Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is new episode series of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last week’s question by clicking on the link here.
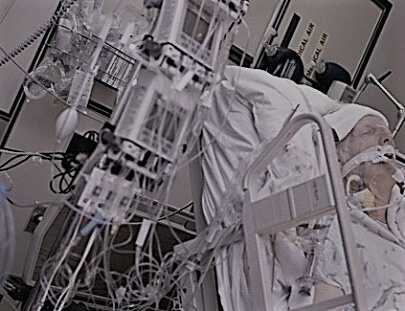
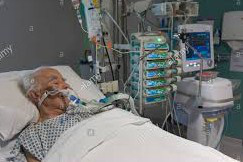
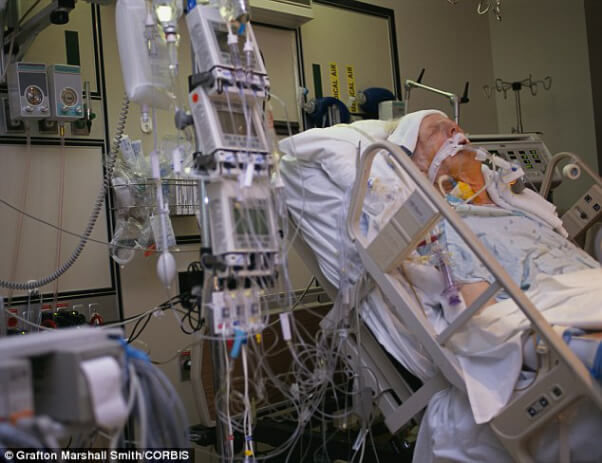
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Sharon who has her 64 year old mother transferred in the Intensive Care due to severe difficulty in breathing and alteration in mental state. Ultimately, her mother was diagnosed with liver failure and is on blood pressure medications and may subjected to dialysis due to renal failure.
The ICU doctors told me that my mom’s condition is getting worse. How should I respond to this?
You can also check out previous 1:1 consulting and advocacy sessions with me and Sharon here.
Hi Patrik,
We head for a family meeting tomorrow. They said because she is simultaneously clotting and bleeding it’s hard to keep in IVs and the kidneys and liver seem to be declining. Because of her current state she is not currently a candidate for transplant. I just don’t know how she can get better without a new liver. They said the liver is doing something right now just not enough. Also kidneys are failing
Sharon
Recommended resource for family meetings in Intensive Care:
Hi Sharon,
I think meeting makes a lot of sense.
Again, do not get bogged down by their negativity.
Yes, the liver and kidneys are not good I understand. Let’s wait for the next 24 hours. Take one day and even one hour at the time. Do not jump to conclusions and wait.
I would be very happy being on the phone during the meeting. What time do you have the meeting?
Kind Regards
Patrik
Related article/video:
Hi Patrik,
It’s 1pm here in New York Time tomorrow. Do I dial you in?
Also do you know what this blood thing is called?
They called it a disease simultaneous bleeding and clotting it was an acronym.
Ok so really it’s this horrible blood problem.
Something that her blood is clotting and bleeding at same time.
Sharon
Hi Sharon,
I can dial in via your cell.
I call you and you can put me on speaker or just let me listen, depending on what you want.
We will need to talk about the meeting beforehand. You need to know what to expect.
Let me know when is a good time to call you. I think the closer we can talk to the meeting the better because of the things that are already happening as we speak.
Also, at the moment you can’t control what’s happening to your mother. I still believe that at this point they are doing everything they can.
What you have 100% control over is how you react to the things that are currently happening.
Disseminated intravascular coagulation (DIC) is the disease you are referring to.
Kind Regards
Patrik
Relate article/video:
Hi Patrik,
They just told us they are starting dialysis tomorrow again.
Sharon
Hi Sharon,
Why are they not starting the Dialysis today? Do you know?
Kind Regards
Patrik
Read more information about haemodialysis/hemofiltration:
Hi Patrik,
I don’t know, my dad spoke to them, they said first thing tomorrow am. Could that help with the blood problem?
Sharon
Hi Sharon,
Dialysis or Hemofiltration is mainly helping with kidneys and keeping fluids off.
Could help mainly with ventilation not so much with blood clotting.
Ask what the kidney markers in the blood are doing. They are called Urea and Creatinine
Kind Regards
Patrik
Recommended:
Hi Patrik,
How long do the platelets start to work?
The blood results are still the same apparently.
She just had a pool of Platelets.
What do you think?
They also lowered the blood pressure medicine is that good?
Could it relate to the clotting?
Sharon
Hi Sharon,
Platelets should work within a few hours and her Platelet count should increase in the blood results.
It is absolutely good that blood pressure medications (Inotropes/Vasopressors) have been reduced yes.
Very unlikely that the inotropes/vasopressors relate to clotting, but you couldn’t rule it out either of course.
It means your mother is having an improved blood pressure naturally.
It’s most likely a result of giving fluids as well as lowering the sedation.
It could also be a result of no Hemofiltration/no Dialysis for the last 24 hours.
Generally speaking, if Patients in ICU are on Vasopressors/Inotropes like Norepinephrine they are either
- Having a severe infection/sepsis
- Hypovolemic (severe loss in blood volume) or dehydrated (severe loss in body fluid)
- in an induced coma with lots of sedation and pain killers which lowers blood pressure
There’s a very good chance the Norepinephrine will go up and down over the next few days.
After Dialysis is being recommenced and fluids removed there’s a good chance the norepinephrine will go up again.
Therefore, I’m not putting too much weight on it either way.
Kind Regards
Patrik
Recommended and more information about sedation and coma:
Hi Patrik,
I don’t think they started any dialysis.
What else is left to do if she has this clotting issue how does she get her blood and IVs.
Sharon
Hi Sharon,
At the moment all they can do is try and correct the clotting with medications such as Heparin. I don’t know if that’s an option with the liver failing. You should ask if they are considering giving Heparin for the clotting.
If that’s not an option, they may try and insert new lines.
It’s good to know that your Mom has opened her eyes and that you think she can hear you.
Take one day at the time, stay positive and try and get some rest.
You can’t run yourself to the ground. Your Mom and your family will need you at your best, one way or another.
Kind Regard
Patrik
Hi Patrik,
No real change at present, the clotting still an issue I just don’t know why they can’t try and fix it.
They are going to start to ween her off the blood pressure medicine (Inotropes and Vasopressors) and try to wake her up a bit because she’s been opening her eyes more. Still clotting but they are not feeling dialysis is as urgent.
Haemoglobin is now 7.
Sharon
Hi Sharon,
Sorry for the delayed response Sharon.
Have they started the Dialysis?
With a Hemoglobin of 7 are they planning to give red blood cells which is a blood transfusion?
That’s great that they are trying to wean her off the blood pressure medicine.
As I mentioned yesterday, it’s most likely a sign that they are getting her out of the induced coma and weaning her off sedatives!
I do believe that when they start Dialysis they may need to increase or restart the Norepinephrine again.
For now, this is great news, because the blood pressure medicine is considered major life support, just like ventilation is considered major life support.
That means with Dialysis off, Norepinephrine reduced she is slowly being weaned off life support.
Yes, clotting still an issue, but for now this is way more encouraging than 24 hours ago!
Focus on the positives!
Clotting will be hard to fix, as the liver is doing its own thing, but there are positives from what you have shared!
Kind Regards
Patrik
Hi Sharon,
Keep asking for blood results, kidney function like Urea and Creatinine in particular as well as LFT’s (Liver Function Tests)
Haemoglobin of 70 is low-ish therefore blood transfusions of red blood cells might be a consideration.
Is your mom more awake? Is she trying to wake up?
Also, how far away is she getting off the ventilator? Can you send me a picture with the ventilator settings?
From what you have shared, things are getting better and not worse.
Don’t know why they are not starting Dialysis; the kidneys must get better if they are not using it or have they not started it because of the clotting issue?
Kind Regards
Patrik
Recommended:
Hi Patrik,
No they said if it goes below 7
No dialysis said they don’t feel it’s as urgent and can’t do it with clotting
They said she was opening her eyes more and did it again this am when I asked.
The ventilator is still at 40. I’ll take a pic of everything tomorrow.
They are not starting because of the clotting but also said she is producing a little urine.
My question remains, how can the clotting resolve? She’s also bleeding a lot from her mouth which is scary.
Sharon
Hi Sharon,
Ok, the clotting is probably not going to resolve without the liver improving.
It’s good to hear that she’s making some urine.
There have been more positives than negatives in the last 24 hours!
Focus on the positives and not on the negatives!
2 steps forward one step back. Brace yourself for some setbacks as well!
Their predictions have been false to this point, if they had come true your mom wouldn’t be here now!
Focus on the positives!
Kind Regards
Patrik
Hi Patrik,
We haven’t gotten any new news since last night where everything is the same. I’m personally having a very rough morning. But most mornings are for me.
They told us again, that there is no hope and she’s going to die.
They said because nothing is getting better she won’t make it
Sharon
Recommended article:
Hi Sharon,
All Vital signs look normal and ventilator is doing all the breathing.
Ask them about sedation and pain killers and what medications she’s getting for that?
Kind Regards
Patrik
Thank you very much for being a part of the previous series of 1:1 consulting and advocacy sessions. We hope you will find these new upcoming episodes informative and empowering.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!