Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from my client Steve and the question last week was PART 4 of
You can check out last week’s episode by clicking on the link here.
You can also find PART 1, PART 2 and PART 3 of this series of questions
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of my clients Steve, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
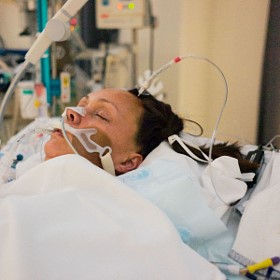
My 73 year old Mom had a stroke and is intubated in Intensive Care. She can’t come off the ventilator and the breathing tube, can she have a tracheostomy and go home and have INTENSIVE CARE AT HOME? (PART 5)
Steve continues with his mother’s situation below
Hi Patrik,
here’s what’s been happening in the last 48 hours.
Even though we initially thought that my Mom is definitely going to die and that we have to let her go, we have still been having second thoughts!
Well, I think at some point we’ll have to make that decision it just seems a little sudden for the rest of the family. So, we’re still not sure if we should agree to stop everything and let her die!
I don’t want to draw it out any further but we did, as a family, want a second opinion. I actually spoke to a lawyer and she advised me this. Then I asked to speak to the medical director of the ICU, on another lawyer’s advice.
The medical director of the ICU has agreed to treat her fully until we get the second opinion. The lawyer shared similar views to you and she went through a similar ordeal with one of her family members. Thanks for following up, it is tough and we are prepared for what will happen but I suppose it’s still important to make sure we won’t let her die without having tried everything. One of the more junior ICU consultants wanted to discontinue her life support tomorrow morning on grounds of futility.
Related article/video:
I also took your advice about my mother not suffering as far as we can see. We think that as long as she’s not unduly suffering we want everything to be done until we are 100% clear that nothing can be done to save her!
She just lies there peacefully and she seems in no pain whatsoever and she’s also not moving!
I also did some research last night about Hyper Baric Oxygen Therapy. I asked one of the ICU consultants about this he said it’s not valid due to the level of damage in brain. What is your opinion on this. Is this something that could’ve been used after my mother’s initial stroke?
Many thanks
Steve
Recommended:
Hi Steve,
no matter how much “prepared” people are, this is a very tough decision to make!
I’m sure you have come to terms that your mother may not recover.
If she’s not suffering you may get second thoughts about stopping life support and that’s only natural.
If you and/or your family want to continue life support you need to discuss with the ICU consultant and you have done this already.
If you want that you need to find a reason why and your reason why, is that you have no trust in the Intensive Care team. Given that they were ready to let her die on her first admission to ICU and she recovered during that admission and given that she was able to come off the ventilator despite the ICU doctor’s dire and negative predictions, you have no reason to have faith in their words.
You have by now realized that ICU teams have agendas that go way beyond your mother’s diagnosis, her prognosis, as well as her care and her treatment!
You know by now that what’s happening “BEHIND THE SCENES” in Intensive Care is way too powerful to be ignored and you know by now that it impacts on your Mom’s care, treatment etc…
Related article/video:
Would you rather have your mother going somewhere else, either another ICU or are you still thinking of taking your mother home with INTENSIVE CARE AT HOME, where she could pass away peacefully in the comfort of her own home, surrounded by you and your family?
It’s a very good alternative to the “one size fits all” approach to dying in Intensive Care!
Related article/video:
The good news is you are already one step ahead of the rest of the 99% of the families of critically ill Patients in Intensive Care who don’t make informed decisions, don’t have peace of mind, control, power and influence!
You have left no stone unturned and the Intensive Care team knows that you are not taking everything you have been told as “face value” and they know that you question everything! Well done!
It’s very healthy for you and your family to keep standing your ground and keep standing up for what you want for your mother, she couldn’t be asking for a better advocate than yourself!
It’s really important to stay sane and staying in control of your mental and psychological health is very important. Withdrawing treatment prematurely whilst you and your family are having second thoughts may have negative ramifications for the rest of your life. You need to do what feels right for your Mum and most of all you want to make informed decisions, get peace of mind, control, power and influence!
It’s also advisable for you to have a look at the following article/video below that we got from a reader a while back and this lady was getting second thoughts when it was actually too late for her mother!
Related article/video:
I also think it’s good that you are talking to lawyers to find out what your options are. Just by you doing that and informing the Intensive Care team about it, is usually often putting them on the backburner because they don’t want to have the lawyers coming to their ICU!
Again, congratulations for going to such great lengths and making sure the Intensive Care team is not doing anything that you and your family don’t feel comfortable with!
You want to make sure you are doing the right things during this “ONCE IN A LIFETIME” situation that you know you can’t afford to be getting wrong!
As you know by now and as you know from your mother’s previous admission into ICU, the biggest concern the Intensive Care doctors have is to treat a Patient for an indefinite period of time with an uncertain outcome.
That’s why they are so quick to withdraw or stop treatment often in a heartbeat, because of their perceived limited resources.
People who are unaware of the dynamics in Intensive Care often agree to let their loved one die in Intensive Care prematurely, without having explored all options!
The most important ingredient for a successful recovery in Intensive Care is often time, nurturing and the creation of a positive environment. Most Intensive Care teams are under so much pressure, whether it be financial and also lack of beds, that once again, they are ready to prematurely “sell” families on a “withdrawal of treatment” for their critically ill loved one! If you are getting “sold” and you agree to a “withdrawal of treatment” you are basically agreeing to let your loved one die!
It’s highly unethical, whilst by the same token, 99% of families of critically ill Patients in Intensive Care are not doing their own research and therefore they make no informed decision, they have no peace of mind, no control, no power and no influence!
You and your family on the other hand have taken responsibility and you have left no stone unturned and the Intensive Care team knows that you are in a position of power!
You know by now that when the ICU consultant is referring to “futility of treatment” and that he wants to stop treatment on the grounds of futility, you know that there is a difference between “real” and “perceived” futility of treatment!
Related articles/videos:
Furthermore, it never harms to get a second opinion, because once again, you have no reason to trust the Intensive Care team after they were ready to let your mother die on her first admission to Intensive Care and you and your family however kept standing up for what you wanted for your mother, which ultimately saved her life on her first admission to ICU.
Recommended resources:
Next, you have also asked if your mother should have received hyperbaric therapy for the stroke when she was first admitted to Intensive Care a few weeks back.
The answer is a clear yes, especially since hyperbaric therapy was available in the hospital your mother was at.
It would have certainly increased chances to get your mother awake more quickly.
It’s too late now because of her not being awake and sustained brain damage, but as we discussed, they never informed you about this option in the first place, which is disappointing.
And that’s why it’s so important for families in Intensive Care to do their own research, to question everything, to not take anything for “face value” as well as hiring someone like me who can help them with getting what they want so they are not becoming a victim of the system!
That’s it for now Steve, you’re doing well and you are doing all the right things to leave no stone unturned.
Wishing you and your family all the very best!
Kind Regards
Patrik
PS: Steve’s Mom passed away a few days later, but not without Steve and his family trying everything within their power to make sure there wasn’t anything they were missing.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



