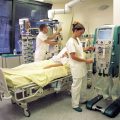
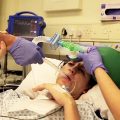
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Bea, as part of my 1:1 consulting and advocacy service! Bea’s mom died in ICU due to medical negligence and Bea is asking if she can file a criminal case against the ICU team?
My Mom Died in ICU Because of Medical Negligence. Can I File Criminal Charges to the ICU Team?
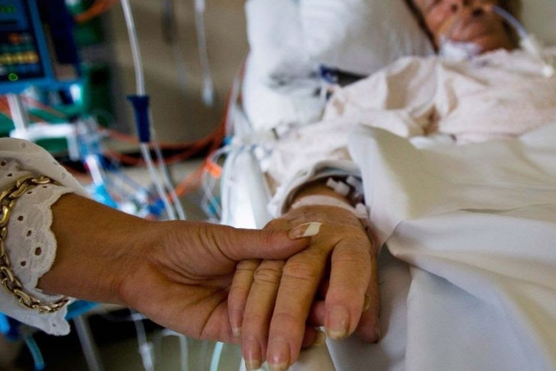
“You can also check out previous 1:1 consulting and advocacy(7) sessions with me and Bea here.”
Patrik: What does it say? What does it say?
Bea: Let me read it to you, okay.
Patrik: Thanks.
Bea: Just a second. Cardiopulmonary arrest.
Patrik: Cardiopulmonary, okay. And that’s it? Anything else?
Bea: Oh yeah. Second it says sepsis, S-E-P-S-I-S.
RECOMMENDED:
Patrik: Yeah, sure. Sepsis is a bloodstream infection. The reason I think this, I tell you where I see a mismatch straight away, okay. So normally apnea testing is only happening when patients are being tested for brain death. Or, for brain death, okay? Now, if your mother was brain dead, that should be the cause of death on the death certificate.
Bea: Really?
Patrik: Oh, absolutely. Yes, a cardiopulmonary arrest is almost always the cause of death. But leading up to this would be brain death. But do you have, besides the death certificate, do you have any other? So you still don’t have all the medical records, do you?
Bea: No, I only have partial. Which is many pages, I have 1000 pages. But let me tell you, on this death certificate, the third item is end-stage Raynaud’s disease, which yes my mother had that. She didn’t die from dialysis. She also didn’t die from infection because the record shows her infection was controlled so well. It’s outside, no blood infection. And she was there for 10 days. You cannot blame that. So cardio-
Patrik: Cardiopulmonary arrest. Yeah.
Bea: Everybody die from that.
Patrik: Well in ICU in particular. But you see, if your mother was brain dead, that should be the cause of death. So, I tell you where there are more missing links then, as far as I can see. Most of the answers that you’re seeking for or some of the answers that you’re looking for would be in the medical records. Now you are the medical power of attorney for your mom or you were the medical power of attorney for your mom?
Bea: Yes. That’s why I was able to get the records from the day she arrived on the day she passed. But, these are records only the hospital that was received but nothing from the nurse station or the ICU nurse notes. I only have some from doctors. Because after that, I think someone was trying to change the record.
RECOMMENDED:
Patrik: Yes, sure. Those records that you have, are they copies of paper or are they online records? What are they?
Bea: There are copies, paper copies.
Patrik: Paper, hard copy? Okay. The reason I’m asking, some-
Bea: Only because they are easy for me to read.
Patrik: Yeah, sure. But you think they are incomplete, that’s what you think?
Bea: Oh, absolutely. Because you know why? Because there are significant amounts of investigation going on with the nursing board. The nursing board detective has called me in one day because he had all the records. And I only have half that there because his record is two more, twice. I read from the record there that I’d never seen before. He has it because he was investigating them and that’s privileged. So I think they’re prosecuting some nurses there.
Patrik: Wow, wow.
Bea: That’s how severe it is.
Patrik: That sounds full on. You being the medical power of attorney for your late mom. You can have access to the medical records. I’ve never had a client who can’t have access to the medical records, as long obviously as they are the next of kin or the medical power of attorney.
Bea: Here is what they asked me, I went in a second time they want me to give in the death certificate. I am not going to go there for that. I don’t want to give them anything.
Patrik: Say that again. Say that again please, they want you to?
Bea: Give them the death certificate before they release any record.
Patrik: I wouldn’t worry about that.
Bea: I have my daughter to do that because the record is her name too, listed to be a person and contact. I want that way to make sure.
Patrik: Yep, absolutely, absolutely. So look, I do believe a lot of the answers that we’re looking for will be in the medical records. And it’s great that you’ve got the doctor’s medical records. But you’re absolutely right, there need to be some nurse’s records. There also need to be some vital signs records from her time in ICU, well from her time on the ward.
Bea: Let me tell you two more items. I thought it was interesting because on that day I receive a call. I told you I was going into hospital, but before I did the doctor called me, admitting doctor, that’s an employee from the hospital. He told me that my mother did the apnea tests and they declare her dead today. Oh, he didn’t say that. He said, “Oh, we need to pull the stuff out of you.” He didn’t say my mother’s already…
RECOMMENDED:
Patrik: Right, right.
Bea: He did that so that I told him, I was really emotional. I said, “Please don’t do that. I have other family members that I need to contact overseas. They will like to come over, to at least say goodbye to my mother.”
Patrik: Absolutely.
Bea: I think that is allowed.
Patrik: Say that last-
Bea: I said at least they would allow me to wait until they come.
Patrik: Yes, absolutely.
Bea: And the doctor seems to do that and they already put my mother to death. Although after she was dead, they put the life support back. It doesn’t do any good. She was already taken that morning when I talked, revived a call. So when I receive a call from this doctor, he told me that they need to pull that, I told him, “Please don’t do that.” I begged him not, this is a doctor whose name on the death certificate as well. He wrote all the reasons. I think he’s very guilty. He knows he’s guilty.
RECOMMENDED:
Bea: So anyway, after that I contact the hospital administrator, the CEO’s office. I talked to the CEO assistant and she was very nasty. She was telling me the same story. I guess they probably report to her already that day. At that time I didn’t know she was treating me badly. I didn’t know that they have already had tons of issues with the floor because of that nurse. Obviously, I didn’t know if you remember that stuff happened on the 22nd or 23rd.
Bea: I actually didn’t know there’s something happened upstairs. But, the administrator did because this nurse has been talking to every possible authority in the hospital. So they called him to the CEO’s office to report the incident and accused these people of murder. Can you believe it? She accused these people of murder because she believed in her intuition. She observed these people to kill my mother. Also, she said he’d seen other people neglected on the same floor by falling off the bed, they let them die. She had a lot of evidence, which is great.
Patrik: Absolutely.
Bea: But, I didn’t know that. So when I contacted the CEO’s office, she was nasty to me. I didn’t know. I actually told her I’m recording our conversation. Obviously, that didn’t last long, she wants to hang up. She don’t want to report. I told her, “I need you to tell me where is that law that you will unplug the life support while waiting for the family member to come over.” Whether or not she’s dead, I don’t know. But we need to say goodbye to her in the proper way.
RECOMMENDED:
Bea: They killed my mother. According to the nurse, some of the people on that floor, which is 7th east, that’s where my mother had gone before, several years ago. As I told you, there were incidents that they tried to keep my mother. I had a fight with them continually because they neglected my mother. I try so hard to save my mother and they painted me as somebody who they think I was crazy. Yes, I am crazy because I want my mother to live. Yes, not dead.
Patrik: Absolutely.
Bea: And then obviously on this incident, I can see some of the records that I order. Some doctors put notes in there, in the case, I was not allowed them to have surgery on my mother. Can you believe it? That’s what they aiming for. They want to do surgery on her arm while she was so lacking in everything. She was a severe anemic in hospitals. She was severe lack of food. She could hardly stand up. She is the lady who can’t hear well. She is literally legally blind, that’s certified. She can’t see, can’t hear any sitter in front of her bed.
Bea: She wanted to get out of bed. They won’t allow her. They told her she needed to stay in bed. We had the food delivered to her room, only to be put on the corner. Nobody offered to her. She doesn’t know where it is, so she had been left starving for days. Each time when I go there, I request them. They bring hopefully a nutrition drink just because I want to make sure, keep her alive. She doesn’t look good.
Patrik: Yeah, I’m following. I’m following.
Bea: In the case they said I am not allowed this and that. Yes, I did not allow. There’s a base. I did not say that you are performing put her life to danger. I did not lie. The people don’t even check, they get my mother doubled blood pressure medicine. One day my mother blood pressure, high one is 80, lower it’s 35. That could die. And I told them, “You’re out of your mind. I give him all the list of medicine. I give you the detail on her condition. I cannot be here 24 seven.”
Bea: And also the nurse witness told me, she also requested my mother to have a sitter because my mother wanted to get off her bed. She’s restless. She doesn’t have any other sickness except the related kidney issues, which is anemic. And the lack of food causes by her restlessness as well. And then she was not getting proper nutrition in her dialysis as well. Although we were trying to coordinate with the dialysis doctor outside. But, the dialysis doctor in the hospital is the doctor who also works in her regular dialysis, that doctor is the evil. And he is also… I think we probably have to find a lawsuit listing his name on it too. We’ll talk about that later.
RECOMMENDED:
Patrik: Right.
Bea: At this moment, at that time, I read the record, some of them were misleading about me. I don’t mind because that can be easily explained. I have a duty to protect my mother who’s helpless.
Patrik: Absolutely.
Bea: And there’s nobody cares. They want to put her to death. They think she’s useless. She can’t see, can’t hear, can’t walk. And then they hated me for wanting her to live.
Patrik: Right. Do you know, when this was happening with apnea testing, do you know whether your mother was in an induced coma or in a natural coma? Do you know the difference?
Bea: I don’t know. She was in a code blue.
Patrik: She would’ve been in a coma. There’s no doubt that your mother was in a coma. The question is-
Bea: Let me give you a detail, sounds like interesting. According to the witness nurse, she was on the floor. She said the nurses on duty giving her CPR when they find out she was not breathing. They put her flat on the bed, no one watching her for several hours. Regardless, she calling for help. They just told her, “We are busy.” And the nurse never came. So by the time the code blue occurred, the nurse supposed to do a CPR on her even laughed at the scene and said, “I forgot how to do.”
Patrik: And what day was that? You mentioned your mom passed away on the 22nd, what day was that when they performed CPR? What day?
Bea: CPR was on the 19th on the floor.
Patrik: I understand. I understand.
Bea: So, I thought it was interesting because this witness later… To just give you a heads up and nothing to do with what I’m telling you. But she had a whistle blow kind of thing attacked by the hospital. These nurses were arranged by the hospital against her in many ways, to harass her. To the point, she had a retaining order and she went to court with these people herself. She had a court order, the court and the restraining order court basically recorded the other people who’re a nurse on duty and they confessed that they forgot how to do the CPR, and they even forgot to put a hardboard under the patient’s bed because hospital bed is soft.
RECOMMENDED:
Bea: You can’t do that, it’s required. He did not do it. She actually accused her, she may not admit, but that was in the court transcript, in the restraining order courts public records. So she, the witness nurse, has a copy. I think she wanted to make sure those are on the record. So that’s why I told you, they’re considering criminal charges on that.
Patrik: Absolutely.
Bea: This is something much more I was anticipated. I didn’t understand, know anything. But, I got a lot of education. Talking to you right now is much more helpful than ever. Because before, I didn’t know what I was talking about.
Patrik: But I can tell you and I don’t want to get sidetracked here, but everything that you’ve said so far, I’m not surprised. I’ve seen this myself. I did what the nurse did in this hospital. I did that in a hospital that I worked at. I didn’t go to court, but I took it as far as I could. And got some of the issues resolved because they knew I was serious that I would take you to the next step. So I’m not surprised by what I’m hearing because I’ve observed similar situations in my clinical practice. So to me, this is shocking, but it’s not new.
Bea: Yeah, I’m telling you. And during that 10 days when she was in the ICU, I was requesting to talk to the social worker because I know they’re trying to abuse her even in the ICU. The excuse letter, even in writings seems to be hating me. They don’t like me because I want to gain a right for my mother to receive proper care.
Patrik: Absolutely.
Bea: It is not a reason to treat my mother badly.
RECOMMENDED:
Patrik: No, no.
Bea: My mother can’t speak for herself.
Patrik: Yep. Absolutely. Absolutely.
Patrik: Yep. Now, before you go on, I just need to mention I need to step outside. So when I go outside it might be a little bit windy. Now if it’s too windy, I will have to call you back. But I will need to go outside, so I’ve got some earplugs. We can definitely continue talking while I’m going outside. But if it’s getting too windy, I will need about an hour and then I would call you right back. But let’s talk for now. But just that you know what I’m doing while we’re talking.
Bea: Alright.
Patrik: Look, it’s, it’s very interesting. However, it’s not new. I’m not surprised. I’m not surprised. Right. Okay, carry on. I’m all here. I’m listening.
Bea: And as I was saying, I need to be the one to speak for my mom and that I know she could have been treated fairly but she had not received any of that treatment because all they are aiming for is for her to be dead, that is how I feel.
RECOMMENDED:
Patrik: Right.
Bea: If only I have known you and seek your help Patrik before all of this happened then I could have changed everything. But I know that there’s still a chance for me to let them know that what they did to my mom is not right and should not be done to any other patients. They have neglected my mother that led to her death. And you know from the story I told you a while ago how it made me think this way.
Patrik: Oh, I know all of them. I know all of them. Right, right. Let me ask you this, so she was in ICU for three days from the 19th until the 22nd, is that correct? So it all happened within three days, is that right?
Bea: Yes. It was unimaginable that within just 3 days, that all happened to my mom.
Patrik: Three days. And you mentioned the code blue. Do you know what led to the code blue, what got her into ICU?
Bea: She was being placed in the ICU because they told her lungs are not good and that they need to put a breathing tube to her to connect her to the ventilator.
Patrik: Okay, but there must be a reason for that. For example, pneumonia. Okay, let me ask you a couple more things. When she was in ICU, did they ever sit down with you, the doctors, did they have a meeting with you?
Bea: Never.
Patrik: Never? Right. What time of the day did your mother pass away? Daytime? Nighttime?
Bea: Daytime.
Patrik: Oh Daytime, okay. Were you there at the time or were you absent?
Bea: Sorry but I can barely hear you.
RECOMMENDED:
Patrik: Oh sorry. What I’ll do is you need to give me about half an hour. You need to give me about half an hour and I’ll call you right back. I’m sorry. I’ll call you right back in about half an hour, three quarters of an hour.
Bea: Ok.
Patrik: I’m sorry. I’ll call you right back. Thanks, thanks. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!