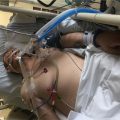
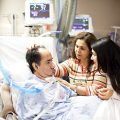
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Do I Know If My Dad Needs to Stay in ICU or Bring Him with Intensive Care at Home?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ronan, as part of my 1:1 consulting and advocacy service! Ronan’s dad is with a breathing tube and is on a ventilator in the ICU. Ronan asks how he can be in control of the ICU team to do everything they can for his dad’s recovery.
How Can I Be in Control of the ICU Team To Do Everything They Can for My Dad’s Recovery?
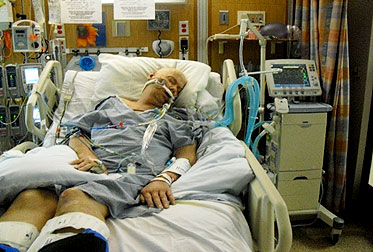
Patrik: So hang on a second. So you are saying there is a doctor looking after your dad that’s working for the health insurance? You should go to the media with this.
Ronan: Well, he’s not technically, but I’m sure there’s…
Patrik: Maybe a shareholder. Excuse my cynicism.
Ronan: No, I hear you. So I can keep delaying the trach I guess. I mean, I have to approve the trach.
Patrik: Okay. Okay. Let just go one step back here. Sorry.
Ronan: Okay.
Patrik: The reason I’m asking this is I’m having similar conversations multiple times a day, like with yourself. And I know what hospitals are saying. Hospitals are saying, “Oh yeah, by next week you have to make a decision.” And I’d just go, like… If a hospital was to come to me, the hospital could tell me, “Jump off this bridge,” and I would just go like, “No. Sorry. I don’t.” And I would respond the same. Your dad has been ventilated more than a month.
Ronan: Yeah. Right.
Patrik: So today it’s on the 17th day. So yeah, I can see the cutoff is sort of the 10 to 14 day mark. I can see why a trach is an option. What I would want to know is as a clinician, I would want to know what his ventilator settings are? What are his arterial blood gases?
Ronan: Currently it’s 20. The O2 is 30%. The PEEP is five and then 10 or something is 400.
RECOMMENDED:
Patrik: Yeah. That’s not enough information. That’s probably just 50 percent of the… Probably not even 50 percent of the information. You need ventilator settings, you need arterial blood gases, you need chest x-ray results, and you need neurological assessment. And that’s the biggest challenge for families in intensive care. They don’t know what they don’t know. So when someone is in a situation like your dad, you’ve probably told me a good 30 or 40 percent of what’s going on, but I’m still missing the other 50 or 60 percent what else is going on to really have a complete picture. I have half of the picture.
Ronan: Yeah. I have his chest x-ray on CD.
Patrik: Sure, sure. But I still probably have half of the picture and I would want to know what medications is he on. I would like to talk to a clinician to find out what are the other 25 things that are going on that they haven’t told you about.
Suggested links:
Ronan: Yeah. So I’m happy to hire you for the week. Do you do consulting live?
Patrik: Yeah, I do that. Yeah. I can do consulting live with the doctors or whoever you want me to talk to. I’ll tell you something. So hospitals are very, very good to pretend they’re operating in a vacuum. They’re very good at that. They tell you, “Yep, you have to make a decision until mid-next week. If you don’t make a decision by that time, all hell will break lose.” Well, no. That’s not going to happen. They are dependent on your approval. They are dependent on your consent. Yes. Look, they work with deadlines. Sure. The doctors work with deadlines that they might get from the health insurance that they might get from the hospital CEO. We know all of that, but it’s your dad. Your dad is not dependent on hospital deadlines.
Ronan: Yeah.
Patrik: I’ll tell you something. If the health insurance was to ring you tomorrow or Monday and says, “Hey, Ronan, your dad is running out of entitlements, that’s when I would get worried.” Not when the doctor tells you.
Ronan: Okay.
Patrik: Not when the doctor tells you.
Ronan: Okay.
Patrik: How can you verify? Just because the doctor tells you, you got to make a decision by next week. How can you verify that’s accurate? You can only verify that’s accurate if you actually talk to the health insurance.
Ronan: That’s true. So do I… Sorry. I said, I keep on saying I haven’t made a decision and I have. I’m still processing, and so I just keep…
Recommended:
Patrik: Absolutely. Absolutely. So I tell you something. Your dad, let’s just say worst case scenario. Let’s just say your dad does not wake up by next week. They will push you.
Ronan: Well, he’s awake, but you mean in terms of cognitive?
Patrik: Yeah. Cognition, cognition.
Ronan: When he follows commands.
Patrik: Follows commands or is doing something. Let’s just say he’s not waking up by next week. They will say to you, “Okay. Make a decision, Ronan. Let’s do a tracheostomy or move him to hospice.” Okay. You may do that. Okay. Let’s just say, hypothetically, you wait another two days and he wakes up, right?
Ronan: Yeah. Just wait?
Patrik: That’s why for them, for the hospital, the hospital wants to sell you a one size fits all.
Recommended:
Ronan: I know. But how long can I drag this?
Patrik: It’s a very good question. What I can tell you is this Ronan. At the moment with COVID, hospitals are waiting longer and longer for tracheostomies, which is probably a result of demand. It’s a combination of demand for beds and also minimizing the risk for staff to get infected. Because doing a trach on a COVID patient is highly risky. Staff can get infected. So at the moment I’m talking to clients, they are in ICU, day 30, still on a ventilator with a breathing tube. No trach has been done mainly because of COVID.
Ronan: Right.
Patrik: Right? So I’m not… Look, I do believe you should not wait much longer than day 20. I am all for that. But I believe you got to look at the unique situation of your dad, which means he’s not waking up. And coming back one step. If your dad didn’t have a brain injury, went into ICU for pneumonia, two weeks on induced coma, and he wasn’t waking up after day two, I wouldn’t be worried. So now you have the combination of a prolonged induced coma and the head injury and he’s not waking up. So there are patients in ICU that come out of prolonged induced coma, no head injury. It takes them two weeks to wake up and their brain is intact. So now you have your dad, brain is not intact according to CT scans, and you’ve got a prolonged induced coma. I believe it’s irresponsible to say to you, “By next week, you have to make a decision. I believe that’s irresponsible.” And they haven’t told you about wake up times for critically ill patients.
Ronan: Yeah. Okay.
Patrik: Right?
Recommended:
Ronan: Yeah.
Patrik: And unfortunately, Ronan, again, the hospitals are very good putting pressure on you and “Yeah, you got to do this and you’ve got to do that.” And I’d just go like, “Okay.” I’ve seen too much over the years to know that, yeah, you can work with deadlines. Yeah. You can have the health insurance saying, “Yeah, he needs to be out of ICU in two weeks time.” Well, the good news is patients recover or don’t recover in their own time.
Ronan: I know.
Patrik: No matter what the perceived deadlines are and…
Ronan: So I should just… I can drag this out as long as insurance will let me?
Patrik: I almost believe you have to drag this out. If by next week, your dad is awake and maybe can make… I don’t think he will be.
Ronan: I don’t think so either.
Patrik: But let’s just say he’s awake by next week. The ideal scenario I believe is where he’s in a position where you can ask him questions and he can make his own decision.
Ronan: And so is it okay that they’re no longer doing the CPAP trials?
Patrik: Say that again.
Ronan: So they were doing CPAP to see if he could… But they’re not going to do it anymore.
Patrik: Oh, why not? Why not?
Ronan: Because they don’t think he is going to… He lasted two and a half days on one and then he lasted eight hours and then they took him off. But they think because he can’t protect his airway.
Patrik: Okay. Okay. Okay. So great question. Do you know if he’s breathing on CPAP as of now?
Recommended:
Ronan: He was today. Yeah.
Patrik: Okay. Good.
Ronan: They took him off to let him sleep tonight.
Patrik: Yeah. Okay. Very good information. Very good information. So if he’s breathing CPAP he has a very high chance of coming off the ventilator, even though he may not be able to protect his airway.
Ronan: Right.
Patrik: However, if he can breathe spontaneously, but can’t protect his airway, he will need a trach but no ventilator.
Ronan: Oh, okay. Interesting.
Patrik: So therefore they should not stop the CPAP trials at all.
Ronan: And how do I get them to keep going?
Patrik: Again, I believe let’s get on a call with them.
Ronan: Okay.
Patrik: But at the end of the day, you, as the medical power of attorney, I believe that in your location, families have actually way more leveraged than here, for example, because it’s sort of a privatized system. I had a client last night, he calls me up and he says, “Hey, this is what’s happening with my mom. Should I be asking them for another CT scan? We looked at the labs and what not. I said, “Yeah, probably.” So I rang them up. We said, “Look, can we have another CT scan?” And they did that. That would never happen here. Would never in a million years happen here in Australia. So I do believe that because the way the system runs, I do believe families have a lot of leverage.
Ronan: Okay. So I should ask them to continue. Okay.
Patrik: No matter what, until you’ve made a decision, Ronan, I do believe he needs to have every opportunity to improve. Every. Until you’ve made a decision, you should push them to do everything that they can unless you think your dad would decide otherwise.
Recommended:
Ronan: Well, I think the CPAP is not… Yeah. I think the trach is more I don’t know. But the CPAP I think is… I was kind of surprised and maybe I’ll get the nurse he had today. Some of the nurses I really get along with. And so they’ll chase down the respiratory therapist and have them do it. So yeah.
Patrik: The other thing that I can see Ronan is… And I can see it with other clients too, unfortunately, in a situation like that, it’s not black and white. It’s not a simply, “I would do a trach.” “We move to hospice.” There’s so many variables.
Ronan: I know there’s so many grays.
Patrik: Right? There’s so many gray areas. And I do believe a lot of it comes down to your values, to your beliefs, to your ethics. As much as I can guide people and can help them, I am not here to make a value judgment on what you decide. I’m here to guide you and say, “If you do this, this is what it most likely will look like down the line.”
Ronan: Yeah. You’re just trying to help me interpret all the stuff that they tell me.
Patrik: Exactly. Exactly. And also make you aware of your rights. You do have rights. It’s not by next week the hammer will fall. No, no.
Recommended links:
Ronan: I just am… unfortunately, I’m a pleaser, so it’s hard for me, to say, “I haven’t decided.” And they try and pressure me. It’s horrible.
Patrik: Yeah, of course. Of course. Of course. I get it.
Patrik: This morning I did an interview with a man who lost his wife in ICU last year. And they were basically euthanizing his wife. He had no idea. He only found my blog way down the line and then he realized, “Oh my goodness. What’s really happened?”
Ronan: No, your blog has been amazing for me this far, in terms of understanding. And you saying no PEG and that I can separate trach and PEG. And yeah. So I love that. Thank you so much for doing that.
Patrik: Oh, thank you. Oh, please.
Ronan: And for sharing all of that. So, yeah. I would love for you to get on a call. So the attending… I would like to do… I would ideally like to do it tomorrow, but the attending that I currently have, there’s a new one coming on early next week and she’s much more sympathetic and much more detail-oriented than the person you would talk to who is covering my father currently. I don’t think the current one will be very open or helpful, unfortunately. But we can try if you want. And then we can try again with… If she doesn’t give you the information, try again next week.
Patrik: Yes, I’ll tell you what the best approach is there, Ronan talking to them. The best approach is I would not share with them you’ve hired a consultant or advocate.
Ronan: Oh, no. I’ll just say a friend.
Patrik: You might just say family friend. Otherwise they might get defensive. But if I was you, if you are dealing with a doctor that is, like you said, is affiliated with the health insurance, I would call them out on it because there is a clear conflict of interest. Clear conflict of interest.
Ronan: I don’t know if they are, but it just feels like it.
Patrik: Oh, right, right.
Ronan: Right. So, because everything has to run through them in order to be covered. They have to submit… For home health insurance coverage services, they have to approve it.
Patrik: Right. Right. And look, the other thing you could do, Ronan, if you really want to go down the track of home health care, you should be talking to some companies…
Ronan: Yeah.
Patrik: Right. You should definitely be talking to some home health care companies that could potentially do some end-of-life care or hospice care. You should definitely do that. Keep your options open, but don’t be pressured. Do not be pressured.
Suggested links:
Ronan: There is a palliative doctor. So he has given me different home health care… Like if I do go to the hospice route that I’ve started exploring because here government insurance takes care of hospice. So literally you tell them you want to do hospice in the morning, and in the afternoon, all the equipment shows up, like the bed. It’s crazy. But yeah, I am trying to… I would love to drag this out and just give her a bit more time.
Patrik: Yeah. Yeah. It needs more time. It needs more time. And Ronan, I need to run in a minute.
Ronan: Okay.
Patrik: What I might do Ronan, is I’ll send you some of the options that I have available. Starts with an hour, goes all the way up to two week options.
Ronan: Yeah, I’ll do the one week and then upgrade to the two if we…
Patrik: Always upgrade if you need to.
Ronan: Yeah. And I’m happy to do it tonight or…
Patrik: So you let me know. You let me know.
Ronan: Okay.
Patrik: I’ll send that to you in a minute and then go from there.
RECOMMENDED:
Ronan: Okay. And so typically what’s a good time for you to conference call?
Patrik: Tell me, when would you like to schedule a call your time? Tell me.
Ronan: So I think they’re going to harass me tomorrow and maybe give me more data. So if we could chat again tomorrow afternoon or evening my time.
Patrik: Yep. Yep. That’s good. That’s perfect. Yeah.
Ronan: Yeah. And then early next week, by Monday with the attending, the new attending, who can give you the information, the download on her probably around like 1:00 or 2:00 my time if that works?
Patrik: Yes. Yes. Yep. That works for me. Yes. That works for me. Yep.
Ronan: Okay. Wait. So should I just email you the times to confirm?
Patrik: Email times. You’ve got my number in my signature file. You can always call.
Ronan: Oh, wow.
Ronan: Okay.
Patrik: Yeah.
Ronan: Wonderful. Great. Well, I appreciate your time and look forward to our partnership on this.
Patrik: Pleasure. Pleasure. Looking forward to talk to you tomorrow. Take care.
Ronan: You too. Bye.
Patrik: Take care. Bye. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!