Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
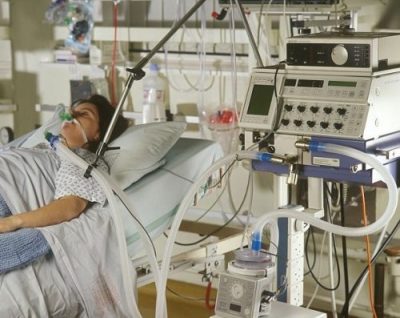
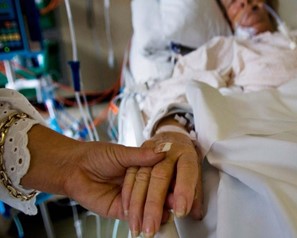
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to share the experience from one of my clients Dustin, as part of my 1:1 consulting and advocacy service! Dustin’s father-in-law is with a breathing tube and on a ventilator. Dustin is thanking Patrik for his guidance. The advocacy & consultancy services from Intensive Care Hotline gave them the confidence to fight for their dad who is suffering from ARDS in the ICU.
With your Advocacy & Consulting Services in Intensive Care Hotline, We Gained Confidence about My Dad’s Fighting Chance with ARDS in ICU.
“You can also check out previous 1:1 consulting and advocacy sessions with me and Dustin here.”
Patrik: You could argue that. Of course, you could argue that. If someone’s state-
Chloe: I was absolutely dumbfounded. I looked at her like she was crazy. And I looked at my stepmother, because I don’t know if she knew about this or not. And I said, “Well, I don’t …” I told the nurse practitioners, “I don’t think you can do that.” And she said, “Well, we have to, because we can’t damage the lungs.” And I was really just dumbfounded. I-
Dustin: And they already told us we’re terminal, that there was no saving.
Chloe: Right. There was the meeting that we had with her, where she told us that he was terminal. So it was really aggravating. I was more mad than upset.
Patrik: Right. Right. Well, nobody said last night that he’s terminal or this morning, your time. Nobody’s saying that he’s terminal.
Chloe: Right. Yeah. Exactly, right. Right, exactly. Now he’s opposite. Now, he’s on the road to recovery.
Patrik: Yeah. I’m pretty sure. I asked the question about the scars in the lungs. I’m pretty sure you both told me yesterday that he had scars in the lungs, but the nurse practitioner couldn’t confirm that last night.
RECOMMENDED:
Chloe: Right.
Dustin: They keep saying damage. His lungs-
Chloe: Damaged. Sure.
Dustin: … lungs are damaged. But they also keep telling us a CT is not needed. That there’s no need for … Did they do it again, just to warn us?
Chloe: Yeah, they told us the same thing this morning.
Dustin: That the CT scan, it’s not necessary.
Patrik: Look, if he keeps improving, I agree that the CT scan is not necessary. If they can keep coming down with the oxygen requirements. If the blood gases are fine, there is no need for a CT scan. I agree with that. Because it’s a risk taking someone for a CT scan, that’s critically ill. It has its time and its place.
Chloe: Sure.
Patrik: But you wouldn’t want to … You wouldn’t want to rush to a CT scan unless you really have to.
Chloe: Okay.
Patrik: What I don’t quite buy is … I’ll tell you what I don’t quite buy. They keep referring to the lungs as the main issue, and I’m not questioning that it’s the case. It’s the main issue, but more often than not in ARDS there’s other stuff happening too. You might’ve heard me asking this morning, I asked issue on vasopressors, which is another form of life support. They denied that, which again is a good sign. They said the kidneys are working. They said the liver is working, with him not being on vasopressors … Vasopressors are usually given for a low blood pressure. And most vasopressors in ICU are given when patients are in a coma because that gets the blood pressure down and vasopressors are also given for low blood pressure during sepsis.
Chloe: And what is this called again?
Patrik: Vasopressor. I’ll send you a link when we come off this call, I’ll send you a link. Okay, great. So given that he’s not on Vasopressors that means his heart is working. His heart is working.
Chloe: Okay.
Patrik: That’s number one. Number two, the antibiotics are probably working for the bacterial pneumonia because if they wouldn’t be working, he might end up with the sepsis that would get his blood pressure all the way down and he would end up on vasopressors. So they are signs.
Recommended:
Chloe: Bacterial infection in the blood can lower blood pressure?
Patrik: Definitely.
Chloe: Okay.
Patrik: A bacterial infection can lead to sepsis. And when patients in ICU end up with sepsis, the first thing you see is temperature, high heart rate, blood pressure plummeting all the way down where it’s life-threatening.
Chloe: Okay.
Patrik: Okay. And that’s when patients end up on vasopressors. And there seems to be no sign of that, which is good. So then you might’ve heard me asking as well. I did ask about blood results. He did say bloods are in order. He did say that the white cell count is okay. Again, the reason I was asking for the white cell count is, the first sign of infection in the blood stream is the white cell count.
Chloe: Sure.
Patrik: If the white cell count is up, it’s a sign there is an infection. Again, if he’s saying the white cells are in order, it means the antibiotics seem to work.
Chloe: Okay.
Patrik: Right?
Chloe: Right.
Patrik: His white cell count at the beginning when he went into ICU would have been probably through the roof.
Chloe: Mm-hmm (affirmative).
Patrik: Right?
Chloe: Right.
Patrik: His white cell count at the beginning of the bacterial pneumonia would have probably been high.
Chloe: Okay.
Patrik: Right. Probably has calmed down with the antibiotics they started.
Chloe: Yes, sir.
Patrik: So those are all positive signs.
Dustin: I heard them saying that. For the last two weeks, even when he was on the other bacterial antibiotics, they said his white blood count has always been low the last two and a half, three weeks. They never indicated high white count. Now in the beginning possibly but that … I thought that was odd too, because I went through that when I was in the hospital and my white blood count was through the roof because of the infection. But they … even on the last couple of checkups in the notes, when we talked to them, they would say that his white blood count was low.
Patrik: Interesting. Interesting. Okay.
Dustin: And they had him on five different bacterial antibiotics.
Chloe: I have a list of all the antibiotics he’s been on and there’s been quite a … I have a list of seven different antibiotics.
Patrik: Right.
Chloe: That, he’s been on.
Patrik: Sure. Okay. Well, okay. You could argue two things. You could argue two things there. If the white cell count is low, you could argue that his immune system is not working 100%. You could argue that. But if he doesn’t have … And again, you wouldn’t necessarily see a temperature. A temperature at the end of the day is a sign that the immune system is fighting an infection.
Chloe: Right, I never thought a fever to be bad necessarily, it’s trying to do its job, correct?
Patrik: Exactly.
Chloe: Yeah.
Patrik: Exactly.
Dustin: And I think he goes off and on. One day he’ll get a fever and then it levels off. And then a couple of days go by, he’ll get a little low grade, nothing crazy. 99, 101, but then it goes back to normal within the same time.
Patrik: Yep. And bear in mind though, what they might be doing with that as well though, is they might be giving him some paracetamol for a temperature job, or they might do some simple things like they might take … they might take the sheet off. Just because it goes down, could simply mean they’re giving him some paracetamol or they’re just taking the sheet off, simple things like that.
Chloe: Sure.
Dustin: Yeah. We figure with his body going through all these medications and waking up from the paralytic that it was going to fluctuate. There was going to be a lot of that, his body getting used to things, and..
Suggested links:
Chloe: Yeah, I never found the fevers alarming really, if anything, I thought it was good news. It’s like his body was trying to survive.
Patrik: Exactly, exactly. That’s exactly right. So I don’t see that as a negative. Okay, well, if his white cell count has never been elevated by the sounds of things, it’s rare. I believe from my experience, it’s fairly rare. I guess all I can say about that is they got to keep an eye on him.
Chloe: Sure. Yeah.
Patrik: So there was no … just from memory, there was no pre-medical history for your dad.
Dustin: Mm-mm (negative).
Chloe: Yeah. Nothing major. Like say, he’s a little overweight, blood pressure and cholesterol. He’s had problems with that, but he’s always kept that control with pharmaceuticals and the things that his doctor prescribed him. But other than that, he’s been fine.
Patrik: Okay. Okay.
Chloe: I can’t remember the last time he’s even been to, or even been admitted to the hospital for anything.
Patrik: Okay. And he’s in his 60’s, did you say?
Chloe: Yes, sir?
Patrik: Yeah. Sure. Okay. All right. I’m just trying to think, what else was there in the meeting. This doctor … where did you leave it? When will you get another update? How has the plan made? Will you get regular updates from this point forward? Because that was a missing link for me.
Chloe: Yeah. They’re to call once, if not twice a week now, whether that’s going to happen or not, again, we’ll see how that plays out. Because this is … of course, I felt like I was fairly assertive today with her and I told her I want to start getting her to communicate with my stepmother and hopefully, that sinks in and it actually happens. By next week, I’ll have an answer on that.
Suggested links:
Patrik: Okay. Sure. If you ring up the ICU now, will you get an update from a doctor, from a nurse? Can you achieve that?
Chloe: Yes. You can get an update from a nurse.
Patrik: Okay.
Chloe: The nurses up in this ICU, COVID where they’re really almost like secretaries. The only thing they can tell you is just his standard vitals. We’ve asked … I had my stepmother ask them some fairly deep questions, nothing too crazy, but certain settings and what and things.
Dustin: And wouldn’t even give us electronic briefs.
Chloe: Yeah, well that was it where the nurse who answered the phone told us he was not allowed to give out the BUN and creatinine levels, the practitioner or the doctor was the only one to give that out, which we later got, but …
Dustin: It’s essentially blood pressure, saturation and ventilation. That’s pretty much the only thing they ever give.
Patrik: Yeah. Okay. And is that because they’re saying you’re not the medical power of attorney, what are the reasons?
Dustin: They won’t talk to her at all.
Chloe: They won’t talk to me at all.
Dustin: Yeah. They’ll only talk to our stepmom.
Chloe: Right. They’ll only talk my stepmom.
Patrik: Okay, because-
Chloe: And I’ve made an attempt to call up there just to see for myself. Matter of fact, I’ve done it twice. Actually, at one time they gave me like very basic model information. And then they asked me to please refrain to just allowing them to communicate with my stepmom only because it was too much for them. They didn’t want to have too many random family members calling in all the time. And I can understand that, people blowing the phones up, but they give you the, “Hey we’re overwhelmed.” Almost like your typical generic news media hype. There’s not enough beds, there’s this … And maybe that is the case. I don’t work up there, but ..
Suggested links:
Patrik: Probably is the case, but that shouldn’t stop them from giving out information.
Chloe: Yeah, right.
Patrik: That’s what it comes down to.
Chloe: You’re exactly right.
Patrik: And some of the hospitals are very good and some of the hospitals are very poor, because if they have a good customer service attitude, if you and I were to get on a call with them, I would get information out of them. I’ve no doubt about it because I would probably ask … I’m a nurse myself. I can talk to them on a nurse level.
Chloe: Sure.
Patrik: I can ask them, “How is your shift going?” I can make them feel good because I’ve been there, done that.
Chloe: Right. Yeah. You can relate.
Patrik: I can relate to them if they’re working at midnight and I get it. But I can also … I can not only relate to them, but I can also ask them questions that are not too threatening, that would be accurate questions to ask for a family. They would want to know. So, I’m happy if you think that might be worth a try. Probably also … I’ll tell you another thing, that I’m sort of finding. If you call them in the middle of the night, you get more information than during the day. Simple reason is it’s usually quieter at night. They’re usually less rushed at nights usually. If you call them at 10 o’clock in the morning, 2:00 PM, hospitals are crazy.
Dustin: Everybody’s calling.
Chloe: Right. Yeah. You’re right. That’s a good point.
Recommended:
Patrik: If you call them, at 11:00 PM, maybe not even … maybe even a little bit later, sort of just before midnight, before they’re having their first break, I find you’re getting way more information. And it’s the same when I used to work in ICU. If the phone rings at midnight … yeah, I might be busy, but I’m not as busy as at 12:00 PM.
Chloe: Yeah. Okay. That’s a very good point. Yeah, you’re exactly right about that.
Patrik: So, we could, or you could, as a next step, I’m very happy we can schedule a call maybe at 11:00 PM your time or whatever it is, or you could try for yourself, but I just think calling at odd hours will give you more information, I believe. It’s at least worth a try.
Chloe: Yeah. Yeah, absolutely. Okay, I’ll keep that in mind.
Dustin: Patrik, is there anything today that you heard that you think that maybe they should be doing that they are not, that you feel strongly about or something, that or you think the track they’re on is where we need to be?
Patrik: Yeah. Look, it sounds like the track they’re on sounds more positive than not what I anticipated after we spoke yesterday before the meeting. Did you say earlier that between the meeting this morning and now, there has to be deterioration? Is that what you said?
Chloe: Yes. A little bit. He had an issue. When they were moving him to his side, his rate peaked up and then I think he started consuming more oxygen. And then his saturation went down to a low 90s. And so they brought the oxygen back up from 72 possibly … I want to say it’s a 100, but he immediately … When they do that, his saturation, it was right back up. He’s at a 100% saturation … 99% right now.
Patrik: So did that happened when they turned him on the side, maybe to wash his back, to change sheets or something like that?
Chloe: Exactly right. Yes, sir. Yes, sir. They were getting ready to bathe him.
Patrik: I see. Look that does happen. My advice on that note and hopefully they would know what to do. If they know that happens, what they should be doing is before they turn him, oxygenate him with 100%, five minutes before.
RECOMMENDED:
Chloe: Okay.
Patrik: All right. And then it may not be avoided, but the risk is minimized I would argue, I remember doing that. You had a patient where you knew when you turn them on the side to wash their back, to change linen, all of that, you would know that they would de-saturate, so you would get them ready for that by giving them more oxygen beforehand to avoid that. Now your dad’s lungs, it may happen even if they do that. I don’t know, but it’s probably … if it does happen well, hopefully next time they’ve learned from it and pre-oxygenate, but that’s what it’s called. The technical term is pre-oxygenation.
Chloe: Okay.
Patrik: Right. It’s a bit of a catch 22, you can pre-oxygenate, and you can also sedate beforehand. Sedation often reduces the risk as well, but then again, you don’t want to give too much sedation either. Sedation again has its time and its place, but your dad is at a point where I believe sedating him would be detrimental to moving him forward.
Chloe: Okay. Yeah. Okay. All right.
Patrik: But coming back to your question, Dustin, should they be doing anything? I did ask last night about the nitric oxide about the epoprostenol and then she mentioned the sildenafil, look, they haven’t done the nitric oxide from what I understand, they haven’t done the epoprostenol from what I understand, it sounds to me like he might be on sildenafil. Do you remember. Do-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!