Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkin’s Lymphoma and is currently experiencing decrease in blood count as well as having second thoughts about the treatment her sister is getting.
The Intensive Care team is wanting to stop or “withdraw treatment” against Andrea’s and her families wishes and she’s not prepared to let her sister go without a fight!
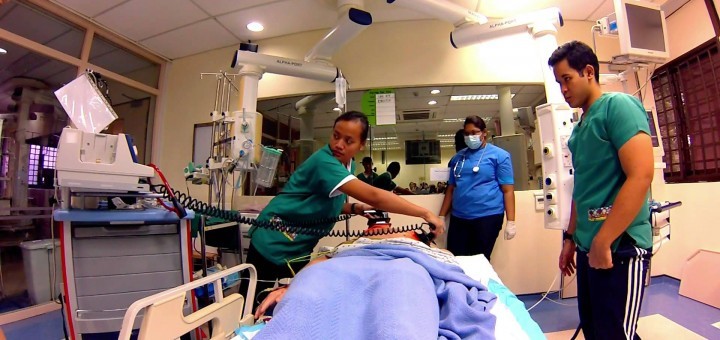
“A Family Conference revealing the hidden mistreatment and delayed management of a dying patient in the ICU.”
“You can also check out previous 1:1 consulting and advocacy sessions with me and Andrea here.”
Dr. Miller: Sure, sure. Are you abreast with what’s happened to….
Patrik: From what it looks, Andrea has told me, I guess, I’ve got bits and pieces but I don’t have the bigger picture from a medical perspective.
Dr. Miller: Sure, okay. Look, okay, so, I just want to first start by saying, I’m very sorry-
Andrea: No, you’re not.
Dr. Miller: … that I…
Dr. Charkow: From what it becomes, we are very sorry.
Dr. Miller: We’re very sorry. Your sister is dying. I mean, really dying, as in she’s coding. So, coding means that she-
Andrea’s Mother: Come again sorry?
Dr. Miller: Coding meaning that her brain has become critically swollen and is now starting to herniate through the base of the skull and she’s progressing to a condition that I would refer to as brain dead. So, she’s going to become brain dead in a matter of hours, if not already.
Andrea’s Mother: How do you know?
Dr. Miller: So, we do that by clinical testing in conjunction with the scan that we have done this morning.
Andrea: Have you got it done this morning?
Dr. Miller: Yes, yes.
Andrea: And what do they say?
Dr. Miller: They show that she’s got massive herniation from a stroke, that lesion she had in the brain causing pressure on the rest of the brain. That wasn’t evident on her scan from last week.
Andrea: And what’s going to happen?
Dr. Miller: Good question. It’s probably getting so, it’s probably, look, I mentioned to you at the beginning of the week while we’re presumption that this was a stroke, with haemorrhage in it but the way it’s behaving I would be suspicious that it’s not just a stroke. That it could be tumour that’s expanding.
Recommended:
Andrea’s Mother: Okay, going back.
Dr. Miller: We don’t know that.
Dr. Miller: A CT scan may help, but a CT scan is not going to help at this point. As I talked to you before, the stroke was the only thing that may potentially have been reversible. She had progressive strokes.
Andrea’s Mother: Can we talk, please?
Dr. Miller: Hmm?
Andrea’s Mother: Can we talk, a day before she’s come here? She said, “Mum, they gave me to much radiation. They gave me too much drugs.” As I had talked to Diana before she has come here.
Dr. Miller: It is not the radiation that gives it. The radiation was to control her symptoms. It was her choice to have radiation.
Andrea’s Mother: Yeah.
Dr. Miller: She had a choice of options-
Andrea’s Mother: But not a lot of radiation.
Dr. Miller: The radiation did not do this. She just deteriorating further and the rest of her condition.
Andrea: Doctor Joshua Miller isn’t it, is it true that chemo radiation from the neck to the head to the chest, increases her chances for a stroke in a first time 5 years?
Dr. Miller: It increases vascular risk but she only had radiation to the chest.
Andrea: But that still increased the chance of the stroke? Chemotherapy is the deep root cause right?
Dr. Miller: Look, this is not the…
Andrea: I understand what you are saying.
Recommended:
Dr. Miller: Radiation will increase vascular risk…
Andrea: She had radiation last year.
Dr. Miller: It’s not something that happened within 12 months. It does not happen in 18 months it’s a long term brain affectation.
Andrea: And do we have clinical studies to back it up?
Dr. Miller: Yes. There are plenty trial studies I read. That was one of the discussions I had with your sister in the beginning, that there are limits to radiation, how much radiation people can take and what are the reasons you could weigh. What chemotherapeutics we can keep and control what radiation she had already had.
Dr. Miller: She unfortunately had herniated the brain. That has been discussed before. It could be a stroke, the way it’s behaving, it’s looking more like a bleed. There’s nothing I can do in the brain. A stroke in the brain there’s nothing else we can do. She was on blood thinners; she’s going to bleed she’s progressed severely. There is nothing else we can do.
Dr. Miller: I have already told you, this is the time she needed a blood transplant. But, there’s nothing that we could do that was going to cure her.
Andrea: Not in even your medical reach? I trusted you!!
Dr. Miller: There is nothing that is going to help. We are at the end stage. This is the end of our work.
Andrea: I know.
Dr. Miller: This is the end. Okay.
Andrea: Then, how come she was not given blood transfusions. I’m very angry about this and the blood products. I am very angry about this. The blood platelets are very low and under your care and under haematology she did not receive any blood.
Dr. Charkow: Can I answer that question? This has got nothing to do with her platelet count being low. This progression of disease would not have changed.
Andrea: But you agreed at that moment. No, no, no no.
Dr. Charkow: Yes, plus I know clinically she has lumps in her neck which weren’t there last week.
Andrea: Okay, how do you know those were lumps?
Dr. Charkow: It’s swelling….
Andrea: You really know huh? I know she was gonna die because, she was with you.
Dr. Charkow: No. She’s untreatable because she has end stage lymphoma. We cannot treat her anymore.
Find out more about recovery and dying patients:
Andrea: But you don’t know that for a fact.
Dr. Charkow: I know that for a fact. There is no-
Andrea: How? Give me the evidence?
Dr. Charkow: There is no other treatment. I regret that this has happened but people die of lymphoma.
Andrea: I know they die of lymphoma. You know what, they actually die out of the treatment of lymphoma.
Dr. Charkow: No-
Andrea: There is immunotherapies, there radiotherapy, it’s all in front you. Then why does everyone, you have cancer, have chemotherapy. Why isn’t other alternative explored and if you walk around…. Let me just say this. When you walk around all the cancer centres the buildings are beautiful and yet…. Why’s that? Who’s spending the money there? It’s sure not the government.
Related article/video:
Dr. Charkow: We’re movin now…
Andrea: Well now that’s my personal opinion.
Dr. Charkow: That’s your opinion that’s fine. Listen, if we had not treated Diana in 2016, she would have died then. She was about to die at that point.
Andrea: That’s right but then you know what, I regret that other options were not explored and I would have never gone down to chemo and radio and other treatment. The other day, one of your staff said that this costing you lots of money. That’s disgusting for you to say that!!
Dr. Charkow: Can I explain that?
Andrea: No!!
Dr. Charkow: I explained it. That….
Andrea: Your juniors are the one caring for you.
Dr. Charkow: Because even… I told you, I told you-
Andrea: Sorry, and another point.
Dr. Charkow: Yes.
Andrea: If you do not make a formal report about this hospital. I will make a formal medical complaint!!
Dr. Charkow: Fine, fine.
Andrea: You don’t answer to this hospital, you don’t answer to the Premiere, you don’t answer to the seniors, the board, and to this people’s commonwealth, you don’t answer to the health minister of New South Wales. Who do you answer to? God? Cuz you definitely do not!!!
Dr. Charkow: Where are you picking that up?
Andrea: And you said “I will not resuscitate her, you should jump on the bed and resuscitate my sister”. That is absolutely disgusting to say that.
Recommended:
Dr. Charkow: I did not say that.
Andrea: You did so. My sister was there.
Dr. Charkow: She said it herself?
Andrea: And you were there too. You did so say that.
Dr. Charkow: That is not true.
Andrea: You are the ones choosing the care for half of your patients, not the family members who to jumps to save their sister!!
Dr. Charkow: Your sister….
Andrea: Did you say that?
Dr. Charkow: Your sister was dying.
Andrea: It doesn’t matter. Did you say that word?
Dr. Charkow: And it’s not-
Andrea: Oh, no, no. I want you to answer that question. Did you say those words?
Dr. Charkow: What did I say?
Andrea: “I will not resuscitate her” and you said you will not resuscitate her and you should do that, you can go and jump on her and resuscitate her.
Dr. Charkow: I don’t recall saying that.
Andrea: Of course you do.
Dr. Charkow: But I did say that I wasn’t going to resuscitate her.
Andrea: And you can jump on the bed.
Dr. Charkow: It’s medically inappropriate to try to resuscitate someone who is in a stage of 3. We have….
But it doesn’t mean we could help. I appreciate, I’ve seen your complaint and we will address the complaint effectively what we hear today. Let’s talk about the patient and where the patient is today and I know you’re extremely angry and I know you’re extremely upset be today, we need to look at, really, your sister’s position in-
Related article:
Andrea: My sister’s condition could end.
Dr. Miller: Let’s get back to what we’re dealing with, let’s get back to what we’re dealing with and where things are and what now. Let’s deal with that.
Andrea: And they killed her.
Dr. Rosebud: Let’s deal with what we’re dealing with right now.
Dr. Charkow: We didn’t kill her. I’m not going to accept that. This is the end stage of the disease.
Dr. Miller:: Okay, we know you’re upset. You don’t know if the cancer had spread-
Andrea: Without a PET scan. I want a PET scan.
Dr. Charkow: I do not need a PET scan for this. We can’t do a PET scan now because number one-
Andrea: No, no, no. You’re not saying that.
Dr. Charkow: It’s not going to help.
Dr. Rosebud: It probably won’t help.
Recommended:
Dr. Charkow: We’re dealing with a situation when where the brain is now swollen to the point where she’s probably not going to utilize the brain-
Andrea: Then look into the blood!!
Dr. Charkow: So, she’s going to become brain dead, effectively going to become brain dead. I can say that with 100% certainty.
Andrea: Yeah, because you did not look into the blood.
Dr. Rosebud: It’s not in the blood.
Dr. Charkow: It is the swelling in the brain.
Andrea: And what was that from?
Dr. Charkow: The swelling is the inflammation when you injure your brain. If you injure yourself, you get bruising and swelling. It is no different if you sprain your ankle. The brain is a closed box. When there’s increased pressure there, it squeezes the brain and reduces the blood supply to the brain and it pushes the brain down which is what is happening now. A blood transfusion would not have helped that.
Andrea: Yes, not today but on Saturday, Sunday, Monday-
Dr. Charkow: No, not the blood transfusion.
Dr. Rosebud: It wouldn’t have helped.
Dr. Charkow: Would not have helped at all.
Andrea: How do you know?
“Look out for next week’s episode of YOUR QUESTIONS ANSWERED where I continue to help Andrea with this challenge of having her 34-year-old sister in ICU!”
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



