Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last week’s question by clicking on the link here.
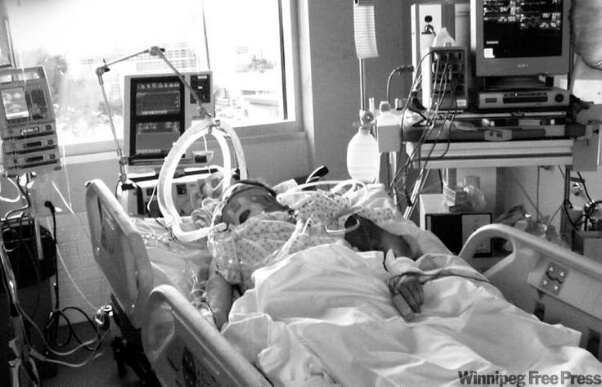
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkin’s Lymphoma and is currently experiencing decrease in blood count as well as having second thoughts about the treatment her sister is getting.
The Intensive Care team is wanting to stop or “withdraw treatment” against Andrea’s and her families wishes and she’s not prepared to let her sister go without a fight!
The Medical doctors completely gave up on my sister and is letting her die. What can I do about this?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Andrea here.”
Patrik: But you didn’t inform the family when you made that decision. You didn’t inform the family when you made that decision. That would be a point of criticism.
Dr. Charkow: No, I forgot. I did actually say, that we would resuscitate her and that I would give blood transfusions as appropriate.
Dr. Rosebud: Yes, but that’s not the question. The question is you spoke to the Russian to the Russian doctor and made the call.
Dr. Charkow: So, a decision has been made not to resuscitate the patient.
Dr. Rosebud: And she asked to resuscitate and your sister said she would do that and then they saw a file, not to resuscitate. So, a decision was made not to resuscitate and was changed back only when the family asked to change it. We don’t know who made that decision, whether they stand and totally agree and we don’t know why that happened.
Andrea’s Mother: The way I see it is there are a lot of questions that aren’t going to be answered today. They’re going to be outstanding because even when trying to answer them in front of answering it with Sarah. So, I don’t know if it’s you know with a way of losing your sister.
Andrea: Okay, I’ll explain to you what happened. I went downstairs asking… all I want is the computer records. I don’t need the paperwork at the moment because I don’t trust you, to be honest with you. I thought it was really there, on the computer, okay. I thought it with my own mind because I’m not happy with the level of care you’re giving out. I’ve been calling lawyers; I’ve been trying to find out who in this hospital do I need to complain. And I bet you, I will find who it is whatever it takes, no matter what.
Andrea: She’s my younger sister and I will fight and I will continue fighting for her, even when she’s under the grave.
Dr. Miller: Your sister has been-
Andrea: I don’t’ know what you’ve been doing to her, bordering malpractice.
Dr. Miller: Your sister has been resuscitated and continues to have been be resuscitated.
Andrea: But… you’ve been doing with her what??
Dr. Miller: No one sits in intensive care with a tube down their throat on a ventilator, not being resuscitated.
Andrea: But you’re not giving her the full care, which is blood. That’s what I’ve been telling.
Related information:
Dr. Miller: …with respect to the order for not resuscitation, it’s not to perform CPR (Cardio Pulmonary Resuscitation) in the event that she, her heart stopped beating.
Andrea: Maybe because she’s got a healthy heart.
Dr. Miller: in the event that she…. Can I just explain what we would..
Dr. Rosebud: She likes to be more informed, okay and you know and I believe everything you say about the patient. The things that this man said to my wife the other day about her sister lying in intensive care is completely unacceptable, okay. Because it’s completely inappropriate. You refused information to my wife, under the freedom of information. You said no.
Andrea’s Mother: Yeah, well, I was trying to finish what I was saying. We will continue to receive complaints so we will manage that.
Recommended:
Andrea: The whole point is that we have feel that our sister has been given the due treatment that you would give to a patient. We feel that the treatment has been inadequate. Our sister be treated with 100% care like you would treat any patient even when they die. What do we have to do today, to move forward because we can do this all day and it’s not helping my sister, so what do we have to do now. To be able to move today.
Dr. Miller: She’s in a deep coma. When she becomes brain dead, she won’t be any… she won’t feel anything. When your brain is dead, you are medically-
Andrea: How do you know when she’s brain dead.
Dr. Rosebud: Your body won’t be able to tolerate….
Dr. Miller: You’re medically and legally dead.
Andrea: And how do you know when she’s brain dead?
Dr. Miller: We will do brain dead assessment at the bedside. If you don’t trust me, I’m happy to get someone else.
Andrea: No, I don’t trust you, to be honest with you, I don’t trust you.
Dr. Miller: Okay.
Find more information about brain death:
Andrea: What’s your name? Can I trust you? And I really think that care possibly I can trust you but you I completely don’t trust you, okay.
Dr. Miller: It has to be done by two separate doctors.
Andrea: And your manner of engagement is deeply unprofessional and I’m sorry, I’m being very direct with you. I’ve been very stressed when move her to a different hospital and that’s very sad because she’s in such a critical condition. How do I get this?
Dr. Miller: All I can say is I’m very sorry that-
Andrea: No, you’re not sorry. If you were sorry, you would have done everything for her. You would have given her blood as she needs it and even she was not going awake up that’s okay, at least you tried. At least you tried. I just want it and I’ll even donate my blood. To keep her alive and you didn’t do all you can. You gave up. I’ll fight for her because she went through everything. She fought through it. She’s strong, she’s always been so strong and you decided that too much blood will cost you and that is a valuable resource that costs too much money. That’s what you said she was. That’s what you said she was. Sunday evening, which I found really disgusting because as a doctor you’ve sworn a professional oath your duty to every single patient, okay.
Andrea: You really need to question whether you. I don’t think my sister is. I know you don’t think that but you’re not God. She’s in the power of, she’s in the hands of God. No one here has got that power to end her life. And not to get treated. And not to give her the full care.
Dr. Charkow: On the basis that she has been having evidence of seizures. On her EEG. On her last recorded EEG (Electroencephalograph).
Recommended:
Andrea: And when was that done?
Dr. Charkow: The 22nd and 23rd.
Andrea: Okay, and you decided on the, what day is it now?
Dr. Miller: I didn’t have the report in front of me and I wasn’t told otherwise and in order to try to get someone to wake up. If that’s what was causing her to be unconscious, I gave treatment to try and see if that would improve her level of consciousness.
Andrea: And what is there a lot of Keppra?
Dr. Miller: I gave Keppra to try to suppress seizures as they were happening. I didn’t have any bedside measures to assess whether she’s having seizures but I was going to increase the dose to see if that would improve her level of consciousness and repeat the EEG (Electroencephalograph) this morning.
How the level of consciousness is being measured:
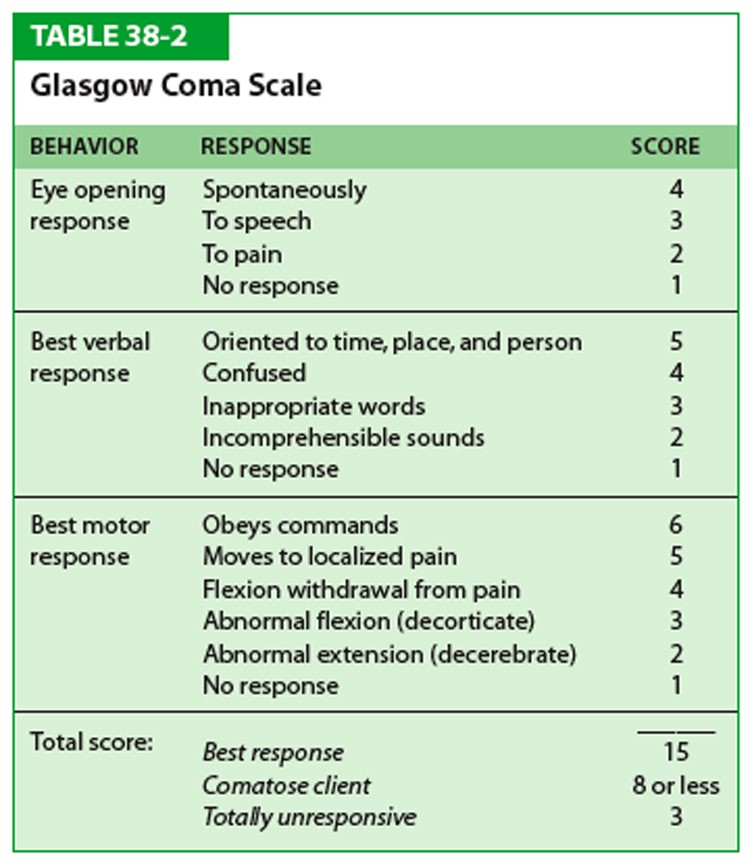
Andrea: But why there’s a lot of Keppra?
Dr. Miller: I gave Keppra to control seizures that were documented electrographically on her EEG.
Andrea: But that was on the 22nd. Its six days later. You saw, okay, you saw when you touch her hand she was moving because it was uncomfortable for her so she actually had movement. She was moving her hand and her eyelashes-
Dr. Miller: I think we should finish now.
Andrea: Of course you do.
Dr. Miller: No, no. I’ve got 14 other sick patients to deal with. I’ve had a very stressful week. You’re not the only sick and family members of patients.
Andrea: I need your background!!!!
Dr. Miller: I’m sorry.
Andrea: I really don’t care about your feeling!!!
Dr. Miller: I have a job to do with other patients.
Andrea: You told me….
Dr. Miller: I’m sorry, that’s really not acceptable.
Andrea: I really wanted to go back I think…
Dr. Rosebud: I’m sorry that’s really not acceptable. I don’t care.
Andrea: Go on, just let him go. What do we need to do now? We want to do something now. Is there any way that you can save her?
Dr. Charkow: No.
Andrea’s Mother: No.
Andrea: At all? You just got your job?
DR Miller: They speak to each other every night. The director of intensive care is aware of what’s going on. She’s got a copy of the treatment, unfortunately, Diana’s not going to change, she’s a product of her disease. I appreciate your presence. You are absolutely free of whatever you need to do. We are available but we want you to spend time with your sister.
Andrea: But why did you to refuse to give her blood?!
Dr. Rosebud: It doesn’t matter. We’ve tried everything.
Dr. Rosebud: We’ve all tried our best. The blood would have not done anything.
Dr. Rosebud: That man told my wife to jump on her chair.
Andrea: Patrik?
Patrik: Yeah.
Andrea: What are your thoughts?
Patrik: Well, my thoughts are that with having told you that a few weeks back, she’s needed a resuscitation and then they decided not to resuscitate her and not give her blood without informing you is highly inappropriate.
Related article:
Andrea: Okay.
Patrik: That is highly inappropriate. Am I on speaker phone at the moment?
Andrea: What’s that?
Patrik: No, that’s okay. My thoughts are, I tell you what my thoughts are. If she is really brain dead or she’s heading towards that, there is very little anyone can do but, you’re absolutely right. What’s been leading up to this is highly inappropriate and I can just hear, how they are. The level of disengagement, it’s highly, highly questionable. There is no question around that. I do believe that with everything that’s happened there, you may have to escalate this.
Patrik: But if your sister, for whatever reason today, becomes brain dead then there is very little they can do at this point in time. I can confirm that if they think that she is brain dead, that there need to be two independent parties to confirm that. I can confirm that. That is standard practice.
Recommended:
Andrea: Okay.
Patrik: What I didn’t quite get is that. She did have a CT brain this morning didn’t she?
Andrea: Yes.
Patrik: So, why are they not, they said they can’t do anything before she had the CT of the brain. I didn’t quite get that. Why are they still waiting for the formal report?
Andrea: What was that? Sorry.
Patrik: Are they still waiting for the formal report of the CT?
Andrea: I’m not sure. Patrik, I’ll call you back.
Patrik: Please.
Andrea: Okay.
Patrik: Please, please. Bye.
“Thank you very much for being a part of these series of 1:1 consulting and advocacy sessions. This will be the end of the story about Andrea and her sister. Stay tuned for an upcoming new series with a new client next week!”
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!