s not a matter of if, it’s a matter of when.
Joyce: Okay, okay. Okay.
Patrik: All right.
Joyce: All right, Patrik. Well, thank you so much. I’ll talk to you soon.
Patrik: Pleasure, take care. All the best, all the best. Thank you.
Joyce: Thank you, Patrik.
Patrik: Bye bye.
Joyce: Bye bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!