Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from “INTENSIVECAREHOTLINE.COM’’ where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in last week’s episode was
My Dad Is Part Of Medical Research In ICU, Can It Cause Harm In Life Threatening Situations?
You can check out last week’s question by clicking on the link here.
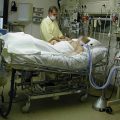
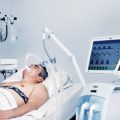
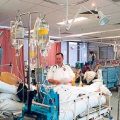
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer the next questions from one my clients Natasha stating that his Dad died in the ICU because of hospital acquired infection and not because of the aspiration pneumonia why he was being admitted initially.
My Dad in ICU hasn’t been treated properly and had hospital acquired infections! Did he die because of it?
“You can also check out previous 1:1 consulting and advocacy sessions with me and here.”
Natasha: Hello?
Patrik: Hi, Natasha. It’s Patrik. How are you?
Natasha: I’m okay. I could be better. How are you?
Patrik: I’m very well, thank you. I’m very well.
Natasha: Can you hear me?
Patrik: I can hear you fine. Can you hear me?
Natasha: Can you say something again? How are you doing?
RECOMMENDED:
Patrik: I’m very well. Can you hear me?
Natasha: Okay. Okay, now I can hear you. I can hear you now.
Patrik: Okay, I think I had my finger on the microphone. I think that’s what’s happened.
Natasha: Um …
Patrik: Yeah, go on. What did you want to say?
Natasha: Yeah, these are a lot of documents. I’ve gotten to page 700 already, out of 1189. The more and more I read, and I’ve been getting some feedback … You know my sister, she’s a rheumatologist, so I’ve been running important things by her, getting her feedback. I also sent it to her to ask her some stuff. She’s looking through it slowly, just because she works. But really, I’m finding out more and more things, and it does seem — I’m gonna tell you this, Patrik — that my dad died because of hospital-acquired infections and not the original reason of aspiration pneumonia that he came in for.
Patrik: Right. What-
Natasha: Let me tell you what else happened. Let me just tell you something new. The microbiology report, okay? My dad died April 8th. April 9th is when the culture from the … What is it? We had a culture done … The Gram-negative bacterium was in his blood. So, they did a blood venous. It says here the colonization date 4/6, 4/6, there was two taken from the blood venous and on 4/7 there was taken a trach aspirate, like a sputum sample. On 4/1, 4/1, 3/31 they did it also then. They took it from the urine catheter — nothing, nothing.
So let me just tell you something. Let me just tell you what the file result was. On 4/9 … I don’t know how to explain it … Hold on, let’s see … He had the Pseudomonas, the trach thingy whatever, the sputum came back as Pseudomonas and the blood venous. But they also found another on 4/12 from the 4/6 sample. They found on 4/12 Candida glabrata also in the blood venous. It says budding yeast but then it says the urine culture … The collection date was 4/1 but on 4/1, they said that there was “many budding yeast”. My sister said that they should have been giving him anti-fungal medicine on 4/1 when they saw … Whatever it was — 4/1, 4/2 … I made a print screen. I did a screen shot of it, the results. She said that when they saw the budding yeasts, they should have started giving them the anti-fungal medication, but that was also in his blood. The Pseudomonas and the Candida glabrata. Those are both most likely hospital-acquired infections.
RECOMMENDED INFO:
Patrik: Yeah, it could be. I wouldn’t rule out..
Natasha: Nursing home.
Patrik: Hospital, could be. But it could also be nursing home related.
Natasha: Nursing home. Yeah because right when he was admitted, so …
Patrik: Yeah, yeah, either or.
Natasha: Yeah, 4/1, duh. Okay, right.
Patrik: And definitely, I agree. As soon as they see yeast, they should be using anti-fungals. No doubt about that. And they haven’t?
Natasha: It’s flucozoid Or something?
Patrik: Yeah, Fluconazole.
Natasha: Is that an anti-fungal?
Patrik: Fluconazole?
Natasha: I don’t know if I read that online or if it was in his chart. I don’t think they used that, though.
Patrik: Okay.
Natasha: You know I’ve been reading a lot of medical research, so I’m not sure if I just read it and … I’m not sure if I just read it and then I’m like, “Oh, did I read it in his chart?” No, I think I read it online. Is that what they would use? Or no?
Patrik: Oh, they should. Anti-fungal Fluconazole is probably the most widely used anti-fungal. There’s a few others but Fluconazole is the most widely used anti-fungal medication. What else did he have-
Natasha: He also had, on 4/7, they also noticed a few Gram-positive cocci. C-O-C-C-I?
Patrik: C-O-C-C-I … Oh, cocci, yeah.
Natasha: Doesn’t that cause staph or steph infection?
Patrik: Yeah, would be something. Absolutely. What other antibiotics was he on, do you know?
Natasha: He was on really light antibiotics. Like Vancomycin and they just gave him broad spectrum. They gave him Unasyn in the beginning. Unasyn, I think.
RECOMMENDED ARTICLES:
Patrik: Right, Vancomycin is heavy hard hitting. It’s-
Natasha: It’s a general one, though.
Patrik: No, not really. Vancomycin is very targeted towards a number of bacterias. It’s targeted towards Gram-positive and Staphylococcus aureus, also enterococci. Given that your dad had an aureus, there would have been some enterococci, one way or another.
Natasha: Oh, really? Okay. For the C diff. Yeah, they were giving it to him for the C diff, or whatever.
Patrik: Vancomycin … The reason I’m saying it’s heavy hard hitting, it’s sort of not a first line antibiotic. It’s sort of an antibiotic being used when everything else isn’t working. What other antibiotics was he on, do you know?
Natasha: I was looking through a chart but I don’t remember. Well, they gave him Unasyn. I know they gave him Unasyn at some point. The day before he died they started Zosyn and that’s the targeted antibiotic they needed for the Pseudomonas, for the Gram-negative whatever. They put him on Zosyn but the interesting thing is that the day that he was admitted to the emergency room, they started giving him Zosyn. And they just stopped that dose. I don’t know why they started it and why they just stopped it. They stopped Zosyn on 3/31/17, yeah.
Patrik: Right. Okay. I’m just trying to work out what Zosyn is because I’m pretty sure it runs … Oh, yeah. It’s Tazocin. Yeah, okay. That is a surprise that they’ve stopped that. And the reason I’m saying that, Tazocin … The reason I’m using Tazocin is it’s Zosyn in America, here it’s Tazocin but it’s the same drug. It is for Pseudomonas infections. You could almost question, given that he had a Pseudomonas infection, that that might have been part of him contributing to his passing in the end. It makes you wonder why they haven’t continued that.
Natasha: They didn’t know, in the beginning. They didn’t know because he didn’t test positive for that.
Patrik: Initially.
RECOMMENDED ARTICLES:
Natasha: He didn’t test positive for that until later, yeah. They actually had to take a sputum sample in the beginning, when he came and then they waited however many days. That’s why I think that it was ventilator associated pneumonia. Because it wasn’t until after that, that’s when he tested positive for the Pseudomonas. What is interesting is that they gave it to him on the first day he went there. I saw on his chart, on 3/31/17, in the emergency room and then they stopped it that night. They started giving it to him and they stopped it. I didn’t understand that, it was just weird. I don’t know … Why else would they give somebody Zosyn, I’m just curious.
Patrik: Zosyn is almost like standard antibiotic mainly for Pseudomonas infections but it’s almost part of … Sometimes patients come to hospital with a general infection or let’s just keep it in ICU. Patients come to ICU with a pneumonia of unknown cause. And Tazocin, or Zosyn I should say, is part of that initial treatment that you would start a patient on until you know what you’re exactly treating.
Natasha: Yeah, that would make sense. Yeah.
Patrik: So that’s why I-
Natasha: Continue doing that.
Patrik: That’s why I’m surprised. Why have they taken him off the Zosyn? How many doses of Zosyn did he have, do you know?
Natasha: No. Like I said, I was going to go back and really refine it. I just noticed that and I was like, “Wait, they did do it and they just stopped it.” Bizarre. Then the whole yeast thing, it wound up in his blood. A yeast infection that starts in your urine … it was in his urine, that started in his urine. And they also found some yeast in his trach … in his, what do you call it?
Patrik: Yeah, around the tracheostomy site.
Natasha: How does that happen? I read that that can happen, though. I read online.
Patrik: It can happen but my first comment on that would be it’s poor nursing care. That would be my first comment. The reason I’m saying that, a patient with a trach he, especially in ICU, should have that tracheostomy site cleaned a minimum of three times a day.
Natasha: Ventilator.
Patrik: Sorry?
Natasha: He had a ventilator. He still had the ventilator.
Patrik: Oh, yeah. Doesn’t matter. You gotta keep in mind, a tracheostomy site is a risk for an infection because it’s and entry point to the body. A tracheostomy site therefore, especially in hospital with the risk for hospital-acquired infection being very high, you need to clean that tracheostomy — sterile — three times a day.
Natasha: Wow, you do.
Patrik: A minimum of three times a day. I don’t know whether they’ve done that. Again, that would be part of the medical notes.
Natasha: That’s gross.
Patrik: That is gross. One of the reasons I’m saying that, number one … Hang on, your dad … Just remind me. Your dad had a tracheostomy even in the nursing home?
Natasha: No, he didn’t have a tracheostomy. He still had the ventilator.
Patrik: How come you’re talking about a tracheostomy?
Natasha: No, the trach aspirate. So it says trach aspirate which is sputum.
Patrik: Okay, the ET tube. Then I don’t know. I don’t know why he had a yeast in his tube. What that basically mean is, on the one hand, you know that he had the Pseudomonas in his lungs but now you know he’s had the yeast there, too. That’s what you’re saying.
Natasha: That’s what I could have sworn. Hold on a second … I could have sworn that my sister had said that … Wait, hold on … Did she write that correctly? I could have sworn that’s what it said, Pseudomonas. Let me see … Few budding yeast … Rare normal respiratory flora present. Non, non. Wait, I may not be reading what she wrote properly. It’s definitely in his urine.
Patrik: The yeast in his urine?
RELATED INFO:
Natasha: It’s definitely in his urine. The Pseudomonas is in his sputum but I could have sworn she had written something that there was some yeast also in his sputum. But, I don’t-
Patrik: Didn’t you say that the Pseudomonas was part of his UTI as well?
Natasha: His what?
Patrik: UTI, his urinary tract infection.
Natasha: No, they said he didn’t have a UTI this time. He didn’t have a UTI apparently.
Patrik: Okay. But he had UTIs in the past, didn’t he?
Natasha: Yes. In the past, he did.
Patrik: There’s a very high chance that when he had a UTI in the past that here was some Pseudomonas growth. There’s a very high chance.
Natasha: Yeah, you had mentioned that before.
Patrik: Yeah, very high chance. And that’s where the Pseudomonas, one way or another, is almost waiting to come out again. And because of that history of UTIs, I would have thought that’s even more a reason to continue with the Zosyn.
Natasha: Yeah, I don’t know why they did that. I was shocked that they did that. But interestingly-
Patrik: Just to remind me, you mentioned you’ve seen the death certificate and in the death certificate it said something of sepsis of unknown cause what was mentioned as a death cause. Was that right?
RECOMMENDED ARTICLES:
Natasha: Well, no. We went over that and you said it was very specific. They said aspiration pneumonia. Again, I believe that from what I’m looking at from the records and from what I’ve discussed with my sister, it really seems likely that he died because of infections he got from the hospital and not being treated properly. Not because of the original aspiration pneumonia. Because, I could have sworn there was also a note where they said, “Oh, the patient is actually doing better,” the second day that he was there. And his blood work wasn’t so bad and then it just got progressively worse, at some point.
Let me tell you something else that’s really interesting, Patrik. Key x-rays are missing from the radiology films. I went to get the x-rays. On April 4th, they talked about how his endotracheal tube was … You know how it was kind of moved from the carina. It as like five centimeters distal … Some language like that. And then they said that there was a pleural effusion. But then on 4/5 there’s no chest x-ray but then on 4/6 there’s a chest x-ray and it says “no pleural effusions, endotracheal tube in place.” And when I have the films, I was looking at it on the disk. There’s about three x-rays on 4/4 which are missing. It’s just white. There’s nothing on 4/5 and then there’s a couple of other x-rays that are just missing from his chart. If something on April 4th says you have a pleural effusion and the endotracheal tube is … It’s basically saying that maybe it moved or something, right? To five centimeters from the carina or something. But then how come you wouldn’t take another x-ray on 4/5?
Patrik: Absolutely!
Natasha: Do you know what I’m saying? And how could the pleural effusion just go away on 4/6?
Patrik: There are a number of things I can see here, Natasha. Number one would be, as I mentioned to you in our last conversation. When tubes get moved in or out, even if it’s only by one centimeter, it usually needs to be followed up by a chest x-ray to confirm that position. That’s not moving. That’s my experience, that’s never been any different. That’s number one. That seems to be missing. Number two, almost every patient in ICU, who’s ventilated and is in an acute critical phase — and your dad was in an acute critical phase all week — from my experience, has a chest x-ray daily.
Natasha: Yes. They’re supposed to, I know! That’s my experience, too. You have a chest x-ray every single day.
Patrik: Here is what I believe is what they haven’t told you. The way I look at your dad’s situation is the following, just by what you’re telling me. Your dad was in a nursing home. Everybody who doesn’t know your dad, outside of your family, would think, “oh, he’s got no quality of life.” And when I say everybody that’s not true, I use it in an ICU context. So, when your dad got admitted to ICU, some of the thoughts that were going around in their minds, and I’m 100% certain on that, was, “Oh, he’s coming from a nursing home and he doesn’t have any quality of life because he’s in a nursing home, he’s had a stroke a while back, he’s immobile … What are we treating?” That would have been the way they would have looked at your dad without being overtly in your face.
Natasha: You know they were, though. You know they were. I told you stories, yeah.
Patrik: Yeah, that’s okay. So, at that level of judgment would have impacted on how they treated your dad. So, I’ll give you an example-
Natasha: I know, that’s what I’ve been saying.
Patrik: I know you’re aware of that but I’ll illustrate that with an example. On some of the board rounds that you weren’t there, when they were doing their board rounds they were looking at the medical things that were going on but the conversation would have always reverted back to, “Oh, but he’s in a nursing home and he’s had a stroke and he’s not waking up so it’s best for him”-
RELATED LINKS:
Natasha: Hypoglycemic anoxic brain injury whatever, yeah.
Patrik: … “it’s best for him to die.”
Natasha: Yeah, I know.
Patrik: That would have been the conversation that would have been going on during their board rounds. That could have well been that even on admission, somebody might have thought, “Oh, maybe it’s best if we’re not using the Zosyn and well maybe it’s best if we’re not going full steam ahead.” And maybe down the line they were thinking, “Maybe it’s best if we’re not using any Fluconazole to treat the yeast.” Having said all of that, this is where I believe there is also a leverage point. We can’t turn the tide back, your dad unfortunately is not here anymore. But here is where I think there is some leverage. Now, we’ve talked about this there was no DNR.
RECOMMENDED:
Natasha: No. Listen to what happened, though. My sister, she did not read the doctor’s progress report when he came in around six … What time did he come in? … I don’t remember, it was 6:30ish or something. When he came in, she didn’t read … Usually, I start typing something on the subject line that’s a part of the body of my email. And you know she’s a doctor, she’s a very smart doctor — she went to excellent schools. I started typing on the subject line but she didn’t see that. All she saw was, “Confirmed placement with endoscope, tube in adequate location, continue to bag patient.” Blah, blah, blah. Then I sent her the actual screen shot, I did a screen shot of the PDF. It actually reads, “Call to see patient regarding hypoxia. Chest x-ray showed ETT high – pushed in ETT and confirmed placement with Ambu Scope – Tube in adequate location.”
He actually pushed it in, it wasn’t pushed in. Then she kind of got all weird because that’s not what happened. He didn’t tell us that he pushed anything in. He just said that it was in place. He just said that it was in place, that there was nothing wrong with it, right? And then she also did a comment that before he actually that, the nurse and the patient care technician, Patrik, they were taking an obscenely long time to change my dad’s diaper.
“Thank you very much for being a part of the previous series of 1:1 consulting and advocacy sessions. We hope you will find these new upcoming episodes informative and empowering.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!