Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can My Dad with ARDS Avoid Tracheostomy So He Won’t Go to LTAC?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Dustin, as part of my 1:1 consulting and advocacy service! Dustin’s father-in-law is with a breathing tube and on a ventilator. Dustin is asking how they can advocate keeping their dad with ARDS in ICU instead of pushing him out to LTAC.
How Can We Win Over the ICU Team in Keeping Our Dad in ICU Instead of Sending Him Out to LTAC?
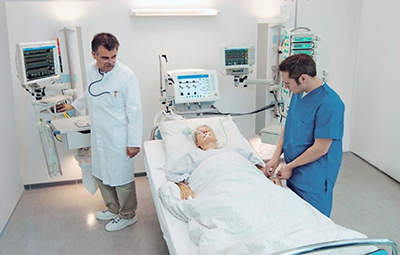
“You can also check out previous 1:1 consulting and advocacy sessions with me and Dustin here.”
Chloe: Right. Yeah, this is … Their daily work routine is dealing with ARDS. That’s what I was trying to give this doctor too. I was hoping to put her in a position where she had to admit that she has no other way to treat him or that he needed additional treatment that she could not provide. And I was clear with that with my stepmother. That was what I was really shooting for. I can’t prove that she can or cannot do what’s necessary for him. But I would’ve liked for her to admit to us, “Hey, I can’t do it. You may need to find another hospital for him.” Which I would have. I would have found something.
Patrik: I guess it would be difficult at the moment I would argue to find another ICU bed somewhere else. Not impossible, but I would argue it would be very difficult at the moment.
Chloe: Right. Yeah, the hospital that I would like him to go to, which has been an hour and a half from here, they said that they could possibly take him, but they said, “Go ahead and get the transfer paper.” The hospital where he is in right now, we have to go ahead and submit the transfer papers. And they may not have something available at the moment. But as soon as one gets opened, he’ll be the next in line.
Patrik: Absolutely.
RECOMMENDED:
Chloe: And they can sustain his life until he could get a spot over there.
Patrik: Yep. Yep. Look, it looks like whatever they’ve done as of today seems … he seems to make some progress. I guess I would argue that over the weekend, you will have an idea where he’s going. Is he heading towards a tracheostomy or not? I do believe that if for whatever reason, he’s not heading towards a trach, I would argue that the conversation around him being terminally ill will come up again. No question.
Chloe: Okay, after this weekend?
Patrik: I think so. That’s what it sounded like to me. The nurse practitioner was saying, maybe for a trach early next week, if it continues like that, if it doesn’t continue like that, I would not be surprised if the whole conversation around him potentially being terminal will come up again. Because where do they go? Where do they go without a trach?
Chloe: Well, that’s what’s aggravating. Instead of calling a terminal, why not just say, “Let’s send him to the best hospital available.” I just don’t understand that. Just let him die versus give him someone else a shot to save him.
Suggested links:
Patrik: Yep. Absolutely. So two things, two things need to happen if he was to go somewhere else, two things need to happen. A referring doctor and an admitting doctor. Those two things need to … well, plus an empty bed.
Chloe: Yeah. Yeah.
Patrik: Plus an empty bed. So those are the things that need to happen. And I would argue that very difficult at the moment. Not impossible, but I would argue it’s very difficult.
Chloe: Okay. So referring doctor and a receiving doctor more or less?
Patrik: And an empty bed.
Chloe: Yeah, exactly.
Patrik: And I would argue that empty beds at the moment are in … Are very rare.
Chloe: Yeah, yeah. I have to agree with you.
Patrik: So then I guess the other thing you got to keep an eye on for now, is that what they’re saying with that all other organs are working is the case almost every day. The reason this is important is, the things … when people are in ICU … Let’s call it for what it is, when people are in ICU, they are as close to death as they will ever be, most of the time, unless someone has been in combat or been in the military or …
Chloe: Sure.
Patrik: Everyday people will be as close to death as they probably will ever be. So you got to keep an eye … It happens very quickly in ICU that the kidneys go off.
Chloe: That’s what I was worried about.
Patrik: Right. So am I. But given that they’re saying he’s not on vasopressors, his blood work seems to be okay. All right. That sounds good. But certainly something that, you need to keep monitoring, liver function is fine, the brain is fine. Heart is … It’s all working at the moment, but got to keep in mind if one organ has failed and the lungs more or less have failed for now, the chances for another organ failing as part of the lungs failing is there.
Chloe: Yeah.
Patrik: And I believe that as soon as that’s the case, as soon as another organ is failing, they will talk about him being terminal again. No doubt about it.
Chloe: Yeah. My main concern is that it’s going to take so long to heal that he’ll end up losing his kidneys by the time it’s all said and done.
Patrik: Look. No, no. If the kidneys are failing, they can pick that up fairly quickly. The first sign of kidneys failing is low urine output. They would be measuring his urine output every hour. So the first time is low urine output. I have no concern that they’re checking their urine output every hour. They’re checking the BUN and the creatinine every day. So I’m sure it will be picked up fairly quickly. I’m not really worried about them not picking it up. But I am worried about that if it does happen that they would say, “Oh yeah, another organ is failing, he’s terminal.” So those are the … those are the things you need to look out for.
Chloe: Okay. Okay. All right. Well, definitely. That’s the one thing I’m definitely … We talked about that before my stepmom. Absolutely. Okay.
Patrik: I can’t, I’m just trying to think … what else? I guess another thing is that if his lungs do deteriorate, would he benefit from proning again? I think he would probably. Again, you’ve got to keep asking the question. Let’s just say, God forbid, he does deteriorate, especially on a respiratory level, and they say, “Oh yeah, he’s …” Again, maybe they talk about terminality again and then your question needs to be, “Okay. Why don’t they prone again?” I know they were talking about swelling in the face.
Chloe: Yeah. That was the excuse last time. And then today it was … once they started improving … like he’s improving, they no longer consider proning necessary.
Patrik: Yeah, sure. And you don’t want to prone on, unless you have to, but swelling in the face from my experience is a byproduct of proning. It’s, you’re turning someone on their stomach, head down.
Chloe: The fluids going up and out of the lungs and into another part of the body.
Patrik: Absolutely.
Chloe: Yeah.
Patrik: It’s a necessary evil.
Chloe: Right. Okay. Okay. Okay. Yeah, because you’d rather have fluid in your face versus your lung. You’re not in the hospital for your face, you’re in the hospital because your lungs.
Patrik: Unfortunately ICU treatment comes with a lot of undesired side effects. Unfortunately that’s the case.
Chloe: Yeah. Okay.
Patrik: This doctor that was in the meeting there, is this the main doctor there? Is she running the show in the hospital?
Suggested links:
Chloe: Yes sir. She is.
Patrik: And there’s nobody else? Sort of she’s the big guru.
Chloe: Right. There’s another one. I haven’t met this guy yet. I was on the speakerphone. We had a meeting with the nurse practitioner. The second day, I couldn’t be there because I was busy talking with another prospective hospital. But they’re from the same clinic. They work together from the same from the same group.
Patrik: Okay.
Chloe: Today we talked to his doctor.
Patrik: Right. Talking about COVID, is your dad COVID negative now?
Chloe: No, no, he’s still positive.
Patrik: He’s still positive. Okay.
Chloe: That was based on a PCR test.
Patrik: Sure. Okay.
Chloe: I hear stories about them oversampling things, 40 times, 70 times, whatever, but … and they’re going to find something if they’re looking. But you would know more about that than I would. I don’t really know what to make of that.
Patrik: Look, some of … Again, there’s so many mixed messages out there about COVID still, but some of the things that I’m hearing is people die with COVID not necessarily of COVID.
Chloe: Exactly. Exactly right. Yeah, it’s not … Dustin has encountered that with his job, and then … We hear it all the time. I’ve seen, and we’ve seen issues with people dying in car wrecks, but they put COVID on … died with COVID, but it was an intersection head on collision that took his life.
Patrik: Exactly.
Chloe: It happens all the time.
Patrik: Happens all the time.
Chloe: I don’t know about over there in Australia, but the way I understand it, our federal government is giving money for these cases. And then you’ll never know the truth about it because everybody’s going to want this free money and they’re going to say and do anything to get it.
Patrik: It’s the same here.
Chloe: Yeah. So we’ve muddied the waters by offering money. We’ll never know the truth.
Patrik: Yep. The same here. The government is handing out money left right and center. And I don’t think it’s the right approach.
Chloe: I agree. I’m sure there’s something out there that’s causing problems, but I’m with you. I just don’t think that’s the way to do it. Everybody’s going to say they got COVID. If you’re giving $13,000 out for positive case, everybody’s got it then.
Patrik: Exactly. Exactly. Well, look, hopefully this COVID thing will be a thing of the past soon, but I don’t think it’ll go away anytime soon. Even with a vaccine, I don’t think it’s going away anytime soon.
Chloe: I don’t know neither.
Patrik: Look, I can’t think of anything else at the moment. I guess we’ve covered-
Chloe: No, yeah.
Patrik: I think we’ve covered both sides.
Chloe: Yes, sir.
Patrik: Trach, probably LTAC, that’s what they want. If it comes to that point … we need to talk about that if it comes to that point, if he’s not improving they will start talking about your dad being terminal again.
Chloe: Okay.
Patrik: Those are the two things that I’m predicting.
Chloe: Okay.
Patrik: Right. And I guess, both sides need to be managed. I need to look it up … When we come off this call, I need to look up this article from this lawyer, and he’s got a very good blog. I need to send you this. I’m pretty sure, unlike in most other places you would probably have very little chance to challenge the DNR unless he’s improving.
Recommended:
Chloe: Okay. Yeah. Yep. That’s the … Dustin and I pretty much should come. And also that idea that that’s something that they can get away with.
Patrik: That’s something they can’t. Yeah, and they can’t get away with it in most cases, but in this situation, unfortunately, it sounds like they can.
Chloe: Yeah. Okay.
Patrik: So, that’s all I can say.
Chloe: Sure.
Patrik: What are your next steps? Are you talking … What are your next steps?
Chloe: Well, the next step is to … I’m very curious to see how this weekend goes, because like you, I believe that’s going to have a huge impact on whether he actually gets the trach or not. And then seeing if actually follow up and do the trach. If he’s improving every day and then they started denying the trach, which I don’t see why they would, then we’re going to have some other issues to talk about with them, but definitely following up, watching his condition either regress or progress, if he gets a trach or not. And then finding out about the PT and OT, the physical therapy, occupational therapy, start looking into that, figuring out … try to figure out where they really are doing it with him or not. That’s the thing. And then long long-term plan on the side of positive, him recovering is looking into this LTAC, while keeping in the back of my mind that they may say this is terminal again. Yes. So …
Suggested links:
Patrik: That’s what I’m predicting. It’s going to be either or. I tell you what I tell you, what is in their head. In their head is, “We need to get him out.” And there’s two ways for him to get him out, either with a trach or letting him die. It sounds blunt, but that’s … Their agenda is they need to get him out. And they have, they have two ways to get him out.
Chloe: Okay. Well, I think the topic of the LTAC needs to come up basically now between me and my stepmother. Just so we’re prepared.
Patrik: Yes. I do argue that you need to bring this up with her stepmother and with your family, so they know what’s going to come.
Chloe: Okay.
Patrik: What I would also advocate for is have a look, what LTACs are in your area and start reading the reviews. Because you will read the reviews and you will see they’re pretty poor.
Chloe: Okay. I will definitely do that.
Patrik: My argument is for someone …A critically ill patient should not have a care episode disrupted. And if you’re going to LTAC, a care episode is disrupted. I believe that is … That in my mind is almost negligent.
Chloe: Yeah. Yeah, yeah. Absolutely.
Patrik: People that have a critical illness, they need a team around them that gets to know the patient and can help them to recover.
Chloe: Yeah. Yeah. I agree. Is there any way to keep them, can you argue keeping him?
Patrik: Yes, you could. Yes, and we’ve done that. We’ve done that successfully. I tell you what the challenge there is. The challenge is that … I believe that ICU is the best place to bring someone off the ventilator, because you’ve got all the expertise. You’ve got ICU doctors, ICU nurses. You’ve got all the expertise. LTAC, there is no expertise from my experience. I would argue, we need to cross that bridge when it gets there.
Recommended:
Chloe: Okay.
Patrik: Yes, there are definitely arguments to be made, but then you have other things like … Physical therapy at LTAC is often better than in ICU, but that’s probably the only thing that’s better.
Chloe: Okay.
Patrik: Right, so …
Chloe: Okay.
Patrik: And, what we could do, if you tell me, “Hey, let’s get on a call at a certain time to talk to the nurse.” I’m very happy to do that. If you don’t want to do that, my advice is call later at night to get more information.
Chloe: Okay. Okay. No, I’m absolutely going to keep that in mind because I know you can get a lot more information, usable information out of them than what my stepmother’s getting, because she’s always just getting these same exact pacifying information, blood pressure, PEEP, saturation. It’s just the same thing. I started writing all this down on a piece of paper when this started and I’m … Always been a big note taker. I’ve done it in my job for years, because there’s so much to remember at work you can’t store everything. I learned that a long time ago. I actually went to her house, over a week ago and brought her a note tablet and throw out, old fashioned handwritten format. When they call you, write it here, your response, your questions, and their response. Because she was the worst about writing anything down. And I would tell, “Hey, well what do they say about this? “Well, I don’t know.'” She would just never, and I told her … I said, “Man, you can’t play games with these people.”
Patrik: As you know, the devil is in the detail.
Chloe: Right.
Patrik: Devil is in detail.
Chloe: Yeah. I kept seeing the same stuff over and over again yet he’s still in there and this is still the same story for weeks. Finally, I just got myself extremely involved. I just, I started pushing her and arguing with her and … It’s been tough.
Recommended:
Patrik: Oh, for sure. For sure. And I guess … As you can see, it’s tough for you and I guess, your stepmother might be a little bit older. She would be completely overwhelmed. It’s overwhelming for anyone.
Chloe: Oh, absolutely, yeah. Absolutely, it is … So yeah.
Patrik: Okay. All right. Well, shall we leave it there for now or do you want to-
Chloe: Yeah. No, no, absolutely. No, I was going to say, I don’t want to keep you too long. And man I have a whole feel of more solid information that I thank you for. Man, you’re really helping us a lot. Again, man I can’t thank you enough because this is … I would have never known about LTAC. You just assume he’s going to stay in there until he’s better, but that’s not the case.
RECOMMENDED:
Patrik: No, no, no, no. Not the case.
Chloe: Yeah. No, no, thank you so much. Hope I’ll be getting some more information and I’ll schedule another call with you again.
Patrik: Yep. And again, if you wanted to get on a call with the nurses at a particular time, just let me know.
Chloe: That’s okay. Yeah, great, great. I’ll do that too. And I hopefully I’ll be in touch with you probably Monday or so give or take depending on what happens.
Patrik: Yep. And if you need me over the weekend, just yell out.
Chloe: Okay.
Patrik: If you need me on the weekend, it’s a 24-hour service, just yell out. I know you might have more time on the weekend. It’s fine.
Chloe: Okay. Okay. Well man, Patrik, thank you so much, man. I really appreciate your time.
Patrik: Oh, pleasure. Pleasure. You’re welcome. You’re welcome. We’ll talk soon. Take care.
Chloe: Okay, have a good rest of your day. Thank you, sir.
Patrik: See you. Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!