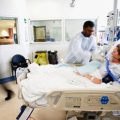
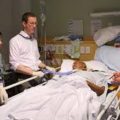
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why is it Crucial to Have Access to Our Mom’s Medical Records While She’s in ICU on Dialysis?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julius, as part of my 1:1 consulting and advocacy service! Julius’ mom is critically ill in ICU due to COVID and he is asking how can he stop the negativity from doctors about her mom.
How Can I Stop the Negativity from Doctors About My Critically Ill Mom in ICU?
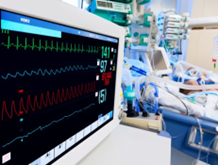
“You can also check out previous 1:1 consulting and advocacy sessions with me and Julius here.”
Emma: Okay.
Ron: She said, “You have to wait until she’s out of the hospital to get it.”
Emma: Yeah.
Patrik: What I’ll do is … I don’t have it right in front of me now, but I’ll send you the … I mean, there’s rules, laws in any state all around the world really, that it’s a right. It’s not a privilege, it’s a right to have access to the medical records. I will send you some stuff there that you can more or less present it to them. What I would do next if I was you, I would just tell them that it’s your right and that you want access to the medical records tomorrow by three o’clock. Just work with a deadline, so they’re aware of your rights. And the other thing-
Julius: And that’s okay, because you know what I’ll call right now? I will call the patient right area, that I’ve been … That’s the only way I have ever gotten any results. And even to get the doctors to talk to us.
Emma: Yeah. Even just to get somebody to come and tell us what’s going on.
Julius: They know about me very well. I must have called them maybe five times now a week.
Patrik: Right. Right. That good. No, no.
Emma: I was concerned, , right? Is that a-
Patrik: I argue, you don’t need an attorney. You won’t need an attorney to get access to medical records because, again, A, it’s a right. B, it’s not only a right under the … I’m just looking it up online as we speak, Medical Records Access Act in the city. And what was I about to say? It’s not only a right, as I said, I’ve never had anyone that couldn’t get access to medical records. But what you’re describing, I’ve seen over and over again. They’re playing dumb.
Julius: Over again. Okay. Yeah. Thank you. Yeah.
Patrik: Right. They’re just playing dumb. And again, what is it that they have to hide? Yeah. The other thing is Freedom of Information.
Julius: Yeah, Freedom of-
Patrik: Freedom of Information.
Emma: Oh, okay. So we can bring that up.
Ron: Yeah. Freedom of Education Act. Right?
Julius: Freedom of Information Act. Yeah.
Patrik: Freedom of Information Act. But is that I’ve just typed into Google, access to medical records in your city, and the first thing that comes up is the Medical Records Act. I can’t just read through it, not right now, but the only thing-
Julius: That’s okay. I can get that now.
Emma: Right. Right. Right.
Julius: I can get that. Yeah.
Patrik: Right.
Ron: Well, we know they’re putting records in every single day. There’s no way they’re not entering something.
Patrik: Well, most hospitals nowadays enter records online or electronically.
Julius: They do.
Patrik: Right?
Julius: Sure.
Patrik: So that’s why I’m saying it’s not even a case of giving you paperwork, it’s a case of giving you access, sending you a URL with a username and a password. That’s what it is.
Emma: That was another thing I found strange because I asked them if they had a flash drive or something digital, why are we doing paper? And they charge you for the paper. And I was like, “What is going on here? What year is this?”
Patrik: Exactly?
RECOMMENDED:
Julius: I you feel like you’re …
Emma: Yeah, weird.
Julius: … like you said, a vacuum there. Because the only other thing I know that I have never set up for my parents was their medical records, is the hospital online. But I do know when we can do the hospital online and the app, it’s the same thing. You don’t get it until … you might get a little bit of her labs maybe, but you won’t get her medical records on that app because they’ll send you to that kind of thing. And I’m like, “Well, that’s great for labs and maybe an MRI (Magnetic Resonance Imaging) or a CT (Computed Tomography) scan“.
Ron: My doctor should be able to call and get that.
Emma: What’s amazing too, they know darn well that it’s a right.
Patrik: Of course they do. Of course, they do.
Emma: And yet they deny you. Yeah. I mean, they know, so how can they do that? If you’re dumb, you just fall for it, I guess. Is that what they’re trying to do?
Patrik: I think they’re trying to keep you at arm’s length. For hospitals, it’s always been important for them to stay in control of the narrative.
Julius: Yes.
Patrik: Right?
Julius: Yeah.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: It’s very important for them to stay in control of the narrative. I mean, you mentioned to me yesterday, Julius, they’re very negative. And your mom is very critical here, there’s no question about that. But they would be negative if she was on 50% of oxygen.
Emma: Yeah. Yeah. They were negative about my mom. We had the same, something like-
Julius: Yeah, my mom has been in too.
Emma: Yeah, she was just in with COVID and she’s back out again now. But at the beginning, it was the same. It was gloom and doom on her.
Julius: Same narrative.
Emma: I thought both my parents are in critical condition. I mean, that’s their narrative. That’s how it goes.
Patrik: It’s all about-
Julius: She didn’t make it up, though. She didn’t get to the ICU, thank God.
Patrik: Right. That’s good. So it’s all about the narrative and the less information they give you or you have, the more in control they can stay off the narrative.
Julius: I did get a list today off the nurse, she was basically … she was whispering all these drugs to me that she’s been on. And I do kind of have a cryptic one. I didn’t get a chance to really look at it, nor did I know if it was really that important. But I kind of did get the low-down on some drugs and what she’s doing for each one of them.
Patrik: Right. Okay. Have you got a list?
Julius: Yeah, kind of. I haven’t really-
Emma: Yeah, we have to write them down on a notepad and ask if it changes all the time.
Julius: I know. And I’m just like, I don’t know. I’m not sure if I got it right, but the Vasopressors, I was trying to wonder what they were doing with the blood pressure.
Patrik: Yeah. Is she on vasopressors?
Julius: Yes.
Patrik: What is she on?
Julius: Something with a Levo.
Patrik: LEVOPHED?
Emma: That’s it.
Julius: Okay. That’s it.
Patrik: Yeah.
Julius: And some vaso, I had.
Patrik: Vasopressin?
Julius: Yes. That sounds right.
Patrik: Do you know how much?
Julius: That’s the question.
Emma: Yeah. You know what-
Patrik: That’s okay.
Emma: … it’s got a readout on the thing.
Julius: The screen.
Emma: I thought she gave it to you. She didn’t give it to you?
Julius: No, she didn’t give me that.
Emma: Oh, geez. We need to write that down.
Patrik: That’s okay.
Emma: Is it milligram? How does it go?
Patrik: Yeah. It depends. LEVOPHED is probably micrograms per minute per-
Emma: Micro.
Patrik: Micrograms per minute per kilo, so per weight.
Ron: Yeah. Maybe if we look at-
Suggested Links:
Patrik: And-
Ron: Mm-hmm?
Patrik: And vasopressin is probably in units per hour. It doesn’t really matter. It’s critical to know that she’s on that. And the reason it’s critical to know is she’s on three mechanisms of life support at the moment. The first one would be ventilation, the next one would be dialysis and the next one would be the vasopressor. So there are three forms of life support, which is basically telling us that, to a degree, three organs are failing at the moment, which is, (A), the lungs.
Julius: Correct.
Patrik: (B), the heart, (C), the kidneys.
Emma: Okay.
Patrik: So that’s certainly concerning.
Emma: What are the pressors? What are pressors? Could you just explain a little bit?
Patrik: Yup. Yeah, yeah. No, I can tell you what pressors are. So pressors, when someone is hemodynamically unstable, which means their blood pressure is not compatible with life, patients in ICU usually have vasopressors, also known as inotropes. So what they do, what the LEVOPHED and the vasopressin are doing, they’re constricting the arteries and the veins in the peripheries to concentrate the blood towards the heart, so the blood pressure that’s compatible with life can be maintained.
Emma: Okay.
Patrik: Right?
Emma: So it’s pressing the blood.
Patrik: Pressing the blood.
Emma: Okay, so pressure.
Patrik: To get the blood back to the heart, because otherwise the blood would just dilate into the peripheries. And it’s a case of really squeezing the veins and the arteries and getting the blood back to the heart, so, again, organs can be perfused. But, again, that’s sort of time-limited … You can’t keep someone on inotropes and vasopressors forever. It’s sort of really an emergency intervention if you will.
Emma: Okay.
Julius: And that was probably back, what, two days ago maybe?
Emma: Oh, when they put her on that? Yeah.
Julius: But then they put her on dialysis.
Emma: Yeah, I’m not sure. And I don’t know if they were on different ones.
Suggested Links:
Julius: That all was starting then.
Emma: I don’t know if she was on different ones either. They might switch them out. I don’t know if there are different ones that they do.
Patrik: Well, there would be other vasopressors, Epinephrine, LEVOPHED, and Vasopressin. They’re the main ones. And Julius, you mentioned yesterday, your mom’s been previously fit and healthy. Is that right? So this comes out of nowhere?
Julius: Correct. Yes.
Emma: Yes. It came-
Julius: It really came out of nowhere, this. Yeah. Because of COVID.
Emma: I mean, other than her age, she was healthy, and once she got sick and this, it’s like everything’s all at once.
Julius: As a matter of fact, I can remember, oh, gosh, the day she went into ICU, she was still in an emergency with really nothing but oxygen. And she was severely dehydrated, very much extremely fragile then, is what they told me. And she had told me, “I’m so glad you’re here.” It was more like an evening. And she said, “They’re going to put me up in the ICU and they’re going to have me on ventilator and Remdesivir. And I went, “What?” But they were-
Emma: Yeah. And I said no Remdesivir because I had heard a million things bad about Remdesivir. But so I felt like that-
Julius: But you didn’t have a … I knew she had to take the Remdesivir to get up to a room. I don’t think a room would’ve been … I think we would’ve been sitting on days two and three without a room.
Emma: She was kind of pressured like, “You must have the Remdesivir or we’re not going to give you any other care.” It was kind of like that.
Patrik: Really?
Julius: I am not kidding.
Emma: I was kind of how it felt. We wanted everything else but the Remdesivir, basically.
Julius: Yeah.
Suggested Links:
Emma: I was cool with every other thing, except that.
Julius: And I got her up in the ICU, and I again had the nurse in the room with my mother when we were talking about, “Is there any other measure?” Because I had a nurse pull me aside when she was in the move to ICU, and she says, “Your mother’s going to be fine. I’m worried about. She’s going to go up to ICU. They’re going to push her with the Remdesivir, and basically, she’s going to die.” And it was-
Emma: Yeah, she was told ahead of time.
Julius: I was told ahead of time. And she says … Now, this is where these nurses can be a little crazy because they are telling us, oh, my God, what’s it? Ivermectin. But see, they don’t know. They’re not the doctor. Right? So-
Patrik: They’re not the doctor.
Julius: So I’m like, “I don’t know if I’m listening to this hearsay.” It’s so bad. I don’t know if it’s bad where you’re at?
Emma: No, it’s not political for us. We just want treatment options.
Patrik: Sure. I-
Julius: It freaked me out.
Patrik: I think COVID is highly political. I mean, if they’re telling you that, “Well, if you don’t take Remdesivir, we’re not going to treat you,” that’s discrimination as far as I’m concerned.
Emma: I know. Yeah. That’s how we felt. Very pressured.
Julius: And I was under the radar on a lot of it, but so I put the hold on Remdesivir, called my sister, and said, “I don’t know what to do.” And now I’m scared as hell. And they’re pushing, “Are you going to take it?” And I’m like, I sat and watched that first bag go through, and within 15 minutes of that bag going through, lo and behold, we had a room upstairs ready. Because they had to, because now … You know?
RECOMMENDED:
Emma: It all hinged on whether she took the Remdesivir or not, which I thought is kind of strange.
Patrik: It’s very strange. That’s very strange. I mean-
Julius: And I got the-
Patrik: You go. You go.
Julius: I got the gold standard in our place, which is U-M, and I actually have the whole plan.
Emma: Yeah. Tell us what you think about that. What do you think about that? I’m curious.
Patrik: What do I think about the whole Remdesivir?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!