Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Emma, which are excerpts from 1:1 phone and email counselling and consulting sessions with me and the question this week is
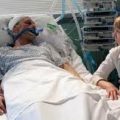
My sister is in ICU on a balloon pump and ventilated after cardiac surgery! The ICU doctors want to stop treatment against our wishes and let her die, what should we do? (PART 6)
You can also access PART1, PART2, PART 3, PART 4 and PART 5 by clicking on the links
In today’s 1:1 consulting and advocacy session Emma and I continue to discuss how Emma can help her sister to get out of Intensive Care alive and how she needs to continuously challenge the Intensive Care team to keep doing the right things.
Patrik: Hi Emma, it’s Patrik speaking from Intensive Care Hotline. How are you?
Emma: I’m okay. How are you?
Patrik: I’m really good thank you. Is this a good time?
Emma: Oh yes, it is.
Patrik: Right. Okay. So look, again, you know, there’s from your emails there is small but steady progress. Right?
Emma: Okay.
Patrik : So if they are weaning down the Dobutamine and the Vasopressin and Norepinephrine that’s good. Okay, if they are weaning the Fentanyl and the Propofol that’s good. If they are increasing the tube feeds that’s good. Ejection fraction 50 to 54, that’s okay but keep in mind, excuse me, the goal is to get that ejection fraction to that 50 or 54 percent without the vasopressors/inotropes. Right? That’s going to be the challenge. To get those vasopressors/inotropes off while maintaining the ejection fraction. And that’s what they mean when they say that her heart is weak. Okay?
Emma: Okay.
Patrik: So the vasopressors/inotropes support the heart, that’s what they do. Okay?
Emma: Okay.
Patrik: And by weaning them down they need to make sure that the ejection fraction stays the same or even improve. Okay?
Emma: Okay.
Patrik: So basically what ejection fraction(EF) means, when the heart contracts, the heart contracts to pump blood through the body. That’s the purpose or the function of the heart. Okay? So with a poor ejection fraction it means pumping the blood is diminished. Right?
Emma: Right.
Patrik: So there is less blood ejected, which is where the term “ejection fraction” comes from.
Emma: Okay.
Patrik: Okay?
Emma: Okay.
Patrik: So the Dobutamine in particular is increasing the compressions of the heart, that’s what the Dobutamine is doing in particular. And the noradrenaline, the Norepinephrine and the Vasopressin are more to constrict the veins and the arteries to get the blood closer to the heart. I don’t want to get to technical here but that’s basically what all of those things are doing. But it’s a good good sign that they’re weaning it down. It’s a good sign that-
Emma: Would the, I’m sorry, would the Vasopressin, she said it was at pump four so that’s the highest, the more issues they have they, it looked like they go from like, she was on eight then they took her down to five. She was on four and that’s it. But it looked like she was on five one day, looks like they’re trying to take it down. Is that normal for them to go like from five to four?
Patrik: Oh yeah. Oh yeah.
Emma: And back up to five.
Patrik: Yep. Yep.
Emma: Okay.
Patrik: Very normal. Very normal. And now I, so I also like that they’re saying that they want to take her off the ventilator in the next few days. I like that. Right?
Emma: Mm-hmm (affirmative).
Patrik: I mean again, excuse me, that’s a very different conversation to have compared to saying we’re going to stop treatment.
Emma: Okay.
Patrik: You know. I mean that’s a very different conversation to have. What we need to look for though is that, so are you saying that at the moment she’s awake? Would you say she’s awake?
Emma: She’s awake.
Patrik: Okay and she’s recognising you, you think?
Emma: She is.
Patrik: Right. Right. Okay that’s good. Is she, when you or the nurses ask her to obey commands, when you ask her to squeeze her fingers, to squeeze your fingers is she doing that?
Emma: She seems to be weak when it comes to that but if I ask her like, I asked her, I say, “Well do you want me to take off from work and come up here tomorrow?” She nodded her head yes. I told her I said, “I love … Do you love … ?” She said yes. And stuff like that or even if it’s a no, she’ll shake her head no. And when I ask her to open her eyes, she opens her eyes.
Patrik: And that’s all appropriate.
Emma: Okay.
Patrik: Yeah. No no that’s good. That’s good. That’s all good. So I like that you’re keeping it brief with the doctors, because you know you’ve said everything you had to say. You’ve made your point very clear. Right?
Emma: Right.
Patrik: And the only thing, the only thing that I would be looking out for if I was you is, so if they want to take her off the ventilator, right? It would be good if she’s ready for that, okay?
Emma: Okay.
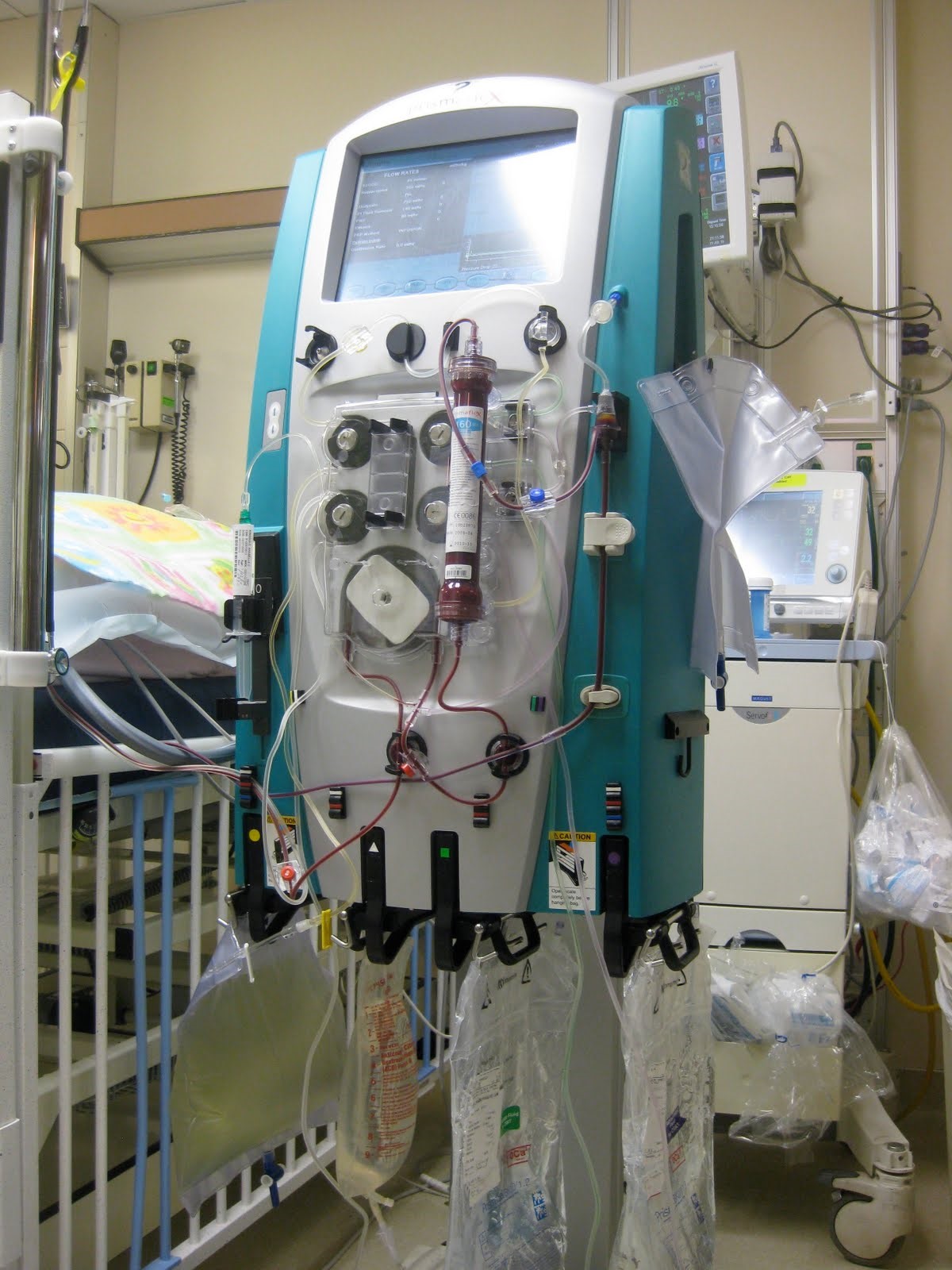
Patrik: Maybe when you’re there next can you, do you think you’d be able to take a picture of the ventilator?
Emma: Oh yes I will. I’ll take a picture of it.
Patrik: Can you do that? And send me the picture in an email?
Emma: Okay I will.
Patrik: That’s number one. The next thing is, can you also take a picture of the monitor? There would be a monitor.
Emma: Which monitor would I take a picture of?
Patrik: Okay so there would be a monitor where you can see her heart rate, her oxygen levels, there would be a monitor.
Emma: Oh yeah, I’ve seen that.
Patrik: Yeah. Can you take a picture of that as well?
Emma: Okay.
Patrik: The only question you probably need to ask them is the following. So it sounds like your sister is coming a lot closer to getting off the ventilator, right? And you need to ask them for plan B. What do I mean by that? Plan B is if she comes off the ventilator, and she can’t breathe by herself what will they do? That’s the question you need to ask. Right?
Emma: Okay.
Patrik: Because there is a, how long has your sister been on the ventilator in total? Do you remember?
Emma: Today makes a week. She had the surgery, she had that surgery last Tuesday and they gave her two days to live, so she’s been on the ventilator for a week.
Patrik: For a week. Okay that’s not, that’s pretty good. So but basically, definitely ask them what are their plans if she fails. You know? They would have to put her back on the ventilator. But I would also like to hear from them, you know, what are their plans, right? I mean at this stage she is for full treatment right?
Emma: Right.
Patrik: And in that respect if she fails coming off the breathing tube, they need to put her back on it.
Emma: Okay.
Patrik: But I would still, I would bring that up as a point of discussion, from your end, to get their response. To get their response, I think that’s going to be really important to get their response about, you know, what are they going to say. And you know, I would also like, that’s why I want to see a picture of the ventilator. So see what’s she up to, how realistic is it, you know they are telling you she might come off the ventilator soon but I do want to know that this is realistic they’re talking. You know, that what they’re talking about.
Because you, I look at the ventilator and I know what it means, right? And I can guide you from there.
Emma: Okay.
Patrik: But look, overall that what you are describing there is progress. Baby steps, baby steps but steps.
Emma: Okay.
Patrik: Right? And I like that she’s acknowledging you I like that she’s nodding head or shaking head, you know that’s all good. That means the brain is intact. The brain is intact. And anymore talk, anymore talk about withdrawing treatment?
Emma: No we’re not talking to me, they’re not talking to me at all and the manager of the unit is going out of her way too. She keeps coming to my sister’s room asking me, “Do you need anything? What, you have any questions?” But the other, some of the other families out there, you know, I talked to them, they said she’s not doing that. But they haven’t said anything about withdrawing treatment, they haven’t said anything about … surgery. They haven’t, we’re just in limbo.
Recommended:
Patrik: Yeah okay. Yes yes you are in limbo but you know, by weaning, okay so the reality is if she can stay off the vasopressors/inotropes, right? That means her heart is recovering slowly. Right? It doesn’t mean that the heart can fully recover but there is a level of recovery happening already. Okay?
Emma: Okay.
Patrik: And I mean again, even look, even if they had withdrawn treatment a few days back she probably would have survived anyway, because you know, patients need time. Patients need time. You know?
Emma: Mm-hmm (affirmative).
Patrik: Recovery in intensive care is a marathon, it’s not a sprint. It can take a long time. And that’s the challenge. ICUs are not prepared to give people the time they need. That’s the challenge. So your job at this stage is still to buy time. So when you’re talking about the nurse manager, are you saying she wants to talk to you? Do you think it’s genuine? What’s your feeling, do you think her efforts are genuine?
Emma: No I don’t think it’s genuine. I do not think it’s genuine at all.
Patrik: Okay. Okay. Who, right, is she talking to your brother-in-law?
Emma: Well he hasn’t been there this week so far and when he does, he doesn’t trust her either. So he’ll go back and so. I been covering and he’ll go back next week to start covering. And if everything goes, you know, good. But the reality is that he doesn’t trust her either. So whenever she comes to him he’s always calling me.
Patrik: Okay. So her words do not, her words don’t match her actions really?
Emma: No she’s not genuine at all.
Patrik: Okay okay. What about the doctors?
Emma: The doctors are being like, during rounds I’m in the room so you know, they come through at two thirty, the visit starts at uh, the visit starts at two, so I’m in the room, so the nurse, mind you, got me out the room today and she told me that, she asked me if I had any questions. I said, “No” because I’m following your advice so, the doctor started talking and that’s when they tell me that he’s trying to get her off the vent. And that her heart is weak and then prior to that one of the doctors, maybe like last week, after everything, after they started getting her off the medications, they said they’re trying to strengthen her heart. And over the weekend I was in her room and there was a doctor, he said that he was her, he was her lung doctor, and he told me that she had made, she had did good and but then he said that like, he started telling me it was weird.
He started telling me that you know, well her kidneys are down, her heart, and now she’s on the lung, she’s on the breathing thing and then he said that she had something called bacteraemia? And so I told him I say, “Well you know” I say, “Call us crazy, but we’re praying and we’re believing that she’s gonna come out of here.” So the conversation changed. He told me, he said, “I don’t know why they didn’t do that surgery on her.” And I said, “Well one doctor wanted to do it, the other one didn’t.” He said, “Could be a number of things with the insurance.” And then he went to tell me that like with the, she got something called bacteraemia, he identified that and they’re treating her with the antibiotics. He told me that her lungs, on the chest x-rays, looked good. There was no pneumonia or anything and he told me that her creatine or something with her kidneys was in her norm. So I didn’t understand. At first he was talking negative and then he started saying that so I don’t understand what he was trying to say.
Patrik: Right. Your sister is a dialysis patient isn’t she?
Emma: Yes.
Patrik: Right.
Emma: Since 2009.
Patrik: Yeah. So they’ve been dialyzing her for the last few days have they?
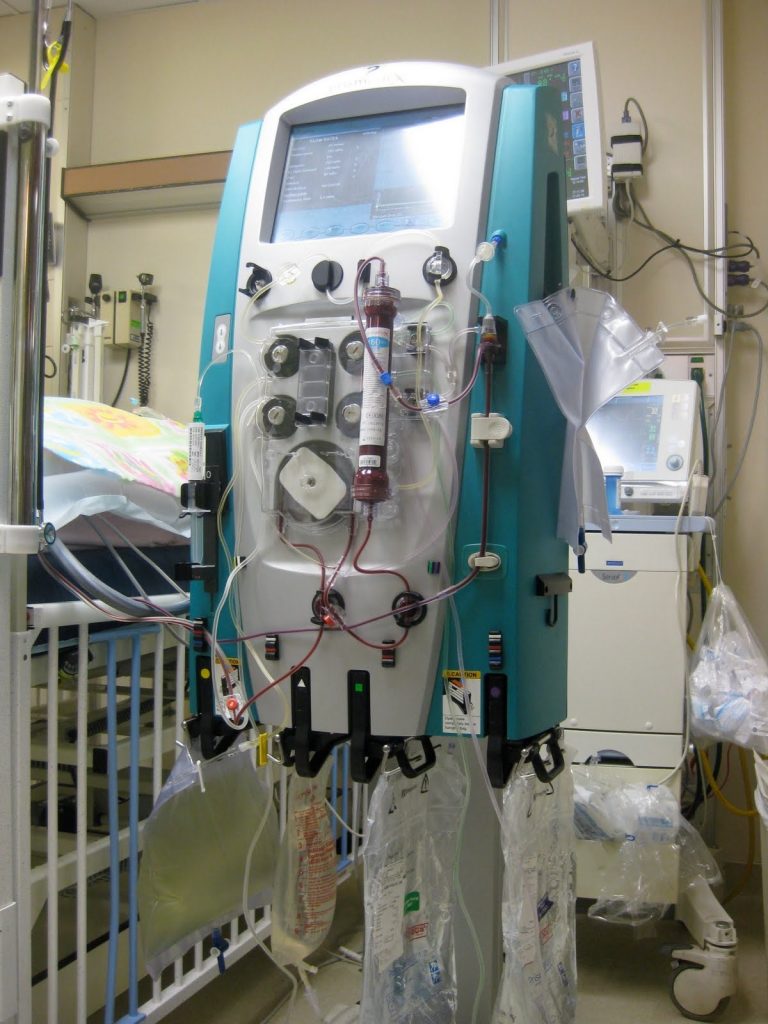
Emma: Yes. Well they doing something, they told me it was CRRT or something like that.
Patrik: Yeah yeah. CRRT, yeah. It stands for Continuous Renal replacement therapy. And how, is that continuous? Is she ever off that? What’s the situation there?
Emma: It’s continuous. We’re going to continue.
Related article/video:
Patrik: Okay. That’s fine. That’s fine. Look her creatine levels would probably vary but as long as they keep doing the CRRT I’m not really worried about it because that’s how they manage it. Okay so?
Emma: Okay.
Patrik: The priority, I’ll tell you what the priority is, the priority will be to get her off the ventilator, to get off the vasopressors(inotropes), that will be priority. So in order to move forward, as I said, send me the pictures of the ventilator and the monitor. And from there I can direct you what you exactly need to ask what their plan is to get her off the ventilator and the breathing tube/endotracheal tube.
Emma: Okay. Okay I’ll do that tomorrow when I go in I’ll take pictures and send them to you.
Patrik: Absolutely absolutely. Any, do you have any other questions at the moment?
Emma: Well I’m grateful to you and with me, I’m so anxious and I want to just run up there all the time. You know and, how can I manage my, what’s a good thing for me to do? Should I just trust them in her, I want somebody there at every visiting. Every visiting hour I want somebody to be there. And if I’m at work, you know, I don’t want them to look in there and not see any of us. How can I manage myself?
Patrik: Yeah. How can you manage yourself? Okay. So the best advice that I can give you is, and I know that’s easier said than done but probably keep the following in mind. Try and stay positive and that’s easier said than done but I’ll give you more insights there. So you know, by staying positive you’re creating positive vibes for yourself and also for your family and for your sister, so that’s one thing. And you know, we don’t have a crystal ball, we don’t know what’s going to happen but even in the event of a negative outcome, right?
Emma: Mm-hmm (affirmative).
Patrik: Staying positive is still better. Imagine you’re negative and then you’re having a negative outcome. But by staying positive and even if you have a negative outcome you will still feel better in the end. Right?
Emma: Mm-hmm (affirmative).
Patrik: And it helps to create positive vibes. Right? And look-
Emma: Right.
Patrik: On the weekend when you first contacted me, you know, all signs were your sister is dying. That’s at least what they told you. But they were adamant to withdraw treatment, “pull the plug” and all of that so at this stage do not look to far into the future. The goal is very clear. The goal is to get her off the vasopressors/inotropes, to get her off the ventilator. Those are the goals for now. Because if she can manage that, she will be alive. Okay?
Emma: Right.
Patrik: So just, we’re still at the point where, baby steps but steps.
Emma: Okay.
Patrik: Right?
Emma: Right.
Patrik: So the situation that you and your sister are in, you know, it’s, if you are, if you have worked in intensive care, those situations happen every day, right? But we also know that those situations are not resolved in a heartbeat. They are not resolved in a heartbeat, takes time. Right? So-
Emma: Right.
Patrik: So that’s the advice for now. And how can you manage yourself even better? Look, you’ve already had a big impact on them. They’re already treating you differently. Would you agree with that?
Emma: They are. They are.
Patrik: So look at the positives, they are already treating you differently, okay? There’s no more talk about withdrawal of treatment or “pulling the plug”, okay? So they know, they probably know that you’re talking to someone who has insights, right?
Emma: Mm-hmm (affirmative).
Patrik: And you know, know that you know that you are a powerful force, right? Know that for yourself. You have already, you know I mentioned earlier in the week I said to you, “You’ve got to turn this upside down” and you have. You have. They’re talking to you differently. Ignore the nurse manager, you know that she’s probably, you know that she’s not genuine, that’s all you need to know for now. She probably doesn’t like you. You know, that’s all you need to know, it’s nothing personal. They’re not used to people challenging them.
Emma: Okay.
Patrik: Right? So you can-
Emma: Right.
Patrik: You can ignore all of that, just all that matters is that your sister keeps making progress, that’s all that matters for now.
Emma: Okay. Okay.
Patrik: And how much time do you spend in hospital at the moment?
Emma: Oh a lot. I was, it’s pretty much every day, probably you know I just started coming home trying to sleep. So I go from the 10 o’clock visit in the morning to the last visit, which is from eight to 10. And then I’ll turn around and go back. I was spending the night up there but I started having nightmares. I can’t sleep at home either so. I go every day, cause I don’t want, I’m afraid that if I miss a visitation or if one of us is not in there then they won’t take care of her properly. You know, I don’t, does that make sense?
Patrik: It does. It does. Okay. Okay. Look, so being there for your sister is very important, Okay, there’s no doubt about that. However, you are more important than your sister and I don’t mean that, what I’m saying is if you don’t function, nothing will work. Because you are the most important person at the moment. Right? So I have-
Emma: Mm-hmm (affirmative).
Patrik: I have seen many families in intensive care burning out you know. Because they spend day and night in intensive care and it’s very stressful, you know. What I’m saying is the last thing that we want is for you to crash and burn. For you to become sick, you know? So if you feel like you need to take a day off, you need to take a day off. Right?
Emma: Okay.
Patrik: How far away from the hospital are you?
Emma: I’m about 45 minutes.
Patrik: So you are-
Emma: 45 minutes to a hour.
Patrik: Right, so it’s not around the corner?
Emma: No it’s not. It’s in Houston. And I’m in Texas City.
Patrik: I see. I see. So when, if you are not there are there any other family members there?
Emma: Well yes. Me and my siblings we just made a schedule. And her husband, he’s been there 24 seven so he’s taking the week off so me and my, two of my siblings are making a schedule out so that somebody will try to be at every visit.
Patrik: Yeah. And that’s good. And that’s good. But just like you said, your brother-in-law has taken time off because he spent 24 seven in the hospital. You don’t want to come to that point. You’ve got to pace, you’ve got to pace yourself. You need to pace yourself.
Emma: Okay.
Patrik: Okay? So be good to yourself. Be good to yourself, give yourself a pat on the shoulder for being so strong and turning it upside down. You can be proud of that. So you know you’ve got to look at the positives. You’ve changed the situation already, you’ve managed to buy your sister time. Right? So definitely look-
Emma: Right.
Patrik: … at the positives. That will make you more confident because you know you’ve gone from them talking about withdrawing treatment and not wanting to give you a choice, to them talking about-
Emma: Right.
Patrik: … to them talking about, okay, we will try and wean off the vasopressors and we will try and wean your sister off the ventilator. That’s a very different conversation to have. Very different conversation. And that all changed within 24 to 48 hours.
Recommended:
Emma: It did. It did.
Patrik: Right. So you need to know that you have some impact there. And when you’re walking in there show them with your body language that you’re not putting up with their crap. And you probably do that already, consciously or unconsciously. But your body language is very important, head up, shoulders out, look them in the eye, that’s very important. It’s subtle but it’s very important.
Emma: Okay.
Patrik: Very important. I look, I worked in ICU for 20 years, I can’t tell you how many families I’ve seen, you know? They walk into ICU, they’re crying and don’t get me wrong that’s all fair. But it doesn’t help anyone. Doesn’t help anyone. You can, you know I think emotions are a healthy sign, but you need to show those emotions at the right time. Show those emotions when it’s over. When you know which, at the moment you need to keep your composure. Show them with your voice, with your body language, with your eye contact, that you’re not taking any fools gladly. And you’ve shown that already. Most families in ICU are intimidated, 99 percent are intimidated by the doctors, by the nurses, you are not, you’ve already shown that. Continue on that path. Continue on that path.
Emma: Okay.
Patrik: Don’t take any prisoners, but at the same time look after yourself. You are the most important person at the moment.
Emma: Okay, okay.
Patrik: Okay. And once I have the, once I have the pictures then we will ask, I will get you, we will ask the next questions.
Emma: Okay. Okay. I’ll get that to you tomorrow.
Patrik: Sure. Sure. Okay? Does that help for now?
Emma: Yes. You have, you don’t know how much you have helped me. I mean I couldn’t have, I was, I am so dumbfound to this here and I would have never known if it would not be for your help and I’m so grateful. I am grateful.
Patrik: That’s what I do. That’s what I’m here for. That’s what I’m here for. So I’m very glad, very glad that it helps. And we’ll talk, we’ll talk tomorrow. Send me those pictures and then we’ll take the next step.
Emma: Okay, okay. Thank you so much.
Patrik: You are very welcome. Have a good rest. Have a good rest.
Emma: You too. Okay bye bye.
Patrik: Bye bye.
Look out for PART 7 of the 1:1 counselling, consulting and advocacy session with Emma in the next few days!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!