Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM’’’ where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another frequently asked question our readers and the question in the last episode was
You can check out last week’s question by clicking on the link here.
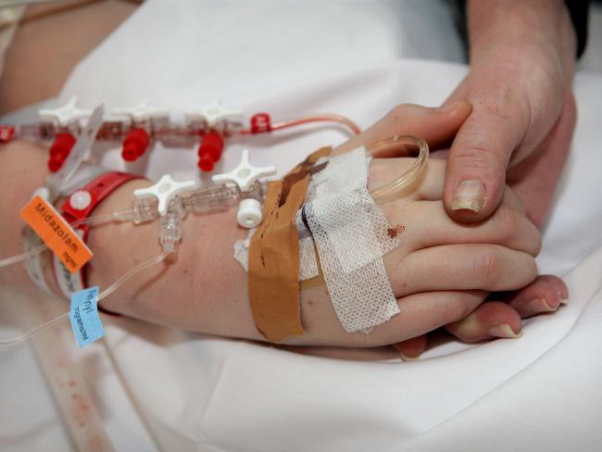
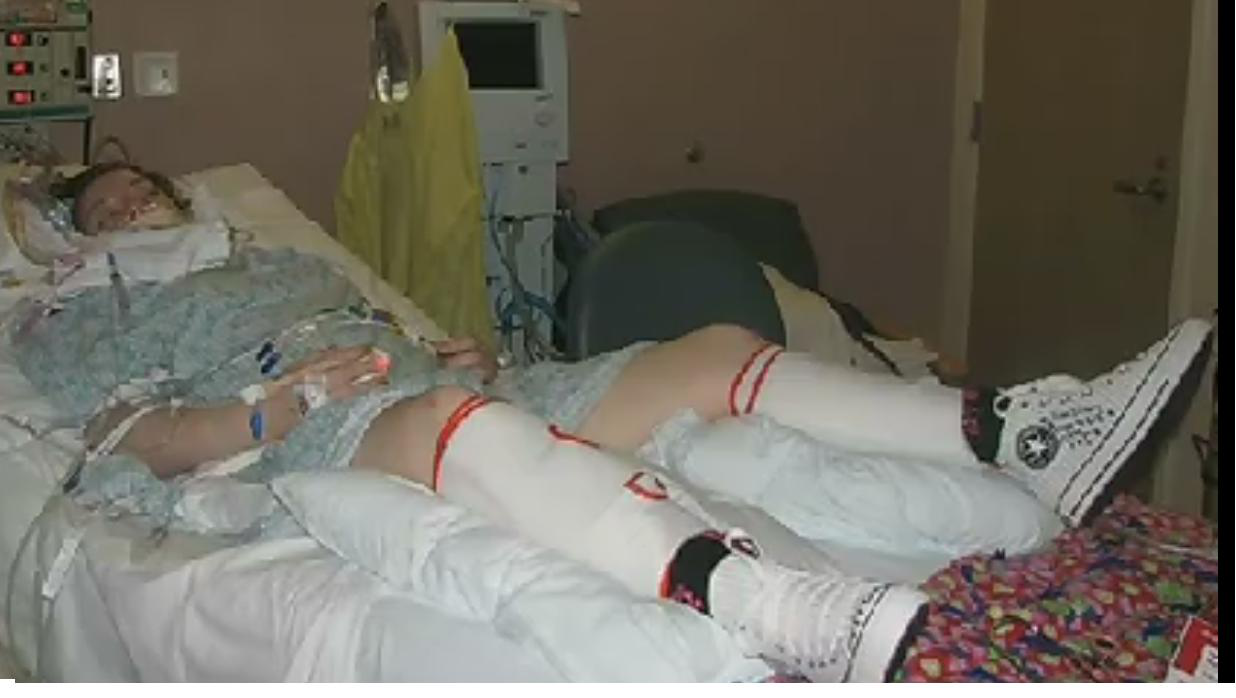
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Sheralee who has her daughter transferred in the Intensive Care due severe brain injury leading to alteration in mental function and state that needs to undergo tracheostomy.
Seems like the ICU doctors want to put my daughter to DNR! Can they do that without my consent?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Sheralee here.”
Sheralee: Probably, yeah. Probably. I don’t think she’s on anything anymore.
Patrik: Yep good, good. But what I’m saying is the Fentanyl or the Morphine are long acting so that means even though Propofol is short acting, if she had Morphine or Fentanyl, that might still be hanging around, and it might stop her from waking up as much as she can at this point in time.
Sheralee: It wouldn’t have been in the last five days or so.
Patrik: Okay, okay. So yeah, so then, I’d say five days if her kidneys are working, she should slowly wake up. She should. But then that is dependent obviously on what’s going on in the brain.
Sheralee: Yes. I’m positive.
Patrik: But at the same time, she will need time, and by time I mean I’m sure, it sounds to me like you’re already clear in your mind that she will need time, she will probably need some rehabilitation.
Sheralee: Yes, I am understanding that and I’m just not, I feel like, I mean, they make it quite obvious that they are writing her off and I’m not ready to write her off.
Patrik: Yeah. Yeah. It does sound to me like you are doing all the right things in terms of how you interact with them, and that’s what you’ve gotta continue doing. You know. You’ve just gotta be very clear on what you want and keep telling them, you know.
RELATED ARTICLES:
Sheralee: Yeah.
Patrik: And the minute it comes to DNR (Do not resuscitate) or NFR (not for resuscitation), you gotta be very careful because I can tell you what’s happening across all hospitals in Australia and in other countries too. If they think it’s “in the best interest” for your daughter to have an NFR or a DNR, they will just put it in the file and won’t even tell you about it. That’s what happening.
Sheralee: Can they do it without me signing it?
Patrik: They can’t, legally, they can’t. And they also have to abide to their hospital policies. But nine times out of ten, they simply don’t.
Sheralee: Mm-hmm (affirmative)
Patrik: And you’ve just gotta be mindful of that and you gotta keep asking them. What we tend to do, you know, and I can tell you we have had some clients in the past where here in Melbourne, or in Brisbane as well, we have dragged the hospital to court, because we know where to look for what they’re doing and what they’re not doing to get the evidence that they’ve basically signed an NFR without informing the family, let alone family consent.
Sheralee: Right.
Patrik: Right. The other thing you’ve got to keep in mind in Queensland, is the law is actually on your side. What I mean by that is, so here in Victoria or in New South Wales, the hospitals have a lot of power in terms of when it comes to end of life decision making. In Queensland, the law is actually on your side, where you have 50/50 say. They won’t tell you about that. But the law is more in your favor compared to other states.
RELATED INFORMATION:
Sheralee: Okay.
Patrik: So what we can do from our end, there is a number of things I would strongly urge you to sign up for our free newsletter, if you haven’t done so already.
Sheralee: I have done already.
Patrik: Right. Right.
Sheralee: I bought your pack on brain injuries, but it doesn’t really, it’s not really talking about hypoxic, but I will finish reading through.
Patrik: Yeah. Sure. It might not talk about hypoxic, but you gotta keep in mind, anything that’s related to the brain, whether it’s a traumatic brain injury, whether it’s a stroke, that’s all hypoxic.
Sheralee: Yeah, okay.
Patrik: That’s all hypoxic, right?
Sheralee: Okay.
Patrik: The mechanism is different in your daughter’s situation.
Sheralee: Yeah.
Patrik: Right? The mechanism has been caused by a different, you know, has been different from the outset. But in terms of the result, it’s the same, whether somebody’s banging their head in a car accident or falling off a roof, it’s still cause of hypoxia.
Sheralee: Yeah.
Patrik: Right? Therefore, therefore, the result is the same as with a stroke. Whether it’s a bleeding stroke, or a hypoxic stroke, the result is the same. Areas of the brain are not being.
Sheralee: Deprived of oxygen. Yeah.
RELATED INFORMATION:
Patrik: Because you are a client, part of what I can do from my end you know, part of the 1:1 consulting and advocacy is to also speak with the doctors and nurses directly if you want us to. We could also participate in family meetings over the phone if you want me to. Your biggest challenge is that you don’t know what you don’t know!
Sheralee: Okay.
Patrik: Right. The other thing that I wanna mention on this note is if your daughter for whatever reason ends up with a tracheostomy and needs home care down the line, you know, we’re also offering a service Intensive Care at Home, that’s home-care nursing.
Recommended:
Sheralee: One question. They’re sort of saying not to, we’ve gotta do something about it, she can’t keep the breathing tube in for much longer they said. She’s coming up to the two weeks now. The question I’ve got is, they’re saying, they haven’t really said it clearly, but basically what they’re doing is they really feel that we should just take the breathing tube out and let nature take it’s course. That’s what they’re saying.
Patrik: Mm-hmm (affirmative) Yup. Of course that’s what they’re saying.
Sheralee: So, I mean my family I sort of yay, you know, she’s breathing on her own, but after last night, knowing she’s has a couple of apneic episodes, she has a chest infection at the moment.
Patrik: Oh, okay.
Sheralee: So, they’ve just done more blood cultures and everything. She had a spike fever of 39.5 I think it was. She keeps getting fevers, and I mean I think it’s a mixture of infection and the fact her brain’s just not regulating her temperature.
Patrik: Yeah, very much so. Probably a combination. If she’s been ventilated now for 12 days, there’s a very good chance she has a ventilator-associated pneumonia, right.
RELATED ARTICLE:
Sheralee: Yup.
Patrik: And, you’re absolutely right that with a brain injury that they have difficulties of regulating their temperature. There is no question around that.
Sheralee: Yeah.
Patrik: And you’ve identified that correctly already that in a 7 bed or 8 bed ICU they have a bed lock issue, you know, and that’s why they will keep referring to taking the breathing tube out and letting nature take it’s course. You have to spell it out to them. Don’t be afraid of telling them, look, you guys have a bed problem and you’re working on that, and you’re not working on what I believe is best for my daughter. You gotta spell it out to them.
Sheralee: Yeah, okay.
Patrik: Who is the Intensivist in charge there, do you know?
Sheralee: They change consultants every week. So it’s not the same one every week. The one we got this week, is less positive than the last week. But then we are a week further on, so, it’s hard to know so the further on, you’d think all of them would be more positive.
Patrik: Yeah.
RELATED ARTICLE:
Sheralee: This one is sort of more that way. The other one was, he didn’t even say if we had options. He was sort of unsure if we had to do a trach. So, I’m sort of, my family really, we had a vote the other night. I have a big family. She’s one of ten children.
Patrik: Right.
Sheralee: So and she’s the second youngest, so most of the old ones of course have an input, and I’m a sole parent so basically my kids. So really, five of them actually, and there were a few partners in there, but five people said that they felt that we should just not do a tracheostomy, and no one gave an opinion about anything more. Most people just withheld their opinion.
Patrik: Yeah. How old is your daughter?
Sheralee: She’s 19.
Patrik: Oh my goodness.
Sheralee: She’s so young.
RECOMMENDED:
Patrik: Yep, very young. Look, I believe you as her mother, you should follow your gut, and I am sure your kids to a degree do as well. What I can tell you is that, my basic experiences with brain injuries of any sort have been time. And by that, I mean give her time.
Sheralee: And she’s not gonna get time if we don’t do a tracheostomy.
Patrik: That’s right. That’s right. You know they don’t want to give her time, and a tracheostomy would buy her time.
Sheralee: Yeah. That’s what I feel.
Patrik: Right. And the reality is if she stops breathing, one way or another, she will stop breathing with a tracheostomy too. And if you still feel down the line, let nature take it’s course, you can still do that.
Sheralee: Yeah.
Patrik: You know. There’s no rush. As long as she’s not suffering, you know.
Sheralee: She’s not suffering.
Patrik: Right. Right.
Sheralee: I mean, we know when she is in pain, because she does grimace.
Patrik: Yeah.
Sheralee: She’s not grimacing unless she’s being hurt.
Patrik: Yeah. Mm-hmm (affirmative)
RECOMMENDED ARTICLES:
Sheralee: And, I don’t know whether you understand this, but I am a Christian and I know that she is still there. I just know it. I feel very strongly that God is telling me she’s still there and she’s coming back. It’s very hard to deal with the negativity, but I’ve just gotta keep holding onto that.
Patrik: Yes, yes, and you’ve gotta, you’ve gotta almost get immune to that negativity. And look, I’m not, I wouldn’t call myself a Christian, but after working in ICU for 20 years, I certainly do believe in a higher authority, and I strongly believe that people should follow their gut, right.
Sheralee: Yeah.
Patrik: Right. You’re her mother. You know her. You know. You know her.
Sheralee: Sorry I’ve just got someone here as well.
Patrik: No, no that’s fine. Look, I’ve gotta go too. I’ll send you, I’ll send you, you’re aren’t you.
RECOMMENDED:
Sheralee: Yes I am.
Patrik: No no that’s fine. I’ll send you the links to our options if you want to.
Sheralee: Yup.
Patrik: You know, you can take it from there. You’ve got my number? Have you got my number? Yeah, in the email I will send you my number.
Sheralee: Okay. Thank you so much.
Patrik: You’re most welcome. All the best.
Sheralee: Thank you. Bye.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!