Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Tracheostomized Husband is in the ICU, now in LTACH. Will They Remove His Tracheostomy Soon?
You can check out last week’s question by clicking on the link here.
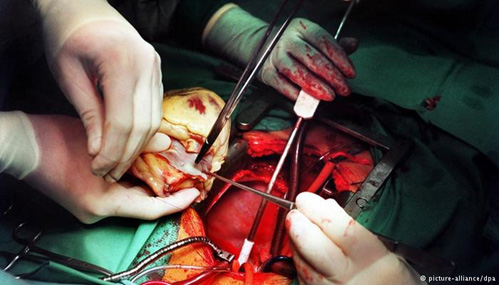
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Eva as part of my 1:1 consulting and advocacy service! Eva’s husband had a cardiac bypass surgery, had a stroke in the ICU and Eva asking if the ICU team is being unprofessional when they told her that her husband has only two options, either to be in the long term care facility or just die peacefully.
My Critically Ill Husband is in the ICU Again Due to Septic Shock. Are They Treating Him or Giving Up on Him?
Patrik: speaking… How can I help?
Eva: Hi, Patrik. My name is Eva Peters. I’m calling from Perth, Australia and I am looking for some advice on how to proceed with my husband who’s in Intensive Care here.
Patrik: Right, okay. How long has your husband been in Intensive Care for?
Eva: He has been five weeks in Intensive Care, one week on a ward. So, he was four weeks in Intensive Care, went to a ward for one week and is back up in Intensive Care. Actually, it’s more than that.
Patrik: Right. Why did your husband go into Intensive Care?
Recommended:
Eva: He had a massive heart attack, a quintuple bypass and a stroke.
Patrik: Right, okay. And that’s all happened in the last couple of weeks?
Eva: It happened December 14th.
Patrik: Right. Okay. And what are you looking for specifically? I’m sure I can help you, but it’s always good to hear what you’re trying to achieve in terms of outcomes, so we can look at working on outcomes.
Eva: Yeah. He actually had made some good progress, was stable, and that’s why he was discharged to the ward. On the ward there was not enough care, and he ended up through not very good support with sepsis and shock, which has further damaged his heart, lung and kidneys. When he went up to the ward he was off of everything. He is back on continuous dialysis although they have not tried him off yet, and they are weaning him off of blood pressure support.
Patrik: Okay. So, he’s on vasopressor, inotropes like adrenalin or epinephrine or norepinephrine?
Eva: Yeah.
Patrik: Yeah. Okay. Okay. Are you the medical power of attorney for your husband?
Eva: I am.
Patrik: You are. Okay. Okay. How old is your husband?
Eva: 68.
Patrik: Right, okay. Okay. What’s your biggest frustration at the moment? Where do you think you need the most help with?
Eva: Well, he has made incredible progress all along, and the last … He actually was not very aware and with it until the last couple of weeks. To continue obviously his brain has been healing as we’ve gone along in terms of his body strength and also his cognitive abilities, and he kind of just yesterday really kind of came to. Not in terms that he wasn’t present before, but he actually knew where he was, knew what was going on, was making decisions, telling me to pay the rent. Kind of…
Patrik: Is he back on vent?
Eva: Regained a level of…
Patrik: Right.
Eva: He’s not. No.
Patrik: So, the only reason he went back into ICU really is for the dialysis and the norepinephrine or the noradrenaline support?
Eva: Yup.
Recommended:
Patrik: And, basically, the reason he went back in is that, but obviously it sounds like leading up to that would be septic shock.
Eva: Yes.
Patrik: Right, okay. Okay. Do you feel like-
Eva: He’d been through a couple of spells … Okay. Go ahead.
Patrik: Do you feel like they’re doing everything that they can?
Eva: They are-
Parik: Do you trust them? Do you trust them?
Eva: Well, I did. However, what happened today is everyone started barraging him with information about how sick he is. And, at the end of the day, it’s about one o’clock our time now, about five o’clock the doctor … And these ICU doctors change weekly or bi-weekly, so this is someone who just came in on Monday, and really I’ve been to every rounds, but had never come in and talked to me or shared any information. He came, sat down and basically told me I had two options, that he’d reviewed his file, he was a really independent gentleman, and he wanted him to know that … at best the prognosis was life in a long-term care facility.
Patrik: Okay.
Eva: And that the alternative is that he could ensure that he died in his sleep-
Patrik: Okay. Now-
Eva: Without pain.
Patrik: Now we’re getting to the crux of the matter, and now I know that I can definitely help you. Basically, what you’re telling me is that their approach has changed from a somewhat positive approach to a more negative approach.
Eva: Yeah, probably.
Recommended:
Patrik: Would you say they’re sort of painting-
Eva: I’ve looked at…
Patrik: Would you say they’re painting a doom and gloom picture?
Eva: Yes.
Patrik: Okay. Yes. Now, that I can… –
Eva: They would say they’re painting a realistic picture.
Patrik: Yeah, sure, sure. But, let’s take the word “realistic” aside for now.
Eva: Okay.
Patrik: Let’s take the word “realistic” aside just for a moment, and you feel like its doom and gloom, it’s black and white. They’re telling you he’s not going to improve and those are the options, without telling you what else could happen on a more positive note.
Eva: Exactly.
Patrik: Yeah, okay. That’s where I can definitely help you.
Eva: Okay.
Patrik: You see, one of those issues is often that, ICUs, they tell you whatever they like really, without telling you what options you have. You also need to understand that ICUs are trying to manage their worst case scenario. Okay, what is their worst case scenario? Their worst case scenario is to look after a patient indefinitely with an uncertain outcome. And that’s your husband’s situation in essence, right?
Eva: Yes.
Recommended:
Patrik: It’s very difficult and important to understand that…that ICUs are trying to manage their worst case scenario. I’m probably exaggerating when I say they couldn’t care less about what’s going to happen to your husband in the long run, I’m exaggerating a little bit, but at the end of the day-
Eva: No, not much.
Patrik: But there is a number in there.
Eva: Yeah.
Patrik: And that dynamic we can definitely manage. I work in Intensive Care for 20 years, I’ve seen it all. I argue, I’ve seen the good, the bad, and the ugly. I understand the dynamic and I understand how to outcomes for families when they perceive that the odds are against them. Now, I would…
Eva: Okay.
Patrik: Now, I would never claim that I can save a life but what I can claim very confidently is that I can help you to buy you all the time in the world your husband needs. And I can claim, absolutely claim that I can get your husband this care and treatment. At the moment your biggest challenge is that you don’t know what you don’t know. That’s your biggest challenge.
Eva: That’s exactly right. No, I don’t and I don’t even know how to go about asking the questions.
Patrik: Exactly, and your biggest challenge is that you can’t ask clinical questions and you can’t really challenge them on a clinical level. Right, and that there I can-
Eva: I’ve tried.
Recommended:
Patrik: Sure, sure.
Eva: They don’t like it.
Patrik: Yeah, no, no. Of course, they don’t like it, at the same time you know as you would appreciate by now intensive care is a highly, highly specialised area. You know, and it will come down to very, asking very detailed, interesting question. And also you know telling them I have seen 100 other patients in this situation. And they improved.
Eva: Right.
Patrik: Right. You see what… I tell you what Intensive Care units are good at and what they are not good at. They are very good at saving lives in the short term. Okay.
Eva: Yes.
Patrik: They are not good at predicting long term outcomes. In fact, they suck at predicting.
Eva: Correct.
Patrik: I mean nobody knows what your husband’s life looks like in six days time, in six weeks time, let alone six months time. Nobody.
Recommended:
Eva: He is already, they couldn’t to date. We are blown away by what he has done.
Patrik: So, so.
Eva: They never would have predicted that he would have lived this long and made as progress as he did.
Patrik: Not bad. And that is positive. And that is probably what you need to keep looking for, you need to look at the positive spot. On a more, let’s call it, actionable level, one link in your situation is to start off asking a lot of questions to challenge them on a clinic level. Let me ask you this, have you had any meetings with the doctors in the last few days or few weeks?
Eva: I have attended rounds.
Patrik: Okay.
Eva: But I have not had any specific meetings about besides rounds.
Patrik: Right. Okay. When you say that the doctor told you on Monday or whenever that your husband has basically has two options. Was that in front of your husband?
Eva: Yes.
Patrik: Right. You need to tell him to stop doing that. It is inappropriate. It is unprofessional.
Eva: Yes.
Patrik: I am ashamed, you know, some people have better bedside manners than others. But imagine you’re lying in a bed in ICU and somebody says something like that to you, I mean that’s not going to help your recovery, does it?
Eva: Absolutely not. No. No.
Patrik: Slightly…
Eva: And
Patrik: Highly inappropriate.
Eva: This was the first day he was actually was even aware of his surroundings.
Patrik: Yeah. Yeah. So what we can do going forward, I have a number of options how we can move forward in helping you.
Eva: Okay.
Recommended:
Patrik: The best option is over the phone of course but I also have like online options where I can help you, via email and in a membership forum. But I can quickly talk you through the options and then you can make a decision from there. The other –
Eva: Okay.
Patrik: The next thing that I also suggest is that once you have made a selection from the options, we should get on the phone to the doctor, we should set up a call or you know even if you are there and in the rounds…
Eva: Yes.
Patrik: I can be there over the phone.
Eva: Really?
Patrik: Ah, absolutely. That’s the type of service –
Eva: Wow. Okay.
Patrik: That’s the type of service I offer.
Eva: I guess if I’d had you two weeks ago, this maybe would have been different. I thought I was actually doing a fairly good job of advocating and I had to call their in hospital help line a number of times to get things done.
Patrik: And I’m sure you have done a great job in advocating, I’m sure you have. I guess where it gets difficult is when setbacks happen. And I would imagine if you said it happened in December, I would imagine you might be tired, exhausted. I can only imagine.
Eva: I am pretty tired and exhausted.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: I can only imagine. And you know it’s very difficult. I mean where do you get help in a situation like that? I’m sure you can get help from like friends and family but where the problem really is, again the Intensive Care is such a highly specialised area. How do you make sense out of such a situation?
Eva: Yeah.
Patrik: And how do you like they are telling you one thing is all gloom and doom. How do you put things in perspective?
Eva: Yeah. And I don’t know I put it in perspective with my husband.
Patrik: Yes, how do you put it in perspective for your husband? And also potentially, you know, I don’t know your situation, other family members, friends, you know whatever your situation is.
Eva: Yeah.
Patrik: Bigger picture.
Eva: Yeah.
Patrik: So
Eva: Okay, well I would certainly like to start with 4 days and you can maybe help me through this situation.
Patrik: Or what do you want to start now?
Eva: Yes, please.
Recommended:
Patrik: Or, what I can do…
Eva: I need some advice for tomorrow morning.
Patrik: Okay. So what I will do… Sorry, what’s your name again?
Eva: It’s Eva. And the last name is Peters. So E-V-A.
Patrik: Okay, Eva what I will do is, are you having access to a computer right now?
Eva: I don’t.
Patrik: I would have to walk you through the check out.
Eva: Would you do that?
Patrik: Yup.
Okay, so… Now that has all gone through. So we can now proceed from here. Thank you for being a client. I really appreciate that.
So you have a meeting lined up tomorrow morning or ward round lined up tomorrow morning?
Eva: I am going to ask for a meeting. I have actually had contact with the hospital ethics people already. And, because I had met them when I first arrived here. And, so I haven’t involved them in a meeting I have just kind of let them know the situation. That’s it. I have discussed it with a friend who has kind of been supporting me. And she said what I need to do is set up a meeting with the doctor for tomorrow. So I have done this already with the doctor who was on call, in charge the two weeks he was here prior, where we actually had a team meeting and discussed care and while there wasn’t any consideration of goals at that point of time, the goals were just to get him stabilised and out of ICU. So, that’s kind of where I am at.
Recommended:
Patrik: Okay, I’ll tell you one thing that stands out to me from the, you know… especially now with the readmission back into intensive care. A set back like that can happen, they happen all the time.
Eva: Yes.
Patrik: Unfortunately. However, that is no reason for doom and gloom. And you know it is just a setback. So first of all we need to change your perspective. You know, so you aren’t getting sucked into that negativity. And I don’t believe that you have been getting sucked into the negativity. Right because otherwise you wouldn’t be-
Eva: It’s…It’s been hard not to.
Patrik: Absolutely. I appreciate –
Eva: I’m trying to have hope –
Patrik: Yes.
Eva: and acceptance.
Patrik: Yes. Look hope, hope is good. Being positive is good. However, having, and that’s what I’m trying to help you with, having clear management strategies are better, or combined with hope.
Eva: Yes.
Patrik: Combined with hope.
Eva: Exactly.
Patrik: Combined with hope.
Eva: Yes.
Patrik: Combined with positive thinking.
Eva: Yeah.
Patrik: Are much better than, I’m all for positive thinking and hope but you will also need some management strategies. For example, what you mentioned earlier about how the consultant talked in front of your husband that he has two options. You need to tell this consultant in no uncertain terms that he needs to stop talking negatively in front of your husband.
Eva: Okay. So I can-
Patrik: And I can come in and do that-
Eva: So I can come in and do that-
Okay…Okay.
Recommended:
Patrik: Right. Because imagine you are a patient in this bed and you are sick and you have people talking in front of you about what your options are which is number one hospice or number two going into a long term facility. Right. There is nobody saying, you know, we do x, y, and z and we will try and get you out of here, alive.
Eva: No. No. No. No.
Patrik: Here’s the other thing Eva that is really important to understand, if your husband was on a ventilator and in an induced coma, right? The situation would be much more grim. Okay. Your husband-
Eva: Absolutely.
Patrik: Is not on a ventilator. Right? That is positive. A lot of patients when they go on shock…
Eva: Yeah.
Patrik: Shock, they end up being ventilated.
Eva: Yes, and they talked about that.
Patrik: But –
Eva: They talked that this week that they just wouldn’t. He wouldn’t recover from that.
Patrik: Aww… they are basically telling you they are closing the door for ventilation if need be. Is that basically what you are telling me?
Eva: Yes.
Recommended:
Patrik: Okay. So. Okay. Do you feel just looking at your husband that he needs ventilation?
Eva: No, no. He is breathing well on his own.
Patrik: Okay, good, good. If God forbid, your husband was to deteriorate would you want him to be ventilated? If that would save his life?
Eva: I don’t think he would be able to recover.
Patrik: Okay, what makes –
Eva: Come off the ventilator.
Patrik: Okay, what makes you think that way?
Eva: His heart damage is pretty significant. His EF is –
Patrik: I was just about to ask you that. Do you know-
Eva: I’m sorry.
Patrik: Do you know about EF, ejection fraction?
Eva: Just what I have learned about here.
Patrik: Sure.
Eva: So, I get numbers that vary between 20 and 30 percent.
Recommended:
Patrik: Okay. Is he currently on medication such as dobutamine, dopamine or milrinone? Have you heard of those medications?
Eva: Yes.
Patrik: Right.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







