Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
Is Withdrawing Treatment And “Pulling The Plug” On My 34 Year Old Sister In ICU Illegal?
You can check out last week’s question by clicking on the link here.
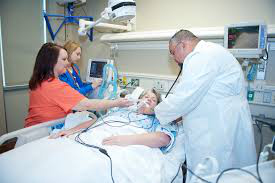
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Andrea who has her 34 year old sister in Intensive Care with non-Hodgkin’s Lymphoma and is currently experiencing decrease in blood count as well as having second thoughts about the treatment her sister is getting.
How do I make a decision if the medical team is telling me to withdraw the treatment for my sister but, I still want to fight for her?
You can also check out previous 1:1 consulting and advocacy sessions with me and Andrea here.
Patrik: It would.
Andrea: Yes, that’s what I thought. I mean, I’m not trained. I mean, it’s just logic. If a machine is doing something for you, you become lazy.
Patrik: That’s right. But, but, there are … and what was the answer to that question? Did they tell you why?
Andrea: To give her lungs a break, cause she’s working hard.
Patrik: Yeah, yeah.
Andrea: And I … I said to them … and I … cause I’ve asked, which part of the machine is her breathing, so I can see what the vitals are, and then, I’ve noticed, when I sit down, I talk to her, she starts breathing on her own. She’s …
Andrea: Yes, please. Cause, the thing is that … my sister said to me, my older sister, she’s nice, “It’s a form of euthanasia somewhere.” If they so much as turn the machines off, they stop treating, which is, essentially, turn the machines off. Alright?
Patrik: No, not necessarily. Number one, I totally agree with you, and it’s always been a point of my discussions in ICU in the past, that … where is the line between gently withdrawing treatment, and euthanasia? Right? I believe there is a very fine line, between both, right? Also, keeping in mind that … yeah, that’s one thing. The next thing, if for whatever reason they want to go down that route, they need to discuss you … you and your mother, and other medical power of attorneys, you need to agree to that. That would be a whole big discussion, I believe. Right, before that would happen.
Patrik: You’ve successfully, I believe, in the last two weeks, said to them, “Look, we don’t want an NFR, we want to continue at this point in time.” Right? And I believe … I believe that … that point of view hasn’t changed.
Recommended articles:
Andrea: No.
Patrik: No, right. Yes, you have a family meeting tomorrow, and they may bring it up, but they may, also, just want to give you an update. If I was you, I would also ask for the neurologist to be there, because, especially, you haven’t had any form of discussion around the results of the CT or the MRI, have you?
Andrea: Nothing, no.
Patrik: Yeah. I would … look, I tell you, a family meeting in ICU, I almost refer to it as high stakes, because they know what to say, cause they doing it every day, and they know what they want out of this family meeting. It good’s if you … and we can work towards that to get you prepared, to know what questions to ask.
Andrea: Yep.
Patrik: And, also, upfront, ask for the neurologist to be there. Also, if you feel, if you get a hint, either today, or tomorrow, that they do want to bring up withdrawal of treatment, and you think they want to move in that direction, maybe to postpone the family meeting.
Recommended articles:
Andrea: Right.
Patrik: Right?
Andrea: We’ll we … we… we won’t feel the pressure, we’ll say no. You need to continue treating her. I … we’re very strong, we’re 100 percent.
Patrik: Good.
Andrea: At that decision. You need to continue treating her.
Patrik: Yeah, yeah.
Andrea: My mom, will not … she’s like … my mom says, “I’m not letting my baby go.” And that’s what, in her mind, in my mind, in essence, that’s what it means to us.
Patrik: Yes, absolutely.
Andrea: Whatever, when she wakes up, and I’m hoping to, dear Lord … they’re all saying she won’t wake up. The brain damage in her brain, it’s too far gone. And, we haven’t even had a discussion with the neurologist, and what it means.
Find more information about this brain damage:
Patrik: That’s right.
Andrea: And, also, and I said to them, I go … I go … and I asked the doctor yesterday, and I say you’d had to… he was just explaining certain things. And I go, “Can the parts of the brain be retrained?” She goes, “They’re dead.” I go, “Can they be retrained?” She’s like, “No.” And I go, “Well, the neurologist said that the cells around those bits that are dead, can take over. And you can retrain the brain.”
Patrik: Yeah, yeah.
Andrea: And he’s saying, “No.” And I go, “Well, the neurologist told us that.” And he goes, “That’s just too many bits.” And I go well … and then I started reading last night that they actually do it in the U.S., stem cells, for brain damage.
Patrik: Yeah, yeah.
Andrea: Anyway.
Patrik: Yeah, I know. I think it’s really important that you speak to the neurologist. And I think you’re right on track that you want to get a second opinion from another neurologist. I … I think … look … I do believe that the ICU, they would be looking at the combination Non-Hodgkin’s and the stroke and … their view is of Non-Hodgkin’s, we’ve seen patients die in the past, plus the stroke, they would be very negative about that. But, that shouldn’t stop you from doing what you’re doing. They’re always things … we don’t know the outcome. But, you’re absolutely right to work everything in favour for your sister.
Recommended:
Andrea: For sure.
Patrik: That’s all we can do for now.
Andrea: Yep. And … and Patrik, is there any drug they can use to wake her up? Is there anything …
Patrik: Uuhhmm. Yep, yep, so, yes, so. Here is … here is… you mentioned the shake before, right? There’s two things there that I could see. Number one, would be the seizure, as we discussed. The other thing is, Midazolam, we’ve talked about the Midazolam, right? And, we’ve talked about morphine. Those drugs are highly addictive. Okay? And if you have Midazolam for a number of days, or morphine for a number of days, some people might go through withdrawal.
Andrea: Right.
Patrik: Right? Because, those drugs are highly addictive. That shake might well be that she’s withdrawing from either, whatever she had, Midazolam, morphine, or maybe Fentanyl. They’re all highly addictive. Most patients, when they’re taken of the Midazolam, morphine, or Fentanyl, they shouldn’t just stop the medication, they should gradually reduce it so people don’t go through withdrawal. I don’t know whether that’s happened, it often doesn’t happen, because they want to wake up people quickly, and all that sort of thing, right?
Patrik: That is one thing, and, if … to answer your question, can they give her drug? If they think she had too much Midazolam, too much Fentanyl, or morphine, yes there are drugs they can give her, there are antidotes, right? Somebody’s overdosing with morphine, there’s a drug called Naloxone they can give and patient usually wake up very quickly. If people overdose with Midazolam, there’s a drug called, Flumazenil for Midazolam overdose.
Patrik: Now, it really comes down to how long your sister was on those drugs, and do they think she had too much of it? Now, as time goes on … how long is she off those drugs, now, do you know?
Andrea: From Monday, I think.
Patrik: That’s a week, tomorrow will be a week.
Andrea: A week.
Patrik: Yeah. Look, I do think that if the shake was a one off, and she’s, sort of, a week down that track, I think the chances that she actually had an overdose on either of those drugs is low. But, again, it’s always good to ask the questions.
Andrea: Can … can they test for that?
Patrik: No. Not really.
Andrea: No… So that’s no.
Patrik: They don’t, no. Having said that, I’m sure there would be some blood tests, but I haven’t seen that.
Andrea: Right.
Patrik: I haven’t seen that. Okay.
Andrea: Is she … is she technically in a coma? Is that what …
Patrik: Yes. She is. Yes, she is technically in a coma. But, at the moment, it’s, sort of, hard to say whether she’s in an induced coma, or whether she’s in an actual coma. Right? Because, people are in induced coma when they get the Propofol, the Midazolam, the morphine. That’s an induced coma.
Andrea: Right.
Patrik: And then, if people don’t wake up, if it takes a couple of days, if they don’t have a brain injury, they’re technically still in an induced coma. And, if they still don’t wake up, then at some point you call it an actual coma. Because, patients don’t wake up for whatever reason.
Find more information about induced coma:
Andrea: Right.
Patrik: Right? I would say, that if your sister, in three days, hasn’t woken up, it’s more like a natural coma. Some people might even say it’s a vegetative state. But, again, I think it’s way too early to call it a vegetative state. A vegetative state is normally if people don’t wake up after months, or after years.
Andrea: Right, okay.
Patrik: Right? But, I think that discussion with the neurologist, and when I say with the … it needs to be with the neurologist consultant. As you might have seen by now, many senior doctors, they send their registrars, they send their junior doctors, you don’t really get to speak to a decision maker, or to somebody who is pulling the strings behind the scenes. I think a neurology consultant would be really, the next …
Recommended:
Andrea: Yeah, and that’s who we … that’s who we haven’t spoken too. We’ve only spoken to one, Saturday last week, and I found her in the hallway. And, she doesn’t … she didn’t actually personally come to actually see us. I was in the hallway and I notice this lady, and I ask her, “Excuse me, are you a neurologist?” She’s like, “Yes.” And then that’s when we got the update. But, we haven’t been physically updated by a neurologist at all.
Patrik: Yep, yep, yep.
Andrea: Only cause I’ve been hunting these people down. Which is really poor, actually.
Patrik: Very poor. It’s very poor. Okay, the other thing, if they ask for a family meeting tomorrow … now, there is a very high chance, today’s Sunday, the ICU consultant, they are usually on rosters from Monday to Sunday, some hospitals vary, but that’s … I’m surprised that they called for a family meeting on a Monday. Cause, Monday is often when they don’t ask for family meetings because on a Monday there’s a new consultant, often.
Recommended:
Andrea: He just started on Friday. Their roster …
Patrik: Ahh… Their roster might be different.
Andrea: Yes, he started on Friday, and the previous one, which was really good, he left. But, this one’s not as great.
Patrik: Right. Do you remember who the previous one was?
Andrea: His name is was… Doct.. Associate Professor Grobatchov, he’s got his name on the board, I could actually …
Patrik: No, right now, Right, no, I wouldn’t, no, I don’t recall that name either. That’s okay.
Andrea: Some eastern European guy.
Patrik: Right.
Andrea: Professor Grobatchov, or whatever.
Look out for next week’s episode of YOUR QUESTIONS ANSWERED where I continue to help Andrea with this challenge of having her 34 year old sister in ICU!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!