Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have peace of mind, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another frequently asked question from our readers and the question this week is
How long should one wait before stopping life support in Intensive Care on a critically ill Patient?
This is another one of those “hot-topic” questions and one of the questions that we get from our readers and clients quite frequently.
And it’s one of the most important questions you as a family member of a critically ill Patient in Intensive Care should be asking yourself, especially if you think that your critically ill loved one maybe approaching their end of life!
But first, let’s go one step back and let’s look at situations where discussions around stopping life support in Intensive Care may come up in the first place.
Many situations in Intensive Care and many conditions in Intensive Care are life threatening, there is no question around that.
Especially if your critically ill loved one is in one of the following challenging, difficult and often heartbreaking situations where they are either
during those situations there may well be a point when the discussions around when and if to stop life support come up!
The first question you and your family may want to ask yourself when it comes to discussions stipulated by the Intensive Care team around stopping life support is whether your critically ill loved one is in a “real” or “perceived” end of life situation!
What’s the difference? Check out this article/video here
Once you are clear if your critically ill loved one is in a “real” or in a “perceived” end of life situation then you can proceed to start thinking or have discussions about
“How long should one wait to remove life support in Intensive Care on a critically ill Patient?”
When it comes to discussions around end of life in Intensive Care or when it comes to discussions around when is the right time to remove or stop life support, it’s rather obvious that the vast majority of critically ill Patients in Intensive Care are in “perceived” and not “real” end of life situations!
The statistics speak volumes! “Only” 6-10% of all Patients in Intensive Care actually die and don’t leave Intensive Care alive!
It means that the vast majority of critically ill Patients in Intensive Care actually survive their stay in Intensive Care and leave Intensive Care alive!
And that’s certainly my experience after having worked in Intensive Care for nearly 20 years and after having worked with thousands of critically ill Patients and their families in an Intensive Care environment in three different countries, where I have also worked as a Nurse Unit Manager for over 5 years!
And it’s certainly also been my experience when I counsel and consult families in Intensive Care, here at INTENSIVECAREHOTLINE.COM that the vast majority of critically ill Patients is surviving their stay in Intensive Care and is leaving Intensive Care alive!
And yet, we have so many families of critically ill Patients in Intensive Care come to us in really difficult situations where they come to us and they tell us things like
- “The doctors in Intensive Care have asked us to agree to stop life support on my mother(father, husband, wife, brother, sister, son, daughter etc…)”
- “The doctors in Intensive Care have asked us to agree to do the unthinkable”
Or they say things like
- “The doctors in Intensive Care have asked us to agree to kill my mother(father, husband, wife, brother, sister, son, daughter etc…)”
And this is where the rubber hits the road really and those statements are really clear statements in terms of what families of critically ill Patients in Intensive Care want and what they don’t want!
What’s happening in reality and from a clinical perspective is not conveyed by the Intensive Care team, because Intensive Care teams tend to be negative!
Related article/video:
Another statement or observation we make quite frequently from families in Intensive Care here at INTENSIVECAREHOTLINE.COM is that families in Intensive Care are telling us
“The Intensive Care doctors are very negative!”
And again it’s my experience too that most doctors in Intensive Care are very negative!
Let’s dive a little bit deeper here and look at why doctors in Intensive Care are so negative!
First off, they tend to be negative, because if they told you that they are going to cure your critically ill loved one no matter what and then they don’t they could be in big trouble…
Next, they tend to be negative because they are running a fairly complex and complicated business that’s dominated by money, by status, politics, power, limited staffing and limited bed resources and it’s also dominated by an often complex hierarchy and politics in the background that heavily impacts on how the Intensive Care team is positioning themselves!
This “Spiel” and what’s happening “BEHIND THE SCENES” also heavily impacts on how the Intensive Care team positions your critically ill loved one’s prognosis, their diagnosis as well as their care and their treatment!
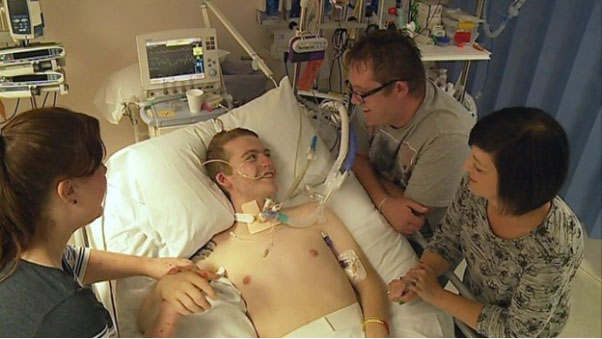
99% of the families of critically ill Patients in Intensive Care make no informed decisions, they have no peace of mind, no control, no power and no influence!
99% of the families of critically ill Patients in Intensive Care also have no idea how to
- Enter discussions around the possibility to stop life support
- Position themselves and their critically loved one in or during those discussions so that they can get the outcomes and results that they want, need and deserve!
Therefore the answer to the question around
“How long should one wait before stopping life support in Intensive Care on a critically ill Patient?”
Is therefore an answer that lies within yourself and not within the Intensive Care team!
After all, Intensive Care units and Intensive Care teams are here to provide best treatment there is to get critically ill Patients out of Intensive Care alive!
Most families in Intensive Care report the opposite and they come to us here at INTENSIVECAREHOTLINE.COM because they often can’t believe what they see and witness with their very eyes…
They simply can’t believe that people who call themselves doctors would ask them to agree to stop live support on their mother, father, sister, brother, son, daughter etc…
It just doesn’t make sense…
What’s even more startling for most families in Intensive Care is that they observe the Intensive Care team telling them that it wouldn’t be in their critically ill loved one’s “best interest” to continue treatment or continue life support because they wouldn’t have any “quality of life” in the future…
Related:
Now, quality of life is a term that’s being misused in Intensive Care and by Intensive Care doctors in particular.
They have misused this term for their own good, to get what they want and to only treat Patients that are of high interest to Intensive Care Units!
The reality and the fact of the matter is that quality of life is something that’s being measured on an individual level and not at an Intensive Care level!
The reality and the fact of the matter is that only your critically ill loved one or you as a family need to decide what is an acceptable quality of life!
Therefore you need to stop being intimidated by the “perceived power” and the “perceived authority” of the Intensive Care team and you need to start making your own decisions.
You may also want to consider things like continuing life support at home with services like INTENSIVE CARE AT HOME where long-term Intensive Care Patients can be safely looked after by dedicated Intensive Care staff in your own home.
The emphasis is on keeping the patient alive as long as there is hope for recovery with a quality of life that is acceptable for you and your family.
And even if there isn’t hope for a full recovery, you may still want to keep your critically ill loved one alive because they wish to be alive and be surrounded by their family!
Again, if that’s the case, have a look at services like INTENSIVE CARE AT HOME. They can provide a genuine alternative to a long term stay in Intensive Care!
Therefore, whatever the positioning of the Intensive Care team in relation to when they think it’s appropriate to stop life support, don’t worry too much about it, because it’s all part of their “hidden agenda”, because you and your family have no idea about what’s happening “BEHIND THE SCENES” in Intensive Care!
Related:
Instead make it your agenda when you or your family think it’s appropriate to stop life support or to continue treatment!
Do so by doing your own research, by asking the right questions and by not being intimidated by the Intensive Care team!
99% of the families of critically ill Patients in Intensive Care are intimidated by the Intensive Care team and they make no informed decisions, they have no peace of mind, no control, no power and no influence!
Don’t be part of the 99% but be part of the 1% who actually make informed decisions, have peace of mind, control, power and influence, because then the answer to
“How long should one wait before stopping life support in Intensive Care on a critically ill Patient?”
Is an answer you will find within yourself and within your own power, rather than trying to find the answer from an Intensive Care team that’s trying to push their “hidden agenda” on to you!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!