Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I want to answer questions from one of my clients Isaac, as part of my 1:1 consulting and advocacy service! Isaac’s dad in ICU is sedated and will undergo a tracheostomy. Isaac is asking why the ICU team wants to do a tracheostomy and gastrostomy tube insertion on his dad to push him out quickly to LTAC.
They Want to Do a Tracheostomy and Gastrostomy Tube Insertion on My Dad in ICU To Push Him Out Quickly to LTAC! Help!
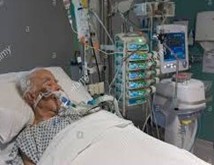
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isaac here.”
Patrik: Intensive Care Hotline, Patrik speaking. How can I help?
Isaac: Hello, Patrik. This is Isaac.
Patrik: Hi, Isaac. How are you?
Isaac: I’m fine. I’m calling you again to talk about regarding my dad’s situation now?
Patrik: Okay. Can I ask you more questions about your dad?
Isaac: Sure.
Patrik: Okay. And just remind me, he has COVID, doesn’t he?
Isaac: No, he doesn’t.
Patrik: Pardon?
Isaac: No, he doesn’t have COVID but he does have pneumonia and he has lung cancer.
RECOMMENDED:
Patrik: Yes. Okay. Yeah. No, no, no, no. Okay. When you talk to your dad, is he responding to you?
Isaac: Yeah, he can. He can move his feet. He can respond to yes or no questions. Squeeze my hand. He’s very alert.
Patrik: Okay. He’s opening eyes for you?
Isaac: Everything. Yeah.
Patrik: Okay. And, they have not trialed the breathing trials, have they?
Isaac: They’ve done it every day. And I guess like he just keeps failing it like today, he only did five minutes.
Patrik: Five minutes. Okay. I see. I see. Are they sitting him up?
Isaac: They put the bed a little bit up, but not really sitting him up.
Isaac: You see when they moved him, once they tried the breathing trial they moved him but he’s back to a hundred percent breathing. Cause like it is hard for him to breathe when they move him.
Patrik: Yeah. No, I get that. I get that. Okay. And they now wanna do a tracheostomy as quickly as possible. Have they given you any timelines or-
Isaac: Well, they’ve been wanting to do it for about a week. Cause they said since it’s been past two weeks. They think it’s of plenty time and then I just can’t find time this week to see him if he’s doing good with weaning. Tuesday last week he did 30 minutes. And then the next day he wasn’t able to do 2 minutes and then went to 10 minutes. You could tell his body just dropped maybe doing the BiPAP but then, they don’t think of it as an option anymore because of all that phlegm that they had to pull out with their fingers. They said it’s thick and it’s difficult when he gets home. Cause they were trying to get him home, versus he’s going to a rehab or whatever they call it. Cause once he gets there, the harder the process. So they said our wishes would go home, let’s do the BiPAP, but they said with him having so much phlegm and all that, they said it would be too hard for him to be on BiPAP. Then, they’re just saying to push for a tracheostomy and the percutaneous endoscopic gastrostomy (PEG) tube and try to get him to a rehabilitation facility for a couple of weeks. And maybe try to get him off the oxygen from the tracheostomy to see if he could go home from there. Because right now it’s like, they’ve been trying, and I’m like trying lean towards it too. Cause I, I watch it and I wanna see, show me, show me, you’re trying to wean him off, and what is he on? And, and I kind of see his body just, it’s not taking it. So I’m kinda like, oh, okay. Each doctor like each week is a different doctor.
Patrik: They’re all telling you the same?
Isaac: Yeah, like yesterday they are trying to push for the percutaneous endoscopic gastrostomy (PEG) tube and they said like, “What are you waiting for?” I said, “Well, what I am honestly waiting for is, for him to be weaned off the ventilator on his own.”
Patrik: Look, it sounds to me like, a tracheostomy is the right next step. If I was you, I would not necessarily consent to a percutaneous endoscopic gastrostomy (PEG) tube. Are they telling you they wanted to do the tracheostomy and the percutaneous endoscopic gastrostomy (PEG) tube at the same time?
Isaac: There’s a feeding tube in his nose. So its kinda like it’ll help. It’ll be hard with the secretions when he has a tracheostomy. So they’re the same time, I sense like, and eventually, we’d be able to close up the feeding tube, and the tracheostomy if he gets better, but they just don’t wanna leave it like that. And they don’t think it’s temporary so-
Patrik: Yeah. Yeah. Look, I, so are they saying a percutaneous endoscopic gastrostomy (PEG) tube first and then tracheostomy? That doesn’t make sense to me.
Isaac: Yeah. Cause they said like it will be really hard for him to breathe if he will be on tracheostomy while doing the percutaneous endoscopic gastrostomy (PEG) tube.
Patrik: Right. And, and when do they wanna do that?
Isaac: Well, they wanted to do it since last week and they keep telling me that it is time, but I told them, “ No, let’s just wait.” And they kept asking, “What am I waiting for?” I said, “Honestly, I’m waiting for this weekend for hopefully he breathes better without the ventilator and we can wean him off on his own”, but I understand it’s not happening. And I’m waiting until Tuesday? And they’re like, “Well, why Tuesday?” I’m like, “Well, you never know if a miracle happens between these days. I’ll just, hopefully, could try to wean him off to tracheostomy, off the ventilator, and to regular oxygen to get him home and just have more relatives there at his side.”
Patrik: Yeah. Look. I, I tell you my thoughts. Let’s put it that way. I do have a problem with the percutaneous endoscopic gastrostomy (PEG) tube and I tell you why I have a problem with a percutaneous endoscopic gastrostomy (PEG) tube. I have seen patients with a nasogastric tube for many months and there is no issue. There is usually no issue.
Isaac: Yeah.
Patrik: Right. So I don’t think. I do believe to a degree. They are misleading you a little bit here and I tell you why. I think they’re misleading you once he has a tracheostomy and percutaneous endoscopic gastrostomy (PEG) tube, he’s a candidate for LTAC. With the tracheostomy, he is a candidate for rehab. They will take the patients to the LTAC. They will do the tracheostomy and percutaneous endoscopic gastrostomy (PEG) tube to kick him out as quickly as possible.
Isaac: Oh, okay.
Patrik: Yeah. That’s why I am not in favor of doing a percutaneous endoscopic gastrostomy (PEG) tube on your dad now.
Isaac: Yeah, I understand.
Patrik: Okay. After I discussed to you the LTAC. May I ask if he’s receiving his feeding?
Isaac: Yes, he’s receiving it.
Patrik: That’s great. He’s absorbing the feeds?
Isaac: Yeah.
Patrik: That’s great. That’s great and then, when I look at the ventilator, he is on a fair bit of support, still, actually on a lot. Has he had time on the tracheostomy mask at all?
Isaac: No.
Patrik: No. Okay. He’s on a lot of support, still on the ventilator. Have they laid out a plan in terms of how they want to wean him off the ventilator?
Isaac: Well, I was speaking with the doctor because when I talked to her two days ago, he has to do the tracheostomy and I declined the percutaneous endoscopic gastrostomy (PEG) tube, and the doctor said, “Well, what is your reason?” I said, “Well, he’s actually feeding through his nose right now and that’s not our main problem. He’s actually getting fed, so we just want to go through with the tracheostomy and see if we can wean him off the tracheostomy to regular oxygen and find out how that goes,” and she says, “Okay.” I said, “Maybe we can wean him now. We never know but when it comes to the percutaneous endoscopic gastrostomy (PEG) tube, we’ll do that later.” She said, “Okay, I agree with you. We’re going to do that.” Then, the operation doctor or whoever was supposed to do the procedure kept seeing him so my dad’s blood pressure goes up very, very high and then it goes very, very low. I’m not sure if it’s due to the .. Is it called Precedex?
Patrik: Yeah, that was my next question. That was my next question. He has had the tracheostomy already, has he?
Isaac: No. No, they haven’t done the tracheostomy because now they want to do the tracheostomy and the percutaneous endoscopic gastrostomy (PEG) tube at the same time when I had declined the percutaneous endoscopic gastrostomy (PEG) tube. I never signed for the percutaneous endoscopic gastrostomy (PEG) tube. I told them, “No,” because I was going after your advice.
Patrik: Right.
Suggested Links:
Isaac: Yes, so then she said since his blood pressure keeps going so low and so high, but I told her, “Maybe his blood pressure is really low right now because you guys have him on a semi-sedation. I know it’s very low but he’s 89 something pounds. I’m thinking why do you guys have it during the day? He only needs it to sleep at night and then, is there anything else that they give him to sleep? I guess he’s getting where he can’t sleep because, I don’t know if he’s nervous or what is it?
Patrik: Right. Are they giving something else besides the Precedex?
Isaac: No, just the Precedex at 18. Oh, they are giving him something for his blood pressure.
Patrik: What are they giving for the blood pressure? Is it-
Isaac: Something to raise it.
Patrik: Say it again?
Isaac: They’re giving him something to raise his blood pressure.
Patrik: Yeah, to raise his blood pressure. Yeah. It’s probably something like Levophed or norepinephrine or epinephrine.
Isaac: Yeah.
Patrik: You haven’t heard of that?
Isaac: Yeah.
Patrik: Okay. Okay, so are they basically not doing the tracheostomy because you haven’t given consent to the percutaneous endoscopic gastrostomy (PEG) tube? Is that what’s happening?
Isaac: I think so because the doctor agreed with me. She said, “Okay. I won’t do your percutaneous endoscopic gastrostomy (PEG) tube.” She said, “I understand how you feel and what the family says and you know? I have no problem with that.” She said that. I said, “Okay so let’s do it,” I said, “But I’m not going to sign for the percutaneous endoscopic gastrostomy (PEG) tube. I don’t want to do that right now.” I said, “I’m not saying he might not need it later. Maybe, maybe not but when we get there, we’ll do it.” She said, “Okay.”
Isaac: A couple of days passed and another doctor came to see them, and he questioned the other doctor, “Why are you agreeing to do the tracheostomy without the percutaneous endoscopic gastrostomy (PEG) tube?” He says, “His blood pressure is going very high and very low. Why are you going to put the patient through double surgery?”
Isaac: I tell him, “Well we could space it out in that case.” I said, “But, right now the problem is not the percutaneous endoscopic gastrostomy (PEG) tube. The problem is doing the tracheostomy. We’ll try to see if we can wean him off the ventilator from the tracheostomy. Just keep the breathing tube out and keep him alive.” Then they said, “Well the problem is, we don’t want to put your dad so fragile. I mean due to his blood pressure going up and down, the other doctor was telling me maybe it’s a better idea we do the two-in-one surgery at the same time so we’re not putting your dad through so much trauma.
Recommended:
- The 10 things you must know about ventilation & tracheostomy weaning in intensive care- live stream!
Isaac: I said, “You know I’m going to wait on that. I do sign for the tracheostomy,” I said but I’ll talk to the family today and I’ll let you guys know tomorrow. Right now, I’m just authorizing the tracheostomy, but I did see my dad’s vitals and I said, “Oh, man. I don’t know if I’m making the right decision. Should I get you a two-in-one?” What do you think?
Patrik: What are they telling you are the next steps? They still want to push you out to LTAC, don’t they?
Isaac: Oh, I told them, “After they do this, you’re just going to send him to LTAC.” “Oh, we’re going to try to wean him off the ventilator and oxygen because you want him home on hospice.” I said, “Yeah,” and I said, “If that fails? How soon are you guys going to send him to LTAC?” She said, “Well, I don’t know why you’re worried about LTAC. I said, “Well, because that’s how it usually goes. He’s not going to stay in here forever with a percutaneous endoscopic gastrostomy (PEG) tube and then the tracheostomy.” Then they said, “Oh, we could send him out to LTAC right now.” I said, “No, you won’t send him to LTAC with a temporary feeding tube through his nose. They’re not going to accept him.” “Oh, at LTAC, they could do the percutaneous endoscopic gastrostomy (PEG) tube as well.”
Patrik: Okay. Well, all of a sudden, the tone changes.
Isaac: Yeah.
Patrik: Mm-hmm (affirmative). Okay.
Isaac: Well, it’s just I signed for the tracheostomy. I’m going to wait on the percutaneous endoscopic gastrostomy (PEG) tube. I’ll talk to the family. I understand it’s like a two-in-one procedure because they’re worried about how fragile his body is and his blood pressure and why put him through two surgeries versus just one. Go through them at the same time and I’m just kind of like.. I do see his blood pressure going really low and then sometimes it goes high. I don’t know if it’s because of the Precedex or …
Patrik: Yeah, the Precedex-
Suggested Links:
- Quick tip for families in ICU:You were absolutely right, LTAC is a complete waste of time after ICU!
Isaac: Or, what it is.
Patrik: The Precedex would get his blood pressure down. No question.
Isaac: For sure, huh? Yeah, I told the doctor that too. I said, “Well, why do you guys have him on Precedex during the day if you guys have him off completely.” “Oh, he wasn’t sleeping.” I said, “He doesn’t sleep during the day just during the nighttime.”
RECOMMENDED:
Isaac: I said, “Well, why don’t we stop the Precedex right now and see how his blood pressure goes?” “No, we want him comfortable.” I go, “He looks comfortable to me.” But, they didn’t stop it. I said, “Well, you guys have been saying he can’t go through the surgery unless his blood pressure goes up, why don’t we turn off the Precedex if it’s not really necessary during the day. Why are we giving it to him,” I told them. “Oh, just to keep him stable,” and then I asked her, “Well, doctor,” I’ll have to ask her like it was her idea because then, they don’t like hearing that. I told her, “Well, don’t you think it can lower his blood pressure?” “Well yeah, it can.” I say, “Well, you have been saying the blood pressure’s too low that you don’t want to do the tracheostomy so maybe we should turn it off?” “Oh, we’ll look into that but right now we’ll just keep him comfortable.” I don’t know.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







