Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
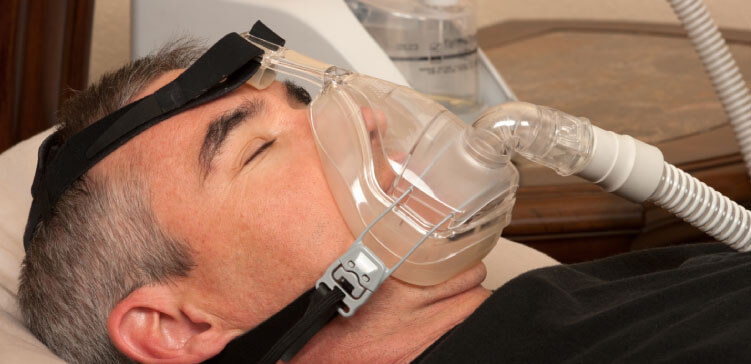
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Larry, as part of my 1:1 consulting and advocacy service! Larry’s girlfriend has a tracheostomy in place and isn’t waking up from an induced coma. He is asking if it is true that mobilizing or stimulating his girlfriend can increase her chances of waking up?
My Girlfriend Isn’t Waking Up from an Induced Coma. Is it True that Mobilizing my Girlfriend Can Increase Her Chances of Waking Up?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Larry here.”
Patrik: That needs to happen. She needs to go into a specialist area. What area is it?
Larry: It’s with all types of patients that might have had a stroke, something like that, but it’s not specific. I was wondering, could she get transferred to another hospital by request or is that something that would be hard?
Patrik: If there are stroke patients in this area, there’s a good chance she is in a neurology ward. You probably have to find out.
Larry: Okay.
Patrik: Okay? If there are stroke patients in this ward, there’s a very high chance she is in a neurology ward. But the next step really is she needs to be simulated and she needs to go onto a rehabilitation ward.
Larry: Okay.
Patrik: Right?
Larry: All right.
Patrik: I’m just trying to think. Is there anything else happening that you think might be sort of playing into the dynamics? Is there a DNR?
Larry: No, there isn’t.
RECOMMENDED:
Patrik: Good. Because that could be… you know, if you were telling me, “Oh, there’s a DNR,” I would say, “Oh, if that’s the case, they probably would give up.”
Larry: Yeah. I get that.
Patrik: Right?
Larry: Yeah. They actually requested DNR a couple of weeks ago. They asked me to check with her family to see if they want to do the DNR and I feel like she made progress even since then. Because she was not moving her legs at all and she was not moving her hands at all when they said that, but she was opening her eyes here and there and they said she had no sleep-wake cycle then. Right after this, she had somewhat they called sleep-wake cycles, and she’s moving her legs a lot.
Patrik: Right. Is she moving hands or arms?
Larry: She’ll swing her arms back and forth and she’ll swing her head back and forth. The neighbour went and saw her and said that she actually cried one time.
Patrik: Right.
Larry: And she made that because she didn’t know what the issue might have been.
Patrik: If she’s crying or if she shows signs of sadness, it’s clear that she might be trapped in her body and she just can’t express herself or the only way she can express herself is by crying, you know?
Larry: Yeah.
Patrik: That’s a sign that her brain might well be working, she’s just not in a position where she can express herself.
Given that she’s off the ventilator, have they tried a speaking valve? Do you know what I mean by that?
Larry: No.
Patrik: Okay. When patients are off the ventilator and they still have a tracheostomy, they should be at least trying on a speaking valve, right? So, patients off the ventilator with a tracheostomy can talk if they have specific speech therapy.
RECOMMENDED:
Larry: Oh, okay.
Patrik: Right? So, you may want to ask them, “Where is speech therapy?” You know, all the allied health professions are missing. Physical therapy is missing because she’s not getting mobilised, right?
Larry: Exactly. Yeah.
Patrik: The speech therapy is missing as well.
Larry: She’s supposed to have been going to a rehab facility, but none of them would take her because of her tracheostomy. So, we were waiting on her to get into a facility, actually, but none of them had actually taken her in.
Patrik: Right.
Larry: Because I went as far as trying to figure out how to get her a stem cell IV or something. I was just coming up with ideas and I couldn’t think of anything that they would allow. They wouldn’t allow someone… I had a guy who could go in. He had wellness and he could bring the stem cells and give her the IV, and they told me that they wouldn’t allow it.
Patrik: Right. Okay. Look, that’s sort of not my area of expertise in terms of stem cells, and I don’t know enough about it to guide you there, but it’s probably worth looking into. But in terms of… you know, the simple things on a day-by-day basis are mobilisation, stimulation. Those are the simple things on a day-by-day basis.
Whereabouts is your girlfriend? Is she in Alabama as well?
Larry: Yeah, she is.
Patrik: Right. I’m not surprised that you can’t find a facility where they take tracheostomy because they don’t exist in Alabama.
Larry: Oh, okay.
Patrik: My understanding is that Alabama doesn’t have what’s being referred to as a long-term acute care facility but that could be a blessing in disguise. I can tell you that much. Because if she can go in the right environment, which would be a rehab, that would be much preferred compared to a specialist facility for tracheostomy. Because all they focus on is the tracheostomy, whereas in your girlfriend’s case I believe they need to focus on rehabilitation.
RECOMMENDED:
Larry: Okay. Yeah.
Patrik: The tracheostomy, it’s not good that it’s there, but I’d say your girlfriend needs to be more alert. Because once she’s more alert, then the tracheostomy will take care of itself, hopefully.
Larry: Yeah.
Patrik: The focus needs to be on stimulation, mobilization. Imagine you’re having an event like your girlfriend, and now she’s basically being bed-bound for two months. Of course she’s not waking up.
Larry: Yeah.
Patrik: Right? There’s no guarantee that she will wake up just because they’re mobilizing her, but the chances will increase.
Larry: I get it.
Patrik: Imagine even if you’re healthy and you would be lying down for two months, you wouldn’t be as sharp mentally as you were as if you’re moving around every day.
Larry: Exactly.
Patrik: You know, it’s easy for them to be negative. It’s very easy for them to say, “Oh, look. She’s not improving.” That’s very easy. They haven’t even tried.
RECOMMENDED:
Larry: Yeah. I mean I know that they have her drugged up to the point where… I mean I know she can pull through. I just really believe that. I’m glad I’m getting your advice as far as hope because I never get any of that like this before.
Patrik: Yeah. Unfortunately, you will need to keep pushing because otherwise, nothing is going to happen.
Larry: Okay.
Patrik: It’s very sad, but at least you know what to do.
Larry: Okay.
Patrik: And it’s really important… I will email you those interviews, those podcasts because it will give you perspective.
Larry: Yeah.
Patrik: It will give you a perspective that other families or other patients have been in a similar situation and that with patience and effort you can get outcomes.
Larry: Yeah. I get it.
Patrik: Now, it’s two months. You said 23rd of December. Is that right?
Larry: Yes.
Patrik: Right. It’s not too late. It’s for two months. Whatever they’re doing at the moment isn’t working but from what you’re sharing I do believe they haven’t put in the effort.
Larry: No.
Patrik: So, you’ve got to keep trying. How often do you see her?
Larry: I come see her twice a week.
Patrik: Do you think she’s responding to you?
Larry: Well, if I say her name, she’ll open her eyes. If I say my name, she’ll open her eyes instantly.
RECOMMENDED:
Patrik: Okay.
Larry: It happened three times already.
Patrik: Good.
Larry: I would just be talking to her, I’ll say who I am, and she’d open her eyes.
Patrik: Yes absolutely. Absolutely. That’s good. So, you can see there’s progress.
Larry: Yes, I can. I just hate the fact that the doctor said that she would have to be long-term because he doesn’t believe that she will recover. That was one other reason why getting into a facility because it was between that and the tracheostomy. But we’re waiting to see, and I will get her sister to try to get them to mobilize her, or even come in more often myself. Are the workers allowed to mobilize her or is this something that has to be approved by the doctor?
Patrik: Not at all. There should be physiotherapy.
Larry: Okay.
Patrik: And they should be instigating it, okay? There will be a day where the physical therapist might be busy or whatever, but the nursing staff should step in.
Larry: Yeah.
Patrik: Look, I’m shocked to hear that. I’m really shocked. It’s very disappointing, you know? I hear it over and over again. I’m talking to people every day unfortunately in similar situations and I’m really shocked to hear what my nursing colleagues aren’t doing. Because, yes, it’s the physiotherapy job but also the nursing staff should be instigating that, too.
Larry: Yeah.
Patrik: It’s very disappointing. Who is in charge of the care from a medical perspective?
RECOMMENDED:
Larry: Her sister.
Patrik: No, I mean the doctor.
Larry: Yes, the doctor.
Patrik: Yeah. But what’s his specialty?
Larry: I’m not sure.
Patrik: You’ve got to find out.
Larry: I will. I will find out and let you know.
Patrik: You need to find out because it could be a pulmonologist, for argument’s sake and what your girlfriend needs is she needs a neurologist at the moment.
Larry: Okay.
Patrik: Right? So, the right specialist needs to guide and potentially even a rehabilitation specialist.
Larry: Yes. Now, as far as the medication, what would I try to get them to lower? Or try to get them to take her off one or two, or…
Patrik: Look, I tell you what could happen. Let’s just say they halve the dose of Dilantin. Let’s just say that for argument’s sake, okay?
Larry: Yeah.
Patrik: There’s a risk that she might have a seizure for that. By the same token, and they might… let’s run through a couple of scenarios. Let’s just say they halve the Dilantin and nothing happens, which would be a sign that she’s over-medicated. But then here is where probably the rubber hits the road, let’s just say they’re having the dose of the Dilantin, and then they start mobilizing her, and then she’s having a seizure.
Larry: Yeah.
Patrik: That’s where it could get tricky. The way I look at this is to let’s mobilize her first, make sure she’s not having any seizures. Once they know it’s safe to mobilise her, then let’s reduce the anti-seizure medication.
Larry: I get it.
Patrik: Right? You don’t want to put the cart before the horse. You want to make sure you’re on the safe side. But the mobilisation, from my perspective, is non-negotiable.
RECOMMENDED:
Larry: Okay.
Patrik: Look, if you’re lying in bed you’re wasting muscles, your brain is not working. She’s getting contractions.
Larry: I get it.
Patrik: She’s getting contractions and hopefully she can walk again one day. But if they don’t mobilize her it will be more difficult for her to do all of that because of the contractions.
Larry: Yeah.
Patrik: I can’t stress this enough, Larry. It’s a non-negotiable. If they’re not mobilising her, they’re lazy. They’re lazy. Lazy and disengaged.
Larry: When people are waiting on a facility, how long will they allow them in the hospitals?
Patrik: Look, it often depends on the insurance.
Larry: Okay.
Patrik: It’s often an insurance issue.
Larry: Okay. Yeah. There was an issue. Then, they said there wasn’t, that the insurance had kicked in. Because she had Medicaid prior but it discontinued. They were handling her Medicaid when she was actually in the ICU, like the first two days. So, I’m not sure if they kicked in there’s an issue. But they did say it was an issue and then they turned around and said that it wasn’t an issue anymore.
Patrik: Right. Look, it can be an insurance issue but then again, from experience, everything is negotiable. I mean the insurance will have an interest in getting your girlfriend better.
Just give me one sec, Larry. Just give me one sec. I’ll be right back.
Larry: Okay.
Patrik: (silence)
Sorry about that, Larry. I’m back now.
Larry: Yeah, that’s fine.
Patrik: It’s often an insurance issue or it can be an insurance issue but your girlfriend is 35. Again, I would be telling you the same if your girlfriend was 45, 55, 65. Age is not a determining factor at all.
Larry: Yeah.
Patrik: If anything, because your girlfriend is so young, I can’t believe they’re not trying.
RECOMMENDED:
Larry: No, they’re not at all.
Patrik: Very disappointing.
Larry: I will get in contact with her sister and try to get that going and I will let you know about the doctor, what his specialty is and go from there.
Patrik: Yeah. Do that. In the meantime, I emailed you the Glasgow Coma Scale because I think it will be important for you to get some idea about that.
Larry: Okay.
Patrik: And I’ll email you a link to this interview of the client that I published last week and as I said, there’s another one coming out on Thursday, so keep an eye on that. Very similar situations, very similar to your girlfriend’s situation and both patients were much older. They were in their 60s.
Larry: Wow.
Patrik: That’s why I’m saying we would be having the same conversation if your girlfriend was above 60, very same conversation. It wouldn’t change the conversation at all.
Larry: Okay. All right. Well, thank you.
Patrik: You’re very welcome.
Larry: Yes.
RECOMMENDED:
Patrik: Yeah. No, I emailed that to you. Have a look and let me know how you go.
Larry: Okay.
Patrik: All your questions answered or did you have anything else?
Larry: Everything is answered.
Patrik: Okay. All right. All the best for now. Keep fighting. Keep fighting.
Larry: All right. Thank you.
Patrik: You’re very welcome. All the best for now, Larry. All the best.
Larry: Okay, thanks.
Patrik: Take care. Bye. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!