Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Emma, which are excerpts from 1:1 phone and email counselling and consulting sessions with me and the question this week is
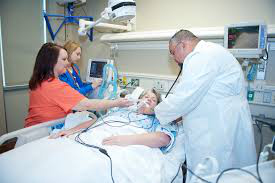
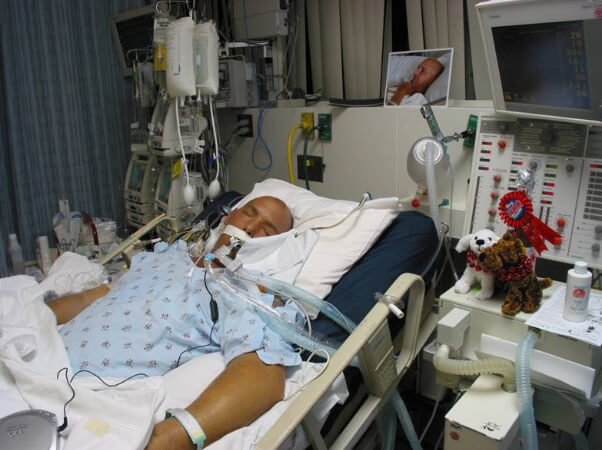
My sister is in ICU on a balloon pump and ventilated after cardiac surgery! The ICU doctors want to stop treatment against our wishes and let her die, what should we do? (PART 4)
You can also access PART1, PART2 and PART 3 by clicking on the links
In the last counselling and consulting session with Emma we were discussing how Emma can keep her sister alive on life support even though the ICU doctors were adamant to stop treatment, remove life support and let her sister die against her and her family’s wishes.
In today’s 1:1 phone consulting and advocacy session with me look into how Emma can further change the dynamics into her and her family’s favour, without feeling intimidated by the Intensive Care team. I’m going to share many gold nuggets in how to use simple strategies in order to get things her sister’s way.
Emma: It’s the cardiac surgeon and the ICU. Both. The doctors are sticking together, you know. And I see some discrepancies in what they’re saying because at times they told us that if my sister would work with physical therapy and start walking, then they would do the surgery and then the same doctor, he said that no, he never intended on doing the surgery at all because the ICU doctor, the head of the department came in and he … I explained to him. He was like, well they wasn’t going to that. They admit as team with her quality of life. So I’m like why would they move that … Because they purposely moved the pump from her groin area to her chest area so she could get up and start working this physical therapy so she can build up for the surgery.
But now they’re saying none of that is appropriate.
Patrik: Right. You know, as I said, just wait for now. Just give it another 24 hours.
Emma: Okay.
Patrik: And tomorrow, you know, when you’re at the bedside, give me a call. I will try and talk to the nurse and get more information and the more information we have then we can ask for a meeting on your terms. Not on their terms.
Emma: Okay.
Patrik: Because their terms, what they’re trying to do is, they’re trying to withdraw treatment. But I think if you do see them, either let, you won’t be seeing them tonight. For you it’s night time at the moment, isn’t it?
Emma: Yeah, it’s almost 9:00 pm
Patrik: Yeah, right, right. So from your end, when you see them next, do you … Who do you see when you see them? Is it the ICU consultant? Who do you see? Who do you speak to?
Emma: It’s the ICU doctor when they make rounds. It’s whatever doctor … I think they call them internists or something.
Patrik: Would be a junior doctor. Would it be a youngish person?
Emma: A youngish person?
Patrik: Yeah, that’s what I’m asking.
Emma: No he’s older.
Patrik: Oh okay. That’s okay. So they are experienced, you think?
Emma: Yeah, I think so. I can’t really tell because sometimes they act like … And it’s a mixture of age groups and stuff. The older ones I’ve seen, the really older ones are the head doctors.
Patrik: Okay.
Emma: And the nurses they act … Like when I ask the nurses questions, they act like they don’t know anything.
Patrik: Really. Okay. Okay. Well I would really like to talk to a nurse to begin with to find out what they know.
Okay and yeah, tomorrow let’s talk … I’ll tell you what the next stops are. Let’s wait, if she’s waking up tomorrow, or not, okay.
Emma: Okay.
Patrik: And then we can determine the next steps. And if tomorrow they can wean off the vasopressors/inotropes even more, that’s another good sign, right.
Emma: Okay.
Patrik: So let’s wait until tomorrow …
Emma: Okay.
Patrik: And see whether she’s waking up. See whether they’ve removed more of the vasopressors/inotropes and then we’ll determine the next steps.
Emma: Okay, okay, okay. Will do.
Patrik: Okay. Does that help?
Emma: It helps a lot. You’ve helped me a lot. I would have went in there just blind sided and I’m like, what you told me yesterday, that’s exactly what I did and I said and I seen their reaction, you know so I they’re scared.
Recommended:
Patrik: That’s good. Yeah. No, no, that’s good. That’s good. So and have a look at the law, the link I sent you. Definitely have a look at that.
Emma: Okay. Will do.
Patrik: I’ll wait to hear from you whenever you need me but probably the next best thing is when you are at the bedside, give me a call.
Emma: Okay, I will do that. Okay thank you so much.
Patrik: You’re very welcome. You’re very welcome. I appreciate it. Thank you. All the best for now.
Emma: Okay thank you bye-bye.
Patrik: Bye-bye
Hi Emma,
Further to our phone call here are some links to articles that clearly highlights that Physicians in Texas can not override the wishes of Patients and/or their families to withdraw life sustaining treatment!
http://medicalfutility.blogspot.com.au/2015/03/texas-advance-directives-act-2015.html
http://medicalfutility.blogspot.com.au/2017/02/simons-law-legislation-introduced-in.html
Use this information to your advantage and position your sister’s situation appropriately!
Kind Regards
Patrik
Hello Patrik,
I attempted to get the nurse to allow me to call you on today allowing you to speak with her the nurse stated for me to try later as she had to leave my sister bedside for some type of skills and that another nurse that was not as familiar with my sister care would cover for her for time she would be gone. I asked her if I could call and conference the call with you later in the day she seemed very hesitant. I am not sure what is going on it seems like the nurse manager and staff is uneasy with my presence. While I was visiting with my sister today ethics and the doctor rounded. They asked me if I had any questions I informed them that I was simply listen. The doctor made the statement that they are trying to strengthen my sisters heart and the nurse manager made the statement that my sister has been weaned down to only 3 blood pressure medications(inotropes/vasopressors) and that was a good thing. I just listened to each of them speak, I have requested to view my sister’s hospital record the manager of the unit said that upon signing the consent to release records that she would have to be present in order for me to view my sister’s record while she is in the hospital. Please can you tell me what is the role of ethics. They(ethics) keep asking me how I feel and I have explained to them that I am not happy with the care that my sister has received at the hospital !
Many thanks
Emma
Hi Emma,
Nice to talk to you a moment ago.
Quick summary of what we discussed
- Keep taking one day at the time and aim for getting your sister through the weekend
- Keep ignoring ethics (Is it ethical wanting to withdraw treatment against your and your family’s wishes???)
- Keep asking for copies of the medical records with a deadline
- Take it as a compliment that they feel uneasy in your presence, they are not used to being questioned and feel resistance
- Continue to focus in your communications with them only about what you want and expect, keep repeating whenever necessary
Questions going forward
- When did your sister last have an Ultrasound/Echocardiogram of the heart?
- What is her current ejection fraction(EF)?
- What blood pressure medications is she on? (commonly used blood pressure meds also known as inotropes or vasopressors are Norepinephrine, Epinephrine, Dobutamine, Dopamine, Vasopressin, Milrinone and Levosimendan)
- What sedation is your sister on currently that’s keeping her in the induced coma? It’s very likely your sister is either on Propofol(Diprivan) or on Midazolam(Versed) for sedation and on Morphine or Fentanyl for pain relief. If you can find out what medications she’s on it would help
I’m looking forward to hear from you!
Keep staying strong and stay positive!
Kind Regards
Patrik
Hello Patrik,
we are grateful to God that my sister is still alive today. She is still intubated the nurse says that the breathing machine is at 40 she is on dobutamine 5, vasopressin 0.04 and Norepinephrine 5 the nurse says that they are attempting to wean her from the Noriepinephrine she was on 8 yesterday and earlier today 5 and last I heard they had weaned the Norepinephrine to 4. They decreased her Fentanyl from 50 to 25 and she is on Propofol 50. They increased her tube feeds to 45 please can you tell me what all of this means? The nurse also told me that she had her last echo on September 4 and her ejection fraction was 50 to 54.
Also the doctors have not called for another family meeting at this time. They haven’t really said anything, I have been attempting to avoid them during rounds today they called me out of my sister’s room and asked if I had any questions I told them no, the doctor stated that my sister heart is weak and that they will try and extubate her when they have weaned her off of the heart medications. My sister is able to open her eyes and nod yes or shake no and respond on command. Please help me to understand

Recommended:
Hi Emma,
Just to quickly summarize our phone conversation
- It’s good they are trying to wean the inotropes/vasopressors down
- It’s a sign your sister’s heart is getting stronger slowly
- Ejection fraction(EF) 50-55% is OK, however keep in mind this is with the support of the inotropes/vasopressors like Dobutamine, Norepinephrine, Epinephrine and Vasopressin
- Ideally EF is >50% without the inotropes/vasopressors because that would be a sign your sister’s heart is working without life support
- Dobutamine is increasing the contractility(=pump function) of the heart, whereas Norepinephrine and Vasopressin are squeezing the blood vessels to have more blood available close to the heart to pump through the body
- Reducing Fentanyl and Propofol is very good, the lower the sedation the better so your sister can come out of the induced coma
- The more awake your sister is the higher the chances she can come off the ventilator
- Before she can come off the ventilator and have the breathing tube removed(=extubation) they need to have a plan what they’d do if she can’t breathe by herself
- Please send me the pictures of the ventilator and the monitor so I can see if your sister is close to being extubated and if it’s realistic that she can be extubated
- Next, please make sure you stay positive throughout all of this, you are the most important person in all of this and you need to stay positive and sane. Don’t let your emotions overwhelm you. Emotions are important and they are a healthy sign, however you need to use them strategically and whenever they serve you. There will be plenty of time to be more emotional after you’ve been through this
- Take time out when you need to, your sister and your family will need you at your best! You are the most important person in all of this!
- Make sure you get enough sleep, rest, fresh air and drink plenty of water
- You’ve gone a long way and you need to give yourself a pad on your back for being so strong and for having given your sister a second chance at life!
- Don’t take any prisoners and don’t let them take you for a ride!
- Moreover, keep displaying good and strong body language. Head up, shoulders out and maintain strong eye contact with the doctors and the nurses. 99% of families in Intensive Care are intimidated by the Intensive Care team and they can’t even look them in the eye and they also show it by their negative body language that they feel intimidated
- Brace yourself for some setbacks, recovery in Intensive Care is often two steps forward and one step back, don’t give up if it happens and stay positive!
Here are some more articles/videos that will guide you(click on the links)
Please send me the picture of the ventilator and the monitor and I’ll advise of the next steps and/or questions to ask. Anything you need in the meantime please let me know.
Warm Regards
Patrik
Look out for PART 5 of the 1:1 counselling, consulting and advocacy session with Emma in the next few days!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!