Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Does Low Hemoglobin Affect my Mom’s Ability to Wean Off the Ventilator While She is in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Angie, as part of my 1:1 consulting and advocacy service! Angie’s mom is still critically ill in ICU but the ICU team keeps pushing her out to LTAC instead of trying to wean her off the ventilator.
Why is the ICU Team Pushing My Mom Out to LTAC While She’s Still Critically Ill?
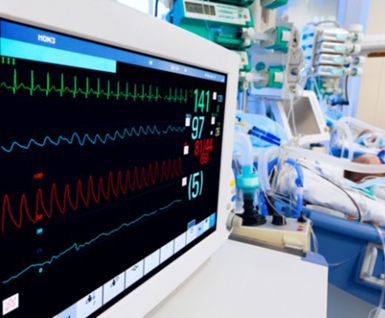
“You can also check out previous 1:1 consulting and advocacy sessions with me and Angie here.”
Angie: Sure. Sure.
Patrik: Right?
Angie: Sure.
Patrik: But nevertheless, that should not stop them from trying the trach collar.
Angie: You’re right.
Patrik: You know?
Angie: Right.
Patrik: But here is the next thing. Obviously, they’re now, from what I understand, they’re trying to push you out of the ICU?
Angie: Yes.
Patrik: And on to LTAC.
Angie: Yes.
Patrik: So, let’s look at this a little bit closer. So, they must have a policy for discharge. Okay?
Angie: Sure.
Patrik: My advice is to ask for that policy and see what that policy says because that policy will most likely say that you need to give consent. Right?
Angie: Yes, definitely.
RECOMMENDED:
Patrik: That’s Number 1. That’s number one. Number 2, have you had time to look at LTAC? Have you engaged with those LTACs? Have you visited them?
Angie: Yes.
Patrik: You have?
Angie: Yes. Yes. Yes. I have. I did that because I thought maybe they can transfer her without my consent, and we don’t have more than two within our driving distance.
Patrik: Mm-hmm.
Angie: So, I started looking at them. The problem is they’re a black box from a clinical perspective. You don’t know which doctor is going to actually see the patient. You just find out very superficial information. One of them provides private rooms, the other one has shared rooms.
Patrik: Mm-hmm.
Angie: One takes more COVID recovery patients. The other one is maybe a little bit closer to his issue, people with pneumonia, older age that are bed dependent.
Patrik: Mm-hmm.
Angie: So, I do not have an objective way of measuring their quality. We’re kind of bound by what’s close to us within driving distance. If I were to choose one, I would choose the one with the private room. Because of her age, I feel she needs family support and encouragement to get her through this period of perhaps doing physical therapy and keeping her motivation up.
But again, they’re both black boxes. There’s no quality measures defined. There’re some minimal ones, like the number of people who have increased mobility, the number of infections within this facility. Those I have compared.
Patrik: Mm-hmm.
Angie: But it’s not enough to make a decision, between the two LTACs.
Patrik: Right.
Angie: But I’m afraid I will not be able to slow down that decision much longer.
Patrik: Right. Why do you say that?
Angie: Because you mentioned the hemoglobin being a hindrance to her coming off the vent. The other one is they’re not trying the trach collar. So, I feel like here, they feel comfortable not progressing her on the weaning path. And the longer she stays, the risks are higher-
Patrik: Yeah.
Angie: … of her remaining vent dependent.
Patrik: Yeah.
Angie: So, I feel like they’re successful in pushing me out.
Patrik: Right.
Angie: To the outside facilities.
Patrik: Okay.
Angie: So, I’m not quite sure how to handle that.
Patrik: Yes. Okay. A couple of things there, Angie. So, the challenge that I’ve seen with LTACs is no matter the credentials and experience of the overseeing pulmonologist, there’s often only one pulmonologist for 30 odd patients. Right?
Angie: Okay.
Patrik: And that is my experience from LTAC. On top of that, they simply don’t have critical care nurses that are well-trained in ventilation/tracheostomy management. That’s my experience. Every time I’m talking to an LTAC, you’re talking to amateurs, really. You know?
Angie: Right.
Patrik: And I’m not saying that the doctors are amateurs, but the doctors simply, they can’t focus on one patient. They just can’t, they just don’t have the time and the resources. Right?
Angie: Right.
Patrik: Which from my experience, makes very poor outcomes.
Angie: Got it.
Patrik: That’s one thing. Then the next thing is, so let’s go back to the hemoglobin issue. Most of the time-
Angie: Sure.
Patrik: … it will be much more difficult. Any adversity, whether it’s needing a blood transfusion, maybe needing to escalate treatments such as inotropes or vasopressors, and I don’t want to get too technical here, they might be able to do that for a short period of time. But if there’s no improvement, people go back to ICU anyway. Right?
Angie: Right.
Patrik: Some LTACs do have an ICU attached.
Angie: Got it.
Patrik: Some of them do.
Angie: Got it. Yes.
Patrik: Something you’ve got to research, have you looked up reviews of those LTACs that you’re in contact with, online?
Angie: Yes. Yes. They’re both bad. One of them is less bad. Some people say, “I had to take my loved one, I had to call 911 to get my father or mother out of the facility.”
Patrik: Oh, my goodness.
Angie: Yes. Yes. So, they’re both bad. Then one of them, I know has bad nursing ratios.
Patrik: Yeah. Of course.
Angie: It’s supposed to be one to four, it’s more like one to five, or one to six.
Patrik: Right.
Angie: So, it’s substantiated. So, I already expect if we go there, family needs to help with turning the patient, or taking care of the patient.
Patrik: Oh, my goodness. Oh, my goodness.
Suggested links:
Angie: Yeah.
Patrik: That’s terrible.
Angie: Yeah. Yes.
Patrik: Oh, my goodness. So that’s…
Angie: Yeah.
Patrik: Right. Right. Okay.
Angie: Yes.
Patrik: Okay. Now I can’t remember-
Angie: Bed sores that… Yeah.
Patrik: No. No. Go on. Go on.
Angie: So, bed sores. Bed sores I know are one of her risks. Bed sores, or bath is another one. Then we have a lot of recovering COVID patients, and these places, I don’t know how good of a job they do-
Patrik: Yeah. Yeah.
Angie: … with the isolating.
Patrik: Yeah.
Angie: And how good their air purification, is either-
Patrik: Yeah.
Angie: … all the facilities?
Patrik: Yep. Yep. Yeah. Yeah. Yep. Yep.
Angie: So that’s another-
Patrik: That’s another concern.
Angie: … big concern.
Patrik: Now, for your own education, LTACs are designed to save money. Right?
Angie: Sure.
Patrik: I mean the ICU bed costs $5,000 a day, LTAC beds I believe the insurance pays $1,500 a day. So clearly there’s a financial driver behind it.
Angie: Sure.
Patrik: On a clinical level, I have nothing to say but I think it’s absolutely abysmal. Right?
Angie: Yeah. Sure.
Patrik: And they would know that the ICU knows that. But nevertheless, that’s always their way forward to managing their beds. So, I can’t remember Angie, was it you yesterday that said you were trying to get to a hospital executive, and you couldn’t? Was it you, or was that somebody else that I spoke with?
Angie: Yes. Yes, it was me.
Patrik: Yep. Yeah?
Angie: I said I tried to find somebody in the administration.
Patrik: Yes.
Angie: Or somebody who runs the money side.
Patrik: Yep.
Angie: I just talk reason with them saying that this patient, because of her age and special circumstances, I don’t think she has a good chance at an LTAC. Can you keep her? And we can find some sort of an agreement. I didn’t say I’d pay all the expenses but to me it’s worth it, to work with this hospital and have her weaned here instead of going to an unknown place with a lower quality of care.
Patrik: Yeah.
Angie: But I could not really reach anyone. I talked to the attending, or case manager, or social worker, or head of patient care, which is kind of like the head of nursing. I even tried to risk management, but they have a subsidy that does risk management consulting for all the medical facilities they own.
Patrik: Yeah.
Angie: So, I even reached them because the reason my mom is in this situation is there was a medical error here.
Patrik: Yep.
Angie: She came in with a broken arm, she ended up getting intubated three days later.
Patrik: Mm-hmm.
Angie: So, I told them, “There was a mistake made here, you guys can make it right. Why do you want to push us out? You have the expertise and I feel she is safe here with your nurses, with your doctors.”
Patrik: Mm-hmm.
Angie: But they just smile. I was not able to find the right contact for that conversation.
Patrik: Okay.
Angie: So-
Patrik: Okay. Have you written to the exec? Have you sent them an email, for example?
Angie: I only tried reaching the… You’re right. Maybe I should have done that, huh?! It sounds obvious. But no, I didn’t. It was more verbal, through phone calls. The only outside person I tried, was through their risk management division.
Patrik: Yeah.
Angie: They have somebody that has a job similar to customer advocacy or patient advocacy.
Patrik: Mm-hmm. Mm-hmm.
Angie: But I did not go directly to the CEO of the health system.
Patrik: I would. I would, if I was you.
Angie: Okay. Okay.
Patrik: A few other questions. So, you have access to the medical records online. Is that correct?
Angie: Yes. Yes.
Patrik: Can you see the daily report the nurses are documenting, or the doctors are documenting? Can you see that?
Angie: I can see the daily reports from the attending.
Patrik: Yeah.
Angie: Which normally, I think the residents and the attending doctor-
Patrik: Yes.
Angie: … oversees.
RECOMMENDED:
Patrik: Yeah.
Angie: So those I can see.
Patrik: Okay.
Angie: The nursing charts, we cannot see the details of.
Patrik: Okay.
Angie: But we can see medication she’s taking for that day or within the last few days.
Patrik: Yep. Okay. Would be good if you could send me what medication she’s on because there may be something in there that would also foster the argument to keep her where she is.
Angie: Got it. Yeah, I can. Sure. I can send that along. Or-
Patrik: Either send me a screenshot, or email it to me, whatever the best way.
Angie: Okay. I will email. Yeah.
Patrik: Because there may be something in there.
Angie: But she’s on her own medications, plus gabapentin for pain.
Patrik: Okay.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!