Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What are the Chances that My Ventilated Mom Will Wake Up After the Tracheostomy in the ICU?
You can check out last week’s question by clicking on the link here.
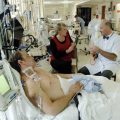
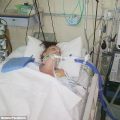
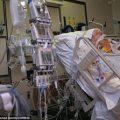
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy. Alexa’s mom is with a breathing tube and on a ventilator with ICU psychosis. Alexa is asking if the ICU psychosis is the effect of giving her mom too many sedatives in the ICU.
The ICU Team is Giving My Mom Too Many Sedatives & Now She Has ICU Psychosis! Help!
“You can also check out previous 1:1 consulting and advocacy sessions with me and Alexa here.”
Alexa: Hi Patrik!
Patrik: Hi Alexa! How’s your mom?
RECOMMENDED:
Alexa: My mother has been in a delirious state since last weekend, which is about 7 days now, and this is what’s concerning me the most, and I spoke to the doctors about it, and they told me it’s encephalopathy, and this is the result of 2 things. Typically, it’s she’s immunocompromised, infection, and then sepsis, also, and then along with also the … Which they don’t do anything. That the drugs have an effect, like the sedatives, but I mean, all the literature that I’ve been reading seems to suggest that the sedative does play a big part in that.
Patrik: For sure.
Alexa: So, that’s my concern at the moment. And her lungs, the respiratory therapist was there today and asked her how her lungs were doing and she’s like, “They’re stable. She still needs support in breathing.” But it’s just been a very long time now.
Alexa: And then one of the doctors that I met with last week, she’s been working in an ICU for almost 30 years. And she just told us, she’s like, “Look, she’s experiencing probably some level of psychosis, and she could be sort of manifesting as hallucinations and dreams and this sort of thing. Could very well be like bad things also.”
Alexa: And so that’s when I went, and I looked up some patients who have gone through these experiences with bad delirium and just see what their experiences were like. And a lot of them, they tell these stories about how they have these nightmare experiences, so lots of concern. The doctors just basically told us her quality of life afterwards for her to recover from all this, it’s not going to be a good prognosis for him. He didn’t say it directly, but she’s like, “If it was my parent who was in this situation, I would’ve considered the other options by now.”
Patrik: Yeah. I’m following and I’ve seen patients with ICU psychosis/delirium/encephalopathy all the time. You’ve seen your mom just now?
Alexa: Yes. I just got back. I just left the hospital.
Patrik: And how would you describe her? Is she awake?
Alexa: Yeah, she’s awake. Her eyes are opening and she’s just really moving her body, her legs and her arms. It’s uncoordinated, so she’s just kicking about a lot. Her arms are just splayed, just kind of moving everywhere. She’s moving her head from side-to-side. Her eyes open and shut. So, she is active. It’s just that I’ve tried to connect with her, and there isn’t any conscious connection that’s going on. She’s not coherent in any way.
Patrik: Yeah. Is she responding to you personally? Is she recognizing you?
Alexa: No.
Patrik: Right. And she never has since she’s come out of the coma?
Alexa: No, she has. When she came out of the coma, it took her a while to wake up and then that same week when she was coming to, I was going to see her and then there was this connection. At that point, she recognized me. The doctor was there. I told the doctor, I’m like, “Look, she’s awake and she’s conscious and she’s alert. She’s mentally, She’s alive. She’s there.”
Alexa: She was like that maybe for three, four days, and then the delirium started.
Recommended:
Patrik: Right. Here is my take. When was the last time she was on sedation?
Alexa: She’s still on sedation today.
Patrik: And what are they giving her?
Alexa: Their daily dose is 12 to 14, I’m sorry. Between 8 and 12 mL of propofol, and then about 8 to 10 of fentanyl.
Patrik: That’s madness. And the reason I’m saying this is madness is there’s a couple of things there, Alexa. So, you may recall when your mom had the tracheostomy, one of the reasons you do a tracheostomy is so you can minimize sedation or stop sedation. So, a breathing tube in the mouth is so much uncomfortable compared to a breathing tube in the neck, i.e., the tracheostomy.
Patrik: So, once you’ve done a tracheostomy, the need for sedation should no longer be there unless people have gone through surgery, they’ve got massive pain. I argue that if she’s getting the propofol and the fentanyl, the delirium is getting worse, not better. So are you saying-
Alexa: I’m starting to think the same thing. Okay, yeah, go on, Patrik.
Patrik: Just remind me, how many days on tracheostomy now?
Alexa: So, I should’ve journaled all this experience, but I would say at the beginning of January, so probably now already 3 weeks in, 3 and a 1/2 weeks.
Patrik: And propofol and fentanyl has been going since?
Alexa: So last time I asked, I didn’t ask them how long of a duration has she been given this on a daily basis, but I can ask to get those specifics, but I think it’s been continuous.
Patrik: Wow.
Alexa: And then when I asked the doctor, because during our last conversation you told me, “Alexa, go ask the doctor why are they giving her the painkillers and the sedatives.”
Patrik: Exactly.
Alexa: And so, I have that nurse and she told me it was for her comfort, and then I asked the doctor, and the doctor said, “No, it’s because her breathing is not synchronized.” So, they’re trying to synchronize her breathing with the machine, and apparently for those reasons, she needs to be given one of those. I don’t know which one, but she needs to be given medication.
Patrik: I can see the need for a little bit of propofol. I don’t see the need for fentanyl. Do you know the difference? Do you know the difference between propofol?
Alexa: I do. Yeah, propofol is a sedative.
Patrik: Yeah, correct.
Alexa: And fentanyl’s an opioid.
Suggested links:
Patrik: That’s right. And one of the main side effects of an opioid is respiratory depression, which means it inhibits respiratory drive. So, it’s like fentanyl has its time and its place, but not for someone in the later stages of ventilation and I argue your mom is in the later stages of ventilation.
Patrik: In the early days, when someone has a breathing tube in their throat and it’s very painful, I understand, and I would support the need for fentanyl or for morphine. But no, not anymore. Your mom doesn’t have any surgical wounds.
Alexa: Yeah, so no surgical wounds of any sort. What about the dialysis?
Patrik: No.
Alexa: Would that be something you’d give her fentanyl?
Patrik: No.
Alexa: Okay.
Patrik: No. Absolutely no. How much fentanyl is she getting? Do you know?
Alexa: Yeah, between 8 to 12 mL.
Patrik: An hour?
Alexa: An hour, yeah.
Patrik: That’s a lot. That’s a lot. Okay. So, the other side effect of fentanyl, unlike the propofol, is addiction. So, if you give too much fentanyl over long periods of time, your body gets addicted. So, your mom is already in an ICU psychosis or in a delirium. If they stop the fentanyl, that would even get worse because she might go through withdrawal. Very likely will go through withdrawal.
Alexa: So, they have to wean her off that?
Patrik: Have to wean her off gradually. Gradually. So propofol is not addictive, but propofol also comes with side effects, of course, I argue. So, here is how I have seen this happen when patients are in ICU psychosis and they’re not waking up properly. They’re agitated, they’re combative, confused, and you could put some other labels on that. Stop propofol, wean off the fentanyl gradually, and start medication such as Precedex in this day and age. I will email you those names, Precedex or dexmedetomidine. Also, medication such as clonidine. Again, I will email that to you. Also, medicine maybe such as quetiapine or olanzapine to manage the psychosis.
Patrik: As I said, as far as I can see, the minute you do a tracheostomy, one of the very reasons you do a tracheostomy is to eliminate the need for any sedatives and opioids. That’s one of the main reasons. And I don’t understand why they continue doing that.
Recommended:
- My mother’s been in ICU for 8 weeks on a ventilator with tracheostomy, can she go home? Live stream!
Patrik: Maybe there is something that I don’t know.
Alexa: I don’t know why. I don’t know. From what I’m reading, but it’s very common in the ICU. It’s part of the culture.
Patrik: No.
Alexa: To continuously give sedatives.
Patrik: No.
Alexa: I mean, maybe.
Patrik: No, no.
Alexa: So, do I have the right, Patrik? Do I have the right? I mean, can I take initiative. Like, I don’t want you guys to give her fentanyl anymore. Do you have the right to ask for that?
Patrik: Well, (a), it’s inevitable for you to ask. It’s inevitable for you to ask because she’s not moving forward, is she?
Alexa: No, but I mean, obviously, I’m assuming that they know that the fentanyl is part of the reason in why she’s in this state of delirium. And then they should have taken it upon themselves to do other … Why aren’t they making these changes? Why would I have to say anything if they’re sort of informed of their … They’re experts.
Patrik: I agree with you. Why are they not doing it? I don’t have the answer. I really don’t have the answer at the moment. I would need to look at all the medical records or what we can do, I’m very happy to get on another call with you with the doctors or with the nurses and dig a little bit deeper. But I can tell you from experience that ICUs can be very complacent. And maybe they’ve tried a different approach and maybe it didn’t work so they went back to the old approach. And maybe they’re scared to try again, I really don’t know.
Patrik: They are the experts. I agree with you. If you look at it from a bigger picture perspective, Alexa, my business should not exist if everyone was doing the right things.
Alexa: Yeah, I get it. Right.
Patrik: And you can now see what they’re doing is not working. Here is another element, I believe. So, in a perfect world, your mom would be off fentanyl, she would be off propofol, and now she should be at the stage where they’re starting to mobilize her. So, imagine, and here is where two different worlds clash, on the one hand you’ve got her now still sedated after all this time. And picture the other side of this coin which would be stop sedation, try different approaches, and get her out of bed, get her mobilized. And I know that sounds crazy to you at the moment, but that is what needs to happen.
Patrik: A good ICU will very gently, step-by-step, and often it’s like you mobilize someone for 5 minutes today. They’re exhausted, you put them back to bed. The next day, you might do 10 minutes. And the next day, you might do 15 minutes. Baby steps. But been there done that.
Alexa: No, I agree with you 110%. What I mean is it doesn’t serve their purpose if these patients are indefinitely sort of committed to the ICU unit. I mean, obviously, they want the progression as much as we want it. I mean, they’re not there providing these long-term hotel stays either.
Alexa: I don’t know why these things are happening, Patrik. Maybe, like you suggested, the doctors on the rotation this weekend is Dr. Moore. He’s a younger doctor, but I have a very good rapport with him and maybe we can get on the phone with him and find out a little bit what’s going on today. He just started his rotation today, so he told me and the was going to get ahold of me tomorrow so that he can sort of study my mother’s file and see what’s changed, what’s not.
Alexa: And so, I’m going to talk to him tomorrow and I’ll try to get more information. But, I guess, Patrik, I don’t mind the time but if you can let me know when you would be available, then I’ll go ahead and schedule that call.
Patrik: Yeah, absolutely. Now here is another thing, Alexa. So, the last picture of the ventilator you had sent through, your mom is on, I wouldn’t say on minimal settings, but on very low settings. Okay, so I argue that if they get the psychosis under control, you have every reason to believe that she will be off the ventilator very soon.
Recommended:
Alexa: I don’t know right now whether she’s on the ventilator because she needs it or whether she’s on the ventilator because of the delirium.
Patrik: Correct.
Alexa: The psychosis..
Patrik: Correct. Absolutely. I think you should be optimistic that once they get this under control, she could be off the ventilator fairly soon, assuming that the last picture you have sent through, she hasn’t deteriorated from there.
Alexa: Yeah, so I’m going to need your help, because obviously, I’m not going to be able to advocate for whatever’s going on. And if it’s this much of an urgency to get her off the fentanyl and wean her off because this is one of the culprits in the delirium and this is maybe what’s causing the delirium, then maybe I wouldn’t be able to express that as well as you would.
Patrik: No, no. I agree. Here is another thing why is this happening. A big thing that is happening at the moment is, and it may sound crazy for you, but staff in ICU all around the world are burned out. They are burned out. It’s been a hell of a last 2 years for everyone.
Alexa: So, everything is on autopilot.
Patrik: Or everything-
Alexa: Standard operating procedure and that we just do what we’re told.
Patrik: That’s right.
Alexa: And it’s not more than that or whatever.
Patrik: That’s right. And also in the last 2 years, there would have been a big influx of junior staff into ICU, whether on a medical or on a nursing level.
Alexa: Yeah.
Patrik: Right?
Alexa: There is actually. There is a lot of resident doctors there.
Patrik: Yeah, a big influx of junior staff because otherwise they couldn’t have coped. So, the junior staff don’t really know what they’re doing yet. As you said, a lot of it is happening on autopilot. People are burned out, they’re tired. And unfortunately for them, your mom is just another number.
Alexa: Yeah, I know. It’s crazy. It’s not like I just brought my car to the mechanic’s shop. It’s a life that you’re dealing with. But they’ve become so desensitized, and I feel sorry for them to a certain extent. So, Patrik, look, we have to do something about it. Because this delirium, I know the longer she’s in this state, the longer there’s this increased chance of mortality from what I’m understanding. There’s also other complications that have resulted in her staying in this state for so long, and that’s what’s scaring the hell out of me.
Patrik: Absolutely. How old is your mom again?
Alexa: 74.
Patrik: Right.
Alexa: And her mind, she was completely mentally intact. She didn’t suffer from any dementia, Alzheimer’s, nothing like that. Her mind was sharp. Full sharp.
Alexa: But okay, last question. In your experience, patients that have gone through such long ICU stays and having experienced delirium. Because they’re selling me, again, the doctor when I met her last week, she’s like, “It’s not going to look for good for even if should he recover.” What do I expect from this? Do you have any..
Patrik: I’ll tell you what you can expect. Approximately 90% of ICU patients survive. Approximately. Of course, there’s always a risk that people don’t survive, but if you look at the numbers, just surviving ICU, the odds are in someone’s favor. Now, what that number doesn’t mean is, or what that number of survivors doesn’t talk about is, what does quality of life look like down the line? And I think that’s the question you are facing here?
Alexa: Yeah, because it’s so long.
Recommended:
- I’m Very Grateful That I Found You! Your work saves Many Lives When ICU Prefers To Kill The Very Ill
Patrik: Correct. So, you got to picture this. I just mentioned a minute ago, mobilization. The longer your mom, for lack of a better term, is withering away in an ICU bed, she gets more and more deconditioned, which is why I kept talking about mobilization. I’m very old-school. I did my training in the 1990s. I’m very old-school. We were mobilizing patients all the time and we got them better. But it’s not happening any more in this day and age. People are complacent.
Alexa: Yeah, it’s just like you’ve been bedridden. Listen, I’ve been reading and like I had asked last time, normally, it’s also maybe some hospital do this differently, but they have occupational therapists that they bring in through the ICU that help people move around because … Yeah.
Patrik: But Alexa, you don’t even need an occupational therapist. You need a nurse and your next-door nurse, the nurse that’s working next to you, and you can mobilize the patient. Yes, ideally, you get an occupational therapist. Yes, ideally, you get a personally therapist, but initiative goes a long way.
Alexa: Okay, and last, Patrik, one question.
Recommended:
Alexa: Because I have this guy that I work with. He’s a trainee nurse right now and he mentioned that the hospital that my mother’s been admitted to, they don’t provide the best care.
Patrik: Sure, sure.
Alexa: There’s another hospital within our vicinity that’s quite close. It’s a new hospital. It’s a teaching hospital as well. So, he told me that I can go ahead and ask the doctor for a request to transfer my mom to that hospital.
Alexa: Now, in the event that people are hypnotizing through this regular ICU standard operating procedure where it’s not benefiting my mother, do you think that would then be a good idea to request a transfer to this new hospital where she might get better care, Patrik?
Patrik: Yeah, yeah. I think yes, like with anything, we all think sometimes the grass is greener on the other side. It could be a good thing. It may not achieve what you want. It’s difficult to say. I think the next step might be for you and for me to talk to the doctor and see whether we can get more information. I would hope that if he was to go to another hospital, one of the first things they would do is look at can we stop propofol? Can we stop fentanyl? And that, I hope, would be one of the first things that would do.
Patrik: Yes, you can achieve that. You can achieve a transfer. There are risks with that as well, of course. Like with everything.
Alexa: Yeah, okay.
Patrik: It’s-
Alexa: At least it’s an option that I can vet at some point if you mention to me at some point, “Look, these guys for whatever reason they are not looking after your mother’s best interest.”
Patrik: Yes, then..
Alexa: We’ll decide at that point, maybe they’d reconsider.
Patrik: That’s right. The other thing is this. From experience, when I worked in ICU and we were receiving a patient from another hospital, which happened all the time. But usually, it was for the reasons that the other hospital didn’t have the expertise to look after this particular patient because they had maybe a heart condition or they had went through a trauma. So, you were accepting patients from other hospitals that the other hospital wasn’t specialized to look after. In your mom’s case, I argue another ICU would not necessarily be specialized on ventilation weaning or on getting a patient through ICU psychosis because that is very common.
Patrik: If your mom had, again, maybe she had a heart attack and she needed heart surgery and they wouldn’t do it in this ICU, that would be a very different story. But transferring a patient that is long-term or a long-term patient, it’s a bit more tricky, if that makes sense.
Alexa: No, it does make sense. Maybe if they have better care management for whatever the reason is. Maybe the director, wherever the person in charge there, does things differently. I don’t know but I just wanted to put the best chances on my mother’s side. But again, I think maybe the best step forward at this moment is just get their reasoning as to why these things are already happening.
Patrik: Exactly. I think so, too.
Alexa: And we’ll just go from there.
Patrik: I think so, too.
Alexa: Okay.
Patrik: Let’s have a talk to them.
Alexa: So, yeah, Patrik, you’ll be there on Saturday?
Patrik: Yep.
Alexa: So, let me know what you’ll be available for and then I can coordinate the meeting.
Patrik: Yeah, Saturday is better for me than Sunday.
Alexa: Yeah.
Patrik: Okay. No, that’s good. That’s good. Yeah, look talk to the doctor and sort of this time of the day is pretty good for me.
Alexa: Okay. I’ll just wait for you to confirm, and then at that point, then I’ll be talking to the doctor.
Patrik: No, no, I can tell you now, Alexa. I can tell you now that we can do four o’clock again tomorrow.
RECOMMENDED:
Alexa: Four o’clock tomorrow? Perfect. Okay.
Patrik: Yeah.
Alexa: So, what I’ll do is I’ll get ahold of the doctor and then I’ll email you to confirm that.
Patrik: Yeah, please. Okay.
Alexa: Okay. Patrik, thank you very much.
Patrik: It’s a pleasure.
Alexa: I appreciate it. Okay, thank you.
Patrik: Okay, I will email you. I will email you some medication names to help someone get out of this situation.
Alexa: Okay. I really hope that all this helps because I can’t see her like that anymore.
Patrik: Yeah, I know. I get it Yeah.
Alexa: Yeah. Okay, Patrik. Have a good day and I’ll follow up to confirm.
Patrik: Yeah, same to you. Thank you so much. Thank you.
Alexa: Thank you, Patrik. Okay.
Patrik: Bye.
Alexa: Bye-bye.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!