Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from my client Veronica and the question last week was PART 1 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Veronica, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
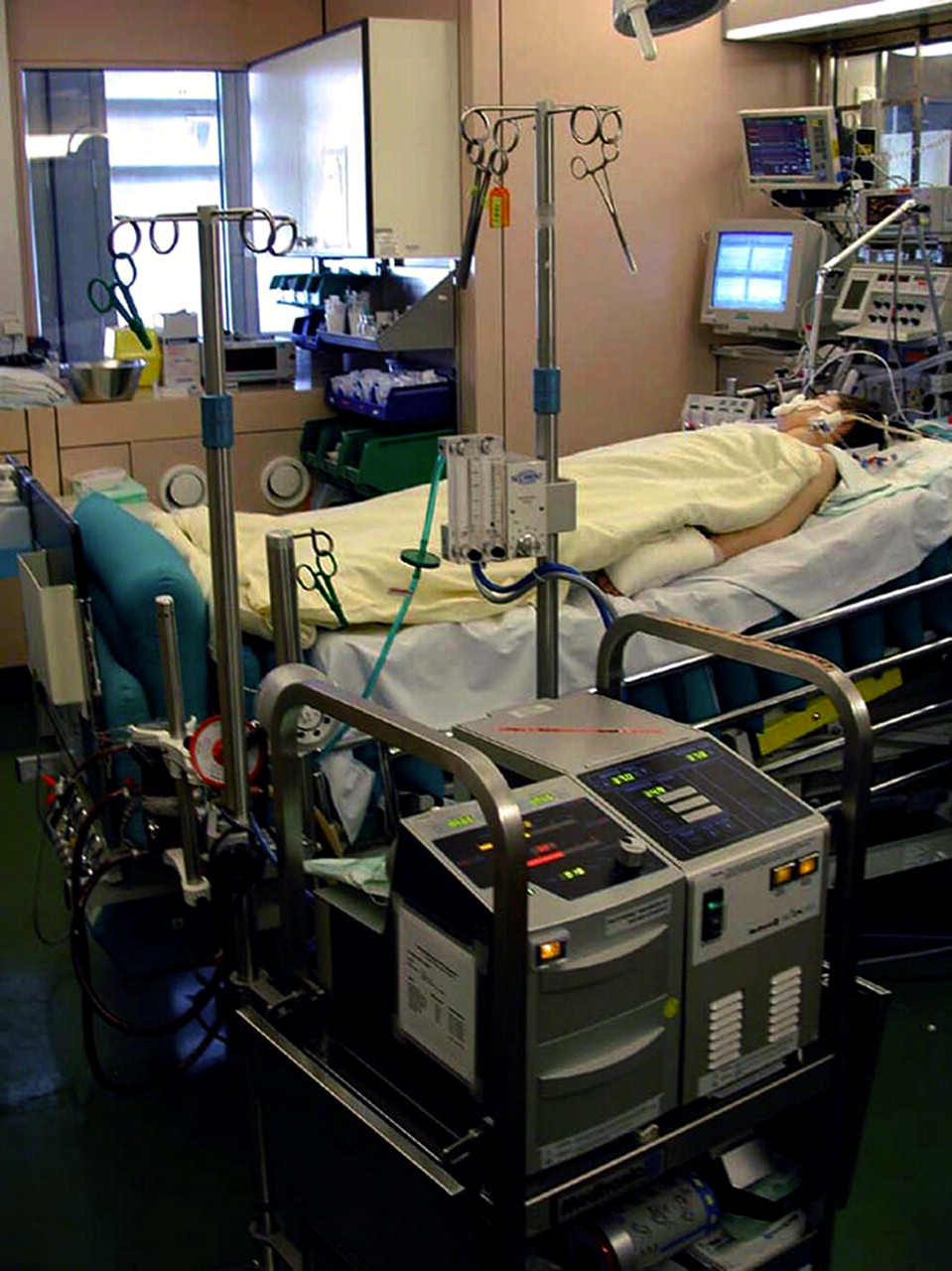
My Dad (71) is in ICU with stage 4 lung cancer & stroke, he’s on the ventilator now and in an induced coma, what are his chances of survival? (PART 2)
You can also find previous counselling and consulting sessions with Veronica here
PART 1, PART 3, PART 4, PART 5, PART 6, PART 7 , PART 8 and PART 9
After I had the first phone counselling and consulting session with Veronica, I send her a summary of the consulting session and you can find below how things progressed from there
Hi Veronica,
It was nice talking to you, I hope the information I gave you was helpful.
Please follow up with the doctors on
- What sedation is your Dad on besides the Fentanyl? Is he a) on Propofol which is a short acting sedative or is he b) on Midazolam a long acting and also addictive sedative
Here is more information about sedation in ICU in general
http://intensivecarehotline.com/sedation/
Next, ask them why his ejection fraction has gone down to 35%. Have they ruled out a heart attack?
In order to investigate if he had a heart attack, they would have to
- Check the Troponin levels in his blood
- Do an ECG
- Do the Ultrasound/echocardiogram or even do a TOE (=transoesophageal echocardiogram)
Next, ask them if he’s getting any anticoagulation besides the Aspirin. He may get some Clexane (Enoxaparin) or Heparin for anticoagulation (=blood thinners).
Also, keep asking for blood results such as Haemoglobin, Platelets, White cell count, Neutrophils etc… If Neutrophils <0 he needs to be isolated. Especially after Chemotherapy, the immune system is weakened and therefore white cell count (WCC) and/or Neutrophils may go down significantly.
Hi Patrik,
Thank you so much for your advice and information last night. I have emailed you to reply to the questions that I had to find out from the hospital and doctors.
I have made a lot of notes and called all the relevant doctors today who are responsible for my father’s care.
Please see my answers below to the questions you said I should ask the doctors about from your summary email:
I called xxxxxxxx Critical Care the consultant Dr Steven H said this morning that my Father is on Propofol and he said we need to be prepared for a hard week with more tough decisions. He also said he was not going to be at the hospital this week as he swaps shifts with xxxxxx hospital and that another Doctor a Professor xxxxxx will be looking after the xxxxxx Critical Care this week including my father and he was doing a hand over this morning.
He said Dad is on a medium dose of heparin and aspirin.
My father had an echo done of his heart.
I also forgot to tell you that my father is on thyroxine (his thyroid burnt out after the first lot of chemo over 18months ago.
I contacted my dad’s GP who is personal friends with my father through years of dad and mum being his patients. His GP was not fully aware of the whole situation since it got even more serious 2 nights ago. Dad’s GP happens to be good friends with the appointed cardiologist (he trained with the GP) as well as the cancer specialist Dr xxxxxxx is friends with the GP. The GP said the cardiologist said his heart should come back to normal once the infection and the Pneumonia that caused the fluid on the chest from the chemotherapy settles down.
He said the cardiologist wants to repeat the echocardiogram when the heart recovers on its own if it is stress related (which is what the cardiologist thinks) if it does not improve it could have been a heart attack, he said there is no suggestion from the eco that was done on 31/3/17 of previous scarring but the heart remains globally weak.
I called the cardiologist Dr xxxxxx he spoke to me at length and said he wants to repeat and echocardiogram once the heart recovers on its own probably this Wednesday or Friday. He said he did not want to risk an angiogram as my dad had blood on coughing before he had his bronchoscopy.
He said if the next echocardiogram is normal he will put it down to stress myocardiopathy. He said he will try to avoid an angiogram for 6 months. He said dad’s heart refraction is in keeping with viral and stress myocardiopathy. He said dad will need to recover totally to be able to have an angiogram.
He said further treatment for the heart artery would need dad’s oncologist Dr xxxxxx to consult and state that dad has a 12 month or more life expectancy. He said he they are giving dad Perindopril an ace inhibitor to treat his Blood Pressure to calm the system. He said he cannot have Beta Blockers at the moment. He said he looked at the chemo drugs dad has been on and he said they are not causing the weak heart.
He believes that dad has heart stress, or very unlikely had a heart attack at home at some point but no markers lead toward that he said and that has resulted in his weak heart. He also said he thinks that dad might have aspirated and that has caused the recent Pneumonia and further complicated the situation and that is why he needed to be sedated also. (no one has confirmed the aspiration to me) the cardiologist said he would be seeing dad this evening.
Once again, he said do not worry about his heart he thinks it’s the lungs that are the concern. I asked him have they ruled out a heart attack and he said No. I then asked him why his ejection fraction has gone down to 34% and he said from that report he said he has not ruled out a heart attack however he said he believes it was unlikely to have been one as his Troponin levels in his blood were in the 100s not in the 1000’s. I requested the echo report that was done after dad had the pulmonary oedema. He is going to investigate further with the other eco but due to risks will not risk doing an angiogram.
I now have a copy of the echocardiogram that was done on the 31-3-17 if you need any details please let me know.
After work I visited dad at the hospital this afternoon and asked the nurse on his duty shift about his bloods, she said his white blood cell count is up slightly but lower then yesterday, his haemoglobin is down slightly. His fever is completely under control, and I asked for blood reports but no one was around that could give them to me so they said if I ask in the morning I should be able to get them then.
This next part is very important: When I said hello to my dad he responded and put his hand up and opened his eyes.
Now, my father is under sedation in the induced coma but the nurse said he is responding to questions. I spoke to dad and he is listening and able to answer my questions by nodding and squeezing the hand. Is this safe and ok? He indicated he is not in any pain, and on one occasion he opened his eyes to see me. I am concerned he is aware of too much what are your thoughts please?
Also, the nurse said this is not very common to be so responsive with the sedation. I hope he is not too aware and not in any pain. Is this good or not good? Do I need to speak up to the doctors for him, the nurse said he is not resisting to the ventilation so they are not too concerned.
Thank you for your advice again and please let me know where to from here and if I need to obtain more information and what I should know daily and what to ask for from them.
Many thanks
Veronica
Recommended:
Hi Veronica,
Thank you for sharing all this very useful information!
You have already done a crash course in Intensive Care/Critical Care and I can see that you are a quick learner!
It’s good to hear that your Dad is on Propofol and not Midazolam (Versed). Propofol is short acting and therefore, once Propofol is stopped, Patients tend to “wake up” a lot quicker, sometimes within minutes or hours.
Midazolam (Versed) is long-acting and therefore it takes a lot longer for Patients to “wake up” after the induced coma.
Therefore, I’m not surprised that your Dad is responding to you and your family and those are all very good signs.
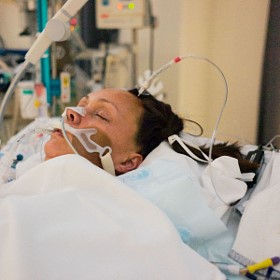
Generally speaking “waking up” after an induced coma is more like switching on a light with a dimmer, rather than switching on a light with a switch. “Waking up” after an induced coma is a process and not an event.
I have written about this extensively here
It’s also positive to know that your Dad is responding especially since he had a stroke a few days back!
As far as the doctor’s comment is concerned about “making tough decisions” in the next few days, my advice is to ignore any negativity for now and keep asking questions.
Intensive Care teams are negative by default and whilst I agree that your Dad’s prognosis is poor, negativity is not going to help anyone but the ICU who wants to manage their financial budget, manage their beds, staff as well as their medical research interests.
Related article/video:
Furthermore, if his Troponin levels are in the 100’s it’s unlikely that he had a heart attack, although they haven’t ruled it out yet. I think they are just cautious, which is fine.
Also, if your Dad has an aspiration Pneumonia, there is a very good chance he might have aspirated during the Bronchoscopy.
You clearly noticed a deterioration after the bronchoscopy from what you shared yesterday on the phone.
This is probably also why they had to intubate (=insertion of the breathing tube) him and put him on the ventilator within the next 24 hours.
With stage 4 lung cancer and an aspiration Pneumonia, the prognosis will be poor going forward. However that doesn’t means your Dad can’t come off the ventilator over the next few days, you have to wait and see.
Therefore I also agree that the lungs are the problem and not so much the heart. The reality though is that you can’t look at either the heart or the lungs in isolation. Lungs and hearts are connected and they rely on each other to function properly.
Moreover, please also keep in mind that his White cell count (WCC) as well as his red blood cells and Haemoglobin levels are probably going down because of the side effects from the Chemotherapy.
Furthermore, I agree that a Beta Blocker like Metoprolol would be contraindicated and even though you haven’t mentioned it, your Dad is most likely on Noradrenalin/Norepinephrine or any other inotropes/vasopressors to maintain a physiological blood pressure and cardiac output (=contractility of the heart) whilst he has a compromised ejection fraction (EF).
The goal you should be working towards is to make sure your Dad is not suffering and that he’s getting the best possible care and treatment until he might come to a point where you can ask him what he wants.
If he doesn’t reach that point, you then need to make decisions on his behalf and it’ll be good for you to think it through what you want for him. We can discuss this on our net phone call.
Because I have seen this situation hundreds if not thousands of times after nearly 20 years Intensive Care nursing experience in three different countries, I can tell you what’s going to happen next.
The ICU doctors will probably ask you to agree to a “withdrawal of treatment” as being “in the best interest” for your Dad as he won’t have much time to live.
At the bare minimum they will ask you to sign an “NFR” (Not for resuscitation) or “DNR” (Do not resuscitate) order in case your Dad’s heart stops.
Again, I wouldn’t do any of it because you want to wait until your Dad wakes up so you can ask him what he wants.
Usually what pushing towards a “withdrawal of treatment” or an NFR or a DNR means is that the ICU is really pushed for beds or they are running out of money and they frame it as if it was “in the best interest” for your Dad because he wouldn’t have any quality of life anyways.
The most important thing in Intensive Care is to read between the lines and understand the dynamics and what it all means. What’s happening “BEHIND THE SCENES” in Intensive Care is so powerful that you need to understand it rather quickly and you can do so here.
It’s also good if you can have a look here to learn about “withdrawal of treatment” as well as NFR and DNR
Furthermore, cardiologists always want to do angiograms because that’s their bread and butter, but I do believe at this stage until they have evidence for a heart attack or if ejection fraction deteriorates further there is no need for that. Also, your Dad probably won’t need another procedure at this stage.
For now, stay put and wait until your Dad is getting more wake so you can ask him what he wants.
Do not respond to any pressure from the Intensive Care team. You are in charge of your Dad’s fate and destiny as long as he’s alive, because you have all the right information at hands.
With the Propofol coming off, he should get more awake and having said all of that the Fentanyl might make him sleepy and might make him drowsy to the point where he won’t breathe enough to come off the ventilator.
He will most likely need the Fentanyl for pain relief and therefore he may not be able to come off the ventilator, but it’s too early to see what’s going to happen next!
Wishing you all the best!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!