Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from my client Veronica and the question last week was PART 4 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Veronica, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
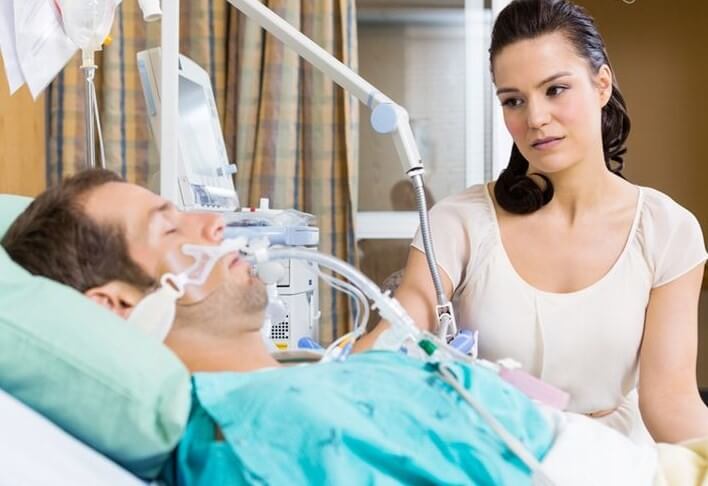
My Dad (71) is in ICU with stage 4 lung cancer & stroke, he’s on the ventilator now and in an induced coma, what are his chances of survival? (PART 5)
You can also find previous counselling and consulting sessions with Veronica here
PART 1, PART 2, PART 3, PART 4, PART 6, PART 7 , PART 8 and PART 9
Patrik: Veronica, how are you?
Veronica: Hi, I’m okay. How are you?
Patrik: Very good, thank you.
Veronica: Excellent. Thank you for taking my call tonight.
Patrik: Oh, you’re welcome.
Veronica: I spoke with the new intensivist, that they’re in charge. Another new person again.
Patrik: Yup.
Veronica: And, his name’s Ben.
Patrik: Right.
Veronica: And, he seems fantastic.
Patrik: Okay, good. I’m so glad to hear that.
Veronica: The nurses and everybody praise him and they reckon that he’s one of the best ones that they’ve got there.
Patrik: Good.
Veronica: He’s only just come on duty today, but he knew dad’s case inside out. So.
Patrik: Right, right. And, over the weekend did you end up dealing with Professor xxxxxxxxxx, or whatever his name was?
Veronica: No, I didn’t really need to. It was like very briefly, just in passing and he said that he hadn’t decided if he was going to give dad the scan on his lungs or the ultrasound. And, I didn’t want to rock the boat, and I just said, “Do you think it would be a good idea?” And, he said, “I’ve been thinking about doing it, but probably not til after Easter, around Tuesday.” And, I thought that’s a very good idea, thank you. And then, yesterday, they did do the scan today.
Patrik: So, they did the scan today?
Veronica: They did the scan today. And, unfortunately not very good findings at all. Sorry. Sorry, go ahead.
Patrik: So, over the weekend they’ve given the steroids?
Veronica: Yes, so they ended up giving the steroids the whole time. So, instead of just the three days he’s had it for five days, and now they’re slowly looking at weaning him off the steroids because … So, this is what this Dr. John xxxxxxx wants to do based on the findings from the ultrasound that was done today at about 2:30pm. But, he hasn’t been able to consult with the oncologist or the respiratory professor yet.
Patrik: Yup.
Veronica: But, he doesn’t think there’ll be much more. They did everything, he believes, because of the new finding. So, on the ultrasound and the CT scan they found that, he said they can’t actually distinguish between these three things. He said there is inflammation. There is damage on the lungs. And, there is also cancer growing. And, he said that it looks much worse from his last scan, which was done on the 3rd of April. And, to top it off dad also now has in the lower lobe of his left lung a blood clot, which he believes has come from his legs while he’s been in sedation, even though they have been giving him the-
Patrik: Clexane
Veronica: Yes, it still formed and he said that’s not a good sign. And, so they’ve increased that today because of the new findings.
Patrik: The Clexane, mm-hmm (affirmative).
Veronica: Yup, they’ve increased that and he said that he thinks himself that if dad breathing on his own now, but the machine, they’ve got the tube. They’ve got him sedated and in the induced coma, and that is helping to basically with the initiation, not with the initiation, it’s helping the breath.
Related article/video:
Patrik: Yup.
Veronica: To make sure that, yeah. But, he said that if they keep dad sedated longer in his condition with his lungs, they can’t do a tracheostomy, that they call it. They can’t do that, he said, because he doesn’t look healthy enough to have that done. So, that’s why I needed to talk to you.
Patrik: Yeah.
Veronica: And, he also said that he still told us he hasn’t had a chance to talk to the others about it, and we’re all meeting together as a family tomorrow with the oncologist himself and then by then they will have spoken with the respiratory professor. But, in his opinion, he believes that they’ve exhausted everything else now and they keep testing the mucus and everything that they keep extracting every two to three hours and he said that there’s no new findings on that either. And, the antibiotics that they’re giving dad they still, yeah, for nothing. He hasn’t responded to any of it.
Patrik: Okay, so that’s basically suggesting the infection is still there.
Veronica: Yes, he said there’s three different things, and they can’t distinguish from the scans whether it’s just mucus, whether it’s cancer that spread that much, but it’s so much inflammation.
Patrik: Right.
Veronica: And, he said it’s progressing really fast. He said, if it’s the cancer, if it’s the inflammation, if it’s the damage, it’s progressing really fast and he believes that, without consulting the oncologist, that he believes that it is the damage from the chemotherapy that’s taken its toll on dad’s lungs.
Patrik: Anymore talk about the surfactant? Remember you brought up last week-
Veronica: No, none at all.
Patrik: No more talk about that?
Recommended:
Veronica: Nope, no more talk about that. And, he said what he would like to do, he believes that dad is going to keep deteriorating being in an induced coma and it might be harder for us to bring him back because more and more other conditions might worsen for him. And, he said already with the high dose steroids that dad said he’s concerned about him too weak to be able to, you know, he just said he didn’t want to become too weak in his hips and everything else from the steroids. So, he said he would really be able to like to be able to take the breathing tube out and let dad breath on his own, sit him up in a chair, get him a really good mask that he said there’s another option of a whole full face mask that dad could use. And, let’s see if we can actually get him out of ICU with him breathing on his own, and then let’s make the next call.
Patrik: Before I go into what I can see, what are your thoughts about that proposal?
Veronica: Myself?
Patrik: Mm-hmm (affirmative).
Veronica: With the oncologist not being there to sort of defend himself, the oncologist already did say that he thought himself that the damage to my dad’s lungs was from the cancer drugs too. And, he said it normally happens earlier on, not at the end. So, I think that they’re pretty much on par, and because dad has so many other things going wrong. And, yeah things aren’t looking the best for him that I would prefer that they wake him up too and he said that weaning him off of the Fentanyl, as well, cause they’ve been giving him some of that as well.
So, he stopped that today because he said that that would make it harder for dad to be able to cough himself, because now they’re not gonna be able to give him suction. They said he’s got to stop the Fentanyl. They stopped it this afternoon, and he said he’s going to have obviously issues with scratching and breathing, you know, all that stuff. And, he said he may not be able to talk for a few days cause it’s gonna be really hard for him and they don’t know how he’ll be because of the stroke as well that he’d had before they sedated him. So, he thinks he’ll still need the feeding tube, but he should be able to breath on his own as to for how long, we don’t know.
And, how I feel about it all is that, yeah I guess I would like to see dad woken up, and then that way, you know, we can see where that takes dad.
Patrik: Right, have you brought up the other treatment options that I sent to you last week? Do you remember when I sent you those treatment options?
Veronica: Yes.
Patrik: Did you bring that up with any of them?
Veronica: Yes, I brought that up with the oncologist, Dr. xxxxxxx, and as much as he’s on our side, he sort of smirked a little bit and said, to be honest, he said, if the steroid therapy doesn’t help to reverse it, the other things won’t help because he said he thinks it’s from the immunotherapy drug that dad had for 18 months that had caused the damage. He said it leaves these pockets and scar tissue where the cancer was.
Patrik: Yeah, yeah, yeah, yeah. Okay. Look, and he would have seen the side effects of that drug before having said all of-
Veronica: And he has, yes.
Patrik: Yeah, I’m sure he has. He would be the expert on the side effects of that drug. Having said all of that, with the inflammation and the pulmonary fibrosis, no matter what course, you know as I said in the email with the treatment options, there’s plenty of patients that I see with pulmonary fibrosis that get that treatment. Irrespective of what caused the pulmonary fibrosis in the first place, right? And, he’s probably right that whichever drug he had is causing the effect.
The question then needs to be raised, okay, I call it what the intensivist refers to as a “one- way extubation”. I don’t know whether he mentioned that term. A “one-way extubation” basically means removal of the breathing tube, and what he’s referring to is we extubate, we take the breathing tube out, and we put your dad on a mask, but we’re not going to put the breathing tube back in. So, that’s an ICU term that’s sort of referred to as a “one-way extubation”.
Now, I guess the question really needs to be raised that on the one end they’re saying a tracheostomy might not be, you know, he might not be well enough for that. So, here is my view on anybody who’s being considered for a tracheostomy. I’m all for trying to take the breathing tube out first, before you do a tracheostomy, if you can do that. Now, in some cases you can’t do that for a number of reasons. But, it sounds to me like in your dad’s case that might well be an option. Take the breathing tube out and sort of see what happens.
Veronica: Yes.
Look out for the next episode where I discuss with Veronica whether her Dad should have a tracheostomy or not!
Many thanks& Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!