Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
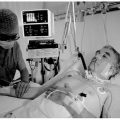
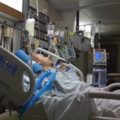
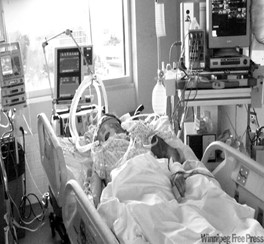
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Erwan, as part of my 1:1 consulting and advocacy service! Erwan’s mother in law is with a tracheostomy and on a ventilator and Erwan feels that his mother-in-law is unsafe in LTAC.
My Mom-in-Law is with a Tracheostomy and on a Ventilator and We Feel that She is Unsafe in LTAC! Help!
Patrik: I’m almost bound to say it’s almost criminal having one nurse looking after four or five patients and one of those patients is on a 100% percent of oxygen. That’s almost unheard of. I would argue it needs to go back to ICU rather soon, or, they need to show to you that she is safe and I don’t think they could show that to you.
Erwan: Okay. And then I saw you have different I guess ranges of agreement. And I was thinking of the two week one, just to help us get through this time or have someone… Well, they’re saying this to us, what’s our response or what can we-
Patrik: Absolutely.
Erwan: And then is that until… Is it basically advice like this, phone console, phone advice, or is there any drafting of, I guess if there’s a document demand or anything like that, or…?
Patrik: Or email, even text messages, whatever… Phone, email, Zoom, text messages, whichever works best. Also, if you wanted me to get on a call with the doctors, with you or your father-in-law or whoever, or with your wife, we can set up a conference call or set up a zoom call, whatever works. But, I do believe a call with the doctors would be beneficial or even with the nurse in charge or the nurse that knows your mom-in-law.
RECOMMENDED:
Patrik: To get information, all the information you said is incredibly important, but, there’s probably more than 50% still missing. I would want to know what the ventilator settings are. What are her arterial blood gas? What is their plan for weaning? Why are they not escalating treatment on a 100% of oxygen or maybe they have, and they haven’t told you. You have shared very valuable and relevant information. The question is what’s happening with the other 50% that we don’t know yet?
Erwan: Right. And so would it be like screenshots of the vent or the machines that are in her hospital room when we’re visiting her or…?
Recommended:
Patrik: That would be very helpful. That would be very helpful, but other things can be simple things maybe we should, one time a day, doesn’t matter what time of the day do a quick phone call to the nurse or to the doctor and get an update. I believe I can get so much more information from them because I know what we need to focus on to get down to the bottom of things.
Erwan: Well for that, I mean, I’m thinking, for two weeks… I’m on my computer real quick, just to say, because that’s why I asked for the consult this early in the morning so we’d have time to do something today if possible. So the two weeks unlimited email counseling consulting, 497. Is that the one that would include you being available to talk to the doctors or is that just-
Patrik: That would be just email. That would be just email.
Erwan: Okay.
Patrik: If you’re looking for phone access to me for two weeks, I think it’s pretty much on top. What I’ll do, just give me a second. I’ll just quickly send this to you. Can you see it?
Erwan: Yes. I see it now. Okay. I had scrolled down too far then. Okay.
Patrik: That’s all right.
Erwan: We’re even just maybe starting with the seven days one.
Patrik: Even if you want to start small, you can even start with an hour and then upgrade. If you for example, even started with an hour and then you wanted to upgrade to the seven days or even to the two week option, I’ll refund you the hour.
Erwan: Okay. Well, I think I’m going to do the four days and then see if we need to upgrade from there. Because I think in the next four days, beginning today, if you’re, I mean, I’d hope if you are available later. I know it’s late in Australia. Because my father-in-law will be at the hospital about the afternoon, but then at least help get you that information on the missing 50% and then we would maybe come up with a plan in the next four days of if we need to have a transfer or not.
Patrik: Okay, So you think maybe did you say 2:00 AM? 2:00 PM?
Erwan: Yeah. 2:00PM is about the time he will be there.
Patrik: Yep. That should be fine. I’ve got a call at 3:00 PM your time, which will be 8:00 AM for me tomorrow morning, but, to begin with, I can definitely talk to you between 7:00 AM and 8:00 AM. And then I have a quick call at around 8:00 AM. Well, I should go with your time. I’ve had 3:00 PM your time for about 15 minutes like this one and then I should be free after that again.
Erwan: Okay. And then that way it’s not coming from me and my internet research to the family since she’s my mother-in-law but I’m not the main decision maker. I think having someone outside based on this will be truly helpful.
Patrik: That’s what we’re finding all the time. The biggest challenge is, families don’t know what they don’t know, and you’ve seen some of that already.
Erwan: Okay. Is there anything that we have to sign or obtain from you?
Patrik: No, there is nothing. That’s nothing you need to sign. It’s really, you go through the checkout. That’s pretty much all. There’s something you need to sign.
Erwan: Okay. I’m just saying, it looks like the payment went through, because I use PayPal, but when we speak with the hospital, we just have you on the phone and what if they say, “Well, who is this? Who are we speaking with?”
Patrik: That is a great question. That is a great question. Look, you could introduce me as a consultant/advocate. You could do that. However, it might get them defensive. If you think it makes them defensive, you could also introduce me as a family friend that’s got a critical care nursing background. That makes it less threatening for them. I believe that approach usually always gets us more information. Because, they do feel threatened you bring in the word consultant/advocate, they do feel threatened. And we can still advocate as a family friend with the clinical background.
Erwan: Okay.
Recommended:
Patrik: That has been my experience. But that’s not to say that the consultant/advocate approach won’t work. I don’t know the team there yet. What’s your impression?
Erwan: I’m probably not the best to, because I’ve only met the nurses and they’ve all been really nice to me and just the few I’ve met. But, I don’t-
Patrik: Nurses will be fine. I’ll tell you what, the nurses will be fine. I’m a nurse myself so I can easily talk to the nurses. I can talk to the doctors too, but the doctors have more to lose in this. The nurses, they’re just doing their job. They’re nurses, they’re trying to help people. For the doctors, there’s more at stake. The doctors are always guarded in what they share and what they don’t share, in how they say things, when they say things, what information they’re withholding. Whereas if you talk to the nurses, you should get all the information from nurses, but they’re also not decision makers.
Erwan: Okay. I feel that we need to do this and figure that out. I’ll share the information with my wife and father-in-law later about the understanding that being on a 100% is pretty critical and if nothing improves, I mean, even if it’s traumatizing to her to move her via EMS or ambulance, hopefully we can communicate with her enough to let her know, “Hey, you’re going to move. This is a way because of the procedure with the insurance or what have you that works out, but at least you’ll be in an ICU.”
Erwan: The only problem is the ICU as I’ve called around here, they won’t let visitors. So at least here we’re able to visit her. But at the big hospitals right now, I see is we’re not allowed to visit.
Erwan: Yes. So that’s my concern, will that hurt her just because-
Patrik: Yeah. If she’s going back to ICU, do you think she’ll be going back to the ICU where she came from?
Erwan: No. So when I called around, they said, you can have the ambulance because it’s your right to have it. It’s not like an ICU to ICU transfer. It would have been before this ICU LTAC, but they have to say she’s critical enough to come back into the ICU, and that makes sense what you just said because I didn’t really understand why. But, they said they could bring her to the closest ICU, but you have a right to pick which ICU you want her to go to in the area, as long as there’s a bed available.
Suggested links:
Patrik: Just about to say. My concern at the moment would be shortage of ICU beds with COVID. That would be my concern. I know for a fact that there are makeshift ICUs coming out of nowhere because of COVID.
Patrik: That’s not to say she can’t find a bed and I don’t know the COVID situation in your place. But certainly, I’m talking to people from places near you, and their situation is very bad there. It’s very bad.
Erwan: Our numbers have gone down. It was definitely a lot worse when we were trying to move her a month ago or before she got to the LTAC. It was like full capacity at that time. But my understanding is there are more options available to us right now until the numbers maybe spike again, or the new strain starts spreading elsewhere. But my other concern is just that they show that she had COVID or was it COVID patient, I don’t know if ICUs would accept her if that’s in her medical records, but maybe they can’t deny her as long as she’s not COVID positive at the time.
Patrik: Sure.
Erwan: Is there a way for you to look at the different hospitals in the area or see-
Patrik: Oh yeah, for sure.
Erwan: We get to that point, but at least to have information to say, well, this is the ICU we would prefer her to go to.
Patrik: Absolutely. Look, there’s not only can we do research, we can look up hospitals, but if you wanted us, we can also make some phone calls, no issue there.
Erwan: Okay. All right. Well, thank you so much. Appreciate your time. And I know we went over, but I look forward to talking to you later today my time and-
Patrik: Shall we-
Erwan: … Tomorrow your time.
Patrik: Shall we aim sort of for like 2:00 PM your time, roughly?
Erwan: Yes. What I’ll do is I’ll message you. Is it easier for texts or email?
Patrik: Text is easier. I won’t write lengthy text messages. I might write a lengthy email, but I can’t type on my phone very well.
Erwan: Sure, I understand.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: But, look, if you need to get hold of me quickly text, and I know you left a message earlier for me a voicemail. It’s not that I didn’t get your phone call earlier. I was on another call. That’s why I couldn’t pick up.
Erwan: That’s fine.
Patrik: But, text is fine. And if you need me urgently, just call.
Erwan: Okay. That’s great. I appreciate it so much. I’ll text after noon o’clock our time here of what time in the afternoon it would be with my father-in-law when he’s up there.
Patrik: Yep. Yep. Absolutely. That’s a real commitment. You’re getting up at 4:00, 4:15. That is real-
RECOMMENDED:
Erwan: I came across your article about a lady who did not get her, or she was being convinced to take her dad to the LTAC, but she didn’t because of the counseling you were providing and her dad ended up being discharged from the ICU he was in three weeks later. It’s crazy because I had come across your website before my mother-in-law had the tracheostomy and I thought about it and I’m like, “Well,” and I was kind of more of an outsider with the family, but I pray that the time she’s lost can be restored and that hopefully, we just have some answers somehow-
Patrik: Absolutely.
Erwan: To know that we did everything. So, thank you.
Patrik: Thank you. Go and get some sleep. We’ll talk later.
Erwan: I will. Okay, thank you. Bye-bye.
Patrik: Thank you, thank you, bye. Bye.
Erwan: Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!