Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
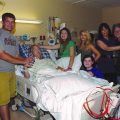
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Larry, as part of my 1:1 consulting and advocacy service! Larry’s girlfriend is critically ill in ICU with seizures and in an induced coma. Larry is asking what makes it unpredictable for his girlfriend to wake up from an induced coma?
My Girlfriend is Critically Ill in ICU with Seizures. What Makes it Unpredictable for Her to Wake Up From An Induced Coma?
Larry: Hello?
Patrik: Hi. Is this Larry, Larry?
Larry: Yeah, this is Larry Web.
Patrik: Hi, it’s Patrik, here, from Intensive Care Hotline. How are you?
Larry: Pretty good. How are you? I’m doing pretty good.
Patrik: Right. We’ve got 15-minute call scheduled now.
Larry: Yes.
Patrik: You were expecting this?
Larry: Yes.
Patrik: Yeah, that’s great. Just quickly before we start, we’ve got about 15 minutes. We’ll start. I’ll start listening to obviously what your situation is, and then I can advise you how I can help you. Beyond the 15 minutes, I do have paid consulting and advocacy options as well.
Larry: Okay. I can make a payment now. It probably would even take longer than 15 minutes. I’m not sure. But I would rather make a payment right now.
Patrik: Okay. Yeah. You can. You can. And then we’ve got plenty of time.
RECOMMENDED:
Larry: Yeah.
Patrik: Yeah, go on.
Larry: Oh, go ahead? I would like to do the hour option for one reason: I just really had a question until I talk to her family because they have … She was my girlfriend, but they have the control on her. They have I guess they have the say-so on whether or not to go forward or to pull the plug or whatever. But I just had a question for myself. And I don’t mind paying for the hour just. . .
Patrik: No, that’s fine.
Larry: … for these questions.
Patrik: Yeah, no, that’s fine. What I’ll do, Larry is I will send you the link for the hour right now. Just give me one sec, please. And you have access to your email? Larry, do you have access to your email at the moment?
Larry: Yes, I do.
Patrik: So what I’ll do is I’m just sending this to you now. You should have it.
Larry: Yes.
Patrik: So it should come through any second. It should’ve come through by now already. Can you have a look? Is it coming through?
Larry: It’s still loading.
Patrik: Okay. That’s all right. That’s fine.
Larry: No, I didn’t see it there yet.
Patrik: Okay. That’s all right. It’s certainly gone out on my end. Let’s try again just in case. I would just like to send it again just in case.
Larry: Alright.
Patrik: Got it?
Larry: Yeah.
Patrik: So all you need to do, Larry, is you need to click on the link. And then you enter your email address. And then you follow the steps. It’s fairly simple.
Larry: Right now she’s been in there for about seven or eight days. Well, no. She’s been in there for since the 23rd of December.
Patrik: 23rd of December.
Larry: 23rd of December, yeah. And the problem that we were facing was that they were giving us bad news but lately, they’ve been trying to give better news. But she’s not brain dead but she’s in an induced coma. And I was just trying to figure out, is it even possible after they lower the medication, it’s gonna be all right.
RECOMMENDED:
Patrik: Why did you go in there in the first place? Tell me a little bit more why?
Larry: She had a seizure and it went to a cardiac arrest.
Patrik: Right. Okay. And this is your girlfriend, did you say?
Larry: I’m sorry, I couldn’t hear you.
Patrik: You are talking about your girlfriend.
Larry: Yes.
Patrik: So she had the seizure. She has cardiac arrest. So do you know whether there has been any downtime? Do you know what I mean by downtime?
Larry: No. Oh yeah. I did CPR on her for, I’m not sure, the first two minutes that it happened, from as soon as she fell, I was doing chest compressions. And the ambulance took 10 minutes to get there.
Patrik: So you were the first responder.
Larry: Yes.
Patrik: Right. Oh my goodness. Okay. Have they given you a time potentially in minutes how long there was an insufficient supply of oxygen to the brain? Have they given you an estimate of that?
Larry: No, they haven’t.
Patrik: Okay.
Larry: They just told me that they had her pulse, I think in 20 minutes. They put oxygen on her within the first 10 or 11 minutes. They was trying to shock her. But that was the issue.
RECOMMENDED:
Patrik: Yes, I can imagine. Yes, I can imagine. So I’ll give you an example, so you will understand why I’m asking this question, how much downtime has there been. So in clinical terms, it’s often being referred to as downtime. So with that downtime, what that means is when you have somebody with the cardiac arrest and they’re not getting oxygen to the brain and the longer there is no oxygen to the brain, the higher the chances are that there is irreversible brain damage. Now, the cut of time for that is usually three minutes. So if somebody’s brain doesn’t get oxygen for more than three minutes, there is supposedly irreversible brain damage. Okay?
Larry: Okay. Yeah.
Patrik: And did you know? Were you aware of that, or is that new information?
Larry: Yes. I was aware of it. I was just told that chest compressions help a little bit. And I wasn’t sure. They said she’s not brain dead. They actually did an MRI and said that there was some type of damage but not to where she couldn’t come back from.
Patrik: Oh, okay.
Larry: But then there also was a radiologist who said that it was too much damage. So the doctor went against what the radiologist said. But I was just wondering, after they’re sedated and to induce the coma, how long does it usually take for them to gain consciousness?
Patrik: That’s a very good question, Larry. Do you know whether she’s still sedated?
Larry: Yeah. She is.
Patrik: And what do you know-
Larry: Oh, go ahead.
Patrik: Do you know what she’s sedated with?
Larry: Propofol and fentanyl. They have her on a lot of medications. And they said that when they try to lower the medications, she has like light seizures.
Patrik: Yes. That would be-
Larry: So they’ve taking a long time to lower it.
Patrik: Yes. I’m not surprised at all. And I’m telling you why. So basically what happens is when … And we’re moving away from the categories for a moment just to talk about the mechanics of how that works with seizures. So are you okay if we move away from the cardiac arrest for a moment, or do you want to stay on the cardiac arrest issue and understand that before we move on to this sedation and waking up issue?
Larry: Yeah, we can go whatever direction.
Patrik: Okay. So we can talk about the cardiac arrest and the not getting oxygen to the brain later if you like. Am I making sense here? We’re moving away from that because there are two separate issues.
Larry: Oh, I get what you’re saying.
Patrik: So the not waking up part, and giving sedation, and potentially having seizures is not directly related to what happened during the cardiac arrest and potentially not getting oxygen to the brain.
Larry: Yes.
Patrik: So I’m moving away from that. So what happens is when somebody goes into an induced coma, okay, they’re always on a ventilator, as you would’ve seen. So there’s actually no other reason for people to go into an induced coma than the critical illness that goes hand-in-hand with mechanical ventilation and the breathing tube.
Patrik: When somebody has a breathing tube, it’s really uncomfortable, really uncomfortable. So they have to be sedated. On top of that, you would also sedate a patient who’s in a critical condition just to sort of lower everything down and making the body work minimally so they can recover from that critical illness.
RECOMMENDED:
Patrik: And could be for many situations. It could be for somebody going for cardiac surgery. It could be for somebody going for back surgery. It could be all sorts of situations. The added-on complexity for anybody with a neurological condition, which could be a brain injury, which could be lack of oxygen to the brain, which could be seizures, of course, like in your situation or your girlfriend’s situation seemed to happen, is that waking up is very unpredictable.
Patrik: And waking up can be very unpredictable even for patients without the brain injury, without seizure. So the induced coma is all great in theory. But the waking up part is very unpredictable for any patient often whether with or without brain damage because there are so many chemicals going in during an induce coma, it plays havoc with the brain.
Patrik: So then you’ve got the added-on complexity of the seizures and potentially a hypoxic brain injury. A hypoxic brain injury, what I mean by that is potential there has been insufficient oxygen supply to the brain during the cardiac arrest that’s causing potentially irreversible brain damage.
Patrik: So those are the mechanics here that are important to understand because it’s adding on complexity to your girlfriend’s situation. So when you then wake somebody up, and they haven’t got the seizures under control, they have to put them back in the induced coma. Why? And that sounds to me like has happened.
Larry: Yes, that’s exactly what happened.
Patrik: And I’ve seen it many, many times. So when that happens, the first thing they need to do is they need to get the seizures under control. Now, you said your girlfriend went into ICU on the 23rd of December. Today is the 4th of January. So we’re talking about 12 days, 12 days. Look, it’s the concern that they haven’t got the seizures under control within 12 days. That’s a concern.
RECOMMENDED:
Patrik: Propofol and fentanyl, okay, I have no problem there, but my question is what are they giving to control the seizures? Do you know what they’re giving to control the seizure?
Larry: I’m not sure. I’m not sure yet.
Patrik: You need to find out. You need to find out. I’ll give you some names for drugs that are probably drugs they’re using for seizure control. One would be phenytoin. Have you heard of that?
Larry: Yes.
Patrik: Right. So they would potentially give phenytoin. Phenytoin is also known as Dilantin. So it’s got the brand name and the generic name, phenytoin or Dilantin. And the other drug they’re potentially giving is Keppra. Have you heard of Keppra?
Larry: Hello?
Patrik: Yes. Are you there? I can hear you.
Larry: Yes. Okay. Yes.
Patrik: Have you heard of Keppra?
Larry: Yes.
Patrik: So they are the two drugs of choice, especially when it comes to sort of acute seizure onset in a situation like that. They would potentially be giving one or both of those drugs regularly. But it may not be sufficient to control the seizures. Here is, then, the next problem, Larry. So they might be giving the phenytoin, and they might be giving the Keppra, either both or one only. The problem is that those drugs have sedative effects. They have sedative effects themselves.
Patrik: So you’ve got the added-on complexity with, you’ve got the complex situation with an induced coma. You’re getting propofol. You’re given phenytoin. And then you’ve got the background issue with the seizures. You’re trying to control the seizures. You’re trying to wake somebody up, and yet they’re still seizing even though they’ve been given the Keppra and the phenytoin. There may be other drugs in the mix as well, something like sodium valproate, potentially clobazam. There’s other anti-seizure drugs as well, but the mainstream ones are Keppra and phenytoin.
RECOMMENDED:
Larry: Okay.
Patrik: Okay? So you’re following so far.
Larry: Yeah.
Patrik: Okay. So then you see, the good thing that I can see in this situation is something like propofol is short-acting. So what does that mean? When you put somebody on propofol, they get knocked out very quickly, okay? And when you stop propofol, often patients wake up quickly too. So from that perspective, I like the propofol because the propofol is a good indicator in terms of can she wake up quickly? How is she responding?
Patrik: So I like that, that they’re giving the propofol because it’s just a better drug to work in a situation like that. There is a little bit of a drawback with the propofol. Have you heard of midazolam or Versed? Have you heard of that drug?
Larry: No, I haven’t.
Patrik: No, that’s okay. Then we won’t go there. That’s okay. If you haven’t heard of it, then there’s a good chance they haven’t even given it to her. And that’s fine. She probably doesn’t need it at the moment. Have they mentioned a tracheostomy as an option? Do you know what I mean with a tracheostomy?
Larry: A hole in the neck?
Patrik: Yes.
Larry: Yeah. They actually, for some reason, they put it in there saying that the other things can cause an infection over time.
Patrik: Oh, so they’ve already done a tracheostomy.
Larry: Yes.
Patrik: When was that?
Larry: It might’ve been four night ago.
Patrik: Okay. And can I just ask on that, are you the decision-maker? Are you the medical power of attorney for your girlfriend?
Larry: No, I’m not.
Patrik: Well, that’s okay. So somebody within the family would’ve given consent.
Larry: Yes. Okay. Yeah, because I asked her about it when I saw it, and she told me, “Oh yeah, they said that something about it can cause an infection with this tube in her throat for that long.”
Patrik: Okay. Well, I give you my thoughts on the tracheostomy. There’s a couple of things there. Number one, yes, they are right. The breathing tube in the throat would cause an infection in the long run, right? I agree with that, seen it many times. That’s one thing. Number two is, if your girlfriend didn’t have seizures and she could wake up normally, and she couldn’t come off the ventilator, then a tracheostomy would make perfect sense. And the reason for that is when somebody has a tracheostomy, you can switch off sedation immediately because it’s so much more comfortable.
RECOMMENDED:
Patrik: But with the added-on complexity of the seizures, you can’t switch off sedation because if they do that, she’s having a seizure. So that’s the added-on complexity. The good news about the tracheostomy is it buys your girlfriend time. If a tracheostomy is doing anything, it’s buying time for patients. And most of the time, that’s a good thing. It’s buying time so that patient can come off the ventilator in their own time.
Larry: Okay, I get it.
Patrik: Right. So I don’t have a problem with the tracheostomy at this point in time with the information that you’ve shared. Who is the primary decision-maker on the medical level? Is it an intensive care doctor? Is it the neurologist? Do you know who’s sort of driving all of this
Larry: No. I’m not sure.
Patrik: Okay, okay. .
Larry: I’m…
Patrik: Go on.
Larry: I know that her sister is making the decisions and working with the person, I guess maybe talking to the doctor or the neurologist. They gave me some information but not as much. But me and the sister are, we’re on good terms. She’s willing to go as far as possible to make sure she’s okay.
RECOMMENDED:
Patrik: Yeah. How old is your girlfriend, if I may ask?
Larry: 35.
Patrik: 35. Okay. I mean, generally speaking, you could argue that the younger patients, that the higher the chances for recovery. At the same token, I’ve seen over the years I’ve seen all sorts of things. I’ve seen patients recover at a young age. I’ve seen patients not recover at a young age. I’ve seen patients recover at an old age. You know, no hard, fast rules. But I think it’s fair to say that the younger, the higher chance is for recovery, of course. So I’m glad, and also what I can also read between the lines here, Larry is when, because they’ve done a tracheostomy, they must think that their hope for recovery.
Larry: I hope so.
Patrik: What happens often is if they think there is no chance of recovery, they wouldn’t even bring up the tracheostomy. Rather than telling you or your family, “We should do a tracheostomy,” they would say, “We should stop treatment.”
RECOMMENDED:
Larry: Okay. Now I understand.
Patrik: Right. So to a degree I’m glad they found the tracheostomy.
Larry: Okay.
Patrik: Right? Because that’s a good sign.
Larry: All right.
Patrik: Okay. What is important now, however, is they need to start controlling the seizures.
Larry: Yes. And I will find out what seizure medication she was taking. And I don’t mind calling you back again. But I’m curious, the main problem that I was worried about was when I noticed the thing in her neck, I didn’t know how to take it. I didn’t know if she’s getting worse or what. And then they explained it to me. But sometimes the way they explained it, it sounded like they were just talking negative or talking in a language I didn’t understand. So yeah.
Patrik: Right. I think it’s probably the latter, that they talked in a language that you didn’t understand. The other good thing about a tracheostomy is, for example, last week when your girlfriend was still having a breathing tube, there’s a high chance she needed more sedation than she does now. It’s a high chance for that, not guaranteed but a high chance because a tracheostomy is just easier to tolerate. Right?
Larry: Yeah.
Patrik: I tell you, there’s a couple of things that are important. When somebody has a tracheostomy, there is a risk that once your girlfriend is off sedation and they can manage the seizures, that she will end up going to LTAC. Have you heard of LTAC? Do you know what I mean by that?
Larry: No.
Patrik: LTAC stands for Long-Term Acute Care Facility, sort of a step down from ICU for ventilated patients.
RECOMMENDED:
Larry: Oh, okay.
Patrik: Okay? I am not in favour of those LTACs. I think they’re horrible. But as long as she’s on the sedation, she’s not a candidate for LTAC. But I’ll tell you what could happen. If they can wean her off sedation and they can control the seizures, she might be a candidate for LTAC.
Larry: Oh, okay.
Patrik: Okay? And that’s a bit of a risk, and I’ll tell you why. Let’s look at the best-case scenario at the moment, okay? The best-case scenario is they can take her off sedation. They can control the seizures, right?
Larry: Yeah.
Patrik: And then she would need to go on to neurorehab. Are you following there?
Larry: Yeah.
Patrik: She would need to go to neurorehab. The problem is ICUs don’t do neurorehab, obviously. The LTACs are often not specialised for neurorehab either. The LTACs are mainly specialised for ventilator weaning. And that could become part of it, depending on how your girlfriend goes in being weaned off the ventilator. But after a brain injury, the focus needs to be on a neurological rehab.
Larry: Yes. Understand.
Patrik: So they haven’t mentioned LTAC as far as you’re aware?
Larry: No, they haven’t.
Patrik: Now, that’s good. I think it’s good. And the reason I say it’s good is I have seen way too many patients being pushed out of ICU prematurely because they needed the beds. It’s cheaper for the insurances to go to LTAC. It’s all of that. So you got to definitely be vigilant around that.
RECOMMENDED:
Larry: Okay. I understand.
Patrik: You have to be very vigilant around that. So the other thing that’s probably important to know is do you know how your girlfriend is breathing? And what do I mean by that? Do you know whether she’s taking some breaths herself already?
Larry: I’m not sure. I haven’t heard anything, but I’m definitely not 100% sure about it prior to or anything like that.
Patrik: Are you there every day? Do you see her every day? What’s your sort of involvement?
Larry: I see her like every three days I go in there. She has a lot of family that comes to see her. And I just come by every few days, but I call every day to check on her, on her blood pressure and stuff like that.
Patrik: Talking about blood pressure, do you know anything there? Do you know, is her blood pressure stable? Do you know that?
Larry: Yeah, it’s been stable the entire time.
Patrik: Okay. Do you know whether she’s been on inotropes or vasopressor? Do you know what I mean by that?
Larry: No.
Patrik: Okay, let me quickly go there. So, again, I think it’s important that you understand the sort of the bigger picture. When somebody has a cardiac arrest, they most of the time end up on inotropes or vasopressors. Now, I don’t want to confuse you with too many medical terms, but it is important to understand when somebody has a cardiac arrest, their blood pressure plummets. They often have a blood pressure that goes very low that’s not compatible with life.
Larry: Okay. I see.
Patrik: In order to reverse that, emergency crews, ICUs, emergency rooms, and so forth, they use drugs called inotropes or vasopressors such as adrenaline, Levophed, norepinephrine. Again, I don’t want to get too medical here, but it’s important for you to understand. Now, those are life-saving drugs, especially during cardiac arrest. A lot of patients in ICU after cardiac arrest stay on those drugs for quite some time to help the heart go back to a normal function.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: So what I’ll do is when we come off this call, I will send you an email with some drug names. I think it’s important that you get a little bit of an idea there because the reality also is that if your girlfriend is still on those inotropes or vasopressors, she’s also not a candidate for LTAC. Right?
Larry: Okay.
Patrik: So the devil in those situations is often in the detail.
Larry: Yeah. I get what you’re saying.
Patrik: Right? It’s often in the detail. I’ll give you another quick example so you can understand. Again, when we come off this call, I will also send you some links to another case study where we worked with a client a while back that was fairly similar to yours. The only difference was that the gentleman who was the patient in the ICU was a lot older. He was sort of early 70s of a similar situation: cardiac arrest, seizure, brain injury, tracheostomy. And they were pushing in the end to send this person to LTAC. And we successfully avoided that. You can learn from that case study. I will send you the links to that so you can have a read, because you’ve never seen this before. It gives you a better understanding of what else could happen and how do you help your girlfriend and so forth. So I will do that. What other question do you have?
Larry: So you answered everything that I didn’t know some things. So we went over everything. I will find out about the medication, more about what medication she’s on.
Patrik: Yes, please. I think that’s going to be really important that you give me a list of medications. I think that’s really important. And then we can look at how far away are they from getting her out of the coma and controlling the seizures because both needs to happen. In order to get her out of the induced coma, they need to be able to control the seizure.
Larry: Yeah. That’s what I’m hearing. That’s what I’m hearing.
RECOMMENDED:
Patrik: And what we can do, Larry, you’ve got another half an hour. If you want to, we can stop here now, and then you can get more information. Then we could spend another half an hour. It’s up to you.
Larry: Yeah. I mean, I appreciate it a lot. What I’ll do is I’ll get that information, and then I’ll see another doctor. I didn’t know if her condition was getting worse. But the nurse, there’s one nurse who spoke as if she would be fine, and she believes that she will be fine. But I guess maybe I didn’t understand the first nurse. But that’s just a big thing with me. I didn’t understand that briefing.
Patrik: Yeah, Absolutely.
Larry: It threw me off. But being that it’s necessary and it’s not a bad thing, then I’m all for it.
Patrik: Yeah. Good. So what I’ll do, Larry, give me about an hour, and I will send you some questions in order for you to find out. And once you’ve got some answers to those questions, please get back to me, and then we can spend another half an hour. And I will also send you a link to a case study so you can have a bit of a read there, and actually a long case study. I think we worked with this guy for a long time. It was broken down probably into 15 case studies, but I’ll send you all of the links. So it was fairly long. But it’s also a good one for people to understand what needs to happen, how can you help as family or a partner. Whatever the case may be, there’s some good information in there.
Larry: Okay. All right. Thank you.
Patrik: You’re very welcome. As I say, give me about an hour. I’m just a bit busy at the moment. I will email you some information. And then you let me know when you want to get on the phone again. You’ve got at least another half an hour.
Larry: All right. Thank you.
Patrik: Okay. Thank you. All the best for now. Stay positive.
Larry: Take care.
Patrik: Thank you. Bye bye. Take care. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!