Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Dad Gets Too Much Sedatives In the ICU. Will He Still Wake Up from an Induced Coma?
You can check out last week’s question by clicking on the link here.
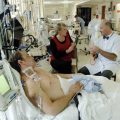
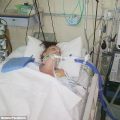
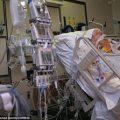
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Rosie, as part of my 1:1 consulting and advocacy service! Rosie’s dad is with a tracheostomy and is on a ventilator in the ICU. Rosie asks how long should her dad wait until he can be weaned off the ventilator and finally leave the ICU.
How Long Should My Dad Wait Until He Can Be Weaned Off the Ventilator and Leave ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Rosie here.”
June: It’s a massive company with many hospitals.
Patrik: Right. How big is this ICU specifically? Is it five beds, is it 10 beds is it 30 beds?
Linda: So he’s in-
June Overflow.
Linda: … overflow unit. Maybe I don’t know. Maybe Sarah knows, Sarah do you have an idea of how big the ICU’s are?
Sarah: I’m googling it right now.
Linda: Okay.
Patrik: The reason I’m asking how big the ICU is, because I’m well aware that all ICUs are having makeshift ICUs at the moment because of the demand. But let’s just say during normal times this is a 5-bed ICU which would be really small okay? I would argue any ICU less than 10 beds is a small ICU, okay. Small ICUs generally speaking deal with less critical patients, with fewer critical patients. They are still dealing with critical patients. But you know you look at a big metropolitan ICU 30, 40, 50 beds they have exposure to ARDS all year round, irrespective of COVID.
RECOMMENDED:
Patrik: You take a 10 bed ICU and now all of a sudden they are exposed to ARDS which is often a novelty for a smaller ICU and they don’t know what to do. They don’t have the expertise.
Patrik: They don’t have the exposure that big ICUs have. Now the smaller ICUs still have doctors visiting that work in the bigger ICUs and they have nursing staff that work in the bigger. So I’m not saying it’s all doom and gloom but from my experience, the smaller the ICUS the less experience the less resources, that’s why I’m asking. I know that this hospital where he’s in now is huge but I also know not every facility that they own has a big ICU necessarily.
Linda: The hospital where he is in, it’s pretty big I would think no?
Patrik: Okay.
June: So all of our doctors have been pulmonologist, it’s not just random specialties or anything like that, right?
Patrik: Okay good.
June: Every single one of them is a pulmonologist even though some of them are very young and probably this is their first rodeo basically right of dealing with this.
Patrik: Yeah okay.
Linda: But his first doctor was the director for pulmonology.
Patrik: Okay good. That’s good to know, good to hear. I mean after four weeks do you still have confidence that they know what they’re doing?
June: You know, two hours ago, three hours ago before the call, with the latest doctor, I was doubting it, I was really doubting it.
Recommended:
Linda: Yeah so Patrik let me tell you, every week he has a new doctor.
Patrik: Yeah sure.
Linda: He’s not had the same doctor. So like the very first doctor was the director of pulmonology he was actually his regular doctor so he was his patient from before.
Patrik: Yeah, I see.
Linda: So he was good. Then every week we’ve been getting a new doctor and each one has their own style. There’s been a little bit of a lack of continuity of-
June: Continuity of care is difficult right now.
Linda: … care. So the last doctor we had was not so good but this new doctor whose first day is today, is more experienced-
June: He gave us some confidence, all of sudden, okay? But you know like I said two hours ago before this call I was really not feeling good about where this was going.
Patrik: So before this new doctor showed up, did they give you a grim outlook? What was the outlook they were giving you before this new doctor showed up?
June: You know they’ve always tempered.
June: They won’t give you any predictions.
Patrik: Okay.
June: They don’t know.
Patrik: But they haven’t been overly negative either?
June: It depends on the doctor. Yeah but it’s always been tempered because they don’t want to promise, give you hope that doesn’t exist.
Patrik: That’s right, they wouldn’t. You’ve never felt pushed to agree to withdrawal of treatment.
June: No
Patrik: They’ve never asked you let’s stop treatment.
June: Never, not even once, yeah.
Patrik: Okay, they’ve asked you to talk? Have they talked about DNR?
June: No.
Patrik: Do you know what I mean by that?
Suggested links:
June: Yes.
Patrik: They’ve never talked about that?
June: No.
Patrik: How old is your dad?
June: He is in his 70’s.
Patrik: That’s pretty young. Any pre medical history? Any significant pre medical history?
June: Maybe depression. He’s-
Linda: Prone to pneumonia.
June: He’s prone to pneumonia. Prone to-
Linda: Infection.
June: Asthma.
Linda: Sinus.
June: Sinus infections. So he’s always had some respiratory issues.
Patrik: Okay with the history of pneumonias any previous ICU stays?
June: No.
Patrik: Okay that’s good. When did they do the tracheostomy how long ago did they do the trach?
Linda: Two weeks ago.
June: Three weeks ago now.
Patrik: Okay. Well I can tell you the positives to me are a lot of families that I’m talking to in a similar situation by now would feel pushed towards withdrawing treatment. I’m glad to hear that hasn’t been brought up, so that’s positive. The negative is four weeks or a month of Nimbex never came across, always temporary maybe up to a week I’ve seen it maybe but that’s probably about it. You know four weeks that is unheard of.
Recommended:
Patrik: With ARDS and not being able to control ventilation which is why the Nimbex was introduced, I do believe a referral should have been made to an ECMO center to an ECMO bed. Because you know once he’s on ECMO the Nimbex could be taken off I argue. The challenge with ECMO is if you look at the literature, the literature suggests no one above the age of 65 is getting ECMO. Your dad is in his 70’s, ECMO beds are in high demand outside of COVID. They are in incredible demand at the moment with COVID. The longer time goes on, the less likely it is he will get ECMO. But ECMO I would argue if he could go on ECMO they could stop the Nimbex pretty quickly.
Linda: You should ask about that.
Patrik: You should ask. Again I think it should have happened two weeks. So if once they realize okay we’re not making progress with proning, we’re not making progress with Nimbex that is when they probably should have made that call. It would be very difficult at the moment to find an ECMO bed.
June: So I don’t think they have it available. It’s not an option.
Patrik: Yeah. They would have to make a referral to another hospital. Which again in this pandemic situation, is unlikely, very difficult. So, is he on vasopressors, do you know what I mean vasopressors or inotropes have you heard of that
June: Is that for blood pressure?
Patrik: Yes.
June: I don’t know if it’s that class of drugs but he is on something for blood pressure yeah.
Patrik: Is he on epinephrine, norepinephrine, or vasopressin?
June: I have to find out, I don’t know the answer to that yeah.
Patrik: Okay. Are they talking about with ARDS what often happens is, you talked about the infiltrates earlier. What also happens in ARDS is the lungs might get scarred are they talking about that?
Linda: They did yeah.
June: Yes.
Patrik: Did they elaborate further on that?
June: Basically what they were saying, we won’t know the extent of his lung function until like months later basically. It will take time to know the extent of this.
Patrik: Damage.
June: Yeah.
Recommended:
Patrik: When was the last CT scan he had done for the lungs?
June: Very recently.
Linda: Yeah.
June: So they thought-
Linda: a week ago, right?
June: Yeah something. It’s like in the last few days.
Linda: So one of the things that’s currently going on with him is like extreme water… Like fluid buildup, he said. So they did a CT scan even of the belly and it’s very swollen and they said it’s most likely just water. This very big, they keep saying it’s a lot of swelling in his body. He talked with the nurse and he said the pelvis is all filled with fluid where even if you touch his the skin breaks.
Patrik: My goodness, okay.
June: So they’re reducing it now with the diuretics-
Patrik: Lasix.
June: … or Lasix yeah.
Patrik: Yeah the Lasix okay. Is he opening bowels?
June: Yeah.
Linda: Yes.
June: He had two, three bowel movements the last couple of days.
Patrik: Okay that’s good. Have they used in this sequence of treatment while he was going through the ARDS treatment have they used the Remdesivir?
June: Earlier on-
Rosie: Yes.
Patrik: Yeah? Have they used nitric oxide?
June: No.
Rosie: No.
Patrik: Have they used epoprostenol?
June: No.
Patrik: Have they used sildenafil?
June: What is that? It sounds familiar.
Patrik: Sildenafil is also known as Viagra but it’s used for ARDS?
June: Okay Viagra no, they have not.
Patrik: Right. You should ask those questions. You should ask-
Suggested links:
Linda: So in nitric, remdesivir we had it or he had it for one week when he first was hospitalized. Nitric oxide Epoproste-
Patrik: Epoprostenol it spelled E-P-O
Linda: Right
Patrik: P-R.
Linda: Yeah.
Patrik: O-S-T-E-N-O-L.
Linda: Okay got it.
Patrik: It’s a nebulizer. Nitric oxide is a gas that they can introduce into the ventilator. It’s a toxic gas but it helps for ARDS. It can only be used temporary in very small doses but I have seen it effective in ARDS. Epoprostenol is a nebulizer and Sildenafil or Viagra is used as a tablet, can be given through the nasogastric tube. Having said that, your dad can’t absorb because of the Nimbex.
Linda: Yeah.
Patrik: Or very slowly absorb.
June: Very slowly.
Patrik: So the Sildenafil is not in IV form it’s just a tablet that they need to crush.
June: So what do these do for him?
Patrik: The nitric oxide is opening up the shunt in the lungs, right. The Epoprostenol is a nebulizer again that’s opening up some of the infiltrates in the lung. The Sildenafil, so when someone in ARDS, there’s a lot of pressure in the lungs, right and it’s called pulmonary hypertension and the Sildenafil is ringing the pressure down in the lungs.
June: Okay.
Patrik: Right? If all that fails, and it looks like so far it has failed, you talked about the … Okay 20 years ago before ECMO the first line treatment for ARDS was nitric oxide and prone position, those were the first-line treatments for ARDS 20 years ago. It’s still to a degree first-line treatment but now you have as a second line of treatment, you have ECMO. That wasn’t there 20 years ago but again I do believe the ECMO you have to do it fairly early on.
Linda: Yeah.
June: Yeah I don’t think that was an option for us maybe-
Linda: They just gave him Remdesivir and basically told us we don’t even know if it works.
Suggested links:
Patrik: Yeah of course no they don’t. They wouldn’t. Let’s just say they could take the Nimbex off and they can make progress with your dad’s ventilation. Let’s just say they can do that there will be a very long road to recovery because you got to picture this, he’s been in an induced coma, and he’s been paralyzed for weeks. I argue, if he could wake up, he couldn’t move even his arm or his legs, he would be paralyzed. Now that’s reversible because it’s caused by medication, right? But it will be a long road to recovery.
June: So would you say that’s in a rehab how many months?
Patrik: That’s probably hard-
June: It depends.
RECOMMENDED:
Patrik: Yeah it depends. Because he can’t move it will be challenging for him to be weaned off the ventilator, right? So you got to picture this, there’s sort of three ways how people leave ICU and let’s just quickly look at those three ways so you understand what that might look like. The first way for someone to leave ICU is you get them off the ventilator and you move onto a hospital floor, that’s the best case scenario. The second way is for people to die, that’s another way to leave ICU and the third way is for people to have a trach and especially where you are patients often end up in LTAC have you heard of LTAC?
June: Yeah.
Patrik: Right. So patients end up in LTAC. If they end up in LTAC, there can be many weeks sometimes months of weaning off the ventilator right? So that’s why a timeline is very hard to say, I would argue your dad can only come off the ventilator, once he can start moving again, right? So the physical therapy, almost needs to be first. Needs to go hand in hand. But you know the physical therapy first, starting again with arm movement leg movement then starting with breathing exercises. Starting with simple things like sitting on the edge of the bed will be a massive challenge going forward.
Patrik: So, that’s why putting a timeline on this is very difficult. I’m always saying to families like as much as you would like to look into the future, ICU is take one day at a time. It’s a difficult situation and you’ve already been very patient and I believe your patience will be stretched to the limit.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!