Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
My sisters’ blood count is low, does she need blood products to get off the ventilator?
You can also check-out last week’s episode with Andrea by clicking on the link here.
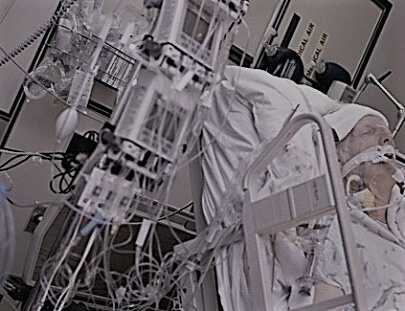
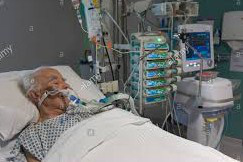
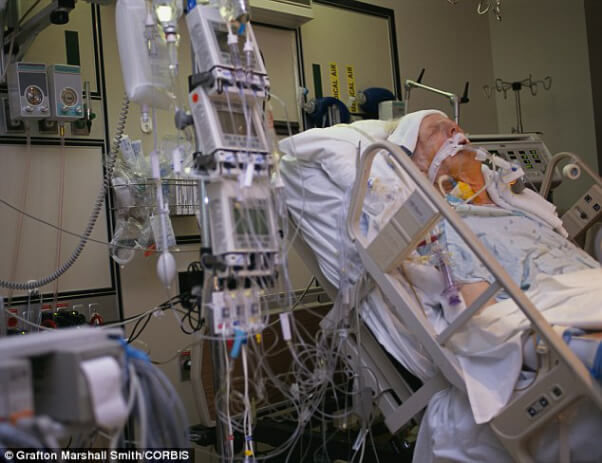
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkins Lymphoma and a stroke.
Today’s questions and excerpt from the 1:1 consulting and advocacy session is
Seizures, stroke and cancer and my sister is still not waking up in ICU after an induced coma! Should we give up???
You can also check-out previous consulting and advocacy sessions with Andrea here
Andrea: Hi Patrik, it’s Andrea calling, I’m so sorry.
Patrik: That’s okay. Do you want me to call you back on my phone?
Andrea: Oh no, not at all, I mean, I’ve got unlimited. So, that’s fine.
Patrik: Okay. Likewise. Likewise. Okay.
Andrea: Okay, thank you.
Patrik: You’re welcome.
Andrea: So, I just saw my sister today. And the nurse that I just saw … she … she was actually … at first she said … they’re all saying she’s not gonna wake up.
Patrik: Right.
Recommended:
Andrea: Cause they extent of her brain damage is quite severe. She’s not brain dead yet. So, just wondering …
Patrik: Sorry, and that was the nurse you spoke to, or a doctor?
Andrea: No, the nurse. But then I started talking to her about certain things, but she’s actually got the same opinion of myself, where chemotherapy really doesn’t work. Anyway, so we went into the whole … yeah … down that path, all the traditional stuff. But anyway, so then I basically said to her, “Listen, I’ve been there before.” Cause she said that she was asking the doctor to prescribe intravenously morphine, and I go, “Why is that? Are you going to make her comfortable?” I go … I go, “Before I go, she’s giving her any medicine?” I go, “I just want to understand. The implications to her … ”
Patrik: Absolutely.
Andrea: And I guess that’s one thing we haven’t done in the throughout the whole 18 months.
Patrik: Right.
Andrea: Is understand the implications. Cause, I mean, the doctor gave us steroids to reduce her cancer growth but she’s developed diabetes, as a consequence. And she never had diabetes.
Patrik: Yeah, yeah, yeah, I’m not surprised. I’m not surprised. The steroids … as soon as you give somebody steroids the blood sugar shoots through the roof. It’s just …
Andrea: And he never told us that.
Patrik: That’s terrible. That’s terrible.
Andrea: Even with the radiation, through my research, you’ve got a high chance of developing a stroke …
Patrik: Yeah, yeah, yeah.
Andrea: Within the first five years. And, I mean, these are the things that they would never explain to us. Cause I would’ve …
Patrik: Right.
Andrea: I’d take a different route. Anyway, and now she’s in the position she’s in, out of … our ignorance. But then … then also not disclosing, which is very frustrating for me. But, anyway, just a few questions for you.
Patrik: Yeah, yeah, please go ahead.
Andrea: So, anyway, so I’ve basically said “she doesn’t look more uncomfortable more and …
Patrik: Yes, and that would’ve been my next question … Morphine for somebody who doesn’t wake up, who’s comfortable, from my perspective, doesn’t make any sense – at all.
Andrea: Yep.
Patrik: Right? If somebody’s in pain, and is waking up, fair enough, give them morphine.
Andrea: Yep. Yep.
Patrik: For somebody who’s not in pain, trying to wake up, from my perspective, and from my experience absolutely contraindicated.
Andrea: I agree. Why are you trying to prescribe her morphine? Are you trying to kill her?
Patrik: Good, good. No, no, that’s a … I think that’s a valid question. I think that’s a very valid question. What was her response to that?
Recommended:
Andrea: I didn’t say that to her.
Patrik: Right, okay.
Andrea: But, I said, “I just want to understand what the implication is.”
Patrik: Yeah, yeah.
Andrea: I go, “With any medicine that you give her, I wanna understand.” I go, “like whatever you’re going to do for my sister’s treatment, I want to understand complete ramifications.” Cause the doctor, gave up on her, once … once she had a feeling as well, she’s like, “I don’t like him anymore, he’s given up on me.” And I should’ve changed her haematologist. Cause he said, “There’s no longevity for you. So, it doesn’t really matter what treatment we use. It does not … there’s no … long … you’re not gonna live long. You’ve got about up to a year, so it doesn’t really matter.”
Patrik: Yeah, yeah.
Andrea: But, anyway, so yes. I agree. I basically instructed not to prescribe … not to give her morphine.
Patrik: Good, good, keep asking for what you want!
Andrea: I don’t want the morphine given to her, unless she’s in real … well …
Patrik: Yeah.
Andrea: Unless I can visually see that she’s in pain. And she’s not in any pain.
Patrik: Yes, yes. And that should be your … your bottom line, really. As long as she’s not suffering, that’s the way I look at those situations. As long as somebody is not suffering, and as long as there’s life, there’s hope. People are suffering, and they’re going through hell, by all means, then let’s discuss what the next steps are. But, your sister is not even at the point where she is in the best position so that she can wake up, and by giving morphine that would be, going in the other direction. But, I …
Andrea: For sure. And … I said to her, I go, “Wouldn’t that keep her asleep longer?” Well she’s actually … she’s already been fed all the information of the doctors, that she’s not gonna wake up. They all have the opinion that she’s not gonna “wake up.” I have a very different opinion …
Recommended:
Patrik: Good.
Andrea: It’s going to take time, it might take weeks, it might take months. It might take years.
Patrik: Correct.
Andrea: I don’t want it to take years. But, I wouldn’t put her through that. But, it might take weeks, it might take months. But, she will wake up.
Patrik: Yes.
Andrea: She’s a fighter.
Patrik: Yep.
Andrea: And she … and also Patrik, what I really … and I challenged the doctor yesterday cause he was giving us all this information ….
Patrik: Good.
Andrea: And, I said to, I go, “Why was she intubated the first time, having a seizure?” I go, “Does everyone have to be intubated?” And he’s like, “Yes.” And I go, “Why?” And they don’t.
Patrik: They don’t. They don’t. Just remind me again, when she was first intubated, was she still on the ward, or was she in …
Andrea: On … on the ward.
Patrik: On the ward, yeah, yeah. And did they give you … did they give you a valid reason why she was intubated? Could they track that back? And they … from my perspective, somebody who … who has a massive seizure and is not intubated, the only reason they need to be intubated is, number one, if they block their airway, right? Because often, their tongue pops back and obstructs the airway, that can happen during a seizure, okay. Or, number two, if they start vomiting, and …
Andrea: She didn’t do any of those.
Patrik: Right, right, right.
Andrea: I think it’s just the way that they’re trained – intubate anyone. And I guess … I guess, so I said to the doc yesterday, “What happens to the person that has a seizure on the streets? Are they not intubated?” And he goes, “Well, the ambulance does it.” Do they?
Patrik: Well, I’m not a paramedic, but an ambulance crew is trained to intubate with a qualified doctor but, again, it all depends … Look, I’ll give you a very … very quick example why people don’t get intubated during seizure. So, part of what I’m doing, I also own a home care nursing service INTENSIVE CARE AT HOME. Right? We’re looking after … let’s put it higher and really sick patients at home where otherwise, might be in intensive care.
Patrik: Cutting a long story short, we’re currently looking after a child at home, she’s thirteen and she’s having seizures regularly. She has no tracheostomy, she’s not ventilated, we’re managing her … if she has a seizure, we’re managing her with medication. We know she’s at high risk of going back to hospital, any minute of the day, really. But, we’re managing her with medication. Right? And, that’s what we do. And she’s seizing, let’s say at least three or four times a week, right? From my … and that’s a child … a child who is even more vulnerable, then an adult.
Patrik: Right? Hospitals are always on the side that, especially, if they have an ICU, wherever patients are… we’ll stick a tube in, we’ll put them in ICU, we’ll sedate them. But that’s not necessarily the right approach. Especially with your sister being so vulnerable, with Non-Hodgkin’s, with radiation, with chemotherapy, you understand all of that.
Andrea: And then … the thing is, Patrik, throughout her whole treatment of cancer, she was … she refused the sedation. They put the vas cath in her, they did puke tubes in hetr lungs and stuff… taking fluids out of lungs, putting holes in her lungs and stuff … tubes out of her – without sedation. She refused the sedation, she didn’t want any sedation. She had a bone marrow, when they put the stuff in your bone marrow in your head, all that, without any … without the whistle, without any form of sedation. She didn’t want sedation. And, to me, it breaks my heart seeing her there, heavily sedated, and they used the … which sedation, those two sedations, they used the heavy one.
Related articles/videos:
Patrik: Propofol … the Midazolam probably. The Midazolam.
Andrea: The Midazolam. I think they used that. And they gave her heavy sedation, and now she’s not “waking up”. Four to eighteen months of treatment, whatever they had to do, any procedures without sedation. And, if her wishes would have been, “Do not sedate me.”
Patrik: Yeah, yeah, yeah, yeah.
Andrea: But they sedated her.
Patrik: Yeah, yeah, yeah, yeah.
Andrea: And I’m really, really, angry about that.
Patrik: Yeah, yeah. Absolutely. And, here is another … know that I’m thinking about this … there is another reason why they might have intubated her. What might have happened is, during a seizure, and managing a seizure with medication, that they often give Midazolam, intravenously. When somebody is seizing, if you give 5 mg of Midazolam, they usually stop seizing very quickly. Okay. But, what the Midazolam does, it basically puts patients to sleep. If for whatever reason they gave Midazolam during the seizure and she went to … went … stopped seizing but also stopped breathing, that’s another reason why they might have had to intubate her.
Patrik: But again, now you’ve got the information and, now again, I’ll put that in an email to you, a bit later, so you got it in front of you, and you can ask those questions. They might … what would’ve happened if she had a seizure on the ward? They would’ve called, either, a medical emergency or even a code blue, and they have some records from that. They must have some records from that event. And there must be some documentation why they intubated her.
Recommended:
Andrea: Yep.
Patrik: There must be some documentation. The answers, even though the doctor may not have the answers straight away, the doctor should be able to either show you the document, or have a look at the document, and then give you the answer, right?
Andrea: Right. Yep.
Patrik: Now. The other thing that stands out to me, what you mentioned before, they’re talking about she’s not waking, but she’s not brain dead. Anybody needs to be very careful in using the word brain dead, including the doctors, or the nurses. I think it’s highly inappropriate from a nurse to say … what did you say, she’s not brain dead, or she …
Andrea: Well a … I’m sorry, she’s got brain damage.
Patrik: Right.
Andrea: But they didn’t say brain dead cause I’d …
Patrik: Okay.
Andrea: Used my words loosely, cause I’d … did reading on the internet.
Patrik: Right.
Recommended:
Andrea: Cause I’m trying to understand. Cause we experienced this before. I’m just trying to educate myself.
Patrik: There is a huge difference between brain death and brain damage, I can’t stress this enough! In fact there is no correlation between brain death and brain damage. You can often live with brain damage but you are going to die when you are brain dead. Therefore there is a huge difference in the two.
Knowing and understanding the difference is key!
Andrea: Yes.
Look out for next week’s episode where I help Andrea in her next steps when it comes to asking the right questions in Intensive Care!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!