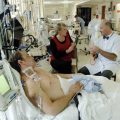
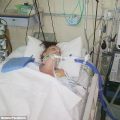
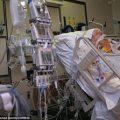
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why is it Risky to Transfer My Ventilated Mom from ICU To LTAC?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Tom as part of my 1:1 consulting and advocacy service! Tom’s mom is ventilated in ICU. Tom is asking why it is risky to transfer his ventilated mom from ICU to LTAC.
How Long Will it Take for My Mom to be Weaned Off the Ventilator in ICU?
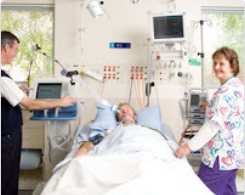
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tom here.”
Patrik: Yeah. I’ll make an analogy here that I think might be helpful. If someone wants to run a marathon, they’re not going to run a marathon by sitting on the couch or sitting on the sofa. I have not seen someone being successfully weaned off the ventilator without training really, and in that instance it’s physical therapy. It’s not going to happen without it.
Tom: Yeah. I know it did increase a bit the last four days.
Patrik: Great.
Tom: Yesterday was like 1 hour, and I think today was like 2 hours.
Patrik: Oh, good.
RECOMMENDED:
Tom: It hasn’t been like that every day since she’s been more alert, so that’s why I was like, 15 minutes one other day.
Patrik: Well, that’s a start.
Tom: Absolutely. Go ahead.
Dad: Patrik, how can we help her with the physical? I was thinking of bringing her a squeezable ball, just so that she can squeeze.
Patrik: Yes.
Dad: I mean, when I’m there, I massage her feet and I move her feet 10 times one route, 10 times the other, and I ask her. I said, “Is the pain more?” She’ll say, “No.”
Tom: It’s not. She says it’s not.
Dad: I try to do a little bit, but I don’t know if I’m pushing too much or what can I do when I’m there the hours that I’ve available to be there.
Patrik: I think that’s a great idea, what you just mentioned there around bringing her a ball so she can squeeze her hands. Just doing light movement of her joints, of her feet, of her ankles, her knees. Just start somewhere. Move her arms. You don’t have to go overboard. Any stimulation after 3 weeks in an induced coma is a bonus.
Dad: I’ve been doing that since we were allowed to go in there.
Patrik: Great.
Dad: Her skin was very dry, so I’ve been taking oils to put on her hands and on her feet, so I’ve been doing this every single day that I’m there.
Patrik: Great, great.
Dad: I was going to bring some of those squeezable things for her to move her hands more so that they’re not so shaky, too, so I will bring that and start doing that with her.
Suggested links:
Patrik: Absolutely. One of the most frustrating things really is that patients after such a long critical illness are so badly deconditioned. It takes a lot for them to recover. The deconditioning side of things is so important.
Tom: Yeah. Well, just maybe another comment or question, and we can close soon and let you get some rest, too. We’re going to do the same tonight until we talk again. How do you suggest addressing or talking with the doctor because the doctor’s notes are continuous within the last three days now saying look for LTAC, with long term ventilator weaning, so how do we approach the doctor then knowing that they’re saying that? They haven’t told us that directly yet, but I anticipate it’s going to come from the doctor soon, knowing that we’re not being very responsive to the discharge nurse.
Patrik: Yeah, so have you spoken to one of those LTACs as yet?
Tom: I’m sorry, spoken to who?
Patrik: Have you contacted one of those LTACs? Have you spoken to someone there that’s in charge?
Tom: No, I have not done that. Should I?
Patrik: Well, maybe you should and get a vibe. Get a vibe. Another good indicator is ask them. Can they set you up with a family that has been in the LTAC and that’s happy to talk to them and see what their experience has been?
Tom: Okay, so you’re talking make a connection with the facility?
Patrik: I would do, and do some online research. Have a look what people are saying about the organization online. I mean, people in this day and age, they leave online reviews.
Tom: Yeah. Well, I’ll absolutely start with that. I just didn’t know if I engaged with them if that’s demonstrating that we’re willing to proceed even though we told them no right now.
Patrik: You don’t need to tell that. I mean, you can just contact them, and the hospital doesn’t even need to. You don’t even need to give your name away. You can make an anonymous inquiry, really.
Tom: Oh. Well, I just figured they’re going to ask me about my mom’s condition and then once I describe it, it’s going to match his call.
Patrik: Yeah. I wouldn’t be too worried about it. Hospitals are busy. Those LTACs are very busy. I do believe you can make an inquiry without giving too much away.
Recommended:
Tom: Okay. I’ll keep that in mind.
Patrik: At the end of the day, they want to do business with you.
Tom: I know. Okay, but anything, any tips on addressing the doctor? The doctor is suggesting LTAC, and she’s ready. What do we say? If we’re like, no, why are we concerned? If we’re going to leave on medical clinical reasoning on why we should stay, but the doctor disagrees, how do we handle that?
Patrik: I would handle it, (A) that you feel very reluctant and very worried for her to go somewhere in such a vulnerable position. You can say that the reviews of LTACs are not great. You can say that you are very concerned of her changing care teams in such a vulnerable condition. You can say things like, “You know, at the moment, the nurse that’s looking after her would have maybe one other patient? It’s probably a 1:2? Is that accurate?
Tom: Where? At where she’s currently at?
Patrik: Yeah. Yeah.
Tom: Yeah, in the ICU, it’s 1:2.
Patrik: Yeah, 1:2.
Tom: I even asked the other day. I wasn’t sure. It’s 1:2, yes.
Patrik: Yeah, so if she goes to LTAC, it will be 1:4, 1:5, maybe 1:10 or 1:8. That’s a massive concern as far as I’m concerned, and they will brush it off.
Tom: Yeah, that ratio.
Patrik: They will brush that off. They say, “Oh, it’s not accurate,” and they know what they’re doing. They will give you every sales pitch they think you need to hear. You can also say that you’re still doing your research. You’re just not ready. Last but not least, I don’t think you should be using that yet, but let’s just say God forbid they’re coming to you tomorrow and they say, “Oh, look. We’ve decided she needs to go to LTAC on Wednesday,” your next step then would be to say, “Well, can I please look at your discharge policy?” The discharge policy will most likely say something along the lines of that patients or families need to give consent to that.
Recommended:
Tom: Okay, and then if we don’t, I’ve already asked you this. We can continue later, but if we don’t give consent, then what happens? That’s where I’m lost now.
Patrik: Yeah. Sometimes what helps is look. I tell you what. I’ll tell you the best case scenario, and then I’ll tell you probably the worst case scenario. The best case scenario is your mom is making progress which will strengthen your argument she should stay where she is.
Tom: Yeah.
Patrik: The worst case scenario is that they’re telling you, “Okay. We’ve decided by Wednesday, by Friday, whatever, she needs to go to Place X.” Then we would ask for the hospital policy about discharges. You could also threaten them with an attorney. You could threaten them with an attorney, and that is often enough to get them off your back, but you don’t necessarily need to hire an attorney. Just you mentioning an attorney is often strong enough to get them off your back for a while. They don’t want to deal with attorneys.
Tom: Good. Just in case that was seriously necessary, what kind of attorney would we reach out to?
Recommended:
Patrik: Yeah. Look. There are attorneys that are specialized on the medical field, not even necessarily medical negligence. I don’t see any medical negligence at the moment, but there are law firms out there. You would have to look for someone, but there are attorneys out there that specialize in the medical field, but I’ll tell you another thing. If they’re really, really pushing you, I would really love to get on a call with the doctors and get a good handle of all that and ask questions to understand more about it and make an argument in front of them saying, “Have you done this? Have you done that? Why are you not doing this? You’re well aware that if you send patients to LTAC that they’re going from a highly skilled ICU to a very poorly skilled LTAC.”
Patrik: Again, for example, if your mom keeps making progress, I think you’ve got all the arguments on your side. I can see. I believe since we started talking, I do believe she is making progress, slowly, slowly, but the Precedex being off. She’s now got the tracheostomy. They need to get rid of the fentanyl. They need to get rid of the fentanyl and hopefully they can then start decreasing the support. Hopefully, once they start decreasing the support, your argument will be stronger, I believe, to keep her where she is.
Tom: Yeah, okay. I’m so glad you put all that in perspective. My goodness. You’ve just informed us tremendously. Thank you, Patrik, on all of this. We’re writing notes and yeah, even just reviewing what you’ve been writing in the email has been really monumental in helping us navigate this. Thank you so much.
Patrik: Pleasure. Just maybe on a final note, don’t be intimidated by them. The worse thing, don’t be intimated by them. Just stake your claim as much as they’re staking their claim.
Recommended:
Tom: Yes.
Patrik: I know it’s easier said than done. I get it. If you don’t ask, you won’t get. It’s as simple as that. If you don’t ask, you don’t get.
Tom: Yes. We’re learning that very quickly. No, thank you, and thanks for helping address our many concerns and worries and just helping even equip us with ideas on how to approach it as it escalates because that’s what I’m having a lot of anxiety about. Okay, I’m willing to do it, but then what do I do next, but you’ve very much eased that this evening, so thank you.
Patrik: Pleasure.
Tom: We’re going to very much be in touch with you, and we may get to that step where we would like you to join a call.
Patrik: I’m happy.
RECOMMENDED:
Tom: I know that you had mentioned previously not introducing you so much as an advocate or a consultant, but we’ll discuss how to introduce you if we have to cross that road.
Patrik: Yeah, exactly.
Tom: But thank you for reminding us that that’s an option.
Patrik: Definitely an option, yeah.
Dad: Okay, we appreciate you very much, Patrik. Thank you for all your expertise and your honesty. We just thank you from the bottom of our heart.
Patrik: You’re very welcome. You’re very welcome. Thank you so much.
Tom: Okay, well, have a good rest of your day or evening, and we’ll be in contact. We’ll definitely fill you in on more as things develop, so you’ll hear from us. It seems like something will develop in the next day or two whether it’s her progress and her condition or them pushing us. Again, something is going to come up. We already know, but we’re much more prepared, feeling a lot more prepared at this point.
Patrik: Yeah, absolutely. Okay, wonderful. Thank you so much, and we’ll talk soon.
Tom: All right. Take care. Thank you.
Patrik: And you. Thank you so much. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!