Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Emma, which are excerpts from 1:1 phone and email counselling and consulting sessions with me and the question this week is
My sister is in ICU on a balloon pump and ventilated after cardiac surgery! The ICU doctors want to stop treatment against our wishes and let her die, what should we do? (PART 7)
You can also access PART1, PART2, PART 3, PART 4, PART 5 and PART 6 by clicking on the links
Hello Patrik,
they have now placed my sister on what they call a lighter sedation overnight the nurse says her MAP dropped to 40’s so they had to increase the vasopressin to 0.08 and the Norepinephrine to 8 they had to just filter on the CRRT and not pull I am not sure what that mean. The nurse said that they tried to do a spontaneous extubation but my sister kept breathing over the machine and they did not continue. The nurse they changed the vent to ASV settings.
The nurse say’s that they are filtering her blood with the CRRT and now at the moment had to stop pulling fluids because her blood pressure dropped.
Many thanks
Emma
Hi Emma,
Thank you for the update and thank you for the pictures.
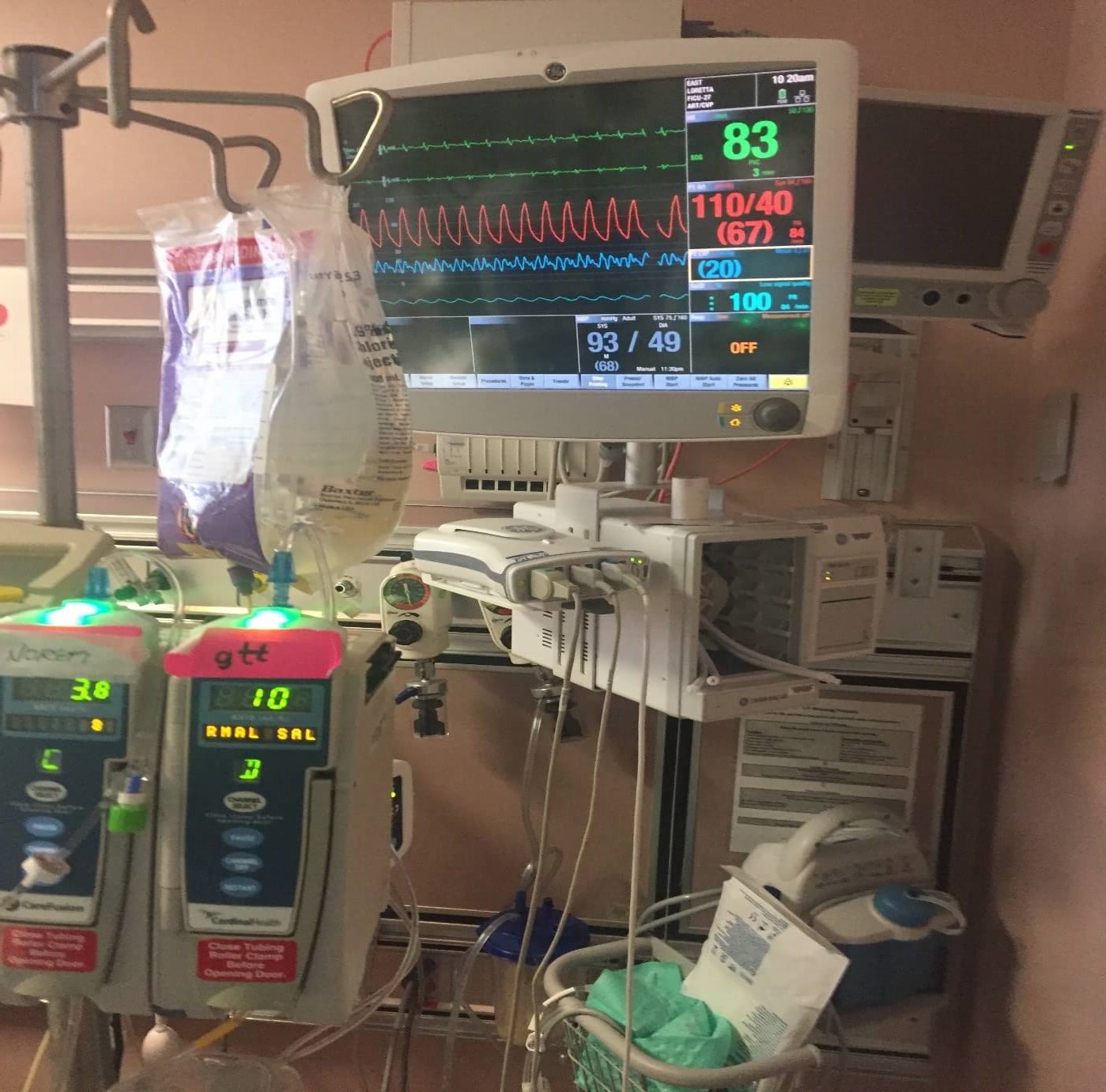
If you could send a picture of the bedside monitor that would be great as well.
I will give you a call in the next couple of hours.
For now, know the following.
If the MAP(=Mean arterial pressure) dropped, they have done the right thing by increasing the inotropes/vasopressors such as vasopressin and Norepinephrine.
The MAP dropping could be a result of a combination of things such as
- The heart not getting stronger
- Aggressive fluid removal via CRRT/Dialysis machine which is what the nurse suggested
- Infection/sepsis
If they tried spontaneous ventilation and your sister didn’t like it, there is a good chance she’s not quite ready for removal of the breathing tube/extubation yet.
I will give you a call shortly.
Hi Emma,
just quickly summarizing our phone call from last night
- Good news that they changed sedation from Propofol and Fentanyl to Dexmedetomidine(Precedex). It’ll help your sister “wake up” and then also breathe up. There is no guarantee that the Dexmedetomidine (Precedex) is going to work but it looks like she had a good day yesterday and it’s definitely worth a try. I have seen Dexmedetomidine(Precedex) being ineffective in many Patients, but it’s too early to see if it’s effective or not. We will reassess as we go along.
- With the inotropes/vasopressors such as Norepinephrine and Vasopressin going up and down I’m not too concerned at this stage. Your sister’s heart is weak and she’s in chronic kidney failure, hence the need to remove fluids aggressively is obvious and that will lower her blood pressure. Furthermore, removing fluids is also necessary to offload fluids for a weak heart. The “more dry” your sister is clinically, the easier it is for the heart to pump blood around the body because of less fluids in the system. Therefore blood pressure will go down, hence the need to increase Norepinephrine and Vasopressin. The “more dry” your sister is clinically by removing fluids via CRRT/Dialysis, the more fluids will be kept off her lungs and the easier she should be able to breathe, that’s what they are trying to achieve. No big deal at this stage from an Intensive Care perspective. The Dobutamine will be more important to watch for a decrease in rate because Dobutamine is improving the pump function of the heart. They will see in the next Ultrasound/echocardiogram of the heart if her contractility(=pump function of the heart) has improved or not. They will also have a new estimate of her ejection fraction(EF) after the Ultrasound/Echocardiogram of the heart. If EF has improved, they will most likely lower the Dobutamine which will be a good sign
- Furthermore, what’s also important to know is that aggressively removing fluids will keep her lungs dry which is very important to get her off the ventilator. Not removing fluids aggressively would put strain on the heart to pump blood around the body and would also cause fluids to be pushed into the lungs making it more difficult for your sister to breathe. Therefore keeping your sister “dry” by aggressively removing fluids will help her heart to recover and will support her to come off the ventilator. Again staying clinically “dry” will lower her blood pressure and the Norepinephrine and Vasopressin take care of that for now and that’ll be OK for a few days
- According to the pictures of the ventilator you have sent through, she should be close to be coming off the ventilator if she continues to improve and if she continues to breathe spontaneously and if she keeps “waking up”. Her Volumes are a little low with ~276 mls/breath but hopefully that’ll improve with chest Physiotherapy(I think you mentioned that they are starting chest Physio). This is going to be important going forward. Please also have a look at this article/video here
- I’m glad they mentioned tracheostomy as a next step if she can’t be extubated, but it’s too early to discuss in detail, we’ll talk about it if she can’t be extubated. Furthermore, talking about a tracheostomy is again a very different discussion compared to withdrawing treatment! It shows that they have plans moving forward beyond withdrawing treatment and it again shows that our strategy works for now and they are trying to do whatever they can to keep your sister alive
- Again, please keep in mind that they have taken her off the Balloon pump(IABP) and their predictions of her not surviving off the balloon have not come true. Another positive sign. Keep looking at the positives, your sister has gone a long way!
Recommended:
- Keep engaging the doctors and nurses, especially if they are more positive. Try and make friends if you can, we will keep looking at their actions not their words!
I hope that helps for now, make sure you get enough sleep, water and do some good things for you, keep pacing yourself and if you need a rest, take a rest, you are the most important person in all of this!
If you need to take a day off and you want me to talk to another family member instead, I’m very happy to do this, it’s all part of the 7 day unlimited 1:1 consulting and advocacy package which you purchased!
That’s it for now, stay positive, give yourself a pad on your back for being so strong and proactive and I’ll talk to you soon!
Take care
Kind Regards
Patrik
Thank you Patrik,
Okay thank you, the nurses say my sister’s vital signs are looking better than before she is still on the drips Dobutamine 5, vasopressin 0.04 and Norepinephrine 4, the ventilator setting is on spontaneous and the Respiratory therapist person says that my sister is doing good on the vent and they are expecting to extubate her soon. My sister is alert and is responding appropriately. As you say take it 24 hours at a time, we are thankful to God for each day. The nurse said that my sister is making slow and steady progress. I was just waiting to see what directions the doctors are going in concerning her plan of care before I contacted you to see what direction I needed to take. Just praying that they will change their minds and perform her needed surgery.
Emma
Hi Emma,
Overall from what I can see your sister is taking small but steady steps forward.
If she’s now spontaneously breathing, hopefully she can come off the ventilator in the next 24 hours, it would be a huge achievement.
It sounds like all they need to be able to achieve is to reduce the pressure support on the ventilator from 12 down to 8. Most Patients in Intensive Care can be extubated on spontaneous ventilation mode, Pressure support<10 and less than 40% of oxygen.
Patients also need to be off sedation and she is now off it from what you’ve explained.
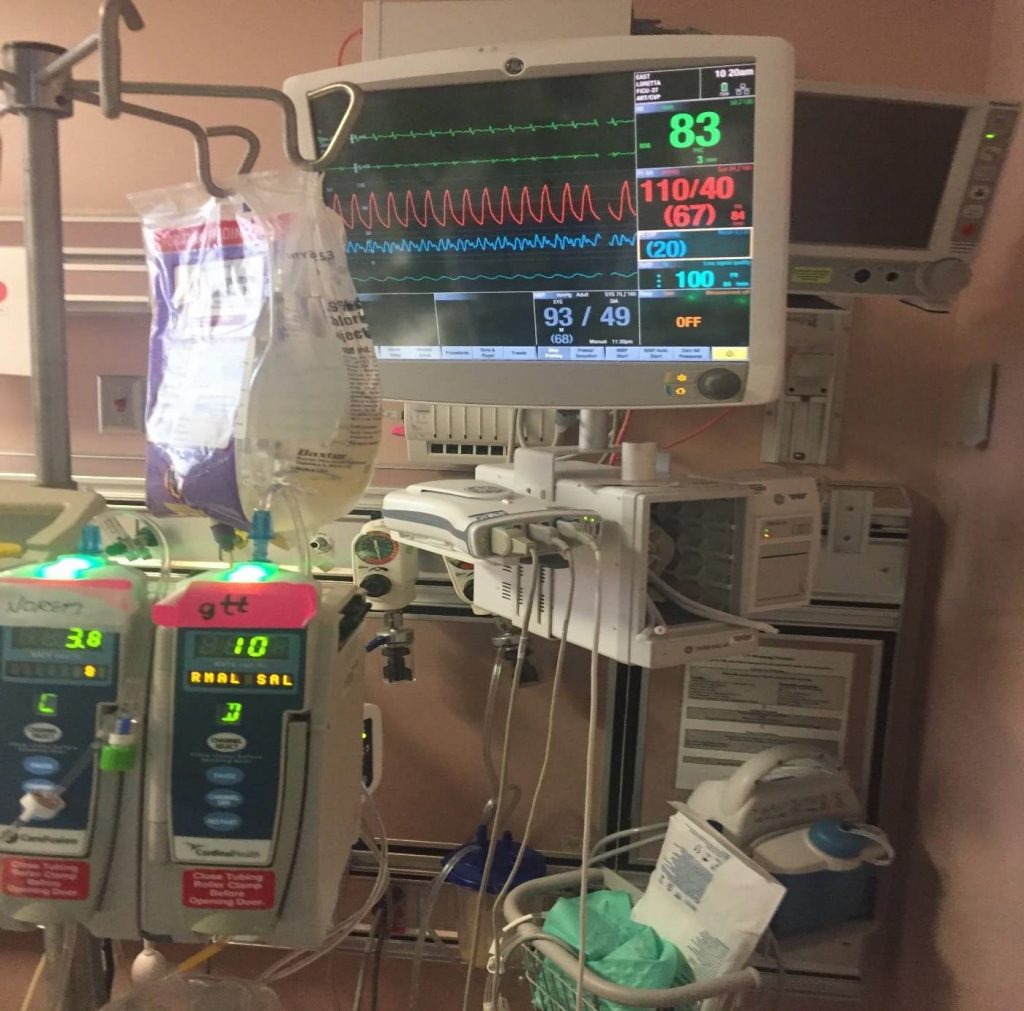
You can also ask for arterial blood gas results. On the last picture you sent with her monitor I could see that they are measuring her arterial blood gases.
In the last picture you had sent from the ventilator she was on 40% of oxygen, hopefully that’s either still the same or has come down even.
In terms of the inotropes/vasopressors like the vasopressin, Norepinephrine and the Dobutamine for now she still needs them as the heart is still relatively weak and her challenge with the weak heart continues to keep fluids out of the lungs which could be detrimental to getting her extubated. That and the ongoing CRRT on the dialysis machine will keep the lungs clear of fluids.
The first inotrope/vasopressor that needs to be reduced is the vasopressin, then the Norepinephrine and then the Dobutamine. Often when Patients come off the ventilator their inotrope/vasopressor requirements do go down, therefore the next step really is to get your sister extubated.
I hope that helps for now, still take it one day at the time, the goal for now is to get your sister off the ventilator.
It’s been great working with you and I would love to continue helping you with your and your sister’s situation.
Any questions please let me know.
Kind Regards
Patrik
Recommended:
Hi Patrik,
Just spoke with the nurse they had to add another blood pressure medication(Inotropes/vasopressors) called epinephrine increased the vasopressin to 6, the dobutamine possibly still the same and they gave her a unit of blood to add volume the nurse says they held her dialysis for now because her blood pressure had dropped so low. The nurse said something about patients wax and wane like that
Not sure what all this means.
Please advise.
Emma
Hi Emma,
Thanks for your email.
From the information that you have shared, I would think that they have been aggressively removing fluids with the CRRT/Dialysis so that
- Your sister stays “dry” to keep fluids off the lungs so that she can be extubated
- On the other hand, removing fluids aggressively will drop blood pressure, hence the need to go in with another inotrope/vasopressor like Epinephrine(“Epi”)
- Using another vasopressor/inotrope like Epinephrine could be a sign of being too “dry” because of aggressive fluid removal or it could mean that the heart is too weak. But it could also mean that they have added it in to wean off the Vasopressin
- Another unit of blood should also help to wean the vasopressin, your sister’s Haemoglobin(=red blood cells) is probably too low
- Here is the order in which they should remove the inotropes/vasopressors 1) Vasopressin 2) Epinephrine 3) Norepinephrine 4)Dobutamine
- Find out if they think they started the Epinephrine because your sister is too “dry” because of aggressive fluid removal via CRRT/Dialysis, if they think the heart is too weak or if they want to replace the Vasopressin with Epinephrine
- It would also be good if you can send another picture of the ventilator and the monitor
- It would also be good if you could get some blood results like Haemoglobin, white cell count, Troponin and arterial blood gas results
I hope it’s not too confusing, very happy to explain over the phone I just left a message on your voicemail.
Are they still trying to take her off the ventilator today?
Kind Regards
Patrik
Look out for PART 7 of the 1:1 counselling, consulting and advocacy session with Emma in the next few days!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!