Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from my client Steve and the question last week was PART 5 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of my clients Veronica, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
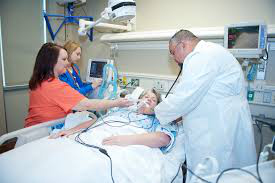
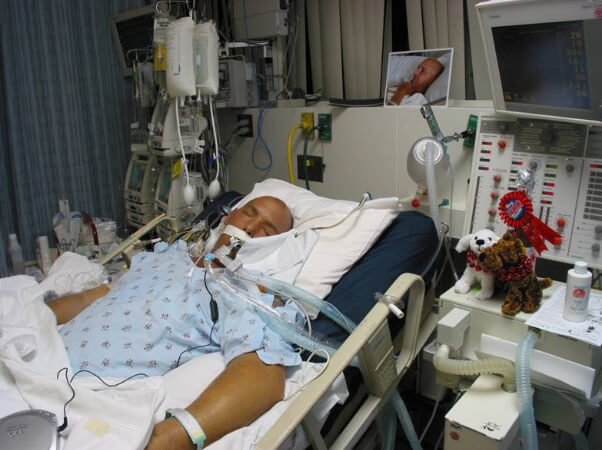
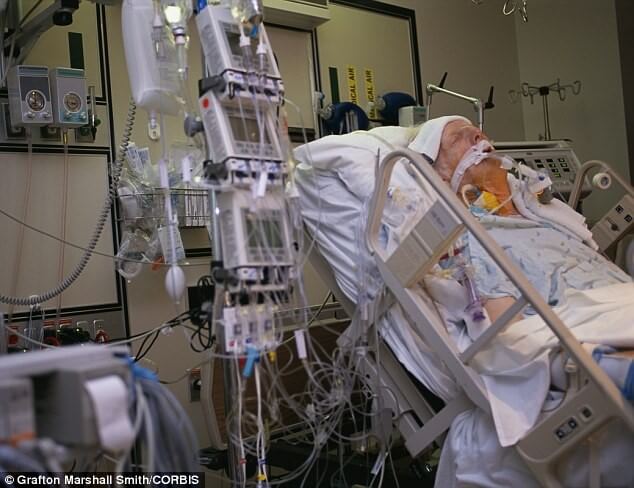
My Dad (71) is in ICU with stage 4 lung cancer & stroke, he’s on the ventilator now and in an induced coma, what are his chances of survival? (PART 1)
You can also find previous counselling and consulting sessions with Veronica here
PART 2, PART 3, PART 4, PART 5, PART 6, PART 7 , PART 8 and PART 9
Hi Patrik,
My dad is 71 he is in Critical care and last night we (Me, my Mom and my brother) were asked by the ICU doctors to decide if dad deteriorated further if we wanted to option one make him comfortable and he may not have made it through the night
or
Option two let the doctors put him into an induced coma and on the ventilator/respirator.
Related article/video:
Option 2 is where he is now and I’m so scared that my dad at his age and with his complications that he was admitted into hospital 8 days ago of lung cancer stage 4 complication of fever and infection and Pneumonia. He has been on treatment for 2 years for his cancer. And he has now rapidly deteriorated since admission to hospital after they did a bronchoscopy on his day 2 of admission.
Since he’s been in hospital he’s had further complications :
- Infection
- Virus
- Pulmonary oedema
- And stroke.
Any advice would be welcome.
Many thanks
Veronika
Recommended:
Hi Veronika,
thank you for sharing more about your Dad’s situation and thank you for being a client and using my 1:1 phone and email counselling and consulting service, I highly appreciate it!
A few more questions to get further clarify your Dad’s situation
- Have you or other family members ever discussed with your Dad what he would want in such a situation? Does he even have an advanced care directive?
- Are you his medical power of attorney/ Next of kin(NOK) and do you have decision making authority
- Do you know if he’s on any inotropes/vasopressors? Inotropes/vasopressors are intravenous medications such as Adrenaline/ Noradrenaline given for low blood pressure and they are considered life support and therefore can only be given in Intensive Care/Critical Care under monitoring
- What cancer treatment was your Dad on? I.e. Chemotherapy, Radiotherapy and/or did he have surgery for the cancer?
- Did he deteriorate after the Bronchoscopy and do you know if it was a factor of the deterioration?
- With your Dad’s pulmonary oedema, have they given you a reason why? Do you know if he also has a weak heart or do you know if he has kidney failure? Both might lead to pulmonary oedoma.
- You mention your Dad had a stroke. When did he have the stroke, this week? If he’s had a stroke they must have done a CT of the brain, do you know the results of the CT brain?
I hope my questions don’t overwhelm you, but the devil is in the detail and the more information the better and the better advice I can provide.
This is a complex situation but that’s what most situations in Intensive Care/Critical Care look like and I will need to break it down for you so that you understand what’s really going on and how you can manage it.
Kind Regards
Patrik
Recommended:
Hi Patrik
thank you for your reply
My father is being given noradrenaline because he has low blood pressure the nurse just told me.
Yes, we have discussed his situation briefly and I am his power of attorney as his daughter. He has given instructions years ago about his advance care to mum and I.
My father was having chemotherapy then immunotherapy and then back to chemotherapy. He had his cancer diagnosed October 2014 and had his right lower lobe of his lung removed in Feb 2015. He was on his 3rd line of treatment awaiting another trial drug due to be available around May.
Yes, I do believe he deteriorated after the bronchoscopy it was meant to be quick and he has been in Intensive Care/Critical care since and the pulmonary oedema occurred the day after the bronchoscopy and then they said he has a weak heart at about 35%. We or he was never told about his weak heart before even the ICU doctors said they did not know this.
He suffered a stroke in Intensive care on Thursday morning, his cancer specialist said it happened because they were withholding the blood thinners after the bronchoscopy. They then said he looks like he would make a near complete recovery from his stroke the day of it and after it, because he retained the strength in his arms and legs (left side was effected) his left side of face and his swallowing and talking is the issue so yesterday they put him on a feeding tube at 1pm and he went downhill fast after with a fever and a new infection.
I saw him just now and we are waiting for the CT scan results of his head they did test this morning.
I will request copies of his tests also.
Thank you for your thoughts and time.
Veronika
Hi Veronika,
Thank you for your reply.
With your Dad having given advanced care directives to you and your Mum, what are those directives? Are they clear for Intensive Care/ Critical Care treatment?
Sometimes it’s very difficult to give advance care directives for situations that may or may not occur in Intensive Care, because at the end of the day, you don’t know what you don’t know…
Also, even though a health professional might explain procedures, treatment etc… in Intensive Care for you, unless you have seen it many times, you don’t really know what it means. It’s really important to understand the pros and cons of all of the options laid out to you.
As you can probably see by now already, most questions that arise when being treated in Intensive Care/Critical Care are not simple “Yes” and “No” answers but they require an evaluation of a much bigger picture.
Here are my thoughts with the information that you have given me thus far.
I do believe that you have made the right decision by putting your Dad into an induced coma and on a ventilator.
Simply because you want your Dad in a position where you have a say what might happen next. If they had stopped treating him yesterday, you would have lost control immediately.
If I was you, I would wait for the CT brain results and make every decision from there.
If his heart is “only” functioning at 35% they would be referring to his ejection fraction(EF), which is how strong the heart is beating. If it’s 35% it’s fairly weak and I’m not surprised he went into pulmonary oedema. A weak heart is unable to cope with all the fluids going through the heart, therefore the heart is decompensating and fluids are pushing into the lungs, hence pulmonary oedema or “water in the lungs”.
Also, as far as the infection is concerned, it’s probably a side effect from the Chemotherapy/Radiotherapy. I would also be asking for his white cell count and his neutrophil count.
I would also suggest that we get on the phone ASAP as we are just scratching the surface here. I have worked in Intensive Care for nearly 20 years and you simply don’t know what you don’t know… I can “hand-hold” and guide you through this “once in a lifetime” experience that you don’t want to get wrong…
I can help you with asking the right questions so that you can always make an informed decision, get peace of mind, stay in control, keep your power and influence. Keep in mind that the Intensive Care team is “managing” families of critically ill Patients 7 days a week/365 days a year and they know what to say, they know how to say it and they know what not to say…
There is a lot at stake on your end as well as from the ICU end. You want to get the best outcome for your Dad and the ICU wants to limit expenses and keep the stay in ICU as short as possible. Keeping the ICU stay short might also mean pushing for an early withdrawal of treatment which could ultimately lead to your Dad dying in a time frame that doesn’t align with your time frames.
Recommended:
By getting your Dad in an induced coma, on a ventilator and on Inotropes/Vasopressors for his weak heart you have bought him precious time to see if he can recover or not.
Yes, stage 4 lung cancer is most likely life limiting but you don’t know how much time he’s got left and by buying him this precious time you can give him more time.
Being aware of those dynamics is important and it help you getting bargaining power in what you want for your Dad!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!