Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
How quickly does a CT or MRI of the brain need to be done after a stroke?
You can check-out last week’s episode with Andrea by clicking on the link here.
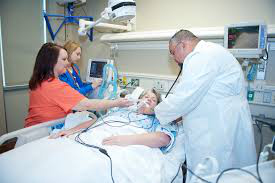
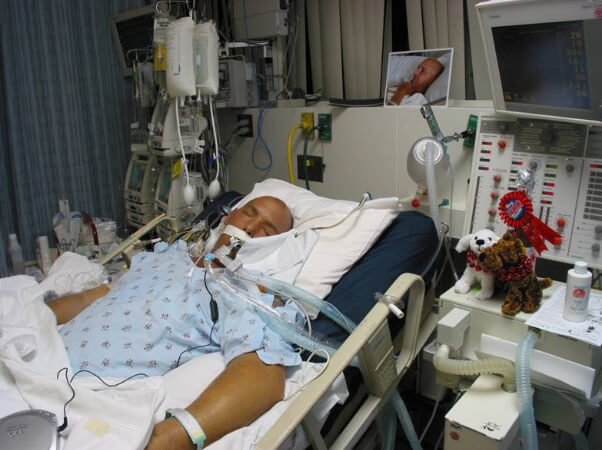
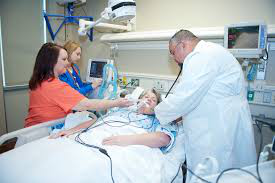
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkins Lymphoma and a stroke.
Andrea and her family have been in an extremely challenging situation with her 34 year old sister clinging on to her life in Intensive Care. To make matters worse, they have a negative Intensive Care team to deal with!
Today’s questions and excerpt from the 1:1 consulting and advocacy session is
Should neurological observations be done every hour after seizures and stroke?
You can also check out previous 1:1 consulting and advocacy sessions with me and Andrea here.
Look out for next week’s episode where I help Andrea in her next steps when it comes to asking the right questions in Intensive Care!
Andrea: Her lungs. They put her at full ventilation …
Patrik: Okay, okay.
Andrea: It’s, like, “Why are you?” Cause, wouldn’t that make your lungs lazy?
Patrik: Yeah, yeah, yeah.
Andrea: Over time?
Patrik: It would.
Andrea: Yes, that’s what I thought. I mean, I’m not trained. I mean, it’s just logic. If a machine is doing something for you, you become lazy.
Patrik: That’s right. But, but, there are … and what was the answer to that question? Did they tell you why?
Andrea: To give her lungs a break, cause she’s working hard.
Patrik: Yeah, yeah.
Recommended:
Andrea: And I … I said to them … and I … cause I’ve asked, which part of the machine is her breathing, so I can see what the vitals are, and then, I’ve noticed, when I sit down, I talk to her, she starts breathing on her own. She’s …
Patrik: Good, good. Yep.
Andrea: A little bit, but, but, enough for me to see that she’s breathing on her own. Cause it’s like, why have you moved her to full … the machine? Breathing for her.
Patrik: Okay. I can explain that to you. Why they might have done that, why they might have … if they’re saying … you’re absolutely right, that if you … the more support you give somebody from a machine, the, sort of, lazier people might get. At the same time, rich ventilation, in ICU, there’s a number of things … when they say she’s working hard … when they put her in full support, they can control a lot of things, including the number of breaths per minute, including how many mLs she gets per breath.
Andrea: Right.
Patrik: Let’s just say she’s getting 500 mLs per breath. Okay? From the machine. If she is breathing by herself and the breaths she’s taking is only 200 mLs, it wouldn’t be enough.
Andrea: Right, I understand.
Patrik: They can … they can see that she might get distressed. They can see it, obviously, in the volumes on the machine. They can see it on the oxygenation, on the monitor. And, number four, they can see it … they would be doing regular arterial blood gases. Have you heard of that?
Andrea: Regular, say what was that?
Patrik: Blood gases. What they do, is they take … she would have, most likely a line in her artery, in one of her arteries. Either in her wrist, or in her groin. Now, that … that line is in her artery and if you take a blood sample from the arterial line, you can get an oxygen level in the blood.
Andrea: Right, yes.
Patrik: If oxygen level is low, or, more importantly, if the carbon dioxide (CO2) level is high, she’s not breathing adequately. And that’s what they might refer to when she’s working too hard.
Andrea: Right, okay.
Patrik: It’s most likely what they refer to.
Andrea: Fair enough, okay. Cool.
Patrik: Right? And … in all fairness, I have seen it over, and over, again, that you want to get somebody off the ventilator, but they are not quite ready and you do give them a rest, you put them back on the ventilator with full support, maybe, for 24, 48 hours. And then, you try again. And often patients do come back. You are absolutely right, you don’t want to overdo this, you don’t want to do this for weeks.
Related article/video:
Andrea: No.
Patrik: But you do want to do it when … when your first attempt of getting somebody off the ventilator has failed. Then you do it to give people a bit more of a rest. And then you do it again.
Andrea: Yep.
Patrik: Right. That’s what probably happened there.
Andrea: I’ll say this Patrik. When I noticed yesterday is … when I came to visit her, her hand was shaking – her good hand.
Patrik: Right hand, yes.
Andrea: Her right hand. That was shaking. I said to them, “Why’s her hand shaking?” She like, “Oh, I haven’t noticed it.” And then, it went up to her arm. And then I said to the nurse “can you please show the doctors” and the doctors are off doing their rounds, and they didn’t have any urgency or …
Patrik: Right.

Andrea: And then I was hovering around, and I said to the guy, once you’ve got your jobs done, can you please tell me … can you please explain to me why half of my sister’s hand is shaking?” He’s like, “It could be from … ” Oh, what did he say? It could be from …
Patrik: Withdrawal?
Andrea: Not withdrawal. He actually didn’t even mention that. I … and he goes, “It could be from the temperature or the … ”
Patrik: Yep, yep.
Andrea: I go, “Are you for sure?” And he goes, “No.” “Then would you please come and have a look?” And then he had a look and he looked at the file notes and the neurologist apparently documented that it could be a seizure as well.
Patrik: Yes, exactly, seizure withdrawal. That would … those would be … temperature probably. The temperature was 39C (102.2 F), she might shake with the temperature. But, the first thing that would … would be my thinking would be, either, withdrawal from medication such as sedation, and I can’t do that in the moment, or, especially if she had seizures in the past, I mean, by all means, there’s a high chance, she might have seizures again.
Andrea: And I said to him, “How do you know it’s not a seizure?” He read her notes and he said, “The neurologist, apparently, put her medication … seizure medication, reduced it a bit… if they saw something, they could increase it back to, whatever.” They just gave her the seizure medicine then.
Andrea: So I was like, “You guys are treating all the symptoms, but you actually don’t know what’s causing them.” Which, is very frustrating.
Patrik: Yeah, yeah, yeah.
Andrea: Cause like, she can’t talk to us. She can’t give us direction. But, yet they’re just observing, it’s like, “Well, we think it’s that.” But it’s like, “How do you know it’s accurate?”
Patrik: Very much so.
Andrea: Very frustrating for me Patrik, I feel powerless.
Patrik: Yes, yes. When … when she had those shakes, did anybody check her pupils? With a torch?
Andrea: No.
Patrik: Right. During a seizure, what normally happens … if somebody has a seizure and you check their pupils with a torch, or let’s put it that way, if you check pupils with a torch on a healthy person, the pupils react to light, and they contract. Okay, that’s a sign that the brain is working.
Patrik: Now, somebody with a seizure, when you shine a torch in their eye, or in their eyes, the pupils don’t react to light. Because, the brain has basically gone into lockdown.
Andrea: They checked her pupils… Cause I mean when … what I saw was that one of the ladies was checking her pupils …
Patrik: Yeah.
Andrea: Was very, very, scared … very sad. Her pupils and they opened her eyelids, when they were checking with the lights, she didn’t respond at all.
Patrik: Okay. And how long ago was that?
Andrea: Probably a couple of days ago, three days ago maybe.
Patrik: Okay. Do you know whether they are still doing those observations, hourly?
Andrea: I don’t think they’ve ever done them hourly!
Patrik: Right.
Andrea: They only did it once.
Patrik: Right. Okay. Right, right. Normally, what happens with anything related to the brain, with a seizure or … or a stroke, at least in the first 48 to 72 hours, those observations with the pupils should be done hourly. Now, given that time has passed …they may not do it hourly. Right? They may do it, full hourly, they may do it once a shift. It depends.
Recommended:
Andrea: Yeah.
Patrik: I appreciate that, after a stroke, the pupils might’ve been in lockdown. But … but it’s probably good for you if you ask what … what they’re doing at the moment.
Andrea: What do you mean?
Patrik: What …
Andrea: What observations?
Patrik: Yes. Not only what observations. I would be very curious to know what the pupils are doing when they shine light in there. If the pupils are equal in size and they react to light, the brain is doing something. You mentioned, earlier, brain death, in brain dead people the pupils … they’re not … reacting to anything.
Related article/video:
Andrea: Right.
Patrik: Right. You may wanna know, wanna find out what … what the reaction from the pupils is to light.
Andrea: Yep.
Patrik: Because that’s one indicator, if the brain is doing anything at all.
Andrea: Right, yep.
Patrik: Alright? And, I’m sure … look, I could be wrong. But, I’m pretty sure they would’ve told you if the pupils are not reacting at all. They would have told you that. I would be surprised, if the pupils are not reacting at all, they would’ve told you that.
Andrea: Right, yep.
Recommended:
Patrik: What else do you need to clarify?
Andrea: If they … if they want to turn the machines off, isn’t that a form of euthanasia?
Patrik: Very much so. Very much so. Is that something …
Andrea: And it’s illegal.
Patrik: Oh, absolutely. Absolutely. Is this something they brought up, since we last spoke?
Andrea: No. But, we have a family meeting tomorrow I think …
Patrik: Okay.
Andrea: At 3pm our time. If you can …
Patrik: I … Yes, no, no. I will make time, if you want me to be there, I will make time.
Look out for next week’s episode where I help Andrea in her next steps when it comes to asking the right questions in Intensive Care!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!