Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Long Will it Take for My Mom to be Weaned Off the Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
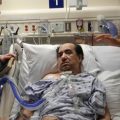
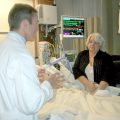
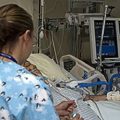
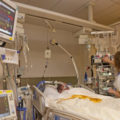
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tom, as part of my 1:1 consulting and advocacy service! Tom’s mom is on a ventilator and with ongoing sedation. Tom is asking how to have control and power over the ICU team so that his mom can get the best care and treatment.
How to have Control & Power Over the ICU team So that My Critically Ill Mom will Get the Best Care and Treatment?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tom here.”
Ronald: Hi Patrik.
Patrik: Hi Ronald, how are you?
Ronald: Oh, hanging in there, we just got back from the hospital with the medical, so.
Patrik: Right. And thank you so much for sending through those reports, they are incredibly helpful. And I certainly have some questions out of that report, and I believe there are things in there that you haven’t mentioned to me. And I believe there are important things in those reports that they pretty much haven’t shared with you or explained to you.
Ronald: Okay.
RECOMMENDED:
Patrik: But-
Ronald: Got it. Good, I’m glad. And when I was certainly trying to get your help in interpreting them, because I read, I’ve been reading them. Actually, I just discovered them like a week and a half ago where they are, and I was like, “Oh gosh, okay.” I didn’t know that we had the right to access it.
Patrik: Right.
Ronald: So it’s a learning process for us, but anyway, I by no means, I don’t, we don’t understand everything that’s going on with them. But yeah, let’s definitely talk about that, and if we can give you a general update on how we have served her today, today was a bit of a tough visit.
Patrik: Right.
Ronald: But I don’t know if we want to go how far into detail on that, or just into your question.
Patrik: Look, why don’t you start with giving me an update of what’s happened from your end, and then maybe we can tie in with the report. Why don’t we do that?
Ronald: Okay. I’ll try to summarize just to kind of try to keep it concise, hope you read that.
Patrik: Yeah.
Ronald: But yeah, so we found her today, I mean just, it was noticeable that her spirit and her mood is… it was down. Today, actually, it was the first time she’s been noticeably, like, she’s sad, she’s feeling a little frustrated, and I believe she’s been feeling that all along, but it was more evident today. And we felt it in the room as soon as she walked in, and we just tried to encourage her and let her know we’re here, despite how long it’s going to take, what and that doesn’t matter.
Ronald: But that was really hard for us to see, so we’re feeling a little just strained right now, too just trying to cope with the changes in moods and feelings that she’s going to have through this.
Patrik: Yeah.
Recommended:
Ronald: So-
Patrik: … and do you see her every day?
Ronald: Yeah, we-
Patrik: Yeah, okay.
Ronald: … have seen her every day, yeah.
Patrik: Yeah, okay. And would you say today was the worst in terms of mood, or?
Ronald: Yes. So very worse in moods, but also there’s been a lot, like the last… I think I would say it’s only been maybe six or seven days where she hasn’t had any more surgeries, procedures, like getting rolled in and out, a lot of commotion. So this is also kind of the first stretch of being in her room and weaning off the ventilator, and very alert, present, oriented.
Ronald: And I think also she is recognizing where she is and from the deconditioning, I think that has started to settle in. So also I guess with that in mind I need to make sense that maybe some of this is settling in this a bit differently for her, you know?
Patrik: Yes. Absolutely. She’s probably just trying to come to terms with things.
Ronald: Yeah, that’s a good way to put that. So yes, so when we say today’s the worst, it’s, I mean, of course we feel terrible, because it’s hard for us to see her that way. Also, maybe this is just kind of the first prompt in that emotional rollercoaster she’s now really all present for.
Patrik: Yeah. In that case-
Ronald: So-
Patrik: … in that case, if there is something positive about that, is it’s… it’s good to see that her brain is intact, it’s good to see that her brain is working. And it’s also good to see that they have weaned some of the sedation down. I mean I remember when we first started talking, it was all about weaning sedation.
Ronald: Yes, we are-
Patrik: And it looks-
Ronald: … so glad to be past that now.
Patrik: … yeah.
Ronald: And understand how significant that is, and all, yeah.
Patrik: Yes. Absolutely.
Ronald: So… so yeah, so that was a bit about his mood. In terms of physical therapy, she had a bit of physical therapy today.
Patrik: Great.
Ronald: They’re not very long sessions, but you know, and that’s what they keep reminding us. But what she is getting up, she did stand up yesterday. Of course she did it all with assistance, but she did stand up the last five days. And yesterday, she took a couple steps, today she took, like, a step, but not a few. But they explained to us that in the next, about, three days they would like to get her to get fit into a chair and then do her CPAP trials seated in a chair.
Patrik: That’s fantastic. That’s fantastic.
Ronald: Yeah. So that’s very promising. Now the other thing, so moving over to her breathing trials, and she’s doing the CPAP trials, she’s only tolerating, from what we understand, about less than two hours a day, that’s what it was today again. But, and they’re breaking it up into separate hours also, because she does express that she’s tired-
Patrik: Yeah.
Ronald: … you know, after the first hour. I anticipate that’s a bit normal to expect her to be tired, but I know earlier in this week, they did tell me, Friday, like he was tired. We asked if she could just go a little longer, she went an hour and a half. But now the last four days, they’ve actually been separating the two hours and giving her a break.
Recommended:
Patrik: Mm-hmm (affirmative).
Ronald: And yesterday and today they conducted a one-hour CPAP trial while we were there. So we’re also learning and observing and just encouraging her through that hour, we could only hope that it helps that we’re there, but I mean, it gives us, it helps us understand, okay, what she’s going through, and then she’s tired afterwards, that’s okay.
Ronald: But-
Patrik: Good, good.
Ronald: … yeah, so she did her CPAP trial while we were there for an hour. The respiratory therapist explained to her and to us, and I read it in the doctor’s notes. So I did ask today that the doctor wanted to increase the PEEP to lower the pressure, like with pressure over PEEP or something, fraction?
Patrik: Yes, makes sense.
Ronald: So… yeah, so then I asked, I said, “What does that mean? Like, is that a technique?” And they were like, “Basically, yes,” if that’s something that we can do to start lowering the pressure, and then gradually wean her off down the PEEP. So today they did 22 over 10, whereas yesterday was 28 over 6. So-
Patrik: Mm-hmm (affirmative). Yeah, that.
Ronald: … they’re going to stay with the 10 denominator for tomorrow also, but try to bring it down to 20. But we don’t, I don’t understand entirely what the 20, the number on top is doing for her.
Patrik: I can talk about that. I can talk about that.
Ronald: Great. So yeah, so that’s the high-level what we observed today. We haven’t had any contact with… the doctor hasn’t approached us in the last five days. I mean of course they’re writing their notes, but they’re not going out of their way to help directly since it’s Saturday now. I’m thinking they’re making it personal. I do sense it because they’re all recommending LTAC and we pushed back twice now pretty hard.
Suggested Links:
Ronald: And so it’s kind of awkward, I feel like they’re avoiding us. But I can’t really, I don’t have evidence of them avoiding us, so I’m not going to go that far yet to say that.
Tom: But that’s okay if you feel that way.
Ronald: But so yeah, so that’s what we’re noticing, but the nursing staff has been very responsive, assistive. Like really, there’s no disconnect or any concern there, but I’m just observing, like the palliative team, the doctors, look, I’m not seeing them anymore. They’re not stopping by anymore.
Patrik: Well-
Ronald: But at least they have in the last-
Patrik: … well-
Ronald: … like, five or six days.
Patrik: … if your gut is telling you that they’re trying to avoid you, your gut is probably right. But you know, you don’t necessarily need to see that as a negative. You know? It means-
Ronald: Okay.
Patrik: … it means they’re probably a little bit intimidated by you now too, because they realize you’re questioning.
Ronald: Mm.
Patrik: If they could do whatever they like, they would probably say to you, “Hey Ronald and Tom, we need to go to LTAC tomorrow and there’s not much you can do.” Right? So if they felt they could do that, they would probably do that, but I don’t see that as a negative of them trying to-
Ronald: That’s a good point.
Patrik: … you know, I don’t, I-
Ronald: Yeah, that’s true.
Patrik: … I don’t see it as a negative of them trying to avoid you. You’ve got access to the doctor’s notes, which is very, very valuable and very important. So, but coming, I just want to summarize what I’m seeing from my end, and see whether you think that is accurate. When you first started talking to me it was all about getting her off sedation, you know?
Ronald: I know.
Patrik: Then she had the tracheostomy, okay? She’s done that. And now sedation is minimized, she’s still on sedation as I can see in the doctor’s notes, but it’s minimized. I mean a week ago you probably wouldn’t have thought she would be standing, would you?
Ronald: No.
Patrik: Right.
Ronald: No.
Patrik: Right, right.
Ronald: Not at all. And I will say, just to add to that comment about sedation even though it’s low, they’ve explained, the nurse, bedside nurse has explained that it’s available on the chart, but they’re not administering-
Patrik: Yeah.
Ronald: … they haven’t been administering it for a couple days, several days now since they got the bleeding under control. That was, the last time they gave her sedation was on Thursday because they had to put in a blood, like, vein filter because they took off blood thinner.
Patrik: Yes, I saw that, I saw that. Now I come to that, I come to that.
Ronald: Oh okay, okay got it, sorry.
Patrik: Yeah.
Suggested Links:
Ronald: I just wanted to let you know that’s what they told us, they haven’t been sedating her since that day-
Patrik: Yeah, yeah..
Ronald: … of reports, yeah. So anyway, I’m sorry. Continue.
Patrik: Yeah, no. So I see a lot of progress. Right? Even if she can’t tolerate the CPAP trials yet, I mean, she’s doing that. You know, it’s… you’ve got to start somewhere. And I can see why she’s not tolerating them yet because she was in a coma for so long. Right? So her breathing muscles should be severely weakened. But that’s why I’m so pleased to hear that they’re standing her up, that they’re talking about sitting her in a chair. That’s how you strengthen breathing muscles.
Ronald: Mm-hmm (affirmative).
Patrik: Right? So, from what you’re sharing, that they’re doing the right things.
Ronald: Okay.
Patrik: So this is how you wean a patient off the ventilator. There’s nothing new in that patients don’t tolerate the CPAP initially, there’s nothing new there. You know? It’s just part of-
Ronald: Okay, there’s nothing alarming about that-
RECOMMENDED:
Patrik: No, no.
Ronald: Okay.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!