Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I shared another question in this series of questions from my client Veronica and the question last week was PART 8 of
You can check out last week’s episode by clicking on the link here.
Previous episodes of this sequel of 1:1 phone counselling and consulting sessions you can find here
PART 1, PART 2, PART 3, PART 4, PART 5, PART 6, PART 7 and PART 8
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Veronica, which are excerpts from 1:1 phone and email counselling and consulting sessions with me and the question this week is
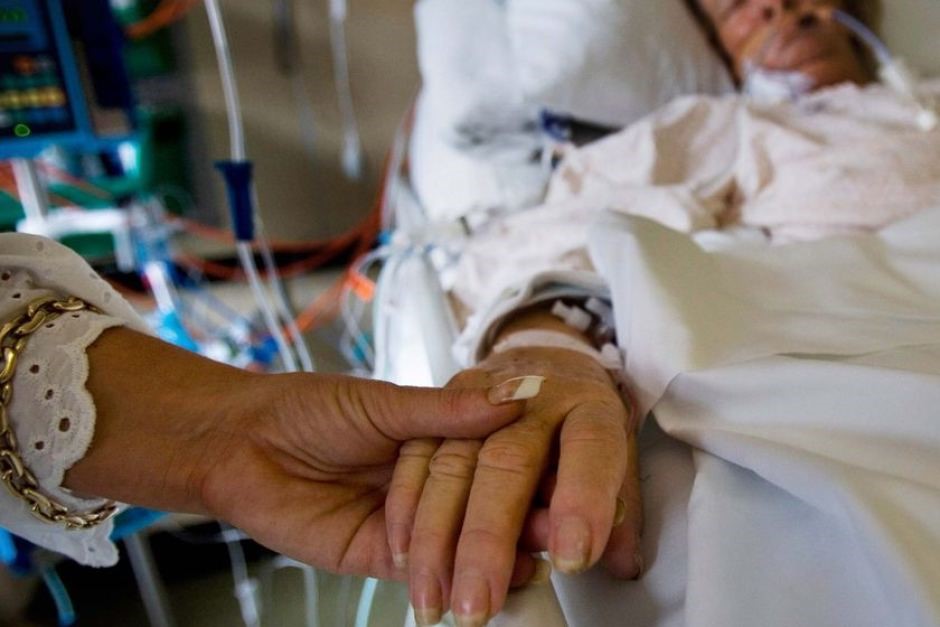
My Dad (71) is in ICU with stage 4 lung cancer & stroke, he’s on the ventilator now and in an induced coma, what are his chances of survival? (PART 9)
Whilst in the last counselling and consulting session we focused on whether a tracheostomy would be the right next thing to do for Veronica’s Dad, in this session we focus on the alternative to a tracheostomy if Veronica’s Dad can’t be weaned off the ventilator and won’t get a tracheostomy. I explain to Veronica what a “one-way extubation” means and how it ties in with an NFR/DNR order. We furthermore talk about what does need to happen to get Veronica’s Dad off the ventilator or whether she should prepare herself and her mother for an end of life situation.
Patrik: And, you see this is the thing, while a tracheostomy can prolong life, I’m not saying indefinitely but for much longer, a lot of patients with a tracheostomy don’t feel in control. That’s a disadvantage. You know, because they can’t talk.
Veronica: No.
Patrik: Right? So, you got to be aware of advantages and disadvantages, right?
Veronica: Yes.
Patrik: But, what I will do, once we come off this call, we have a number of articles on our website when you should do a tracheostomy, when you shouldn’t do a tracheostomy. So, I will send you some articles so you get a bit of a feel, what are the advantages, what are the disadvantages, you know? The other thing that I can see, especially what we’re doing in home care as well, from my perspective is taking your dad home on a mask, for example, you need some ventilation with the mask. That can all be done, but the same can be done with a tracheostomy at home. But, the question is how does your dad feel about either of those options?
Veronica: Exactly. So, he will need to be informed.
Related articles/videos:
Patrik: That’s right. That’s exactly right.
Veronica: Yeah.
Patrik: He needs to be informed, and what we also don’t know at this point in time is your dad might be well enough to get off the ventilator, but he may not be well enough to communicate properly. He may not be strong enough to even write, or we don’t know any of that.
Veronica: No, exactly. And, that’s what he’d already said too. Yeah, that’s just a whole other thing.
Patrik: And, do you know whether in the last few days the ABGs have deteriorated, like the arterial blood gases?
Veronica: They had gone down, yes.
Patrik: They’d gone down. Because, so here is another thing that I can see, you said he’s on 50% of oxygen?
Veronica: Yes, he was on 45% of oxygen and then they increased to 50%, but that was probably after about three days of being on that.
Patrik: So, here’s one thing that you probably need to know. So, when somebody gets taken off the ventilator, they rarely get taken off the ventilator with more than 30% of oxygen.
Veronica: Okay.
Patrik: So, what he’s, and that’s what I sort of said a moment ago, he’s probably referring to a “one-way extubation”. A “one-way extubation” means we’re taking the breathing tube out, but we’re not planning to put it back in.
Veronica: So, I need to clarify that with him.
Patrik: Yeah, I think it needs to be clarified, because that’s a 50% of oxygen, even 45% of oxygen, is not a number where you can safely take somebody off the ventilator.
Veronica: Okay.
Patrik: Cause, you know how much PEEP(=Positive end-expiratory pressure) he’s on? Does that ring a bell, PEEP? Have you heard of that?
Veronica: What is it?
Patrik: Okay, PEEP is the positive pressure he’s getting.
Veronica: Oh, that’s right. It says it on the machine.
Patrik: Yes-
Veronica: Is that just like a one number? Is it like an eight?
Patrik: Five, yeah eight. Eight makes sense. Yup. It’s usually between five and ten. Eight is, so if he was on 30% of oxygen and PEEP of eight, and do you know his pressure support by any chance?
Veronica: Yes, it says 400, I think.
Patrik: No, that can’t be pressure. But, that’s his volume. But, that’s fine.
Veronica: That’s the volume, yeah.
Patrik: Pressure support it probably somewhere between eight and fourteen, I would think. Anyway, it doesn’t matter, the PEEP of eight and oxygen of 30%, I’d say yeah probably you can extubate if the arterial blood gases are okay and he’s obeying commands, then you can probably take the breathing tube out. But, 50% of oxygen is probably he’s referring to taking the breathing tube out and not putting back in. That would be his plan without having it properly discussed with you.
Veronica: That’s what I think it is too, because I’m pretty sure that he used that word that you just said.
Patrik: One-way extubation?
Veronica: Yes.
Patrik: And, do you know his numbers from his arterial blood gas by any chance?
Veronica: Yes, let me get it. I took a photo of it, just a second.
Okay, it is, sorry I’ve got you on speaker cause I’ve got my phone.
Patrik: That’s okay.
Veronica: Okay, I’ve got PO2, 91.8.
Patrik: Okay.
Veronica: PCO2, 49.2.
Patrik: Mm-hmm (affirmative). PH?
Veronica: PH, 7.4.
Patrik: Yup, and that’s pretty much all I need to know really. Have you got saturation down?
Veronica: His saturation, which is just the one that’s from his finger on the monitor, you mean?
Patrik: Yeah, but there should be a result on the blood gas as well. It might just say O2 sat, doesn’t matter. That’s alright, I’ve got enough information there. That’s alright.
Veronica: I’ve got it all here, but I can’t-
Patrik: That’s alright. And, is his haemoglobin, has he got his haemoglobin?
Veronica: That’s strange … Here you go look, I’ve got the pressure support and everything written on here.
Patrik: Right, what’s his pressure support?
Veronica: Okay, it says it all here. Pressure support, eight.
Patrik: Eight, okay. That’s good.
Veronica: And, it says here PEEP(=Positive end-expiratory Pressure) 5.
Patrik: Okay, five.
Veronica: Pressure is four to eight. And, it’s got the tidal flow. It’s got everything.
Patrik: Yeah, that’s enough information. So, CO2 49 is just a little bit on the high side. It would be great if it was below 45. They could probably get the CO2 down by putting the pressure support up or by putting the PEEP up, either or. But, if they did that, you know, they would get the numbers right but then at the same time they’re not numbers where you could safely extubate.
So, with all of the information here, I’d say he must be referring to a “one-way extubation”. And, that’s all, you know, I guess-
Veronica: I think it’s because it’s based on how bad the scan looked.
Patrik: Yes.
Veronica: But, he said look, I still have to consult with the other physicians. There might be more stuff to tell us tomorrow.
Patrik: Well, you see this is the thing. He certainly has to consult with the physicians, but he has to consult with you too.
Veronica: Yes.
Patrik: Right. So, okay-
Veronica: And, what you’re saying is if dad had a tracheostomy, he will never be able to talk again?
Recommended:
Patrik: Well, that’s not accurate. Some patients who end up with a tracheostomy will have a speaking valve eventually. Okay? But, the question is more like if your dad was to get a tracheostomy, what’s the end goal. Is it there’s a fairly high chance your dad might never get rid of this tracheostomy? Okay, but the other-
Veronica: No, I don’t think dad has much time left if he had a tracheostomy.
Patrik: Well, but the question then also is, you know, what do you want to achieve with that tracheostomy? Do you want to buy your dad time? You know, even though he can’t speak. Because within the time he has left, it probably won’t be enough time to use the speaking valve and train him because it takes some training and it’s not going to happen-
Veronica: And, he had the stroke, which affected his tongue, the swallowing and everything.
Patrik: Well, this is okay, this is another point, now especially with the swallowing. But, how do they know that it affected his swallowing because he hasn’t been off the ventilator since the stroke. How do they know?
Veronica: Because he went into ventilation a few days after the stroke.
Patrik: Oh, that’s right.
Veronica: Yes, because they had introduce a feeding tube because it took him an hour to feed himself, and he couldn’t swallow.
Patrik: So, here is the thing. Here is the next thing, with the swallowing issue, if they take out the breathing tube, if he has swallowing issues, he will aspirate on his own saliva.
Veronica: I know.
Patrik: So, again, that’s where a tracheostomy would help. So, you know it’s really a matter of what do we want achieve?
Veronica: What are we looking at?
Patrik: That’s right.
Veronica: What are we trying to achieve?
Patrik: That’s right. But, I still think while they’re painting not a great picture, but I still think you need to be informed what a tracheostomy can and can’t do.
Veronica: Yes. As long as he’d be strong enough, which we don’t know, if he had the tracheostomy to at least be able to communicate by writing and to have some quality of life. But, if he’s got no quality of life then it’s not worth it for him.
Patrik: Yeah.
Veronica: And, because we don’t know and the doctors don’t know what.
Patrik: That’s right, that’s exactly right.
Veronica: But, like you said, if they keep him on the ventilator now, he’s gonna continue deteriorating.
Patrik: Look, I think taking him off the ventilator makes sense, even though the numbers don’t look flash. But, he can’t be on the ventilator with that breathing tube forever and a day.
Veronica: No.
Patrik: I think what the next step really is, you and the doctors need to be clear, have some scenarios what if.
Veronica: Yeah, have other plans in place for when things happen.
Patrik: That’s exactly right. And, sort of have a few scenarios and lay out some plans, what if?
Veronica: Yes. Okay.
Patrik: And, that also, sorry and I probably should mention that, let’s just say your dad is well enough to go to the ward even, but then also have a plan, if he deteriorates, is he to go back into ICU or not?
Veronica: Yes.
Patrik: You know, they’re all things, and they will probably try and discuss this within this meeting tomorrow, within 30 minutes or whatever without you probably even know what they bring up. So, I’ve now painted a few scenarios for you now. But, they would probably all bring it up within 30 minutes without you having even considered, okay well if he’s going to the ward, what if? Can he go back to ICU? You know, do you want that? Does he want that?
Veronica: Exactly, I don’t think he would. Not now after what he’s just experienced.
Patrik: And, also if he’s going to the ward then, should he be NFR. And, as long as you agree with all of that or the rest of your family, that’s fine. I just don’t like, what I’ve seen over and over again is doctors making decisions for NFRs without even talking to the families and they can’t, well, legally they can’t do it but they do it all the time.
Veronica: Yeah. Yes. Which is probably why when he said the “one-way extubation”, he just quickly said it, and I was like hm.
Patrik: And, that’s basically you know sort of already implying that NFR.
Recommended:
Veronica: Yeah.
Patrik: And, again he’s throwing around with all those terms. You hear a term and you have an idea what it could mean, but you haven’t fully understood the bigger picture what it all means.
Veronica: No, that’s right. No, you’re right. Because, that’s what it is. It’s Not For Resuscitation. So, I need to make sure I clear that up with the doctor.
Patrik: That’s right.
Look out for next week’s consulting session where I continue to help Veronica with her Dad’s difficult situation.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



