Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from our client Robert and the question last week was PART 10 of
You can check out last week’s episode by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer the next question from one of our readers and I want to feature another CASE STUDY this week, which is an excerpt from a 1:1 phone counselling and consulting session with one of my clients!
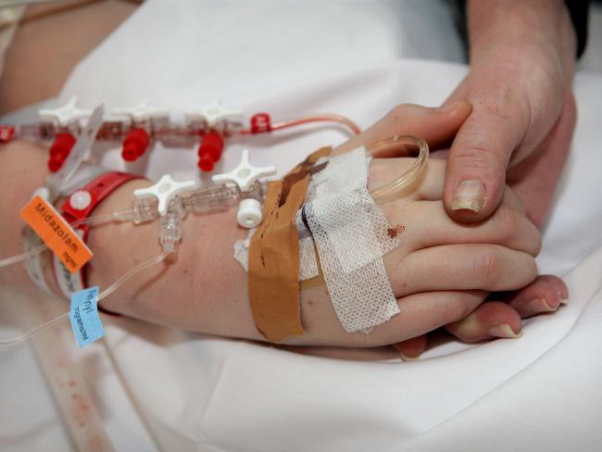
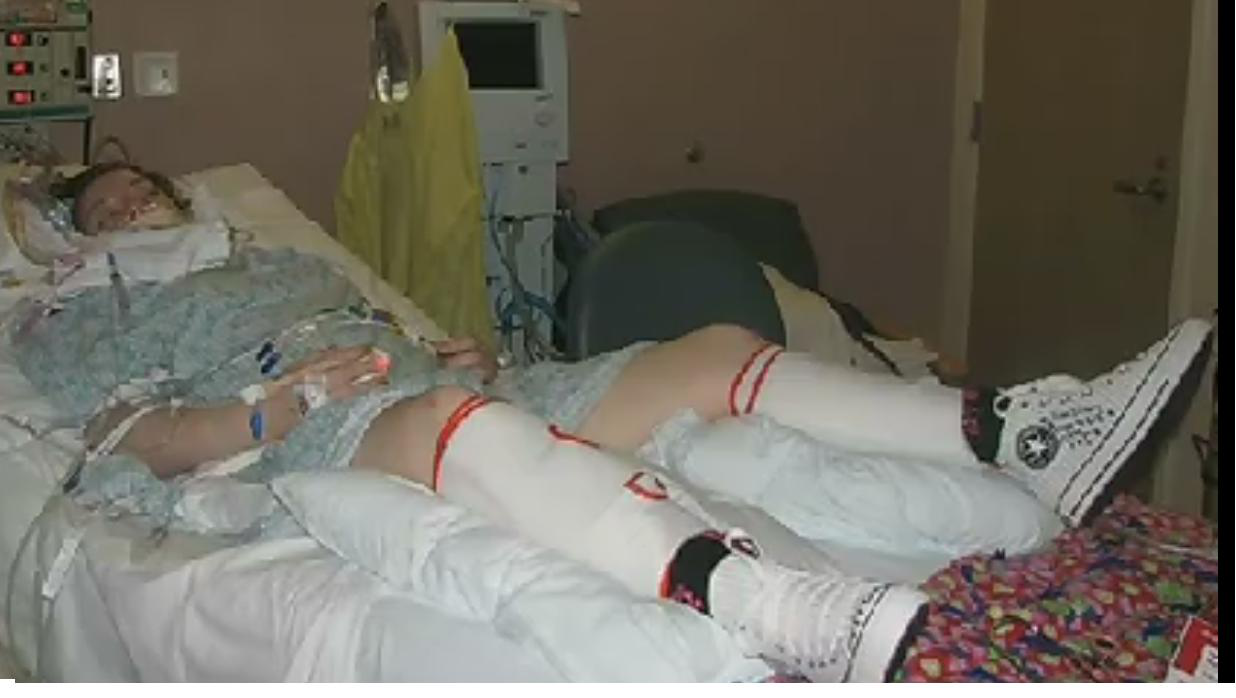
CASE STUDY: My 63 year old Dad’s been in Intensive Care for 10 weeks! He’s still on the ventilator and tracheostomy, when will he be off the ventilator?
This is another great CASE STUDY from a 1:1 phone counselling and consulting session with me, where I can talk a client through what is happening with his Dad after 10 weeks being in Intensive Care and stuck on a ventilator!
Remember, if you have a loved one critically ill in Intensive Care, you don’t know what you don’t know and the sooner you ask for help and the right advice, the quicker you can make sense in such a complex and “ONCE IN A LIFETIME” situation that you know you can’t afford to be getting wrong!
Read the CASE STUDY here
Dave: Hi, I have questions about respiration and ventilation and tracheostomy.
Patrik: Sure, Yes please. What are your questions?
Dave: My father’s in the ICU right now. He has a trach collar that has … he’s been on the ventilator, I don’t know, a very low moderation of it and last night … yesterday morning at 6:00 AM they had the tracheostomy collar … they put the trach collar on and he’s been breathing … his pulse has been in the seventies, his blood pressure’s been down 121/60 right now, his oxygen level has been 95 to 100 and his heart rate has been between 35 and 45 consistent since they put him in the trach collar and I have a respiratory therapist that just came in. It’s been … almost been, yeah it’s been 30 hours maybe since he’s had the trach collar on and I had a respiratory therapist step in and she came in … and I’m trying to wean him off of this so if you have respiratory issues, you know I’ve got to think my dad becoming ventilator dependent…
Patrik: Mm-hmm (affirmative)
Dave: But she stepped in and just straight up walked up to him and asked him, “Do you want the ventilator put on?”
He said, “Yes, obviously, of course.” I’d discussed with her that his body’s had a change … that he seemed pretty stable so I didn’t see the need to put him back on a ventilator –
Patrik: Yeah.
Dave: … if he’s been stable and she’s gone to many doctors and I’ve consistently told her, “No, no, no,” but she went to many doctors trying to get them to come in and talk to talk to me about putting him back on the ventilator.
Patrik: Right.
Dave: My question to you is with that information … his oxygen being at 98 right now, his heart rate being at 46 … is that something that he needs, to go back on the ventilator?
Patrik: No. Look, the answer depends on a number of things. You definitely are correct to say that with most of the vitals that you described that he probably doesn’t need to go back on the ventilator, but how many … tell me a little bit more … how many days has your dad been in intensive care? How many days has he been on the ventilator? When did he have the tracheostomy? Can you tell me more about that?
Dave: He’s been in the hospital in ICU for two and a half months.
Patrik: Right.
Related article/video
Dave: He’s been … he was intubated two months and a week. He was intubated a week after he was in the ICU. He had the trach collar put in two months ago … I mean the tracheotomy was done two months ago, so he’s been on the ventilator for about two months.
Patrik: Sure. And when did they first start using the trach collar? How long ago did they first start using it?
Dave: They installed the trach collar I believe three and a half weeks, four weeks ago.
Patrik: Okay, and how long during that period, how long have they been using it on a day-by-day basis … like how many hours?
Dave: They had been using it on a pretty consistent basis up until recently, within a week when they started taking him off for several hours at a time and he would tell the respiratory therapist that he needed to get put back on so that they would put him back on.
Patrik: Right. Okay. Is this a day time thing, the trach collar? Is it a night time thing? Probably would be a daytime thing, I would imagine.
Dave:: It has been a daytime thing and … because they had been putting him on the ventilator just systematically over the night time.
Patrik: Yeah.
Dave: So they just every night time just immediately put him on the ventilator and during the day, the morning, they’d take him off and then halfway through, midday he’ll say he needs it back on because of the dependency and they’ll put it back in and they’ll use the ventilator again and they’ll keep him that way. I came in from out of town because I said, you know I need to discuss this more further with … I need to be here with my father to make sure he’s getting the proper treatment.
Patrik: I agree.
Dave: … and him being … better than having doctors just …
Patrik: Absolutely. Can you tell me why is your father in ICU in the first place? What led him to this?
Dave:: He had a series of strokes that affected his … they were in his cerebellum, the left side cerebellum … and he’s … there was one in the medulla oblongata.
Patrik: Okay.
Dave: That’s what led him to be here in the first place.
Patrik: Sure. When he’s on the trach collar, can he talk? Have they tried to speaking valves?
Dave: Oh, yeah he’s got the past two valves, he can talk, he looks … he’s completely aware, he looks at you when you’re there.
Patrik: Okay.
Dave: He knows where he’s at, he knows who I am. The problem which he has … he has a bit of a panic when he’s … when he can’t make any sounds…
Patrik: Yeah, okay. Do you know … have you heard of arterial blood gases or ABG’s? Have you heard of that term?
Dave: Arterial blood gases?
Patrik: Yeah, mm-hmm (affirmative).
Dave: No, no I haven’t.
Patrik: That’s okay. So the reason that I’m referring to that is, they should be checking some blood gases … maybe once, twice, maybe even three times a day and that could be an indicator … the results from the blood gases could be an indicator for him needing to go back on the ventilator. Now when patients get weaned off the ventilator and the tracheostomy the steps usually are daytime trach collar and then night time ventilation. Okay that’s a sort of a normal pattern, if you will, to wean somebody off the ventilator.
Now, given that it’s been two and a half months, your dad probably could have progressed further. At the same time there is often a psychological dependency on the ventilator and that’s probably the biggest challenge to break through. At the same time I would like to know what his ventilator settings are. Do you know how much oxygen he’s getting while he’s on the trach collar?
Dave: I believe they had it set at ten over five?
Patrik: Okay. Oxygen …
Dave: But I can’t believe … do you know what the settings were on his ventilator prior to him being put on the trach collar? Give me one second I’m going to work it out
Patrik: That’s alright, so did you say ten over five?
Dave: I believe it was ten over five.
Patrik: That’s pretty good. That’s pretty good. If that’s the case that’s pretty good, that’s pretty low. That’s pretty low.
Dave: Yeah, his CPAP was ten over five.
Patrik: That’s pretty low. Okay, that’s good. So just from that information alone I would say your dad must be close-ish to coming off the ventilator. Now … and how long … sorry I’ve got to ask again … how long has he been doing this daytime trach collar and night time ventilator? How long? Two weeks, two months?
Recommended:
Dave: He has been doing that for probably two and a half weeks.
Patrik: Okay. Okay. Is he sleeping at night?
Dave: But he’s been on the trach collar for two months.
Patrik: Right?
Dave: Is he sleeping at night? He’s having a lot of trouble sleeping at night?
Patrik: I’m not surprised, I’m not surprised. So that could be one issue. The day/nighttime rhythm is often disturbed in intensive care, so that could be one issue. So one focus could be to get him to sleep and night and that could be by getting him tired during the day. Are they getting him out of bed?
Dave: And also he had … are they … they’re, yes, they’re pulling him out of bed and they’re also sitting him up in a chair. He doesn’t have movement of his legs or anything like that, but he also does have pleural effusion, very minor.
Patrik: Okay, okay. Very minor? So he doesn’t have a chest drain?
Dave: Mm-hmm (affirmative)
Patrik: He doesn’t have the chest drain?
Dave: I’m sorry? No he hasn’t had the drain because they said it was so minor.
Patrik: Okay, good, good, good. Okay, so there are … okay they definitely need to keep mobilising him, that’s very important, that’s one thing. The next thing is that the day/night time rhythm could be an issue, so basically they need to tyre him out during the day by mobilising him and maybe they need to give him some melatonin at night or some light sleep medication to help him sleep at night. Alright?
Dave: They had been giving him morphine for a week, a heavy dose of morphine, and when I got here I told them to stop giving him morphine because that was affecting his respiratory function!
Patrik: Oh, absolutely. Absolutely. And as long as your dad is not in pain there’s absolutely no reason he needs to be given morphine.
Dave: So since I’ve been here for the past three days they’ve stopped the morphine and he went on the trach collar and he spent thirty hours on the trach collar and they’ve only been administering Tylenol.
Patrik: Good, and your dad is not in pain? You’re certain of that?
Recommended:
Dave: No, no. I mean his knees a little sore, he’s been saying his knees a little sore, but for the most part he’s not in pain unless he’s being moved because of the … because he hasn’t been … he’s been bedridden for the past two and a half months almost three months.
Patrik: Sure. Okay. So I think from what you’re describing, there could be a psychological dependency on the ventilator, especially with ten over five, that’s reasonably low. Also would like to know how much oxygen he’s getting through the ventilator? Right? He must be on a percentage of oxygen as well as when he’s on the trach collar he would be on a percentage of oxygen. I would also be curious to know …
Dave: 40%.
Patrik: 40% on the trach collar or on the ventilator?
Dave: On the trach collar right now, he’s at 40%. He was at 90% and over the course of today they have brought it down to 40%.
Patrik: And when … how long ago was he on 90%?
Dave: I would say four hours ago.
Patrik: Okay, okay, that would be one stumbling block. 90% … you can’t be having somebody breathing independently on 90% for a long time. That would be a stumbling block.
Dave: But they brought him down to 40% …
Patrik: Yeah, sure but …
Dave: And staying at 90 over 46.
Patrik: Right, but still, you wouldn’t have … somebody would not be ready to be completely off the ventilator if they are at least intermittently breathing on 90%. Not ready. And that’s where the block gases come in. Right? They should probably do a blood gas on 90% of oxygen, see what it looks like and then do a blood gas on 40% of oxygen and probably do a blood gas on the ventilator to have that comparison.
Dave: The arterial blood gas thing?
Patrik: The blood gas. No no no the arterial blood gas. So that could be a stumbling block. SO the sleep … the day/night rhythm issue … the high level of oxygen and probably the psychological dependency on the ventilator, especially after such a long time. Those would be some stumbling blocks. I do believe your dad is close, right, to coming off the ventilator, but those are probably the issues that they need to look at.
Now, is your dad getting any physical therapy?
Dave: I’m sorry give me one second, I’m on the other line with the doctor.
Yes he’s receiving very minimal physical therapy.
Patrik: And what do you say is minimal?
Dave: They’re working him out, sitting him up in a chair for a couple hours. Aside from that though … their primary concern is the trach and his breathing.
Patrik: Oh absolutely. But with that he should have chest physical therapy. So there should be a physical therapist who is focusing only on his chest.
Dave: I don’t believe he’s receiving any physical therapy.
Patrik: Yeah, got to ask. I think that’s another missing link. Anybody who needs to be weaned off the ventilator should be having daily physical therapy and chest physical therapy in particular, with breathing exercises. You think that’s not happening?
Dave: Not since I’ve been here.
Recommended:
Patrik: Okay. Definitely got to ask for that. That’s another missing link. What … have you seen them suctioning secretion?
Dave: Yes, they’ve been suctioning the secretion and they’ve also been using the nebulizer.
Patrik: Okay, how often are they suctioning him?
Dave: Once every hour I would say and the nebulizer I think they’re running at a similar pace, maybe every couple of hours?
Patrik: Okay. Once an hour, that’s not too bad. And he’s got a cough? He’s got a good cough?
Dave: Yes.
Patrik: Okay. Okay. Alright, okay how old is your dad?
Dave: 63.
Patrik: 63? That’s very young. Well that’s good. That’s good. Well age is a factor and it’s good. The younger patients are the more chances they have to come off or to fight those issues. Your dad doesn’t have lung disease like COPD or asthma or any of that? There’s none of that?
Dave: No, he suffered from diabetes during this situation right now from lack of maintenance.
Patrik: Sure, okay. So I would think focusing on those issues that we’ve discussed … and you’re absolutely right, definitely no morphine, he needs to stay off the morphine. Physical therapy, keep mobilising, sleep at night … what else did I say … arterial block gases to compare the results, but 90% of oxygen is too high. It’s a lot. It’s a lot. That’s where the chest physio might come in.
Dave: From the arterial blood gas there?
Patrik: No no, just … if he’s on 90% of oxygen they need to start doing some breathing exercises. And there are respiratory therapist might do some of it but I do believe a physical therapist is usually much better qualified to do that.
Dave: Absolutely. And as far as your professional opinion on whether or not he should go back on the ventilator?
Patrik: If he feels that way, I’d say yes. But. But, they need to be daily … the time he’s off the ventilator on a day-by-day basis needs to increase.
Dave: Yes sir. Alright.
Patrik: That’s what they need to keep working on. If he in the mean time needs to go back I’d say let him go back, but they need to be aware of that the time is off the ventilator every day needs to increase and they need to be aware that part of him going back on the ventilator could be the high oxygen demand or that could also be still a psychological level of dependency right.
Dave: I understand.
Patrik: One of the most important things for your to understand really is to know that weaning off the ventilator in Intensive Care is often two steps forward and one step back! Your Dad has been making progress by all accounts and now he’s taking a step back. Let him do that, he might just need to rest, don’t panic!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!