Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives of Families of critically ill Patients in Intensive Care, so that you can have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from one of our readers and the question last week was “How long does it take to die after removing the breathing machine or life support?”
Youcan check out the answer to last week’s question here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I answer another question from one of our readers and this week’s question is
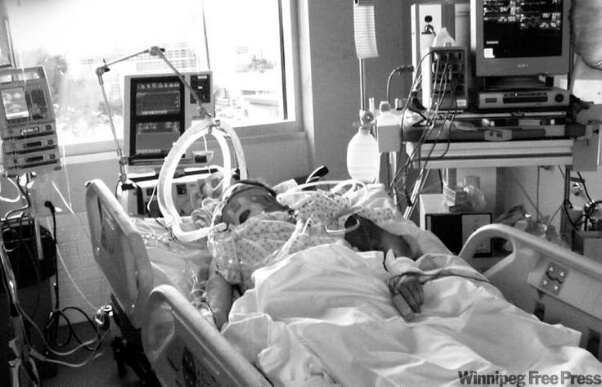
”My wife is in Intensive Care VENTILATED with HIGH OXYGEN requirements and with OESOPHAGEAL CANCER, is she going to be OK?”
Hi Patrik,
my name is Steve and I live in England in a little town.
First of all what a fabulous website you have, really helpful!
My wife had an operation for oesophageal cancer, it went well, the surgery was successful, then there was a problem with Pneumonia!
My wife has been in Intensive Care for 5 days now and she’s on a ventilator. They did hope to do a Tracheostomy today but weren’t able to because her oxygen requirements were very high she was on oxygen of 70%.
My question for you is, I want to make sense of the machines in front of me, sometimes they get excited when the pulse rate, which was as high as 140 beats per minute when she was first admitted, is down as low as today is 92 beats per minute and I feel that’s good. Over time I look at the oxygen levels and it is 94, 95% but then I recognize that she’s on 70% of oxygen.
Other times I look at the blood pressure and so my question really is what should I be looking out for, how do I interpret what those numbers mean, any advice you can offer would be really helpful! Thank you!
I do have another question. My wife has been in hospital now for 16 days and she has had no bowel movements. They tried an enema ( in her co motored state) but that did not do the trick. There are also no signs of faeces in the rectum. They are administering a laxative and feeding her through a feeding tube into the duodenum. Will the lactose slowly but surely help move the faeces down?
What thoughts do you have?
Thank you
Hi Steve,
thanks for your question and thanks for your kind words regarding our website!
I’m also sorry to hear that your wife and your Family are having such a terrible time in Intensive Care!
As it relates to your question, you are absolutely correct to say that your wife’s heart rate of 140 beats/ minute is very high.
It’s nothing unusual that when Patients first get admitted to Intensive Care, even though they are unconscious, in an induced coma that their heart rates are high. It’s a stress response and it could also be a response to a fever, temperature or infection or severe pain. It could also be a response to fluid depletion, especially after surgery.
Even a heart rate of around 90 is still quite high, but of course better than 140. A normal heart rate would be around 60- 80. As a rule of thumb, any Patient in Intensive Care tends to have a higher heart rate than in a normal situation. Keep in mind people are out of their comfort zone, they are stressed and they are often in pain as well.
As it relates to the oxygen levels you were referring to, know this:
Oxygen saturation should be above 95%, however as you correctly pointed out, your wife is on 70% oxygen so the Intensive Care team may have adjusted their parameters they want to achieve regarding the oxygen saturation and they may well be happy with levels above 90%.
As the Oxygen levels on the ventilator come down, oxygen saturation goals again, may be adjusted accordingly. Just keep asking.
Blood pressure is another separate parameter and a normal blood pressure is anywhere between 100- 150 on the upper(systolic) scale and 50-90 on the lower scale(diastolic). In Intensive Care we also often look at the medium or mean blood pressure and the mean blood pressure should be above 65 for a good kidney perfusion.
Also, as far as your question with the bowel movement go know this, 16 days without bowel movement is a very long time, very unusual and it can also be very dangerous!
I believe that with Oesophageal cancer you wife would have had TPN(Total parenteral nutrition) for a while and therefore there would be a delay in opening bowels. This would also explain that there is no sign of faeces in the rectum.
Starting feeds via the duodenum makes sense and giving laxatives as well, to get the bowels going.
Ask the Intensive Care team why there’s no faeces in the rectum, also find out how much feeds your wife is getting, usually in ml/hr.
The most important thing to look out for though, is to find out that there’s no Ileus(bowel blockage), again keep asking. This can be diagnosed in a CT of the abdomen.
I hope this helps Steve and I wish you and your wife all the very best!
Please let me know if you have any other questions!
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s episode of “YOUR QUESTIONS ANSWERED” and I’ll see you again in another update next week!
Make sure you also check out our BLOG section with more tips and strategies or send me an email to [email protected] with your questions!
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Sincerely, your Friend
Patrik Hutzel