Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
My Dad is having a DVT and he’s now on a Heparin infusion! Will he need an IVC filter?
You can check out last weeks question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkins Lymphoma and a stroke.
Today’s questions and excerpt from the 1:1 consulting and advocacy session is
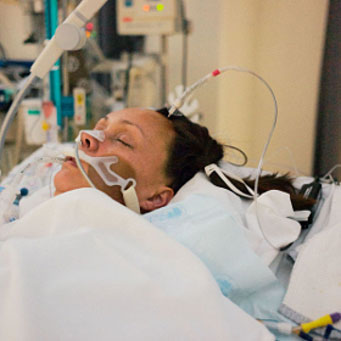
My 34 year old sister is in ICU with cancer and she had stroke! She’s not waking up! Help!
Hi Patrik,
My sister who is only 34 years old has been sedated for 4 days after suffering a stroke and has stage 4 aggressive non-Hodgkin’s lymphoma (refractory cancer- she has had chemo, radiation, stem cell transplant and nothing has worked to cure her).
The doctors did a brain CT scan today and they could see more than one stroke has occurred since she has been in ICU.
She hasn’t woken up after 3 days off the sedation.
Doctors are saying its up to the family to either take off the machines and let her die naturally or we can continue treating her. The head of ICU says it is possible that she will wake up.
We won’t give up on our sister/daughter and have given the orders to continue treating her and hope to the powers above she “wakes up”. They don’t know what caused the stroke/s and the impact on her body.
Questions:
- Have you had a similar situation in your experience?
- Do you have any suggestions on how to deal with the ICU team?
- Any advice on how to manage the situation from your experience?
- What has worked well in similar situations from your experience?
Thank you so much. I look forward to speaking to you tomorrow.
Kind Regards
Andrea
Hi Andrea,
it was nice to talk to you this morning.
Thank you for being a client, I appreciate it!
You and your family are facing a major challenge, but as we discussed, I think staying positive is the best option even though it will feel hard at times.
Here are some questions that you may want to bring up with the ICU team
- Was your sister on Propofol or on Midazolam for sedation?
- Also, was or is she on Morphine or Fentanyl for pain relief?
Depending on which drugs she had or still has, it may further delay “waking up”, as for example Propofol is short acting and Midazolam is long acting.
Especially with the liver being compromised there may be a delay in the drugs being metabolised and therefore a further delay in “waking up”.
Please find more information about those drugs here
https://intensivecarehotline.com/sedation/
Also, for the seizures she may have had last week, they most likely have started her on a drug called Keppra (Levetiracetam) or Phenytoin (Dilantin). Both are anti-convulsive medications and both are given to prevent seizures. Those drugs also come with side effects including but not limited to further slowing down “waking up”.
There is also a very high chance that with the sepsis your sister is currently battling and a potentially low Haemoglobin (red blood cells) she is needing Inotropes/vasopressors such as Noradrenaline or Adrenaline.
The inotropes/vasopressors as well as the ventilator and the breathing tube/endotracheal tube are considered major forms of life support, without it your sister most likely couldn’t stay alive.
Your sister will most likely need some calf compressors instead of anticoagulation medicine, because of the low Platelet count. The calf compressors will “massage” the calf and keep the blood flowing to prevent blood clots.
Also, if I was you, I would ask the Neurologist why she didn’t have a CT scan of the brain after her first stroke. A delay of three days seems inappropriate to me.
As discussed, we should speak to the doctors because I speak the medical language and I can help you in asking all the right questions. It often helps tremendously if families have an advocate involved.
Patrik
Related article/video:
Andrea: Hello, Andrea speaking.
Patrik: Hi Andrea, it’s Patrick speaking from Intensive Care Hotline, how are you?
Andrea: Yeah, I’m okay, how are you Patrik?
Patrik: Very good thank you. Thank you for making contact and I’ve had a read through your email.
Andrea: Yes.
Patrik: Where are you? Are you in Sydney or are you in Melbourne?
Andrea: We’re in Sydney. Yeah.
Patrik: Which hospital is your sister at?
Andrea: Saint George hospital.
Patrik: Public or private?
Andrea: Public.
Patrik: Public, okay. It sounds like a difficult situation. At the same time, she’s only 34. How long has she been having the Non-Hodgkin’s Lymphoma for?
Andrea: Probably about 18 months now. She was diagnosed November 2016. So probably close to 18 months, yeah.
Patrik: Okay. And is this her first ICU admission?
Andrea: No. Well it is in the true ICU stage, but before she was like, she was never sedated or the breathing tube in her mouth, but she’s had complications from transplants, various thing in the past but not the ICU…whether that lower ICU and not the super ICU unit, you know what I’m talking about.
Patrik: Yeah. HDU
Andrea: Yes, the high dependency unit.
Patrik: Okay. Okay. But at the moment she is still on a ventilator?
Andrea: Yes, that’s right.
Patrik: Yeah. Yeah. And you’re talking about the head of the ICU. Have you got a name I used to work in Sydney I used to work at Prince of Wales Private ICU.
Andrea: No, no I don’t know his name, sorry.
Patrik: That’s okay, that’s okay. I mean from my perspective three days in ICU off sedation, even with a stroke it’s way too early…you know, this is very early days. The combination of the stroke and the aggressive Non-Hodgkins Lymphoma, it’s not a good combination but at the same time this way too early to you know-
And when I say way too early, three days of sedation, it’s nothing. If she was of sedation for two weeks and she was doing nothing than I would say okay, we’ve got some concerns here.
But even after two weeks you’ve got to give it time, alright? There’s no hard and fast rules how long it should take for somebody to wake up, right? So, that’s one thing. What I have seen over the years especially with like, Non-Hodgkins Lymphoma, not many patients end up in ICU with Non-Hodgkins Lymphoma and the only time I have seen them coming into ICU is usually; they go through some radiation or they go through some chemo-therapy and then their immune system crashes-
Related articles/videos:
Andrea: Yeah. Which has probably happened here, yeah.
Patrik: Yeah.
Andrea: Her bone marrow is pretty much depleted.
Patrik: Yeah. Is she Neutropenic do you know?
Andrea: What’s that sorry?
Patrik: Neutropenic yeah. So what often happens is Non-Hodgkins Lymphoma after chemo-therapy or after radio therapy, the immune system crashes and one of the symptoms of that would be to have no neutrophils in the blood. And it’s probably something you’ve got to ask them.
What it basically means if there are no neutrophils in the blood it basically means that there is no immune system whatsoever.
Andrea: Right. Okay.
Patrik: Do you know whether she is in a negative pressure room?
Andrea: No she’s in mixed up with everyone.
Patrik: Okay then she’s not neutropenic. Then she’s not neutropenic. Because otherwise she would have to be in a negative pressure room isolated from any other bugs.
Andrea: Right. A haematologist came by and he said that she’s basically got no bone marrow. They’ve given her blood I think platelets and stuff like that. But he said that you know, they gave her a stem cell transplant last July and clearly with her own cells. And obviously her bone marrow and her stem cells are of a babies, there not what she was grown up with.
That’s my thoughts, I’m not a medical professional but I mean that’s just logic.
Recommended:
Andrea: Okay. What’s the hematologist’s point of view in terms of the stroke, what are they saying?
Andrea: They’re saying it’s very grim. They think that the Lymphoma’s taken over that that’s grown and spread. I was taking her to a Chinese acupuncturist, he was boosting her system with all the Chinese medicine, traditional Chinese medicine.
And then when she had her last blood count done her blood went from 1800 down to 700 and the haematologist was surprised by it. She was undergoing, she was just starting her rounds of- He prescribed her high doses of steroids and she didn’t want to go through chemo so-
Patrik: Okay.
Andrea: And then high dosage of radiotherapy. My personal view is that the radio therapy has given her the stroke, of some sort or the steroids.
I was doing my research last night by your therapy the first five years you’ve got a high chance of a stroke. So she had a stroke a week … two weeks ago on a Friday. And since then I think she had a stroke slash seizure a week later, or six days later.
And then apparently they’ve scanned her brain yesterday with CT scan and then her brain had multiple areas of impact. So they think multiple strokes.
Patrik: Yeah. Yeah.
Andrea: So they don’t know what the impact is. I mean, because before she had her whole left side was stiff or numb and now she’s not waking up. And they’re very negative about it. We’re very hopeful that you know there is god out there. That powers that be you know, above. That if she’ll wake up then she’ll wake up.
Recommended:
Patrik: And to put this in perspective for you. Every ICU team is negative and it doesn’t matter whether somebody has Non-Hodgkins or a Pneumonia, it doesn’t matter they’re all negative.
That’s something that a lot of families can’t come to terms with and I agree with that. The biggest challenge in ICU is, no ICU team is ever going to tell someone, ah look we’re definitely going to cure your mom, your dad or your sister, it’s not going to happen.
They will never say that, never ever. And that’s why it’s so important that you do your own research and you know… and be hopeful. Nobody can guarantee you the outcome but the way I look at those situations is that I believe that no matter the outcome it helps if you have hope, and it helps if you are positive.
Related article/video:
And that’s very challenging. I mean the situation your describing is very challenging. But at the same time being positive and being hopeful I believe helps. Right? Now again to put this in perspective for you.
Somebody who’s been in and induced coma for four days and doesn’t have a stroke might not necessarily wake up straight away. So if your sister didn’t have a stroke but was in an induced coma for something else, you know for pneumonia or for whatever else, she may not wake up after three days, alright? So, that’s number one.
So the stroke is probably putting a delay on that. We can appreciate that. But at the same time there’s hundreds of patients every day that come out of an induced coma with no stroke, that don’t wake up after three days.
Andrea: Right yeah.
Patrik: So, that’s what I’m saying. Three days is nothing and it’s not a long time by any means.
Andrea: Yup. I agree completely. Considering her liver is not functioning well either. You know, my experience at ICU is you actually don’t ever want to end up there. Because you feel like, you actually walk out of there dead. Like what are the statistics of people going in there and walking out alive?
In her situation I mean, they’ve treated all these symptoms and put lots of drugs and drugs and drugs into her, that it’s impacted her liver now.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!





