Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
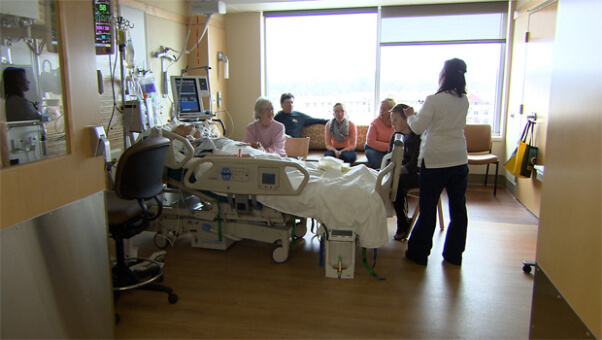
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another frequently asked question from our readers and the question in last week’s episode was
You can check out last week’s question by clicking on the link here.
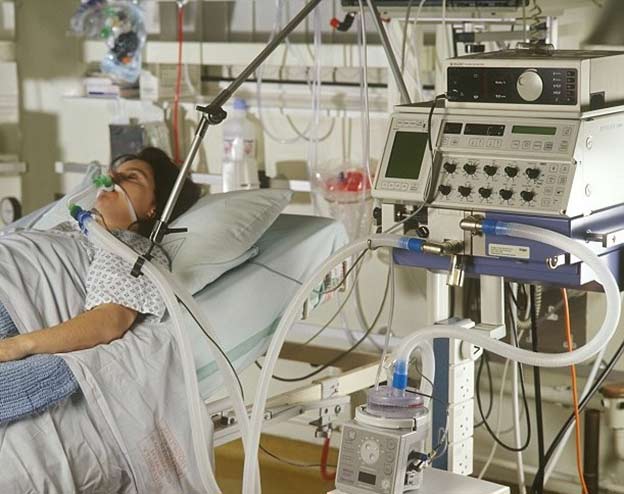
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions from one my clients Sharon who has her 64 year old mother transferred in the Intensive Care due to severe difficulty in breathing and alteration in mental state. Ultimately, her mother was diagnosed with liver failure and is on blood pressure medications and may subjected to dialysis due to kidney failure.
The ICU Doctors said my mother’s survival is unlikely! Is there any hope?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Sharon here.”
Patrik: Hi Sharon.
Sharon: Hi. I’m so sorry to call you again so quickly, but I got just one more bit of news that I just wanted to share with you. So they’re just giving her the platelets now because her blood was clotting and blocking some of the catheters.
Patrik: Her blood was clotting. Right. Okay.
Sharon: Yeah.
Patrik: And who have-
Sharon: But they’re not doing a full blood transfusion-
Patrik: Good.
Sharon: They’re just doing the platelets.
Patrik: The platelets. Yeah. No, no, that’s good. And … you know I mean, the less they do the better it is, you know I mean, that’s a sign, yes she has some clotting issues, but all they do is give the platelets and then probably reassess in a few hours.
Sharon: Right. So the clotting, is that different kind of than what we were talking about?
Patrik: No, no, no, no. Clotting and coagulation are the same.
Sharon: Okay. Okay. So, but the fact that they’re just giving her the platelets to start is a good thing?
Patrik: Yeah, look, I mean, yeah-
Sharon: Or it’s just a thing?
Patrik: It’s just a thing. I mean, the other blood products they’re giving to manage the coagulation is the fresh frozen plasma, also known as FFPs. Right?
Sharon: Right.
Patrik: They’re often giving both, but it’s good that they’re only giving platelets. I see that as a good sign, you know, again, the less they are giving, the better it is.
Sharon: Yeah and her blood pressure was up to something like 112 over like 68 or something.
Patrik: But that would be on norepinephrine, most likely.
Sharon: I’m sorry?
Patrik: That would be on some norepinephrine.
Sharon: Yeah, but not a lot.
Patrik: Okay, good.
Sharon: They lowered it down.
Patrik: Yeah and-
Sharon: So it’s probably back … It’s probably back down to like the eighth.
Patrik: Good, and that would also most likely … giving blood product will get the blood pressure up.
Sharon: Okay.
Patrik: Right.
Sharon: Okay. All right then.
Patrik: So that all makes sense by giving blood products, her blood pressure is coming up. That makes sense.
Sharon: Okay. All right. Thank you. I just wanted to-
Patrik: You’re very-
Sharon: … let you know that.
Patrik: You’re very welcome.
Sharon: All right. I will connect with you later.
Patrik: Sure. Take care.
Sharon: Okay. Thank you. Bye.
Patrik: Your welcome. Bye.
Recommended:
Patrik: Hi, Sharon, how are you?
Sharon: Not good. They were just very, very negative. So I wanted to get your advice. At first we talked to a nurse who seemed very positive and… not positive, but she’s like, “These are the things we deal with.” Blah blah blah. And then the doctor came. She’s like, “Well, she suffered a very serious setback with the clotting, and we just might start asking to talk about… we’re not sure if she’s going to make it now.”
Patrik: And sort of was that a lengthy discussion? Or was that just at the bedside, sort of as they were passing by? How did that sort of situation goes?
Sharon: No. We were just having a sit there, and she just kind of told us.
Patrik: Okay. So that wasn’t a formal meeting, it was just sort of at the bedside, right?
Sharon: No. No.
Patrik: Right. Okay. And did you ask any questions? You sort of just let it sit there? What was your response?
Sharon: She just said that because… I said I want to keep doing whatever we have to do, because people say that with time she can heal. And they were like, “Well, we just want to be, with the setbacks, honest with you because with the blood clotting…” And she is bleeding a little bit from her gums, I guess.
Patrik: Okay, yeah. Yeah. I think the next step really is that sooner or later you almost have to ask for a meeting with the treating specialist. Right?
Sharon: Okay.
Patrik: The nurse you were talking to, was that the bedside nurse?
Sharon: No, she was a doctor. She was a doctor.
Patrik: Oh, she was a doctor.
Sharon: The nurse was nice; the nurse was positive. It was the doctor that was negative.
Patrik: Okay. And what that doctor-
Sharon: And then the other doctor was like, “I can’t talk to you right now,” and very rude to us.
Patrik: Okay. Okay. Look, I don’t know whether you can recall yesterday when we had our first call. They will be negative throughout. No ICU will ever promise you that your mom, or any patient for that matter will survive their stay in ICU. Nobody’s going to promise you that for a number of reasons, including sort of the legal reasons. What if they told you from day one-
Sharon: So would they come right out and say it’s unlikely she’s going to survive? Because that’s what they just said.
Patrik: Say again, so they did say she does or she doesn’t survive? What did they say?
Sharon: They said she’s in going to get better, and they said, with this setback, it’s unlikely.
Patrik: Right. Right. And that’s the word they would be using all the way along. I can tell you. I’m talking to people all over the world every single day, and that’s the gist that most families get, right, that ICUs are very negative. So imagine a patient goes into ICU, and the doctors or the nurses are telling you, “Yeah. We do this, this and this, and in a few days your family member will be out of intensive care alive.” Now that could have legal implications for an ICU, because if it doesn’t happen, in theory, you could sue the hospital. You could sue even the individuals. Right?
Sharon: Right.
Patrik: So they’re almost advised on a professional level to be negative. Right?
Find out more information about ICU’s attitude towards patients:
Sharon: But this is like the most negative they’ve been.
Patrik: Yeah. Yeah. Look, I’m not surprised. I’m not surprised because they will be negative. They will be negative. But the doctors that you’ve spoken to, what’s their role in all of this? Are they ICU doctors?
Sharon: I literally have no idea. They don’t talk to us. We have to go search them down. I have no idea. The doctors we had in the beginning haven’t made an appearance once. I have no idea who these people are. I know they’re doing life-saving measures, but she just keeps getting worse in every different unit she goes to.
Patrik: Okay. I think what you need to ask for as well is you need to ask for a meeting with the treating team, which will be ICU as well as liver specialists. Right? They really need to sit down with you and say, “Look, this is the situation. This is what we’re doing. These are the next steps.” Right? I mean-
Sharon: But from what I can tell, they’re leaning towards us to get us to stop treatment.
Patrik: Say that again?
Sharon: I feel like they’re pushing us to get prepared to stop treatment.
Find more information about withdrawal of treatment:
Patrik: That will always be their positioning, because they want to stay in control of what’s happening. Right? It’s all about positioning. Right? I can’t tell you. I’m talking to people all over the world that are dealing with negative intensive care teams. And also, from a health professional perspective the things that doctors and nurses are dealing with in intensive care can be overwhelming. Right? Just like it’s overwhelming for you at the moment. Right? So it’s very important to read between the lines. I think the next step really is to hear from them what are they proposing. Are they wanting to put on a transplant list? It’s also unprofessional from them to make hints almost as they are passing by.
Sharon: Yeah, I agree.
Patrik: It’s very inappropriate. Very inappropriate.
Sharon: I agree. I agree. It was very inappropriate. Especially since this nurse that we had been talking to, she was so positive. We have a glimmer of hope and then this doctor just walked by and delivered this very news and this sad face on. I don’t even know what her name is. You know what I mean?
Recommended:
Patrik: Yeah. Yeah. And that’s why it’s so important you’re doing your own research. The number one complaint we are getting here is that ICUs are negative. Well, we know that for a fact. Right? And we know the reasons behind it. Right?
Sharon: Right.
Patrik: So whilst patients don’t survive intensive care, some patients, of course, we know that too. But no matter the outcome, they will be negative all the way along. And you need to-
Sharon: But that negative to the point where they’re implying that you’re never going to get better?
Patrik: Well, that’s what they want to imply to a degree because at the end of the day they want to keep their options open. And again, I can’t stress enough that they will never tell you that your mum will survive this because what I’d she doesn’t? Right?
Sharon: Right.
Patrik: That’s the reality. Right? And I also know for a fact that the pressure on ICU beds tends to be very big. So that means, again, their worst case scenario is that somebody is occupying an ICU bed for the next four, six or eight weeks, and they can’t use that bed for other patients who are critically ill. Right? So there’s a whole bigger picture to be looked at. Right?
Patrik: Your mother is certainly very ill. There’s no dispute around that. But unless they have sat down with you and your dad and really talked about the finer detail, right… I mean, you’ve now got a series of questions that you can ask. Unless they’ve talked-
Sharon: I mean; they’ve told us about the blood clots. They said that they gave her the platelets. They put it in her groin Something in her groin. They said they’re having a lot of trouble with the line because of the clotting. Does that make sense to you?
Patrik: Not really, because if the… okay.
Sharon: Or because of the bleeding?
Patrik: Yeah.
Sharon: Because of the bleeding, maybe.
Patrik: Oh, I see. She might be bleeding from the groin. She might be bleeding from the groin. That could be-
Sharon: No, I don’t think from the groin. I don’t think from the groin. But they keep changing her line because she’s… I don’t know, because of the bleeding or whatever happens.
Recommended:
Patrik: Right, so they keep changing-
Sharon: But there’s has been a lot of trouble with her lines.
Patrik: Probably because of the bleeding. Okay. Well, it does make sense. And they need to keep giving her probably the platelets, that she stops bleeding. But then again, at this point in time they’re not giving you the details really, are they? As they’re passing by they’re throwing some stuff without giving you the details in front of you. Again, it’s inappropriate. They need to sit down with you and explain things in detail. Now, what’s your feeling in this place? Are they very busy?
Sharon: Yeah. That’s what the doctor said. “I can’t talk to you now.” I mean, not for like hours. That’s how she spoke to us. And my mother is lying there dying, so I don’t really appreciate being spoken to that way.
Patrik: No. No, no. Look, again, your mother is very sick. I’ll just give you some examples. We’ve worked with some clients, right, they are in similar situations. Right? And they get told their loved one is dying and blah, blah, blah, and at the end of the day as long as they keep doing things, and as long as they keep doing things that are in the best interest of your mother, there is a chance that patients still recover. Right? Again, I can’t stress enough, the negativity is going to be the number one challenge that you have to… I’m not saying you should ignore it, but you can’t be bogged down by it. You can’t, because that’s going to be an ongoing recurring theme, the negativity.
Recommended:
Sharon: Like they’ll use the word unlikely a lot? Like unlikely recovery?
Patrik: Oh, they probably will be using that all the way along. Again, what you are describing here is nothing unusual in ICU. I know it’s overwhelming. I know it’s an absolute nightmare for you. But everything you’ve seen so far happens in ICU.
Sharon: But even this big setback issue was it?
Patrik: Oh, absolutely. Absolutely.
Sharon: With the blood clotting thing?
Patrik: Oh, absolutely.
Sharon: Okay.
Patrik: Absolutely. You’re dealing with a critical illness. Right? Well, everything so far is… that’s intensive care.
Sharon: So do I just tell them to keep not giving up? What do I say?
Patrik: AS long as there is no paperwork, or no documentation, or no meetings around giving up, they have no choice but to keep treating because you and your dad, as the surrogate decision makers, you will have a say. Your mum doesn’t have an advanced care plan? She didn’t, six months ago or a year ago, put a plan together in case a situation like this ever comes up?
Sharon: No.
Patrik: No. Right. So that means you and your dad are automatically the surrogate decision makers. Right? So the only-
Sharon: So if they say like… yeah.
Patrik: Go on.
Sharon: I’m sorry. Go on.
Patrik: The only thing that-
Sharon: So they like if they say… No, you tell me. Go fine.
Patrik: No, no, no, no, no, no. No, no. I think I know what you’re going to say next. Say it. Say it. It’s important.
Sharon: Okay. So say… No. You go.
Patrik: The only thing that could potentially happen that could potentially put a stop to all of this is if your mother suffers a cardiac arrest. Right? But as long as that’s not the case, they have to continue treating.
Sharon: Okay. Okay. All right. Yeah.
Patrik: But you were going to say something. You were going to say something. Tell me what you were going to say, because I think it’s important.
Sharon: I was going to say if they advise us to stop treatment, what do we do?
Patrik: Yeah. So there is a very good chance that they may say that. Okay?
Sharon: Right.
Patrik: Now, your positioning in all of this is… My understanding is that at this point in time neither you or your dad want to give up. Right?
Sharon: No, we don’t.
Patrik: Yeah. Yeah. And then you tell them.
Sharon: No, we won’t.
Patrik: And then you tell them.
Sharon: I just told her that, too.
Patrik: Yeah, of course. But it wasn’t a formal meeting. I think it’s really important that, again… If I was you, I wouldn’t engage in any sort of informal conversations at the bedside, because it’s very inappropriate. If I was you, I would just ask for a formal meeting with the treating team. That’s what I would do if I was you. Stay away from any sort of informal communication at the bedside, because it’s very inappropriate to have those conversations in front of your mother.
Find out more information and recommendations about family meeting:
Sharon: I agree. I agree.
Patrik: Tell them.
Sharon: You’re right. You’re right.
Patrik: You should tell them that. Don’t be afraid.
Sharon: I mean I will say that next time.
Patrik: Yeah. Yeah. Be very-
Sharon: I mean, I can go back and say that now, and say that I was very disappointed with the way that news was delivered to us.
Patrik: Absolutely. Absolutely. I think you should. The worst thing you can do is be intimidated by them. That’s the worst thing you can do. Don’t be intimidated by them. Again, I know it’s easier said than done. Be calm, be firm, and be concise in your communication. Don’t go overboard. Just state what you want. Just state what you want.
Related article:
Sharon: All right. Thank you. I’m going to go back in there now before we leave.
Patrik: Sure. Sure.
Sharon: Okay. I will let you know.
Patrik: Sure.
Sharon: Okay. Thank you.
Patrik: You’re most welcome.
Sharon: Bye.
Patrik: Bye-bye.
“This will be the last part for this series, thank you very much for being a part of 1:1 consulting and advocacy sessions. We hope you will find these new upcoming episodes informative and empowering.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!