Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Sister Has a Severe Pressure Sore & the ICU Team Says it’s Not Going to Heal! Help!
You can check out last week’s question by clicking on the link here.
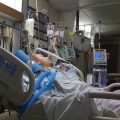
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joyce, as part of my 1:1 consulting and advocacy service! After a couple of months of fighting with her condition, Joyce’s sister is now off the ventilator but still has a tracheostomy, can’t be weaned, and had developed severe pressure sores. Joyce is asking how to take control and have peace in making decisions for her critically ill sister in the ICU.
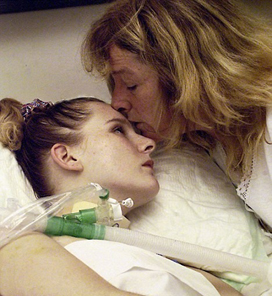
How Do I Take Control and Have Peace in Making Decisions for my Critically Ill Sister in ICU?
Patrik: Oh, yeah, because her tolerance is through the roof. That’s why. She’s probably addicted to it, and she doesn’t even know.
Joyce: She doesn’t even want it though. She will say no to you.
Patrik: Yeah, of course. Of course, I get all of that. Look, it’s … and this is, I remember when I first spoke to you.. I can’t remember. I mentioned to you, no matter which way you go, you’ll open up a can of worms. I said it there and then. No matter, even if you had stopped then, you would’ve always asked yourself, “What if? What if? What if?” It’s a very tricky-
Joyce: I’ve realize how far we’ve come, and for her to be-
Patrik: Absolutely.
Joyce: And you told me after three months, it’s kind of like they won’t get off. She did it after five and a half months. And not only did it get off, but she’s 100% there. Names, she’s writing.
Patrik: So she can communicate with you.
Joyce: Oh, 100% communicate, 100%.
Patrik: That’s great.
Joyce: Very coherent with who she is.
Patrik: Yeah, that’s great.
Joyce: You know Patrik, it’s just as bad.
Patrik: Sure.
RECOMMENDED:
Joyce: As good as it is, it’s just as bad.
Patrik: Yeah, of course, of course. So I have seen wounds heal, but it takes ages. It can literally take months.
Joyce: Oh I think, they say that the odds of it closing, because she’s not mobile, she’s not getting nutrition. He goes, “The crater is so big, and by the time we get her food, all the nutrition is seeping out of the wound. The pus, the water, and all that.” Usually, when our body is closed, our nutrition circles.
Patrik: That is where it’s supposed to be. What about, have you heard of a debridement?
Joyce: She’s been doing that. So every time it’s been black, they’ve been debriding, and it’s been really nice and pink for a couple weeks now. She hasn’t needed a debridement. But regardless, he says, “It’s not if, it’s just when she’s just going to get the next infection.” So goes, “There’s no way she’s going to not …” Even though she’s been three weeks without an infection. He says it’s just going to be waking up, that bone infection is going to come back.
Patrik: Who’s telling you that? Who is it? Who is he?
Joyce: Several people, the doctors … And I will say this, I’m not as suspicious, because they have a new doctor every week, and it’s operated in a big hospital. I don’t think they have incentive like that little hospital got. I felt like it was very business. I felt like these doctors who come in are telling me the truth.
Patrik: Sure.
Recommended links:
Joyce: And I feel like 95% of the whole board are telling me the same thing. They’re saying, “It won’t heal.” She can’t sit in a cardiac chair. She can’t even be in a wheelchair. I don’t even know what it would take to get her in a wheelchair. And the kicker is, this is the sad part. If I would’ve had this operation at home, she would be okay being in bed, being around us. I don’t have that.
Patrik: What are they doing? Is she on an air mattress? Are they doing regular … and are they turning her regularly?
Joyce: Religiously. They’ve doing very good care. I will say to you that they’re taking such good care of them that I can’t even take in effect with comfort care. I’m waiting for … Listen, I’m telling you. I’m waiting for something to happen.
Patrik: Yeah. Is palliative care involved?
Joyce: I just got them involved a week ago. I called them. I don’t know what to do.
Patrik: What are they saying?
Joyce: He was very, very sweet and very supportive. Very different from the other one. He just said, “Your situation looks like this,” like I told you, and he goes, “You can decide what you want.” Right now, the way I have it is, I took the vitamins away, whatever. Just so they can … Look, I’m ultimately buying time in the hospital. So I want to show them that I’m going to do comfort care. So I took the vitamins out, not a big deal. And then I said, “If she pulls out the feeding tube, we will not put it back, and if she runs an infection, I will not treat it.”
Joyce: But what we’re morally struggling with is the moral aspect of us not having to choose, and us … because she’s so mentally there. And I would ask my sister, “Do you want to go?” She’s not going to say no. She’s not going to want to say no. My sister’s scared to death of dying. She will fight. Listen, you saw how much she fought to be with us. Here we are 12 hours a day because of the situation, but to be honest with you Patrik, is it wrong for me to say that I’d rather let her go than be in a subacute? I’d rather kill her, than..
Patrik: Well, I don’t think that subacute is an option. You’ve sussed that out already. Subacute isn’t an option.
Joyce: Well, not necessarily. They have tricks up their table. I’m not saying … who knows? They still want to get her out.
Patrik: Sure.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Joyce: But I don’t know when the next bomb’s going to come. It’s just seven of them said no, but who knows?
Patrik: It’s a very tricky question. I guess, the pain is big. And I can see now that your sister is mentally with you, I can see why you would be saying no. Can you override those wishes? Very difficult. And where do you go from there?
Joyce: Do you think they’ll ask her? I don’t think they’ll ask her.
Patrik: No, I don’t think they’ll ask her.
Joyce: Right.
Patrik: I think the only people that can ask her is probably you and your family.
Joyce: I wouldn’t do that. I’m waiting for her body to tell us what to do, and then I’ll just say, “Hey, it’s not us.” If she runs a really, really high infection and it’s getting too miserable, I’ll cut the food out. I just can’t mentally think. I’ve gotten this far. How horrible, Patrik, to get this far-
Patrik: Horrible.
Joyce: … and then I have to do this? You saw my fight. You saw our fight. I’ve never been committed to something in my whole life.
Patrik: How does the rest of your family feel about this?
Joyce: All feel the same. We all feel the same.
Patrik: You’re all united, you’re all in this.
Joyce: We have moments. We have some fights, and we’ve had some really, really … This is when the true nature came in, when the subacute aspect came to about a week ago, and we were contemplating, does she go, does she go home, or do we do comfort care? And we’ve sat as a family and we decided subacute. I call the place, he goes, “It’s a half an hour every other day, if that.” And we said, “Oh my God, no way.” That’s too much..
Joyce: And then taking her home, there’s no way. There’s just no way, no, no way, cannot. The whole family would be too stressed about it. As we said, “We don’t want something to happen at home.” I think that fairytale of bringing her home through hospice is not who we are. We’re just not able to do that. As they say, whatever it would sound like, I don’t think any of us want to take that on, because we’re tired. And we’re just..
Patrik: Yeah, fair enough.
Suggested links:
Joyce: … supported, do at a place that it’s supported and whatever. And then basically, we were about to say to them, “Pull the feeding,” but then the subacute came and said, “Oh, we can’t accept her.”
Patrik: Look, I haven’t seen the wound, but I have seen nasty wounds. It sounds to me like it’s bigger than-
Joyce: It’s bigger.
Patrik: … beyond that what I’ve seen. If the VAC-
Patrik: Yeah, yeah. Where is she? Which area is she in at the moment? Is that like a step down ICU, is it like a floor area?
Joyce: It’s DOU, it’s still DOU (Definitive/Direct Observation Unit). So it’s a step down from … DOU.
Patrik: Still attached to ICU?
Joyce: Yes.
Patrik: Yeah, okay.
Joyce: And the reason she’s there is because I fought for her not to go to another floor, and I made connections with the thing, and I said, “Look, everybody knows her wound. Starting all over is illogical,” and whatever.
Patrik: I think you’re probably on the right track to wait and see what the body is going to tell you. Is she on antibiotics at the moment?
Joyce: She hasn’t been needing them, and that’s the crazy part. I’m waiting for the blood cells to go up. It’s at 15.9, or 15.6. It was a 14 and 15. Now it’s 15.6. My question is, are we looming an infection? She doesn’t have a fever.
Patrik: Wait, wait. I mean, you-
Joyce: Is a 15 looming, or there’s no … it can go up and down?
Patrik: It can go up and down a little bit. It can go up and down a little bit. 15, if it was 20, I’d say, yeah, sure.
Joyce: But it can go up to 20?
Patrik: Just wait, just wait. It’s a tricky one. With the Dilaudid, I’ll tell you where I’m a bit … Sort of, you say she’s mentally there, I do believe that if she’s been getting Dilaudid for many weeks now, I argue there is … it’s suppressing her mental capacity a little bit, because it’s morphine. You don’t think so?
Joyce: Patrik, I asked her something about where this, she told me exactly where it is. And the only concern is, I think Dilaudid is not working.
Patrik: Yeah, her threshold is too high. Her pain-
Joyce: And so what do we do? What can we go up from here? That’s the problem. I’m going to surpass these medication, and she’s going to be burning inside.
Patrik: If you ask her on a scale from zero to 10, zero no-
Joyce: Eight.
Patrik: Eight.
Joyce: She always says eight. But then again, she’ll … Say, she’ll be in pain, and she’ll refuse the … She’ll be okay with being in pain, but she’ll just be super, super uncomfortable, and super grumpy.
Recommended:
Patrik: Does she sleep at night?
Joyce: Nothing. I tried to give her the sleeping pill, and last night, she yanked the nurse. She’s getting stronger with her hand, so now she’s yanking and saying, “Nope, I don’t want nothing.” So she’s not sleeping at night right now, or at least last night. She’s not sleeping because she’s not willing to take any medication to alter her mental status. She wants to be up and she wants to be whatever. My only question is, am I giving up? You know that I did everything I can. And listen, it pains me. How much can … Listen, I’m at home and all I do is I’m thinking this lady is stuck in bed.
Patrik: Look, I think all you can do at the moment is wait, in terms of what’s your sister’s body is telling you. It sounds to me like an infection is not a matter of if, it’s a matter of when, and that could be the end of it. Or miraculously, if they’re giving her good wound care, maybe it starts slowly. But it would be probably a process that would take months.
Joyce: Months to get an infection?
Patrik: No, no. No, no. Months to get it healed. I think infection, again, it’s probably not a matter of when, it’s not a matter of..
Joyce: You say no matter how good the wound care is, she will get still an infection no matter what. No matter how good the wound care.
Patrik: Yeah, I agree. And then the question is can she survive that, is her body strong enough to fight that?
Joyce: Well, we have a lot of antibiotics, but to be honest with you, what’s the end game? She’s in the room, I can’t bring her home. I know that subacute is knocking at the door. If not now, in the next thing. Unless I tell the hospital, “Listen, I’m doing comfort care. Cut the feeding.” And I stay in the hospital, because I don’t want to leave the hospital. And that will be the only ticket to stay.
Patrik: Yeah, yeah. Is the health insurance breathing down your neck?
Joyce: Nobody.
Patrik: Okay.
Joyce: No, because she’s fully covered. She has this low income, she has this full umbrella. Nobody’s breathing down my neck at all.
Patrik: Yeah, okay.
Joyce: But how bad … Let me ask you a question. What else can I remove for it to be humanly humane without me feeling guilty? So I-
Patrik: Well, tracheostomy.
Joyce: The trach?
Patrik: But that’s removing the lifeline.
Suggested links:
Joyce: Let me ask you a question. The minute I put her at room air, she desaturates. But it’s so minimal, she’s only getting 28. But if I do take that aerosol out, that number will start going down, down, down, down, down, down. And she can die from not having the very small oxygen. That’s how sensitive it is.
Patrik: I hear you, I hear you.
Joyce: No, but I’m saying, that’s how sensitive it is, Patrik.
Patrik: Yeah, yeah. Oh, it can be. Yeah, absolutely.
RECOMMENDED:
Joyce: That’s how much she needs … But it’s that minimal. Because I looked at the trach, and barely any air is coming out. You know what I’m saying? That aerosol’s not coming out that much, but it makes such a huge difference. I take that out, she … within minutes.
Patrik: So let’s just run through what you might perceive as the worst case scenario. Let’s just say you go down the track of comfort care, you remove the trach, you stop the feeds, and you do what-
Joyce: I can’t remove the trach, because the trach will be within half an hour. That’s too dramatic.
Patrik: Right, right. But even if you start with removing the feeds, what would you need to do? You need to probably up even the Dilaudid more. You would have to give her a sedative. You could argue-
Joyce: It would have to be in the drip.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!