Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
Should neurological observations be done every hour after seizures and stroke?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkin’s Lymphoma and is currently experiencing decrease in blood count as well as having second thoughts about the treatment her sister is getting.
Is withdrawing treatment and “pulling the plug” on my 34 year old sister in ICU illegal?
You can also check out previous 1:1 consulting and advocacy sessions with me and Andrea here.
Hi Andrea,
I’ve had a read through this policy that’s attached.
It’s pretty much a standard policy that you find across all major public hospitals.
There is enough information in there to build an argument in favour of giving your sister full treatment.
We have successfully used a similar policy in Queensland just a few months ago to build a case for a client in ICU where ICU wanted to limit treatment.
Happy to discuss.
Kind Regards
Patrik
Hi Patrik,
I hope you are having a good day.
My sisters blood counts for today are:
WCC – 1.65
HG – 67
Platelets – 16.1
INR – 1.3
I noticed the counts are dropping on a daily basis. The nurse said the counts don’t mean much without taking the entire condition into account.
I have sent an email with a formal complaint and visited their office too.
The family meeting is supposed to be tomorrow. I am not sure on the time but I would love for you to attend.
Kind regards
Andrea
Find more information about family meetings:
Hi Andrea,
please see my comments in red below in relation to the blood results.
I’m glad you’ve made a complaint and spoke to them. It’ll probably get more difficult before it’ll get easier, but at this point in time you’ve got to do what’s necessary.
I don’t agree that the blood counts don’t mean much without taking the entire condition into consideration. Because the entire condition is so critical, by not giving blood products your sister’s general condition can’t be optimised and hence “waking up” might get delayed.
Related Articles:
I also have another name for a lawyer if you want to and I’m probably getting another name later this afternoon.
A lawyer may not be necessary if we think they will be responsive to your requests, but we’ve got to be prepared in case things get more difficult.
I would really urge you to keep an eye if your sister’s blood pressure drops and if she needs inotropes/vasopressors as it could change many things.
Also, do you know what her Neutrophils are?
Any questions please let me know.
Also happy to talk pretty much anytime from now on if you want to.
Here are my answers in red to your questions
WCC – 1.65> WCC very low, concerningly low in fact
HB – 67> likewise as WCC, concerningly low. Again some ICU’s give red blood cells if HB is <70 and others if <60 but it also comes down to if your sister needs inotropes or not. As long as she can stay off inotropes/vasopressors for low blood pressure, a low HB can be tolerated for a period of time. However, in your sister’s case with low WCC and low Neutrophils she would greatly benefit from blood products.
Platelets – 16.1> Very low with high risk of bleeding
INR – 1.3> almost normal and not too bad. Your sister is most likely still at risk of bleeding with low Platelets. Another parameter to look for coagulation of the blood is APTT
I forgot to mention Andrea that I’m very happy to attend the family meeting tomorrow over the phone.
More information about what family meetings are:
Let me know what time. It would be advantageous if we can talk before the meeting to map out a strategy. Most families go into those meetings without a strategy and that’s a big mistake!
Also, I will be in Sydney next week potentially Wednesday and Thursday. I will be spending most of the time in the Blue Mountains with a potential client for my in-home nursing service INTENSIVE CARE AT HOME. But I will be of course available over the phone and via email.
I would also be available for a meeting if you think that helps, most likely on the Thursday.
Here is a link to Keppra and side effects.
https://www.drugs.com/sfx/keppra-side-effects.html
One side effect that’s mentioned and that I was unaware of is decreased neutrophils, which is a concern.
Here is what you may want to consider and put in perspective.
I have never seen such high doses of Keppra. I believe you mentioned that your sister is 90kg and I still haven’t seen such high doses of Keppra with Patients >100kg with grand mal seizures (A type of seizure that involves a loss of consciousness and violent muscle contractions.)
Not sure if your sister had grand mal or minor seizures?
In any case, what I can see by them giving such high doses of Keppra is the following
- They want to rule out any seizures to further cause damage to the brain
- I still think the goal would be to “wake up” your sister which will be difficult but not impossible with such high doses of Keppra, but as I said I haven’t seen such a high dose ever
- We will need to ask them tomorrow why such high doses
Related Articles:
I’m way more worried about them not giving blood products just like you’ve mentioned.
At least by having such high doses of Keppra your sister hopefully won’t have anymore seizures for now which is important too.
Also, you may want to check out the attachment in relation to GCS or Glasgow coma scale.
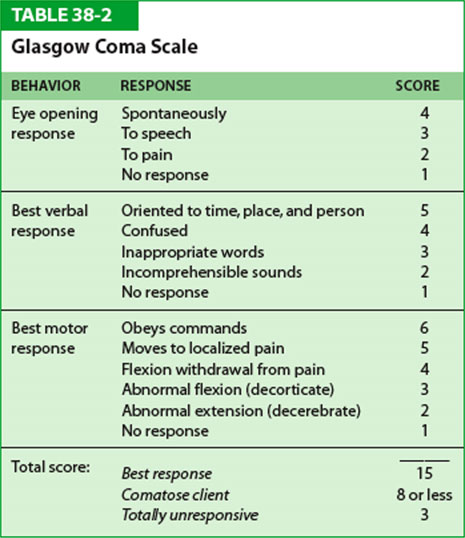
This is most likely something they will bring up in the meeting tomorrow and I would also want to know what her GCS is like currently.
GCS is basically an assessment score for Patients in a coma. ICU teams often use this score to determine future treatment or the lack of such.
We should discuss this tomorrow before the meeting so you have a basic understanding about this functional score.
I will be busy for the next hour or so but can be available after 9/9:30 pm if you want to talk.
Kind Regards
Patrik
Recommended:
Hi Patrik,
Thank you so much for your support, guidance and advice over the past week.
I am very grateful that I found you.
My sister and I are staying with Susan overnight. Her temperature is dropping and so is her blood pressure, my assumption is that her body is slowly going.
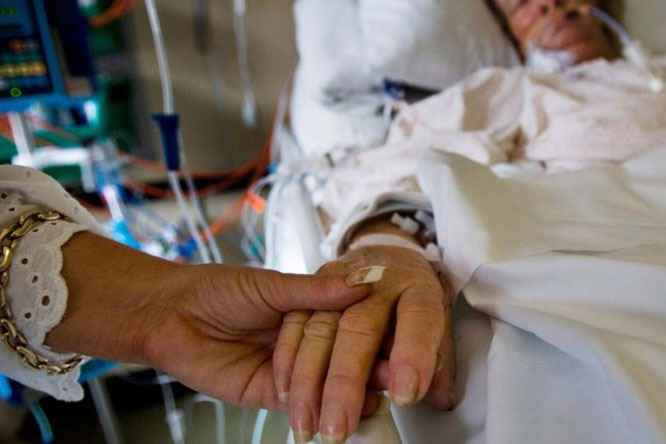
I still will continue fighting the system once she passes. What they have done is unethical and it should be exposed before more families are shattered.
I would be more than happy to write a recommendation about you and your services.
Thank you for everything.
Kind regards
Andrea
Related Article:
Hi Andrea,
You’re most welcome!
I hope you get a rest after you’ve spent the night with your sister.
The system is shocking and yesterday’s family meeting was a prime example in how the system is treating people. I was shocked too but not too surprised because I have seen it before…
I would also like to support you in fighting the system and have some ideas around that. But let’s not put the cart before the horse…
Another thing you may want to keep in mind is if you and your family may want to consider an autopsy when your sister passes to find the exact cause of death.
Not a pleasant topic, but you don’t want to find out about those options when it’s too late.
In any case, please let me know how I can help today or over the next few days. My phone is on.
Kind Regards
Patrik
Recommended:
Hi Patrik,
I thought you should know that my sister passed away yesterday at 12.20pm.
I am hoping you took notes from the family meeting you attended on Wednesday?
If you could please send me your recollection of the meeting that would be greatly appreciated.
After we finalise everything for my sister next week, I am seeking further action against the doctor. This shouldn’t have happened the way it did. He should be held accountable.
If you are able to help that would be greatly appreciated.
Kind regards
Andrea
If you want to learn more about this topic and empower yourself:
Hi Patrik,
Thank you for all your support and help with my sister. I am very grateful that I found you.
We discussed the option of autopsy and my mother wanted to pursue this and I did too, as we wanted to know exactly what caused her death.
But after thinking about it on a deeper level, I explained to my mum that she came into this world whole and she should go out of this world whole. I didn’t think it was humane nor fair to her to cut her up to bits and analysis her body parts under the microscope. I just wanted her to go to heaven with dignity. Something I feel the hospital and doctors (if you can call them that) didn’t give her.
I look forward to the notes and speaking to you soon.
Kind regards
Andrea
Look out for next week’s episode where I help Andrea in her next steps when it comes to asking the right questions in Intensive Care!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



