Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Husband Is in ICU with COPD. Will He Be Able To Wean Off The Ventilator?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer questions from one of my clients Rebecca as part of my 1:1 consulting and advocacy service! Rebecca’s husband is ventilated in the ICU, on ventilator weaning and is asking why does the ICU team delays early mobilisation for him.
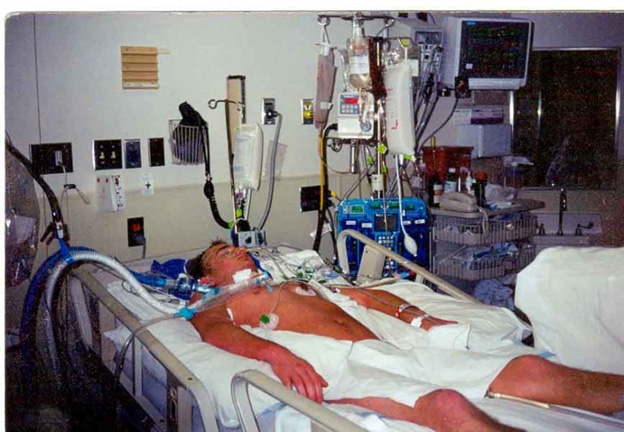
My Husband is in the ICU on Ventilator Weaning with COPD. Why does the ICU Team Delay Early Mobilisation for Him?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Rebecca here.”
Patrik: Sure.
Doctor A.: Situations.
Patrik: Okay, so at this point in time, he’s breathing in SIMV, or in CPAP at this… right at this point in time?
Doctor A.: At night he’s on support.
Patrik: Right, right, right. And then during the day you put him into CPAP or what’s your sort of process around managing that?
Rebecca: Patrik?
Patrik: Yes.
Rebecca: I’m sorry for some reason the phone dropped.
Patrik: That’s OK.
Doctor A: Alright, I’m going to run along. Any other questions?
Patrik: Yeah, the other question that I have is, so, what’s your process around getting in between CPAP and SIMV, getting him on SIMV overnight to give him a rest and get him on CPAP during the day, or…
Recommended:
Doctor A: And that’s the strategy.
Patrik: Right, right.
Doctor A: CPAP during the day consistently then we try and go to the twenty-four hours.
Rebecca: When you say consistently…
Doctor A: Meaning no issues, no going backwards. CPAP straight, remove him from the SIMV mode and we know that for the last five day he’s had CPAP, no issues, no going back, no somebody coming in saying that they had to shut him down and put him over. Then you know that you’ve reached that one goal, and then now it’s been back and forth, back and forth, back and forth, back and forth. But at night you should consistently give him twelve, because that was our goal, that can he handle the CPAP during the day, then if he handles that then you start to go back on the pressure supports and eventually, maybe, get him on the T-piece. And he has to graduate, and he hasn’t graduated. He’s been failing a couple classes.
Rebecca: Ok, so Patrik he’s saying you have to do the CPAP for at least five consistent days.
Patrik: Yeah, I hear that, I hear that. And doctor tell me his secretion management and issue? Are there a lot of secretions that need to be managed or…
Doctor A: No immediate problems.
Patrik: OK, so OK it’s not a secretion problem, it’s just a strength problem really.
Doctor A: Yes. His spontaneous has been variable. We had him start at like three hundred, but he’s actually between three and five.
Patrik: And how much oxygen and PEEP is he on at the moment?
Doctor A: He’s not on much. He doesn’t require much, at 28%.
Patrik: Right, and PEEP is?
Recommended:
Doctor A: But he hasn’t really had an oxygenation problem.
Patrik: And what’s his PEEP and pressure support like at the moment?
Doctor A: He’s on PEEP at five, but it should go to ten.
Patrik: Right, so not much really on that aspect. Right, OK, OK, well thank you, thank you so much for taking the time. I do believe that from our perspective, you know, mobilisation is going to be a critical part and we need to find out what’s happening on that end.
Doctor A: I believe because he’s got that wound vac on and you can’t sit on that and you kind of suck in trying to make that thing granulated.
Patrik: Sure, but early mobilisation from my experience, early mobilisation is critical. And yes, acute care is slightly differently, but never the less I’m sure you would have seen early mobilisation being a big component of having a successful wean.
Doctor A: Yeah, before he got here they had issues with that and he wasn’t moving around early, early on because whatever else happened in the beginning. And I have to refer back to when he first came here, it was a couple months ago, but while he’s been here why he hasn’t been able to progress, that you’d have to, Rebecca would have to check with the rehab people and then Doctor A and maybe have a meeting with him to find out what’s going on, what’s the goal, you know each week has goals. He would say, “This week we’re going to try this, this week we’re going to try…” I always knew what I was thinking, and so we were both, you know we were able to share notes when we come in. So now, they need to kind of do the same thing for other aspects of his care as far as rehab is concerned. See what the impasse is and go from there.
Patrik: OK, hey look thank you so much for explaining the situation to me from your perspective. Thank you.
Suggested links:
Rebecca: OK.
Patrik: OK, Rebecca, do you want me to call you back shortly or…
Rebecca: No, no, no, he just left so we can go ahead and talk.
Patrik: OK, great. Look, what he’s saying makes sense to a degree. I mean, he’s hand balling off responsibility to other people in terms of mobilisation, you know he’s saying he’s not responsible for that. Well, you know, a situation like that takes a team, it doesn’t only the one person to make it a success.
Now, if he’s telling me that your husbands CO2 is 113 on CPAP at times, he’s definitely not ready to come off the ventilator, I agree with that, if the numbers are accurate. Right, I mean…
Rebecca: Right, I don’t think the numbers are accurate though…
Patrik: You don’t think the numbers are accurate?
Rebecca: No. So they’re going to do another one tomorrow.
Patrik: Right, OK.
Rebecca: Is that too soon, Patrik?
Patrik: What do you mean is it too soon?
Rebecca: I mean will the levels be gone by then, let’s say…
Patrik: Oh, yeah, yeah, yeah. So I’ll tell you how that works, so, he’s telling me his CO2 levels are a hundred and thirteen, so by CO2 we’re talking about carbon dioxide, do you know what that means?
Rebecca: Right, yes.
Patrik: That’s right, and because he’s got COPD, isn’t that right, your husband has COPD?
Recommended articles:
Rebecca: You’re right.
Patrik: Right. So I can see how his CO2 levels might go off, if he’s not ready to breathe by himself. So let me explain this to you. A normal CO2 level is between 35 and 45, OK. He’s telling me your husbands CO2 levels at times is 110, sometimes 137. OK. Now, bear in mind with a patient on COPD, their baseline COPD level is usually higher, so you know when I say 35 to 45, that’s for a healthy person. For somebody with COPD the CO2 would probably be more like around the 50 or 60 mark as a base line, OK.
Rebecca: And that was his last ready, 51.
Patrik: Right, right, there you go. So, with then the CO2 at the moment sort of above the 110 mark, that is a concern, right. The other thing that often happens, when patients have a high CO2 level, I mean he told me that your husband isn’t always, sort of, responsive. If his CO2 levels are too high it’ll impact on his brain. He will become drowsy with a high CO2. Right.
So then, when they change him to SIMV, when he has a high CO2 level it will get his CO2 levels down fairly quickly, within hours normally. So from that perspective I’m following what he’s doing, I’m definitely following there what he’s doing. My biggest concern, and you know that’s the reality of COPD, my biggest concern really is the not mobilisation.
And why do I keep coming back to that? Could you hear what he and I were talking about? Could you hear that?
Rebecca: Absolutely, I sure did.
Patrik: Right, right, so you would have noticed I asked him that your husbands been there since the first of February, and now we’re you know the end of April and there hasn’t been any progress.
Rebecca: No progress.
Recommended links:
Patrik: Or not much, right. So then I said to him, “Well, why has there been no early mobilisation?” Right, and he’s making up all these excuses that he’s not in charge of that, but at the end of the day him as the Pulmonologist, and in charge of weaning the ventilator, well he should liaise with his colleagues to make sure your husband is getting mobilised.
Rebecca: Exactly, that’s the same that I said, Patrik. Yes.
Patrik: That’s the missing link. You know he makes perfect sense to me from just talking about ventilation, that all makes sense, right, I’ve seen that over and over again. But the missing link, to me, is not being mobilised. Now, one way to strengthen breathing muscles is by mobilising him. That’s one way to strengthen breathing muscles.
Rebecca: Right.
Patrik: Right. And that to me is massive concern that is hasn’t happened. Now, he’s talking about the pressure sore and all of that, yes I get that, but you know, you’ve got to weight up what’s more important, they can put a cushion, a really soft cushion on a chair and still mobilise him, even if it’s only for an hour a day to begin with. Right.
Rebecca: I agree.
Patrik: You’ve got to start somewhere, and they’re making too many excuses there. Let me ask you another thing, have you had any meetings with the whole team involved?
Rebecca: Not yet. I’m going to go to the first meeting on Tuesday. Normally my daughter goes, but I’m going to go this Tuesday.
Patrik: So, you’ve had meetings, it’s just that your daughter went instead of you, is that what you’re saying?
Rebecca: Correct.
Patrik: Right. And that’s with the whole team?
Rebecca: Correct.
Patrik: Right, OK, OK. Look, I would be very happy to be there over the phone with you if you like.
Rebecca: OK, I certainly would. So, I have to go into another…
Patrik: Look we can either do that, or we can stop now and you know you’ve used about half an hour, I’m not counting minutes, you’ve used about half an hour, very happy to get into the meeting and see how it pans out.
Recommended articles:
Rebecca: Yes, I would love that. And if it’s going to be more than I will pay that.
Patrik: That’s fine.
Rebecca: I’m going to go on Tuesday and I would love to conference you in.
Patrik: Yeah, what time…
Rebecca: It’s Tuesday at 11:00.
Patrik: Tuesday at 11:00. Yeah, that should be…oh…you are sure that it’s Tuesday at 11:00?
Rebecca: Tuesday. They probably don’t start at the right time, it’s going to be, it’s Tuesday between 11:00 and 1:00, so…
Patrik: Between 11:00 and 1:00, just give me…yeah yeah, yeah yeah. It’ll be a bit tricky…It’ll be a bit tricky for me. Let me see if I can make arrangements and get back to you. If I can’t make it, we’ll use that half an hour to set you up with the right questions.
Recommended:
Rebecca: OK. What I could do, I’m going to tape the meeting…
Patrik: That would be helpful, but prior to that if I can’t be there, let me check my diary and I’ll get back to you, if I can’t be there, we’ll half an hour talk before the meeting and I will set you up with some important questions to ask.
Rebecca: Fabulous. Thank you, oh my gosh, thank you so much.
Patrik: You’re very welcome. You’re very welcome. I’ll be in touch.
Rebecca: OK, thank you. Have a good evening.
Patrik: And you, bye bye.
Rebecca: Bye.
Patrik: Bye bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!