Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of my clients Emma, which are excerpts from 1:1 phone and email counselling and consulting sessions with me and the question this week is
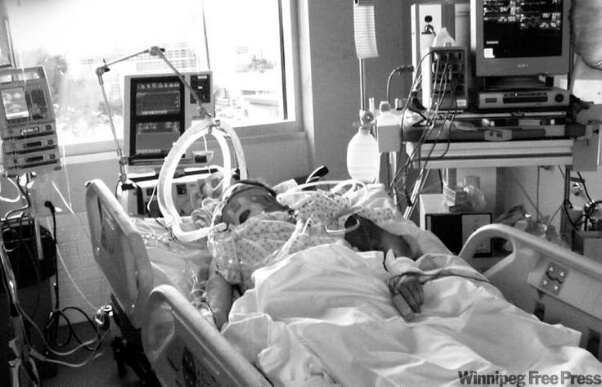
My sister is in ICU on a balloon pump and ventilated after cardiac surgery! The ICU doctors want to stop treatment against our wishes and let her die, what should we do? (PART 2)
In the last counselling and consulting session with Emma we were discussing what led to her sister’s situation and the potential options to improve her sister’s situation. In today’s counselling and consulting session, we focus mainly at why the doctors in Intensive Care can’t just stop life support without Emma and her family giving consent. We work out strategies going forward to buy her sister time to get through this if she can.
Let’s tune right in.
Patrik: That is good. Your sister coming off the inotropes/vasopressors is good. That’s a good sign. Okay.
Emma: Okay.
Patrik: That’s good because that’s life support. If they can wean that off, I like that they’re doing that. And blood pressure 100 over 40, that’s okay. It’s within normal limits. Because what happens, Emma, is when they wean off the vasopressors/inotropes, right, the blood pressure can go down, but given that they’re weaning and she’s maintaining a blood pressure within normal limits, that’s good.
Emma: Okay.
Patrik: Okay. The next thing that’s important really is you can’t … Don’t worry about the doctors getting upset. You really need to stop worrying about that. You know-
Emma: Okay.
Patrik: … that’s something you’re observing, that’s fine. Observe it, but just, you know, you can’t absorb their emotions. You can’t. Because that will stop you from getting what you want.
Emma: Okay.
Patrik: So I know this is a tough road. You know, this is a tough road but you can’t be watching what their emotions are. You’ve got to manage your own. That’s way more important. Way more important.
Emma: Okay, okay.
Patrik: Also, so it’s good to know, on the one hand that they’ve got ECMO on the other hand it’s very disappointing that they didn’t tell you about it from the start. That’s not being transparent, right?
Emma: Okay, fine.
Patrik: i think it’s highly inappropriate not informing you about this. You know that this could potentially be an option. If I said to you, 15 years ago instead of ECMO, they were using the balloon pump/IABP. The balloon pump is more or less coming out of vogue in this day and age because ECMO is the standard therapy for that type of situation. Right.
I hear what you’re saying in terms of they can’t perform the surgery. I have yet to find out whether that’s accurate or not. But even if they can’t perform the surgery for a medical reason, or I should say for a valid medical reason, even if they can’t do that, then they should still offer your sister ECMO to potentially be listed for a heart transplant. But, I mean, that needs to be discussed with you and your family. I do believe that’s inevitable. To be discussed.
Emma: Okay.
Patrik: And not discussing it, it’s not transparent. It’s not laying out the options for you.
Emma: Okay.
Patrik: Right. So here is the next thing that’s really important. So the last email that I sent you, the third email, there is an advanced directive in Texas that’s, hang on. Just give me a second because I’ve got it open here on my computer. Just give me one second. Let me read this out to you. But you’ve gotta go on this site when you have time because this is so important. This is a law, legislation, just for Texas. Just give me one second. I’ll read this out to you because this is really important. So …
“Life sustaining treatment policy” Okay this is a law in Texas. “On request of a patient or authorised health care proxy,” which would be you or your brother-in-law, “treatment efficient on behalf of a patient or prospective patient, a health care facility or physician treating the patient shall disclose in writing any policy relating to the provision of life sustaining treatment to the patient in the health care facility.”
Okay?
Emma: Okay.
Recommended:
Patrik: This is something you can use because that’s a law.
Emma: Okay.
Patrik: Right? Now I’ll carry on. I’m going now to section B. Okay.
Section B says, “Health care facility or physician may not withhold or withdraw life sustaining treatment from or place any restrictions on the provision of life sustaining treatment unless withholding or restricting the provision of life sustaining treatment is authorised.”
Okay. You have not authorised anything.
Emma: No, we have not.
Patrik: So, you know, that is why you can’t … You know you can observe that they are upset but you are acting within your rights. You’re acting within the law and they are trying to breach the law. That’s why I don’t think that you referring to murder is an exaggeration. I don’t think it’s an exaggeration at all. Because the law is crystal clear.
Emma: Okay.
Patrik: Right? So it’s all in the email that I sent to you. I put a link to that article so that you can go back to them and say, “Hey, are you trying to breach the law?” You’ve got to be very firm with them because they are used to getting away with all sorts of crap because people don’t question. You’ve got to be really firm with them.
And if I was you, I would not … You know, all you’ve got to tell them is what you want. Don’t go overboard. Just stick with saying what you want. And now that you’ve got a reference to the law, I’m pretty sure they will look at you very differently.
Recommended:
Emma: Okay.
Patrik: Right. So, there are no guarantees, but for now, as I said in the email, your goal is to get your sister through the next 24 hours and through the next 24 hours until we know what’s happening clinically.
Emma: Okay.
Patrik: Right.
Emma: Okay.
Patrik: What’s your next step … Are you … So for you it’s night-time at the moment. What’s your next step in terms of, you know, are you going to see the doctors tomorrow? What’s your next step?
Emma: So what they’re doing, they haven’t said anything about another family meeting-
Patrik: Good.

Emma: What they do tomorrow … So that’s good if they haven’t said anything about a family meeting?
Patrik: Well, I think it is good because, I tell you what happens in family meetings. I’d say nine times out of 10, in family meetings, they deliver bad news. How many family meetings have you had so far?
Emma: So far, we’ve had two.
Patrik: Okay and was there any good news in those family meetings?
Emma: None. None. Nope.
Patrik: No. No. No. Family meetings in Intensive Care are designed to deliver bad news nine times out of 10, bad news are being delivered, right? And it’s almost like a power display. You know they probably … Have they had a meeting in a room? Have they dragged you into a room?
Emma: They have. They have.
Patrik: Yeah, you know, it’s a power sign. You know, they drag you into a room. You play to their rules and they deliver bad news. Don’t play that game.
If there is another family meeting, number one, you want to know what the agenda of the family meeting is. You want the agenda in writing, right, and then you decide whether you go there or not depending on the agenda.
Emma: Okay.
Patrik: You’ve got to change your communication with them. You’ve got to be very firm. You’ve got to turn it all upside down because 99% of families in Intensive Care do not question. You are in the 1% bracket already but you’ve got to turn it all around. You’ve got to change your communication.
Related:
Your three major concerns at the moment are number one, your sister staying alive on life support. That’s number one. Getting the withdrawal of treatment policy, which you probably don’t need anymore because you’ve got the law even on your side, right? And number three, look into the options for either surgery or ECMO and that’s all you’ve got to tell them. Stick with that. Don’t go overboard. Don’t go into any discussions about quality of life because that’s all bullshit. Excuse my language, but it’s a perception.
What’s quality of life? Who’s to judge quality of life? That’s up to the individual not to the doctors.
Emma: Okay.
Patrik: Right? That’s a perception, I can’t, nobody should be questioning what quality of life is acceptable for your sister or for you. That’s something that’s up to the individual, not to the doctors.
Emma: Mm-hmm (affirmative).
Patrik: Right.
Emma: Okay.
Patrik: So don’t go into those discussions. Don’t even go there. Just stop them and say I don’t want to talk about it. Just stick with those three points.
Emma: Okay.
Patrik: Your three points are: Keeping your sister alive on life support; Referring to the law about withdrawal of treatment and; Investigate why they’re not doing the surgery because I still haven’t had a medical reason for that and investigate ECMO. That’s all you’ve got to do for now.
Emma: Okay. Okay.
Patrik: Does that-
Emma: Like tomorrow, huh?
Patrik: Does that make sense so far?
Emma: It does and I’m glad that we getting it a little bit at a time because we … So that’s what I’ll focus on with them. But like tomorrow, they make rounds like with the nurses and the patients at 10 and they involve the family, so what should I do at that time of the meeting with the family? With the rounds.
Look out for PART 3 of the 1:1 counselling and consulting session with Emma in the next few days!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!