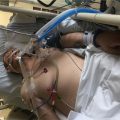
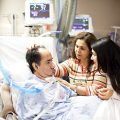
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Your Questions Answered Live: Avoiding Tracheostomy in ICU!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is now off the ventilator but still has a tracheostomy and with severe pressure sores. Joyce asks how she can promote comfort care to her sister with a severe pressure sore in her back.
My Sister Has a Severe Pressure Sore & the ICU Team Says it’s Not Going to Heal! Help!

Joyce: Hey, Patrik. Hold on.
Patrik: Hi, Joyce. How are you?
Joyce: Oh my gosh. Okay, let me give you a … Can you believe we’re still doing this? Okay, let me give you a quick update. So my sister has been off the ventilator for a month. Ever since she got off, she never went back on.
Patrik: Great.
RECOMMENDED:
Joyce: Yeah, she’s been really, really stable. She has reduced her secretions by quite a bit. Still with a tracheostomy, requiring only 20% oxygen through the humidifier. Was tolerating talking valve, recently she’s not … she’s not saturating. She just feels like she’s choking. She doesn’t prefer the talking valve. Arms strong, all off a sudden moving, like a gladiator. Okay?
Patrik: That’s great.
Joyce: Her arms are strong. Her feet, moving. Okay? Super, when I say to you 1000% there, 1000% there mentally in every department, okay?
Patrik: That’s great.
Joyce: But here’s the kick. Wonderful, until this issue. The bedsores are stage four, severely … Now, I up until this point have never seen them. Now, mind you, I’m still in the hospital, because seven to eight sub- acute rejected her because of the severity. In all of 20 years, maybe 35 nurses throughout all their experience has said they’ve never seen a wound this bad. I didn’t master it until the other day, until three days ago. I said, “I have to see this wound.” It is like a huge crater in the back, huge, down … thickness is this with two on the side, one of them even being connected. Huge. I never even thought something like this existed.
Joyce: So sub-acutes have been rejecting her. I’ve been playing this game with the hospital and they’ve been bullying me, but everyone has … And then she’s also susceptible to these infections, so wherever she goes, she has to be isolated, which also a kicker. So I bought myself time in the hospital, I’m still there. They’re okay. But here’s the deal, the deal is, the bedsores are just horrendous.
Joyce: So on one part, I have my sister back 100%. I have her back, she’s strong. She’s 100, we’re doing 12-hour shift from eight to eight, every single day in the hospital, and she’s never alone throughout the day. Arms are just beast. But here’s my deal, my deal is these bedsores. Every time we put her in the cardiac chair, she cannot tolerate it. It’s beyond, beyond anything she can tolerate. Everyone around me said these wounds are not going to heal. They’re really bad. They’re the worst thing I’ve ever seen. And they’re so bad, Patrik.
Recommended links:
Joyce: And I believe, listen, I’m in a better hospital. I’m in a much bigger hospital. And every week, there’s a different doctor, I kind of trust them, the other one was like the wild, wild west, which obviously, I’m actually suing the other hospital because of their neglect. But no here, no there. So we have now chosen … There was a moment that it was like, “Subacute or home?” So we were playing with the idea of bringing her home.
Joyce: There’s no way to bring her home, because the level of care she would need is so horrendous. I even was interviewing care takers. The system here is flawed. The system here to find a 24-hour caretaker is no here, no there. It’s impossible. She’s getting the best care possible in the hospital right now, and that’s 12 hours, 12 hours with a professional nurse. And even the professional nurse, it’s too much for her, let alone someone who’s not in the medical field.
Joyce: So bringing her home, and my mom would not be able to handle it, so that’s not an option. Taking her to a sub- acute where they’re going to give me a half an hour visit every other day is not going to be an option. It’s not going to be an option.
Recommended:
Patrik: Can I ask a few questions about the pressure sore? So what are they doing about it?
Joyce: Okay. So they have been changing the dressing once a day. They have-
Patrik: Is it a VAC dressing? Have you heard of a VAC?
Joyce: Yes. They tried a wound VAC, but because her anus is literally right there, what happened with the wound VAC is the poop would go in there, and it never worked, so they took it out.
Joyce: I will say this, they’re taking care of the wound very well, because she doesn’t have infections. She’s been there for three, four weeks … I told you, couple weeks ago she had an infection down to the bone. They discovered she had an infection in the bone. They treated it with antibiotics, and ever since then, she hasn’t had infection, but we know it’s looming inside.
Patrik: It’s there.
Joyce: So here’s … yeah.
Patrik: What are they doing with the wound? Are they washing it with saline every day? What are they putting?
Joyce: Yes, and then stuffing it with … I think they’re stuffing it with gauze. I believe they’re cleaning it, stuffing it with gauze, dressing. I will say that I think she’s getting good wound care, because it’s becoming nice and pink.
Patrik: Okay, that’s good. How big is it? How big is it?
Joyce: Huge.
Patrik: Talk about 10, over 10 cm?
Joyce: Let me see. Hold on, I’m going to show you. It’s huge. It’s from here to here.
Patrik: Oh my goodness.
Joyce: Hold on, let me see. Maybe this big for the back.
Patrik: Oh my goodness.
Suggested links:
Joyce: And then there’s two circles here. I would take a picture, but I don’t want that picture on my phone.
Patrik: No, no.
Joyce: Worst thing I’ve ever seen in my life.
Patrik: How deep is it?
Joyce: Pretty deep, where you get to see muscles.
Patrik: Bone?
Joyce: They say they see bones.
Patrik: Oh my goodness.
Joyce: They see bone. She said you can definitely touch the bone. And you know what’s surprising Patrik, my sister survived. My sister got off the ventilator after five months. She would’ve been home in a wheelchair of some sort, and she actually would’ve even been walking, because this girl is a gladiator, like I told you.
Patrik: Yeah. Well, what stops … I mean, the wound shouldn’t stop her from walking, really.
Joyce: What do you mean? She can’t even sit. They’re saying in order for her to walk, she would have to sit first. And she can’t even tolerate sitting whatsoever. She cannot tolerate.
Patrik: Why is that? Why can’t … Didn’t you say she’s getting in a cardiac chair?
Joyce: She was, but she cannot tolerate it, cannot. I got her, the pain is so excruciating. Now, she’s on Dilaudid every … Here’s my problem. So we’re kind of even considering comfort care, and the reason is because she’s in so much pain. She’s in so much pain. And when I try to do the cardiac chair, he goes, “Listen, if you want ever your sister to walk again, she would have to sit. You have to sit before you can walk.” She can’t even sit. She can’t even sit. Not for five minutes. She says, “It’s burning all over my body. I cannot tolerate it. I can’t tolerate it.”
Joyce: So listen, Patrik, I’m at a point, we’re all at a point … we got this far, and she’s so mentally there, she’s so mentally there. She can hold your hand tight. I’m talking like … the turnaround is drastic. I have my sister back, I have her strength back, I have her personality. I have her back. But what I am worried about, is this wound. And I really do trust they’re saying it’s never going to heal. She’s not getting-
Patrik: Have you spoken to a surgeon, to a wound specialist?
Joyce: Yes, and they said, “In order to even do a … to get to that point, the tissue and muscle have to heal from the inside before we can even get …” So here’s my thing. Okay, so here’s the kicker, where I’m at. We’re contemplating comfort care. And the reason we’re contemplating is say, look, if she gets another infection, we’re not going to treat it. If something bad happens, we’re going to let it ride out.
Joyce: And the reason is, is because she can’t come home, and she can’t go to a subacute. I would end feeding before I let her be in a subacute for half an hour. She’s so used to seeing us 12 hours, and she’s already in agony. She doesn’t know what the next door ahead of her is. And I’d rather her not be traumatic. The reason I’m talking to you, maybe it’s not medical advice, as much as ethically-
Patrik: Where to?
Joyce: Ethically, I just kind of want to plan with you because, look, she called me every … She knows how to communicate. She called me every two hours last night. She doesn’t want the sleeping pill. She doesn’t even want the pain killers, because she wants to be in control mentally. She’d rather be in pain. That’s how strong this girl is. Even though she looks comfortable when she’s taking pain killers, it gives you that false sense of security, saying, “Oh, she looks good. Her face looks good, and she’s not in pain.” But if she’s not on Dilaudid, her whole body is on fire. Her chest has been peeking out. I even think she even got skinnier.
Patrik: So when you’re saying she’s mentally there, have you put the comfort care to her?
Joyce: I don’t think she would want the comfort care.
Patrik: Okay.
Recommended:
Joyce: I can, I’ll tell you … Let me explain it to you. There was a moment that she ripped the tube out, and we were like, “Oh my God.” We reinforced it, and we said, “You know what? We’re going to leave the tube hanging out. If she pulls it out, that’s on her choice, we’re not putting it back in.” And we said to her, “Sis, if you pull this out, we’re not putting back in?” And ever since we said that, she hasn’t been touching it, at all.
Joyce: My sister got comfortable with her situation. You’re telling me, would your sister want to live like this? I think she got used to it. She poops, she goes, “I pooped. I got to get cleaned.” My sister got used to it because we’re there 12 hours. She gets to see us. I think she kind of surrendered to the fact saying, “Okay, I still want to …” Now, mind you, she cannot leave the room, so she’s confined in this room. Okay?
Patrik: Do you think she’s depressed?
Joyce: Yes, 100%. I gave her anti-depressants. I’ve been giving her anti-depressant. My sister would be anti all this … She didn’t want, anti, but I’m throwing them in there. 100% depressed. My question is, if I asked her, do you want to continue, she would want to live.
Patrik: She would want to live. What’s happening, what stops her from having the trach removed?
Joyce: From what I understand, even though her secretion has lowered, I’ve been, keep asking for a swallow test. The last couple swallow test, she has not succeeded. So-
Patrik: Okay, now that’s..
Joyce: But overall, I mean, she’s pretty comfortable. She’s on the trach collar. Very minimal, minimal..
Patrik: So it’s the swallowing that stops her at the moment.
Joyce: At the moment, and coughing up her own secretion, but her secretion has reduced significantly, but I’m sure she’s still weak to cough it up.
Suggested links:
Patrik: Yeah, sure. I mean, I’m sure they will be trying again in terms of the swallowing. I’m sure they will, but it sounds like that’s the obstacle. How much Dilaudid is she getting?
Joyce: I don’t know, I think it was … don’t quote me on … Maybe, does 0.25 make sense to you, or no?
Patrik: 0.25, yeah. But how often? How often?
Joyce: So she has an order in the morning. She has it every 12 hours, and then as needed every two to three hours. She’s been taking it, I say, about three times a day. And she doesn’t even want to, but she’s in pain, so I just give it to her.
Patrik: It’s a nasty … when I say it, it’s a drug that helps with pain, but it also … It’s morphine. It’s morphine.
Joyce: It’s higher than morphine.
Patrik: It’s higher than morphine. So it’s pretty-
Joyce: It doesn’t knock her out. Patrik, it does not knock her..
RECOMMENDED:
Patrik: Oh, yeah, because her tolerance is through the roof. That’s why. She’s probably addicted to it, and she doesn’t even know.
Joyce: She doesn’t even want it though. She will say no to you.
Patrik: Yeah, of course. Of course, I get all of that. Look, it’s … and this is, I remember when I first spoke to you.. I can’t remember. I mentioned to you, no matter which way you go, you’ll open up a can of worms. I said it there and then. No matter, even if you had stopped then, you would’ve always asked yourself, “What if? What if? What if?” It’s a very tricky-
Joyce: I’ve realize how far we’ve come, and for her to be-
Patrik: Absolutely.
Joyce: And you told me after three months, it’s kind of like they won’t get off. She did it after five and a half months. And not only did it get off, but she’s 100% there. Names, she’s writing.
Patrik: So she can communicate with you.
Joyce: Oh, 100% communicate, 100%.
Patrik: That’s great.
Joyce: Very coherent with who she is.
Patrik: Yeah, that’s great.
Joyce: You know Patrik, it’s just as bad.
Patrik: Sure.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!